Resuscitation Strategies for Trauma Patients Post-Injury
Beyond Damage Control: A Scoping Review Investigating Resuscitation for Trauma Patients in the Post-Hemostatic Period
Carrie L.H. Atcheson, MD, MPH, FASA¹ and R. Christian Skinner, BS¹
ABSTRACT
Background: Quality improvement for the surgical care of trauma patients has focused predominantly on interventions within the first 24 hours after injury and has yielded significant outcomes in recent decades. However, many trauma patients require multiple procedures coordinated with a variety of care providers, and the economic impact of trauma injury care delivery remains underexplored.
Methods: This scoping review aimed to identify the current literature on damage control surgery and damage control resuscitation for trauma patients immediately post-injury.
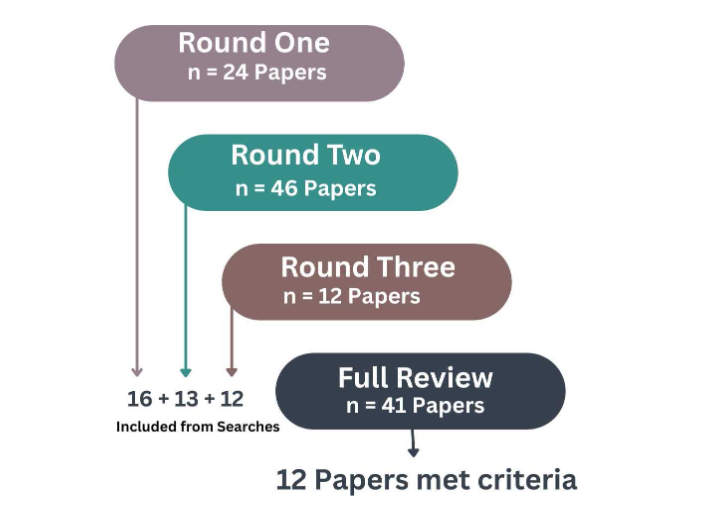
Results: The initial search yielded 24 results. From the final 12 publications, papers were omitted based on their methodological rigor and clinical relevance. The final results were exported to a citation management program (Mendeley by Elsevier Inc., Frisco, CO) and duplicates were removed.
Conclusion: The findings of this review highlight the importance of a multidisciplinary approach to trauma care, emphasizing the need for further research in the post-hemostatic period.
Keywords
trauma, resuscitation, damage control surgery, post-hemostatic period, quality improvement
Background
According to the *figure on page 3*, the extent of trauma injury and the survival of ICU patients is influenced by various factors, including genetics and the nature of the injury.

Going forward, given the volume of surgical patients and the number of practitioners, consultants, and subspecialists providing care during the late resuscitation/early recovery/post-hemostatic period of trauma care, multidisciplinary research teams could draw from: trauma surgeons, trauma anesthesiologists, critical care physicians, advanced practice nurses and nurse anesthetist, ICU nurses, blood management specialists, and social workers. These teams would need to be equipped with the information technology resources needed to integrate clinical information with large databases, ideally with the help of artificial intelligence and machine learning algorithms. And finally, to truly move the needle on reducing the incidence of multiorgan failure among critically ill trauma patients, consensus on a common definition of this high-morbidity syndrome is urgently needed.³⁵,⁴⁸
Conflicts of Interest:
None to Disclose
References
1. Centers for Disease Control. QuickStats: Injury Deaths* as a Percentage of Total Deaths, by Age Group — National Vital. Morbidity and Mortality Weekly Report. 2021;70(31):1066.
https://www.cdc.gov/injury
2. Rossiter ND. “Trauma—the forgotten pandemic?” Int Orthop. 2022;46(1):3-11. doi:10.1007/s00264-021-05213-z
3. Gunst M, Ghaemmaghami V, Gruszecki A, Urban J, Frankel H, Shafi S. Changing Epidemiology of Trauma Deaths Leads to a Bimodal Distribution.
4. Gunst M, Ghaemmaghami V, Gruszecki A, Urban J, Frankel H, Shafi S. Changing Epidemiology of Trauma Deaths Leads to a Bimodal Distribution.
5. Rossaint R, Afshari A, Bouillon B, et al. The European guideline on management of major bleeding and coagulopathy following trauma: sixth edition. Crit Care. 2023;27(1). doi:10.1186/s13054-023-04327-7
6. Committee on Trauma. Advanced Trauma Life Support®, ATLS®. Student Course Manual, 10th Edition.; 2018.
7. Holcomb JB, Tilley BC, Baraniuk S, et al. Transfusion of plasma, platelets, and red blood cells in a 1:1:1 vs a 1:1:2 ratio and mortality in patients with severe trauma: The PROPPR randomized clinical trial. JAMA – Journal of the American Medical Association. 2015;313(5):471-482. doi:10.1001/jam a.2015.12
8. Holcomb JB, Del Junco DJ, Fox EE, et al. The prospective, observational, multicenter, major trauma transfusion (PROMMTT) study: Comparative effectiveness of a time-varying treatment with competing risks. JAMA Surg. 2013;148(2):127-136. doi:10.1001/2013.jamasurg.387
9. Black JA, Pierce VS, Kerby JD, Holcomb JB. The Evolution of Blood Transfusion in the Trauma Patient: Whole Blood Has Come Full Circle. Semin Thromb Hemost. 2020;46(2):215-220. doi:10.1055/s-0039-3402426
10. Dorken-Gallastegi A, Spinella PC, Neal MD, et al. Whole Blood and Blood Component Resuscitation in Trauma. Ann Surg. Published online December 6, 2024. doi:10.1097/sla.0000000000006316
11. Braasch MC, Turco LM, Halimeh B, Wessel E, Winfield RD. FORTRESS: The Fluid and Organ Failure in Trauma Resuscitation Study. American Surgeon. 2023;89(3):462-464. doi:10.1177/000313 4820956936
12. Shakur H, Roberts I, Bautista R, et al. Eff ects of tranexamic acid on death, vascular occlusive events, and blood transfusion in trauma patients with signifi cant haemorrhage (CRASH-2): a randomised, placebo-controlled trial CRASH-2 trial collaborators*. The Lancet. 2010;376:23-32. doi:10.1 016/S0140
13. Guyette FX, Brown JB, Zenati MS, et al. Tranexamic Acid during Prehospital Transport in Patients at Risk for Hemorrhage after Injury: A Double-blind, Placebo-Controlled, Randomized Clinical Trial. JAMA Surg. 2021;156(1):11-20. doi:10.1001/jamasurg.2020.4350
14. Roberts I, Shakur H, Coats T, et al. The CRASH-2 trial: A randomised controlled trial and economic evaluation of the effects of tranexamic acid on death, vascular occlusive events and transfusion requirement in bleeding trauma patients. Health Technol Assess (Rockv). 2013;17(10):1-80. doi:10.331 0/hta17100
15. Imamoto T, Sawano M. Effect of ionized calcium level on short-term prognosis in severe multiple trauma patients: A clinical study. Trauma Surg Acute Care Open. 2023;8(1). doi:10.1136/tsa co-2022-001083
16. Mangnotti LJ, Bradburn EH, Webb DL, et al. Admission ionized calcium levels predict the need for multiple transfusions: a prospective study of 591 critically ill trauma patients. The Journal of Trauma: Injury, Infection, and Critical Care. 2011; 70(2):391-397.
17. Vasudeva M, Mathew JK, Groombridge C, et al. Hypocalcemia in trauma patients: A systematic review. Journal of Trauma and Acute Care Surgery. 2021;90(2):396-402. doi:10.1097/TA.00000000000 03027
18. Beni CE, Arbabi S, Robinson BRH, O’Keefe GE. Acute intensive care unit resuscitation of severely injured trauma patients: Do we need a new strategy? Journal of Trauma and Acute Care Surgery. 2021; 91(6):1010-1017. doi:10.1097/TA.0000000000003373
19. Braasch MC, Turco LM, Cole EM, Brohi K, Winfield RD. The evolution of initial-hemostatic resuscitation and the void of posthemostatic resuscitation. Journal of Trauma and Acute Care Surgery. 2020;89(3):597-601. doi:10.1097/TA.000 0000000002576
20. Callcut RA, Kornblith LZ, Conroy AS, et al. The why and how our trauma patients die: A prospective Multicenter Western Trauma Association study. In: Journal of Trauma and Acute Care Surgery. Vol 86. Lippincott Williams and Wilkins; 2019:864-870. doi:10.1097/TA.0000000000002205
21. Braasch MC, Turco LM, Cole EM, Brohi K, Winfield RD. The evolution of initial-hemostatic resuscitation and the void of posthemostatic resuscitation. Journal of Trauma and Acute Care Surgery. 2020;89(3):597-601. doi:10.1097/TA.000 0000000002576
22. Theusinger OM, Madjdpour C, Spahn DR. Resuscitation and transfusion management in trauma patients: Emerging concepts. Curr Opin Crit Care. 2012;18(6):661-670. doi:10.1097/MCC.0 b013e328357b209
23. Black JA, Pierce VS, Kerby JD, Holcomb JB. The Evolution of Blood Transfusion in the Trauma Patient: Whole Blood Has Come Full Circle. Semin Thromb Hemost. 2020;46(2):215-220. doi:10.1055/s-0039-3402426
24. Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. The BMJ. 2021;372. doi:10.1136/bmj.n71
25. Tobin J, Barras W, Bree S, et al. Joint Trauma System Clinical Practice Guideline: Anesthesia for Trauma Patients.; 2021.
26. Committee on Trauma. Advanced Trauma Life Support®, ATLS®. Student Course Manual, 10th Edition.; 2018.
27. Murphy S, Russell A, Meaders D, et al. Transfusion of Whole Blood Is Not Associated With Increased Rate of Hemolytic Transfusion Reaction. Mil Med. Published online March 19, 2025. doi:10.1093/milmed/usaf080
28. Fröhlich M, Lefering R, Probst C, et al. Epidemiology and risk factors of multiple-organ failure after multiple trauma: An analysis of 31,154 patients from the TraumaRegister. Journal of Trauma and Acute Care Surgery. 2014;76(4):921-927. doi:10.1097/TA.0000000000000199
29. Beni CE, Arbabi S, Robinson BRH, O’Keefe GE. Early Fluid Is Less Fluid: Comparing Early Versus Late ICU Resuscitation in Severely Injured Trauma Patients. Crit Care Explor. 2024;6(7):e1097. doi:10.10 97/CCE.0000000000001097
30. Weykamp MB, Beni CE, Stern KE, et al. Predicting high-intensity resuscitation needs in injured patients in the post-hemostasis phase of care following intervention. Journal of Trauma and Acute Care Surgery. 2024;96(4):611-617. doi:10.109 7/TA.0000000000004156
31. Yakkanti RR, Mohile N V., Cohen-Levy WB, et al. Perioperative management of acetabular and pelvic fractures: evidence-based recommendations. Arch Orthop Trauma Surg. 2023;143(3):1311-1321. doi:10.1007/s00402-021-04278-0
32. Braasch MC, Turco LM, Halimeh B, Wessel E, Winfield RD. FORTRESS: The Fluid and Organ Failure in Trauma Resuscitation Study. American Surgeon. 2023;89(3):462-464. doi:10.1177/000313 4820956936
33. Mullis BH, Mullis LS, Kempton LB, Virkus W, Slaven JE, Bruggers J. Orthopaedic Trauma and Anemia: Conservative versus Liberal Transfusion Strategy: A Prospective Randomized Study. J Orthop Trauma. 2024;38(1):18-24. doi:10.1097/BO T.0000000000002696
34. Tseng CH, Chen TT, Wu MY, Chan MC, Shih MC, Tu YK. Resuscitation fluid types in sepsis, surgical, and trauma patients: a systematic review and sequential network meta-analyses. Crit Care. 2020;24(1). doi:10.1186/s13054-020-03419-y
35. Ting RS, Lewis DP, Yang KX, et al. Incidence of multiple organ failure in adult polytrauma patients: A systematic review and meta-analysis. In: Journal of Trauma and Acute Care Surgery. Vol 94. Lippincott Williams and Wilkins; 2023:725-734. doi:10.1097/T A.0000000000003923
36. Gelbard RB, Griffin RL, Reynolds L, et al. Over-transfusion with blood for suspected hemorrhagic shock is not associated with worse clinical outcomes. Transfusion (Paris). 2022;62(1).
37. Vasu ST, Raheja L, Parmar K, Ramachandran S. Efficacy and Safety Profile of Tranexamic Acid in Traumatic Thoracolumbar Fracture Management: A Systematic Review and Meta-Analysis. Int J Spine Surg. 2022;16(3):567-580. doi:10.14444/8257
38. Roberts DJ, Bobrovitz N, Zygun DA, et al. Evidence for use of damage control surgery and damage control interventions in civilian trauma patients: a systematic review. World Journal of Emergency Surgery. 2021;16(1). doi:10.1186/s13017-021-00352-5
39. Lammers D, Betzold R, McClellan J, et al. Quantifying the benefit of whole blood on mortality in trauma patients requiring emergent laparotomy. Journal of Trauma and Acute Care Surgery. Published online November 1, 2024. doi:10.1097/ta.0000000 000004382
40. Sperry JL, Cotton BA, Luther JF, et al. Whole Blood Resuscitation and Association with Survival in Injured Patients with an Elevated Probability of Mortality. J Am Coll Surg. 2023;237(2):206-219. doi:10.1097/XCS.0000000000000708
41. Gelbard RB, Griffin RL, Reynolds L, et al. Over-transfusion with blood for suspected hemorrhagic shock is not associated with worse clinical outcomes. Transfusion (Paris). 2022;62(1).
42. Jabaley C, Dudaryk R. Fluid Resuscitation for Trauma Patients: Crystalloids Versus Colloids. Curr Anesthesiol Rep. 2014;4(3):216-224. doi:10.1007/s 40140-014-0067-4
43. Martin GS, Bassett P. Crystalloids vs. colloids for fluid resuscitation in the Intensive Care Unit: A systematic review and meta-analysis. J Crit Care. 2019;50:144-154. doi:10.1016/j.jcrc.2018.11.031
44. Goel R, Patel EU, Cushing MM, et al. Association of Perioperative Red Blood Cell Transfusions With Venous Thromboembolism in a North American Registry. JAMA Surg. 2018;153(9): 826-839.
45. Vasu ST, Raheja L, Parmar K, Ramachandran S. Efficacy and Safety Profile of Tranexamic Acid in Traumatic Thoracolumbar Fracture Management: A Systematic Review and Meta-Analysis. Int J Spine Surg. 2022;16(3):567-580. doi:10.14444/8257
46. Beni CE, Arbabi S, Robinson BRH, O’Keefe GE. Acute intensive care unit resuscitation of severely injured trauma patients: Do we need a new strategy? Journal of Trauma and Acute Care Surgery. 2021; 91(6):1010-1017. doi:10.1097/TA.0000000000003373
47. Hutchings L, Watkinson P, Young JD, Willett K. Defining multiple organ failure after major trauma: A comparison of the Denver, Sequential Organ Failure Assessment, and Marshall scoring systems. Journal of Trauma and Acute Care Surgery. 2017; 82(3):534-541. doi:10.1097/TA.0000000000001328
48. Sauaia A, Moore EE, Johnson JL, et al. Temporal trends of postinjury multiple-organ failure: Still resource intensive, morbid, and lethal. Journal of Trauma and Acute Care Surgery. 2014;76(3):582-593. doi:10.1097/TA.0000000000000147

