3D Modeling in Pilon Fracture Surgery: A Case Report
Enhancing Preoperative Planning for Pilon Fracture: Clinical Utility of 3D Computer Modeling in Surgical Planning and Internal Fixation – A Case Report
Michael Masoomi, MRCP, PhD1,2,3,*; Latifa Al-Kandari, MD3; Meshal Alhadhoud, MD4; Hany Elrahman, MPH1
- Department of Nuclear Medicine, ADAN Hospital, MOH, KUWAIT.
- Department of Research and Innovation, Portsmouth University Hospital, UK.
- Department of Radiology, ADAN Hospital, MOH, KUWAIT.
- Department of Orthopaedic Surgery, Al-Razi Hospital, MOH, KUWAIT.
*Correspondence to: [email protected]
OPEN ACCESS
PUBLISHED: 31 March 2025
CITATION: Masoomi, M., Al-Kandari, L., et al., 2025. Enhancing Preoperative Planning for Pilon Fracture: Clinical Utility of 3D Computer Modeling in Surgical Planning and Internal Fixation – A Case Report. Medical Research Archives, [online] 13(3). https://doi.org/10.18103/mra.v13i3.6374
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i3.6374
ISSN 2375-1924
Abstract
Background: A Pilon fracture is a complex ankle fracture that, if not properly reduced, can lead to poor alignment of the articular surface and abnormal widening or narrowing of the ankle mortise. This misalignment may result in traumatic arthritis and severe dysfunction. Therefore, it is crucial to select an appropriate technique to optimally display the anatomy and disease processes. The use of 3D computer modeling in medical procedures has demonstrated promising results in improving surgical outcomes. In this case, we used 3D printing technology to reconstruct the details of a Pilon fracture in a patient and evaluate its application in preoperative planning for fracture repair, as well as its potential role in postoperative communication and follow-up. This study aims to evaluate its application in preoperative planning and fracture repair, as well as its potential role in postoperative communication and follow-up.
Case Presentation: A 54-year-old female was admitted to the Accident & Emergency (A&E) department of ADAN Hospital following high-impact trauma. Non-enhanced Multi-Detector Computed Tomography (MDCT) images of the left foot, acquired using a GE Revolution GSI CT, provided detailed insight into the extent of the injury. The images were captured with a 120 kVp, Smart mA (312-370), slice thickness of 1.25 mm, a 50 cm SFOV, 0.984 pitch, and an exposure time of 500 ms. The images revealed a comminuted fracture involving the distal tibia and fibula, with intra-articular extension into the tibio-talar articulation.
Clinical Discussion: The pixelated quantitative color CT density map (QCTDM) display provided an effective platform to create a global 3D view of the fractured ankle, enabling the precise placement of fixation screws to prevent loosening post-internal fixation. A 3D computer model and prototype were designed, produced, and printed by the authors for preoperative planning. The 3D see-through, 360-degree cross-section of the ankle clearly depicted the embedded fractured pieces, allowing the surgeon to plan an efficient approach for the removal of the broken bone with minimal time. The operative time was reduced by 50% due to thorough preoperative planning and virtual reality practice, leading to faster postoperative recovery.
Conclusions: 3D computer modeling is a valuable tool in the preoperative management of broken ankles requiring internal fixation. It improves surgical precision, reduces operative time, and enhances patient outcomes.
Keywords: 3D, Computer Modeling, preoperative Workout, Broken Ankle
Introduction
A Pilon fracture is a complex and often high-energy injury to the ankle, involving the distal tibia and fibula, with potential involvement of the articular surface of the ankle joint leading to compromised function of the joint. If not properly reduced, a Pilon fracture can result in poor alignment of the articular surface, which in turn causes abnormal widening or narrowing of the ankle mortise. These misalignments often lead to traumatic arthritis, a debilitating condition that can result in severe dysfunction of the ankle joint, chronic pain, and impaired mobility.
Achieving an accurate reduction is critical for the healing process, as improper realignment can result in long-term complications, such as post-traumatic arthritis, joint stiffness, and disability. Surgical intervention is typically required to correct the alignment of the bone fragments and restore the function of the joint. However, successful surgical outcomes depend heavily on meticulous preoperative planning. Traditional methods of planning, such as X-rays or basic CT scans, may not offer sufficient detail, especially in complex fractures where the fracture fragments are highly comminuted.
In recent years, the integration of 3D computer modeling has been increasingly recognized as an innovative tool in surgical planning. This technology enables clinicians to view fracture patterns in greater detail and provides a highly accurate, manipulable representation of the fracture. By integrating 3D models into preoperative planning, surgeons are able to visualize fracture geometry more effectively and plan internal fixation strategies with greater precision. This approach is expected to reduce operative time and improve the quality of the surgical outcome, particularly in complex fractures such as the Pilon fracture.
Studies have demonstrated that virtual reality-based surgical rehearsal and preoperative simulation using 3D models can enhance surgical precision, reduce intraoperative surprises, and potentially improve patient recovery times. Materialize Mimics Care Suite Research is a comprehensive software suite designed for the creation of 3D models from medical images, which can be particularly useful in complex fracture management. The software enables the conversion of medical imaging data (such as CT, MRI, and ultrasound) into high-quality 3D models, which can then be manipulated and analysed for detailed surgical planning. However, 3D potential benefits, particularly in complex cases where traditional methods are less effective, make it a promising area of development in modern orthopedic surgery. In this case, we utilized 3D printing technology to reconstruct the details of a Pilon fracture in a patient and evaluate its application in preoperative planning for fracture repair, as well as its potential role in postoperative communication and follow-up.
Case Summary
A 54-year-old female was admitted to the A&E department at ADAN Hospital following high-impact trauma. Non-enhanced Multi-Detector Computed Tomography (MDCT) images of the left foot, acquired using a GE Revolution GSI CT, demonstrated the extent of the injury. The images were captured with a 120 kVp, Smart mA range (312-370), a slice thickness of 1.25 mm, a 50 cm SFOV, 0.984 pitch, and an exposure time of 500 ms. The images suggested a comminuted fracture involving the distal tibia and fibula, with intra-articular extension into the tibiotalar articulation.
We developed a pixelated Quantitative Colour CT Density Map (QCTDM) which is a colour visualization technique built upon data collected from a CT scan of the left foot using MATLAB software to display data in small, discrete units or pixels, each of which corresponds to a specific Hounsfield Unit (HU) value, and to set accurate threshold values for generating a 3D model: bone (124-1626), soft tissue (-700 to 225), fat (-205 to -51), and compact bone (662-1626). The fracture pattern suggested significant complexity, with the potential for misalignment and compromised joint function if not properly addressed. The pixelated QCTDM of a selected sagittal image clearly displayed various density levels of the selected region.
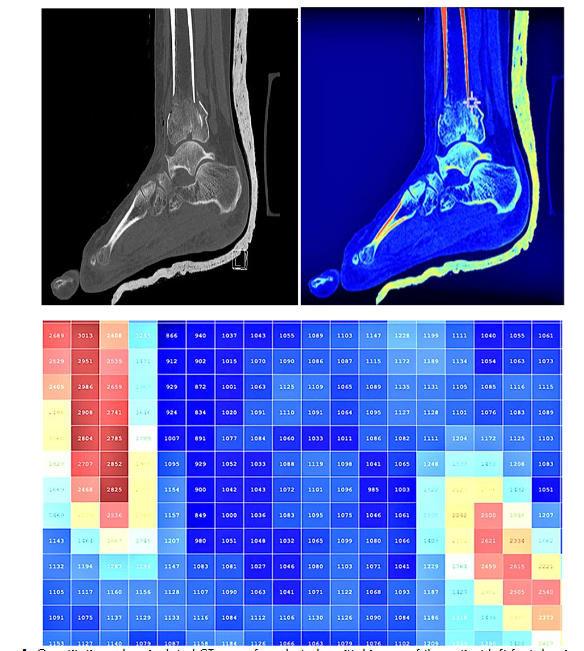
Materialize Mimics Care Suite Research which uses advanced algorithms to process imaging data and reconstruct precise anatomical structures, was then utilized to generate an unrestricted 360-degree viewing model of the foot in a virtual reality environment, allowing for detailed visualization of the shattered ankle bone and its localization, including separation of muscles, soft tissue, and fat. The software also includes features for the integration of virtual reality (VR) and 3D printing, allowing for preoperative rehearsal and the creation of physical prototypes of the anatomy. The QCTDM display provided an effective platform to produce a 3D global view, indicating the optimal locations for the application of fixing screws to avoid loosening post-internal fixation.
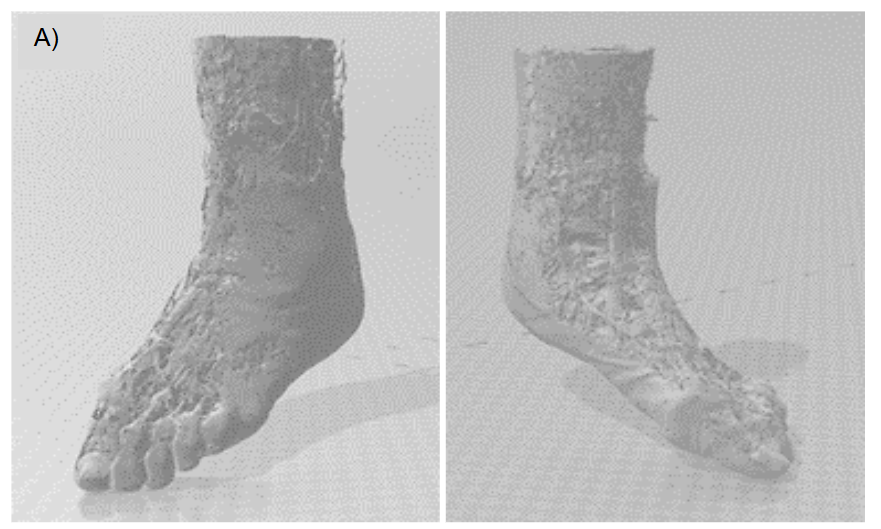
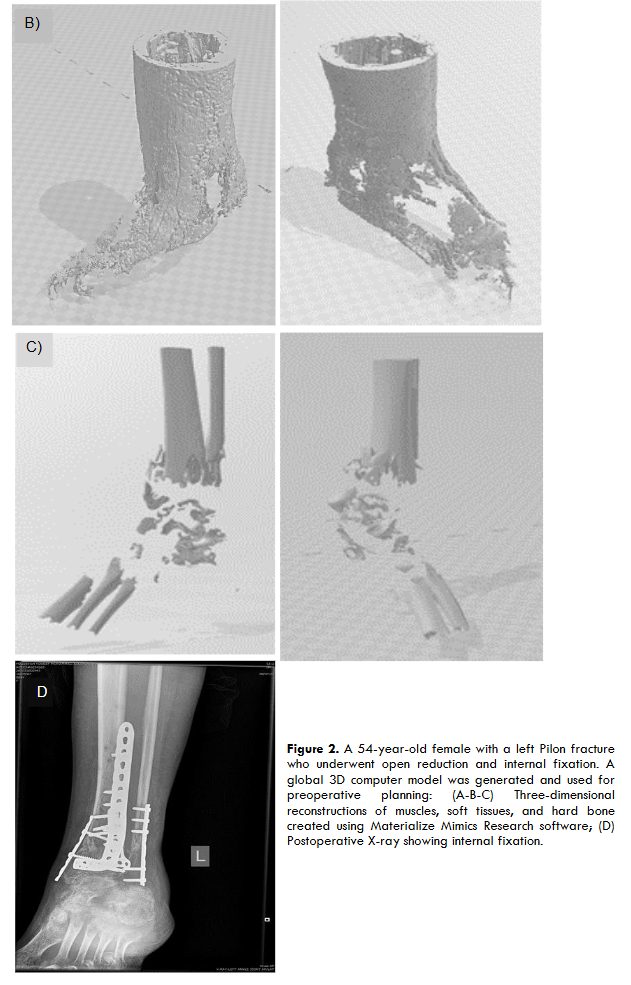
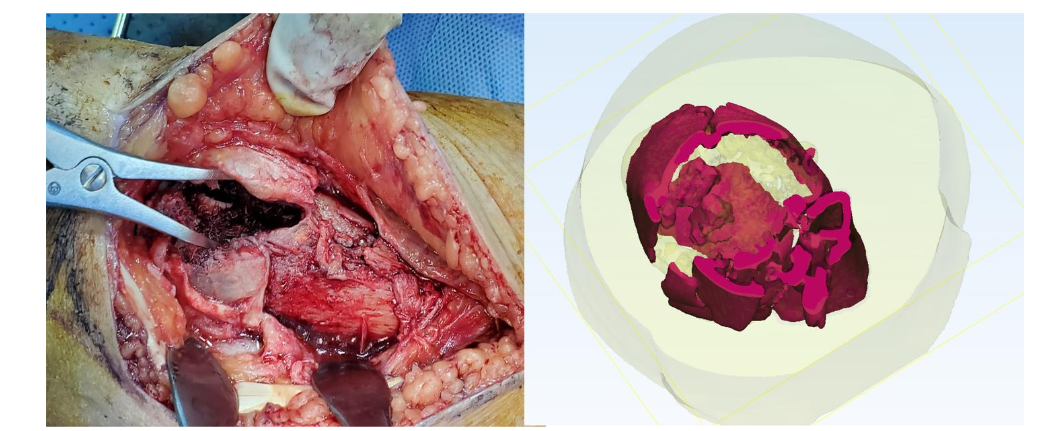
A 3D computer model and prototype were designed, produced, and printed by the authors, and were used for preoperative planning. A see-through 3D 360-degree cross-section of the ankle clearly showed the embedded broken pieces in the region of interest, enabling the surgeon to plan a direct approach for the removal of the broken bone with minimal time required for the procedure.
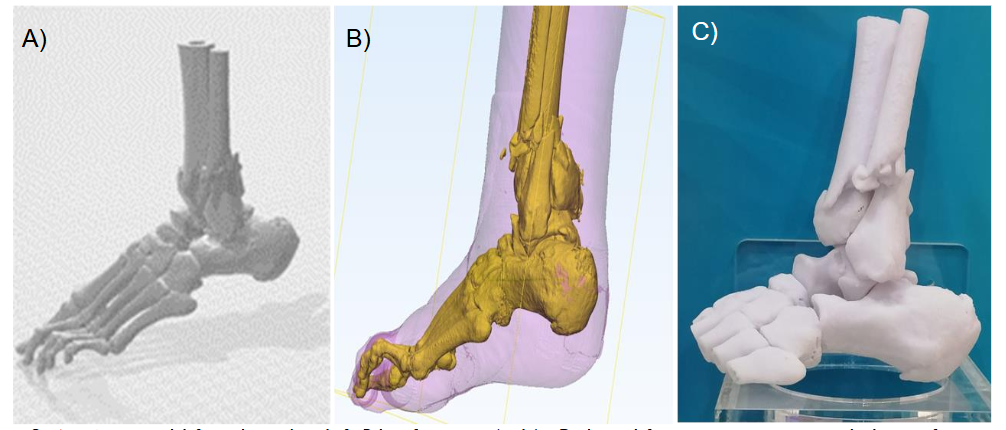
Discussion
The use of advanced software, particularly Materialize Mimics, enabled the authors to generate a highly detailed and accurate 3D model of the ankle from MDCT (Multi-Detector Computed Tomography) scans, which created a comprehensive global view of the fractured bone structure. This 3D model was critical in understanding the complex anatomy of the injury and served as an essential tool for preoperative planning. By transforming traditional 2D imaging into a three-dimensional representation, the model facilitated a more precise evaluation of the fracture’s extent and the surrounding anatomical structures, thus enabling a more informed surgical strategy.
Once the 3D model was generated, it was used to simulate the surgical approach and plan the precise placement of internal fixation devices, including screws and plates. The ability to visualize the fracture in three dimensions significantly enhanced the surgical team’s ability to avoid potential complications, such as screw loosening, misalignment, or malposition of the bone post-fixation. These complications, common in traditional methods, are mitigated by the enhanced precision of 3D modeling, which allows the surgeon to plan for optimal screw positioning and alignment prior to the procedure.
Simulating the reduction and fixation process in a virtual environment also provided surgeons with an opportunity to identify potential challenges before initiating the procedure. This practice of virtual rehearsal enabled the team to anticipate intraoperative obstacles, such as difficulty in accessing the fracture site or complications related to fracture reduction, thereby minimizing unexpected events during the actual surgery. Additionally, the 3D model allowed for more efficient preoperative planning regarding the removal of broken bone fragments, optimizing the surgeon’s approach for minimizing tissue disruption, which contributed to a reduction in operative time.
The use of 3D preoperative planning proved to have a profound impact on the surgical procedure. Several key benefits were observed:
- Enhanced Precision: The ability to visualize complex fracture patterns in 3D allowed the surgical team to place fixation devices with higher accuracy. This precision reduces the likelihood of postoperative complications, such as malalignment or loosening of the hardware, which are common challenges in Pilon fracture repair.
- Faster Decision-Making: The 3D model provided clear insights into the fracture’s geometry, allowing the surgical team to quickly identify potential problem areas, such as areas at risk for non-union or malalignment. This faster identification and decision-making process reduced the time spent troubleshooting during surgery.
- Reduced Risk of Postoperative Issues: The ability to plan and rehearse the surgical approach virtually significantly reduces the risk of intraoperative surprises, ultimately resulting in better alignment and fewer postoperative complications. In this case, the operative time was reduced by 50%, as the surgeons were able to proceed with a clear, practiced plan. This reduction in surgical duration is particularly important as it decreases anesthesia time, which in turn may lower the risk of anesthesia-related complications and improves recovery outcomes.
Postoperatively, the patient showed quicker recovery, with improved alignment and reduced pain compared to traditional approaches, where preoperative planning is often less detailed. The precise planning provided by the Quantitative Colour CT Density Map (QCTDM) and the 3D model allowed for a more controlled and efficient surgery, which contributed to less trauma to surrounding tissues and minimized the need for excessive soft tissue dissection. Studies have shown that such preoperative strategies are associated with a faster recovery period and reduced postoperative complications due to less tissue disruption and more accurate surgical execution.
The advantages of QCTDM and 3D modeling, however, are not without limitations. One of the primary challenges is the reliance on high-quality CT imaging, which can be influenced by technical factors such as resolution, contrast, and artifacts. If the imaging is not of high quality, the resulting 3D model may be incomplete or inaccurate, potentially leading to misinformed surgical decisions. Another limitation is the accessibility and cost of the technology. Both Materialize Mimics software and 3D printing require financial investment in terms of equipment, software licenses, and ongoing maintenance. Furthermore, specialized training is required for both radiologists and surgeons to effectively use and interpret the 3D models.
Finally, while 3D modeling holds significant promise, its application should be considered in the context of the available resources and the clinical needs of the patient. The technology is particularly useful for complex fractures, such as Pilon fractures, where traditional imaging may not provide sufficient information.
Conclusion
The integration of 3D computer modeling and QCTDM into preoperative planning for Pilon fractures represents a significant advancement in orthopedic surgery. By enhancing the precision of fracture reduction and fixation, reducing operative time, and improving postoperative recovery, 3D technology offers significant benefits. The evidence from this case suggests that the use of 3D modeling and printing should be considered a valuable addition to the toolkit of modern orthopedic surgeons.
Informed Consent
Written informed consent was obtained from the patient for publication of this case report.
Conflicts of Interest Statement
The authors have no conflicts of interest to declare.
Funding Statement
The Materialize Mimic Research Software Suit for this study, was obtained by the grant (PR20-13NR-01) from the Kuwait Foundation for the Advancement of Sciences (KFAS).
References
- Gardner MJ, et al. Pilon fractures: A comprehensive review of their treatment. J Orthop Trauma. 2006;20(4):287-293. doi:10.1097/01.bot.0000200131.90735.8d2.
- LernerAJ, et al. Management of pilon fractures: Current concepts. Orthop Clin North Am. 2005;36(4):499-507. doi:10.1016/j.ocl.2005.06.0043.
- Patel S, et al. Impact of 3D modelling on operative time and outcomes in orthopaedic surgeries. Int J Orthop Sci. 2020;9(1):55-62. doi:10.22271/ortho.2020.v9.i1a.17914.
- Sampath S, et al. Preoperative 3D planning and its effect on surgical outcomes in orthopaedics. J Orthop Surg Res. 2014;9(1):1-8. doi:10.1186/s13018-014-0018-2.
- Bruno TM, et al. The role of 3D modeling in orthopaedic preoperative planning. J Bone Joint Surg Am. 2018;100(4):314-320. doi:10.2106/JBJS.17.004476.
- Zhao X, et al. The role of 3D printed models in surgical training and planning: A review of the literature. Orthop J China. 2017;25(3):124-132. doi:10.3969/j.issn.1002-1892.2017.03.0017.
- Hsieh M, et al. Virtual reality in orthopedic surgery: A review of the clinical applications and potential benefits. J Orthopedic Research and Development. 2021;3(2):1-9. doi:10.36959/2573-4916.2021.02.000125.

