Intervertebral De-Tethering in Early Onset Scoliosis
Anterior Scoliosis Correction with Intervertebral De-Tethering Releases for the Treatment of Patients 5 to 10 Years of Age
M. Darryl Antonacci, MD¹, Janet Cerrone, PA-C², Anthony Yung, MMSc³, Laury A. Cuddihy, MD⁴, Randal R. Betz, MD⁵
- The Institute for Spine & Scoliosis, Lawrenceville, NJ 08648
- The Institute for Spine & Scoliosis, Lawrenceville, NJ 08648
- Rutgers-Robert Wood Johnson Medical School, New Brunswick, NJ
- The Institute for Spine & Scoliosis, Lawrenceville, NJ 08648
- The Institute for Spine & Scoliosis, Lawrenceville, NJ 08648
OPEN ACCESS
PUBLISHED: 30 December 2024
CITATION: Antonacci, MD., 2024. Anterior Scoliosis Correction with Intervertebral De-Tethering Releases for the Treatment of Patients 5 to 10 Years of Age with Early Onset Scoliosis. Medical Research Archives, [online] 12(12).https://doi.org/10.18103/mra.v12i12.5982
COPYRIGHT: © 2024 European Society of Medicine. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v12i12.5982
ISSN 2375-1924
ABSTRACT
Anterior Scoliosis Correction (ASC) with anterior longitudinal ligament and annular disc complex (intervertebral) de-tethering releases is the authors’ multi-year advancement of their original mini-open vertebral body tethering technique to include a dual screw-line construct and multi-level intervertebral de-tethering releases. The study included patients diagnosed with early onset scoliosis, aged 5-10 years of age, Sanders stage 2 or less, Risser sign of 0, open triradiate cartilages, and a minimum of 2 years of follow-up. Within a database encompassing 840 patients treated by ASC, 15 patients (17 curves) met the inclusion criteria. The average duration of follow-up for this cohort was 48.3 months (range 25 to 86 months). The mean age at the time of surgery was 8.8 years (range 5.7 to 10.1 years). Preoperative scoliosis curves averaged 81° (range 58° to 100°). At the most recent follow-up, the instrumented curves improved to an average of 22° (range -15° to 68°) and mean correction of 75%. Preoperative 3-D kyphosis, calculated as an average of -6° (range -23° to +20°), was improved to an average of +28° (range -1° to +59°) at latest follow-up. As may be anticipated with early onset scoliosis, 11 of the 15 patients underwent a secondary surgical procedure an average of 43 months following the index procedure. Of these 11, lengthening was necessary for overcorrection in 3 patients (20%), revision or subsequent stage ASC was done for additional correction adjustment in 6 patients (40%), and spinal fusion was performed in 2 patients (13%). In conclusion, a cohort of 15 patients aged 5-10 years with early onset scoliosis treated by ASC with intervertebral de-tethering releases (initial average curve of 81°) demonstrated a substantial mean correction of 75% in the instrumented curve. Although 2/15 patients (13%) subsequently underwent posterior spinal fusion, these early outcomes suggest a potential alternative to traditional posterior growing rod system approaches and posterior spinal fusion for these young patients.
Keywords: tethering, vertebral body tethering, anterior scoliosis correction, growth friendly spine surgery, de-tethering
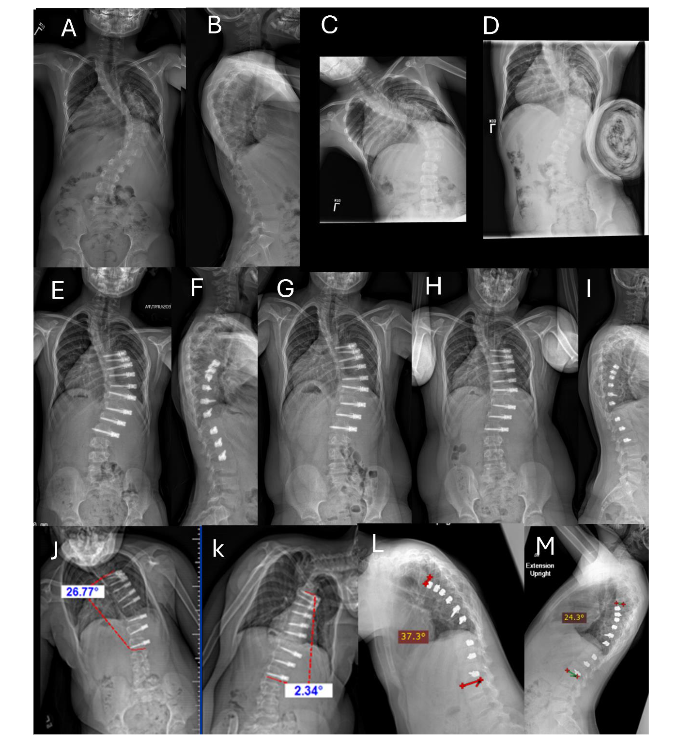
Table 1. Data Summary: 15 Patients (17 Curves) with Early Onset Scoliosis
Patients/% | Average (Range)
Mean age at surgery (years)
8.0 (5.7 to 10.1)
Mean follow-up (months)
48.3 (25 to 86)
Construct of curves (n=17)
Single line construct — 9 (53)
Dual line construct — 8 (47)
Intervertebral De-Tethering Releases
patients — 14/15 (93)
Avg # levels per patient — 3.3 (1 to 7)
Coronal Curve
Maximum | Instrumented
Pre-op (°)
81.1 (58 to 100)
Average flexibility (%)
50.9 (21 to 71)
First erect post-op (°)
33.2 (16 to 66) | 26.9 (6 to 46)
Average correction (%)
57.5 (23 to 78) | 65.9 (47 to 91)
Most recent post-op (°)
30.6 (-38 to 73) | 22.5 (-15 to 68)
Average correction (%)
63.5 (25 to 158) | 74.7 (30 to 123)
2D Sagittal Curve
Pre-op (°)
25.0 (7 to 57)
Most recent (post-op) (°)
35.1 (2 to 55)
3D Sagittal Curve
Pre-op (°)
-5.6 (-23.2 to 19.7)
Most recent (°)
27.6 (-0.8 to 58.6)
3.4 REVISION OR SUBSEQUENT STAGE SURGERY
Within the cohort, 11 of the 15 patients underwent a secondary surgical procedure at an average interval of 43 months (range 23 to 77 months) following the index procedure. Return to the operating room for lengthening due to overcorrection occurred in 3/15 patients (20%). See Figure 2.
3.5 CASE HISTORY FOR FIGURE 2
Example of a unilateral thoracic ASC with intervertebral de-tethering releases needing lengthening for overcorrection at 29 months postoperative. Preoperative PA (A) and lateral (B) radiographs of a 5½-year-old girl with an idiopathic thoracic curve measuring 80°. The patient underwent right T5 to L2 ASC with single screw-line, double cord construct and 5 level intervertebral de-tethering releases (T7–T12). Erect PA (C) and lateral (D) radiographs at 6 weeks postoperative: the instrumented Cobb angle measures 36°. Erect PA (E) at 16 months showing 20° of distal overcorrection from T11 to L2. Right supine bending radiograph (F) at 16 months postoperative shows intra-construct flexibility from 35° to 20° (T5 to T11). Left supine bending radiograph (G) of the lumbar curve at 16 months postoperative shows intra-construct flexibility from minus 20 to minus 10° (T11 to L2). (F) and (G) demonstrate preserved mobility and the ability to delay surgical release of the cord. (H) PA radiograph of the patient in a night brace to delay cord lengthening revision. She refused to wear the brace after 6 months. (I) At 29 months postoperative (pre-revision), the maximum curve measures 35° from T4 to T10 and minus 45° from T10–L12. (J) The left fulcrum bend Cobb angle measures 1° from T11 to L2, demonstrating continued flexibility. Revision involved removal of distal instrumentation in L1–L2 and the addition of all new cords from T4 to L2 and 9 intervertebral de-tethering releases. Specifically, the construct has slack between the screws to allow for growth and curve correction. Most recent PA (K) and lateral (L) radiographs at 6 weeks post revision (30 months after index procedure) measure 27° instrumented curve and 45° maximum curve. The patient is now 8 years old. It is expected she will continue to grow and the curve will continue to correct. However, she still only has a single line construct, and it is possible that construct breakage and loss of correction could occur, requiring another stage of surgery.
Fig. 2A-L. Example of unilateral thoracic ASC with intervertebral de-tethering releases. See Section 3.2 Case History for Figure 2.
Six of 15 patients (40%) required a subsequent stage ASC for additional curve correction. The other two patients (13%) required spinal fusion. One patient with a stiff curve measuring 106° had a fusion for persistent crankshaft. The instrumented curve corrected to 36°, but the curve crankshafted below the L2 instrumentation necessitating a fusion 3.5 years after initial ASC surgery. She had 3.5 years of growth before needing a fusion. The other patient with Prader-Willi syndrome needed a fusion for uncontrolled proximal kyphosis above the instrumented spine as is commonly seen in patients with this syndrome.
Interestingly, there is a trend that the 11 patients who required second surgeries initially had fewer intervertebral de-tethering releases, with an average of 2.5 per patient during the index procedure. In contrast, the 4 who did not require subsequent surgery underwent a higher number of intervertebral de-tethering releases, averaging 5.3 per patient. This trend requires further analysis after longer follow-up.
3.6 MEDICAL COMPLICATIONS
The study identified 3 medical complications in 3 separate patients. One patient with a known preoperative history of a minor temporary encephalopathy experienced a recurrence of encephalopathy postoperatively, which spontaneously resolved within 4 weeks. Another patient developed minor wound dehiscence that did not require surgery, and a third required extended intubation for secretion management. Notably, all patients who encountered these complications had pre-existing syndromes, suggesting a possible link between their underlying syndromic status and postoperative complication risk.
4.0 Discussion
4.1 COMPARATIVE ANALYSIS OF CORONAL RADIOGRAPHIC OUTCOMES AND CLINICAL SUCCESS AGAINST VERTEBRAL BODY TETHERING IN THE EXISTING LITERATURE
We found no other studies of similar aged patients undergoing VBT. The only potential study with which to compare was by Mackey et al.¹⁸ with patients with average age 11.3 years (range 10.9 to 11.8 years) at index surgery. In the Mackey study, VBT resulted in a 41.1% correction of the spinal curvature at final follow-up in a series of 37 patients. The median angle of the major preoperative curves in their cohort was only 50°, which is significantly less than the average preoperative curve angle of 81° found in our cohort. They noted an unplanned revision surgery rate of 16.2%, a figure that is comparatively lower than what was observed in our patients. It is critical to note that our cohort was not only characterized by a greater mean preoperative curve severity but also included much younger patients (by an average of 3 years) who were more skeletally immature (Sanders ≤ 2), both of these factors may contribute to an increased likelihood of a second surgery. Despite these challenges, our cohort of patients undergoing ASC with intervertebral de-tethering releases achieved a notable overall correction rate of 75%, which substantially surpasses the 41.1% correction rate achieved by VBT of Mackey et al.¹⁸
4.2 COMPARATIVE ANALYSIS OF CORONAL RADIOGRAPHIC OUTCOMES AND CLINICAL SUCCESS WITH GROWTH FRIENDLY DISTRACTION-BASED SYSTEM IN THE EXISTING LITERATURE
Historically, distraction-based growth-friendly systems have been the primary approach for managing EOS, yet they are often associated with a higher complication rate and suboptimal curve correction.³¹ Bess et al.¹⁵ reported an overall correction of 49% at an average follow-up of 59.6 months among 140 patients who underwent treatment with traditional growing rods. A recognized limitation of this intervention is the requirement for multiple planned surgeries. Notably, patients in this cohort experienced a 450% rate of return to the operating room (OR) for lengthenings every 4 to 6 months, a factor that is associated with an increased risk of complications. To mitigate this issue, magnetically controlled growing rods (MCGR) were developed to reduce the frequency of surgical lengthening interventions. Mackey et al.¹⁸ observed a significantly reduced
planned return to the OR rate of 31% with the use of MCGR, which is notably lower than that reported in the study of traditional growing rods by Bess et al.¹⁵ However, it is important to highlight that Mackey et al.¹⁸ reported an overall correction of only 34% in patients with EOS treated with MCGR. Overall, both distraction-based systems have substantially lower correction rates observed in comparison to our cohort undergoing ASC with intervertebral de-tethering releases. Additionally, Mackey et al.¹⁸ reported a conversion rate to posterior spinal fusion of 33%, while Bess et al.¹⁵ documented a slightly higher conversion rate of 36%. These rates are considerably higher than the 13% conversion rate observed in our cohort undergoing ASC thus far (see Table 2). However, our patients are still much younger and further from skeletal maturity, and the final outcome is not yet known. Based on how the 13 patients without a fusion are doing at most recent follow-up, we feel our ASC with intervertebral de-tethering releases group will continue to show a lower rate of needing fusion in the future.
Table 2. Comparison of Studies Using Anterior Scoliosis Correction and Distraction-Based Growth-Friendly Systems
| ASC | Bess, et al.¹⁵ Growing Rods | Mackey, et al.¹⁸ MCGR | |
|---|---|---|---|
| No. of patients | 15 | 140 | 51 |
| Age at initial growing rod implantation (years) | 8.0 (5.7–10) | 6.0 (1.7–10) | 9.6 (8.8–10.2) |
| Curve magnitude (°) Initial | 81 (38–106) | 75 (32–147) | 64 (55–75) |
| Curve magnitude (°) Last follow-up | 23 (-10–68) | 47 (4–104) | 42 (34–54) |
| % correction | 74% | 49% | 34% |
| Follow-up (months) | 48.3 (25–86) | 59.6 (24–166) | 34.8 (29–47) |
| Levels per patient | 9 (8–13) | 13 (7–18) | 13 (12–15) |
| Patients with final fusion | 2/15 (13%) | 50/140 (36%) | 17/51 (33%) |
| Return to the OR (N) | 9/15 (60% total) | 633/140 (450%) | 16/51 (31%) |
| Overcorrection | 3/15 (20%) | — | — |
| Loss of correction | 6/15 (40%) | — | — |
Distraction-based growth-friendly systems have shown high complication rates.³⁸,³⁹ The study by Bess et al.¹⁵ indicated an 11% rate of unplanned return to the OR due to infection, compared to a single incident reported by Mackey et al.¹⁸ and none in our ASC cohort. These recurrent OR visits in the context of traditional growing rods with paraspinal muscle disruption may contribute to the increased infection rates, given the multiple surgeries required for rod adjustments during patient growth. Additionally, Bess et al.¹⁵ encountered 4 neurological complications, whereas no such complications were noted in our ASC cohort.
Our data indicate that ASC with intervertebral de-tethering releases provides better coronal curve correction with a comparatively similar rate of radiographic complications but fewer medical complications when compared to existing distraction-based systems. These observations advocate for consideration of ASC with intervertebral de-tethering releases as a possible alternative to growing rod techniques, particularly in children younger than 10 years of age presenting with severe spinal deformities.
5.0 Authors’ Current Recommendations
At this time, subjective recommendations from the authors for consideration of ASC for patients with EOS include: age 5 to 10 years, no preexisting proximal kyphosis, curve size up to 80°, upper end vertebra T4 (preferably T5), maximum number of 10 vertebrae in Cobb angle, and curve flexibility down to 30° and possibly 50° (if willing to do intervertebral de-tethering releases). We recommend correction on the OR table to a Cobb angle of < 30°.
When discussing the procedure with the parents, we acknowledge no long-term data, and we extrapolate the outcomes from our experience with ASC and intervertebral de-tethering releases in patients with AIS. Proposed potential outcomes to parents include the following:
- “One and done” surgery is VERY unlikely; a second and maybe third surgery for overcorrection is possible.
- Anterior subsequent stage surgery for construct loss of curve correction compared to first erect post-op is likely.
- Revision/PSF for inadequate final correction is possible.
- Continued growth and flexibility of their child’s spine is likely.
6.0 Limitations of This Study
The authors recognize several significant limitations within this study, yet emphasize the value of disseminating these findings on EOS patients treated with ASC and intervertebral de-tethering releases given the paucity of existing literature on the subject. The modest cohort size and the data sourcing exclusively from a single primary surgeon (MDA) may limit the statistical power and potentially affect the external validity and generalizability of the results. Nonetheless, this single-surgeon model also ensures a high degree of consistency in surgical techniques and postoperative management. As a retrospective analysis, the study inherently provides a lower level of evidence compared to prospective research designs and is subject to potential biases, including selection, recall, and misclassification biases. Further limitations are evident, such as the absence of patient-reported outcome measures, the lack of a concurrent comparative cohort undergoing treatments with distraction-based systems, and the relatively short follow-up period, which is brief for evaluating a novel surgical technology. These patients absolutely need to be followed through skeletal maturity. In addition, pulmonary function needs to be studied, especially since most patients will probably have more than one surgery to their chest cavity. Spinal height also needs to be studied, but this currently requires sophisticated software for accurate measurement and is not readily available to us. These factors must be considered when interpreting the study’s outcomes and extrapolating the findings to broader clinical practice.
7.0 Conclusion
The study’s assessment of ASC with intervertebral de-tethering releases in a cohort of 15 patients with EOS revealed an average preoperative curve magnitude of 81°. Following ASC with intervertebral de-tethering releases, the mean correction was significant, achieving 75% for the instrumented curve and 64% for the maximum coronal curve, across an average follow-up of 48 months. Of particular note is that only 2 patients (13%) required conversion to posterior spinal fusion. These results suggest that ASC with intervertebral de-tethering releases could be considered a feasible alternative to conventional posterior growing rod techniques for managing severe spinal deformities in patients younger than 10 years. The potential of ASC with intervertebral de-tethering releases to provide substantial curve correction, effective derotation, and lower incidence of surgical fusion underscores its therapeutic promise in the treatment of these challenging patients.
Conflicts of interest:
RRB has received royalties from DePuy Synthes Spine, Globus NuVasive, SpineGuard, and Thieme Medical Publishers; Consulting fees from Globus NuVasive and SpineGuard; and stock options from ApiFix, Orthobond, SpineGuard, and Wishbone Medical. The other coauthors report no conflicts of interest.
2. Jones RS, Kennedy JD, Hasham F, Owen R, Taylor JF. Mechanical inefficiency of the thoracic cage in scoliosis. Thorax. 1981;36 (6):456-461. DOI:10.1136/thx.36.6.456
3. Fernandes P, Weinstein SL. Natural history of early onset scoliosis. J Bone Joint Surg Am. 2007;89(Suppl 1):21-33. DOI: 10.2106/JBJS.F.00754
4. Winter RB, Moe JH. The results of spinal arthrodesis for congenital spinal deformity in patients younger than five years old. J Bone Joint Surg Am. 1982;64(3):419-432.
5. Campbell Jr RM, Hell-Vocke AK. Growth of the thoracic spine in congenital scoliosis after expansion thoracoplasty. J Bone Joint Surg Am 2003;85(3): 409-420. DOI: 10.2106/00004623-200303000-00002
6. Karol LA, Johnston C, Mladenov K, Schochet P, Walters P, Browne RH. Pulmonary function following early thoracic fusion in non-neuromuscular scoliosis. J Bone Joint Surg Am. 2008:90(6):1272-1281. DOI: 10.2106/JBJS.G.00184
7. Vitale MG, Matsumoto H, Bye MR, Gomez JA, Booker WA, Hyman JE, Roye Jr DP. A retrospective cohort study of pulmonary function, radiographic measures, and quality of life in children with congenital scoliosis: an evaluation of patient outcomes after early spinal fusion. Spine (Phila Pa 1976). 2008; 33(11):1242-1249.
DOI: 10.1097/BRS.0b013e3181714536
8. Danielsson AJ, Nachemson AL. Back pain and function 22 years after brace treatment for adolescent idiopathic scoliosis: a case-control study—part I. Spine (Phila Pa 1976). 2003;28(18):2078-2085. DOI: 10.1097/01.BRS.0000084268.77805.6F
9. Green DW, Lawhorne 3rd TW, Widmann RF, Kepler CK, Ahern C, Mintz DN, Rawlins BA, Burke SW, Boachie-Adjei O. Long-term magnetic resonance imaging follow-up demonstrates minimal transitional level lumbar disc degeneration after posterior spine fusion for adolescent idiopathic scoliosis. Spine (Phila Pa 1976). 2011;36(23):1948-1954. DOI: 10.1097/BRS.0b013e3181ff1ea9
10. Hsu PC, Feng CK, Huang SH. Chiu JW, Chou CL, Yang TF. Health-related quality of life in children and adolescent with different types of scoliosis: a cross-sectional study. J Chin Med Assoc. 2019;82(2):161-166.
DOI: 10.1097/JCMA.0000000000000020
11. Kepler CK, Meredith DS, Green DW, Widmann RF. Long-term outcomes after posterior spine fusion for adolescent idiopathic scoliosis. Curr Opin Pediatr. 2012;24(1):68-75. DOI: 10.1097/MOP.0b013e32834ec982
12. Lykissas MG, Jain VV, Nathan ST, Pawar V, Eismann EA, Sturm PF, Crawford AH. Mid- to long-term outcomes in adolescent idiopathic scoliosis after instrumented posterior spinal fusion: a meta-analysis. Spine (Phila Pa 1976). 2013;38(2):E113-119. DOI 10.1097/BRS.0b013e31827ae3d0
13. Motoyama EK, Yang CI, Deeney VF. Thoracic malformation with early-onset scoliosis: effect of serial VEPTR expansion thoracoplasty on lung growth and function in children. Paediatr Respir Rev. 2009;10(1):12-17.
DOI: 10.1016/j.prrv.2008.10.004
14. Skaggs DL, Akbarnia BA, Flynn JM, Myung KS, Sponseller PD, Vitale MG, Chest Wall and Spine Deformity Study Group, Growing Spine Study Group. A classification of growth friendly spine implants. J Pediatr Orthop. 2014;34(3):260-274. DOI: 10.1097/BPO.0000000000000073
15. Bess S, Akbarnia BA, Thompson GH, Sponseller PD, Shah SA, El Sebaie H, Boachie-Adjei O, Karlin LI, Canale S, Poe-Kochert C, Skaggs DL. Complications of growing-rod treatment for early-onset scoliosis: analysis of one hundred and forty patients. J Bone Joint Surg Am. 2010;92(15): 2533-2543. DOI 10.2106/jbjs.i.01471
16. Agarwal A, Kelkar A, Agarwal AG, Jayaswal D, Jayaswal A, Shendge V. Device-related complications associated with Magec Rod usage for distraction-based correction of scoliosis. Spine Surg Relat Res. 2019;4(2):148-151.
DOI: 10.22603/ssrr.2019-0041
17. Thakar C, Kieser DC, Mardare M, Haleem S, Fairbank J, Nnadi C. Systematic review of the complications associated with magnetically controlled growing rods for the treatment of early onset scoliosis. Eur Spine J. 2018;27(9):2062-2071. DOI:10.1007/s00586-018-5590-4
18. Mackey C, Hanstein R, Lo Y, Vaughan M, St. Hilaire T, Luhmann SJ, Vitale MG, Glotzbecker MP, Samdani A, Parent S, Gomez JA, Pediatric Spine Study Group. Magnetically controlled growing rods (MCGR) versus single posterior spinal fusion (PSF) versus vertebral body tether (VBT) in older early onset scoliosis (EOS) patients: how do early outcomes compare? Spine (Phila Pa 1976), 2022;47(4):295-302. DOI: 10.1097/BRS.0000000000004245
19. Stokes IA, Spence H, Aronsson DD, Kilmer N. Mechanical modulation of vertebral body growth. Implications for scoliosis progression. Spine (Phila Pa 1976), 1996;21(10):1162-1167.
DOI: 10.1097/00007632-199605150-00007
20. Mehlman CT, Araghi A, Roy DR. Hyphenated history: the Hueter-Volkmann law. Am J Orthop (Belle Mead NJ). 1997;26(11):798-800.
21. Baroncini A, Courvoisier A. The different applications of vertebral body tethering – narrative review and clinical experience. J Orthop. 2023; 37:86-92. DOI: 10.1016/j.jor.2023.02.012
22. Cuddihy L, Swiercz M, Antonacci C, Betz R, Antonacci M (2021) Predicting the major coronal curve angle on initial standing x-rays based on intraoperative correction during anterior scoliosis correction and vertebral body tethering: comparison of single vs. double cord/screw constructs. 28th International Meeting on Advanced Spine Techniques (virtual), April 23-25, 2021.
23. Cuddihy LA, Antonacci MD, Vig KS, Hussain AK, Levin D, Betz RR. Progressive double major scoliotic curve with concurrent lumbosacral spondylolisthesis in a skeletally immature patient with Marfan syndrome treated with anterior scoliosis correction. Spine Deform. 2020;8(1):139-146. DOI: 10.1007/s43390-020-00031-6
24. Cuddihy LA, Antonacci MD, Hussain AK, Vig KS, Mulcahey MJ, Betz RR. Progressive neuromuscular scoliosis secondary to spinal cord injury in a young patient treated with nonfusion anterior scoliosis correction. Top Spinal Cord Inj Rehabil. 2019;25(2):150-156. DOI: 10.1310/sci2502-150
25. Betz RR, Antonacci MD, Cuddihy LA. Alternatives to spinal fusion surgery in pediatric deformity. Curr Orthop Pract. 2018:29(5):430-435
26. Antonacci MD, Yung A, Kozicz A, Cerrone J, Antonacci CL, Verma Y, Sweeney M, Cuddihy LA, Betz RR. Double screw-line technique of anterior scoliosis correction with thoracic disc releases for thoracic curves > 65 degrees: surgical techniques and outcomes. Med Res Arch J. 2023;11(7.1). DOI: 10.18103/mra.v11i7.1.4095
27. Antonacci CL, Antonacci MD, Bassett WP, Cerrone JL, Haas AR, Haoson DS, Cuddihy LA, Betz RR. Treatment of patients with scoliosis using a unique anterior scoliosis correction technique. Med Res Arch J. 2021;9(7).
DOI: 10.18103/mra.v4i7.2463
28. Trobisch P, Mahoney JM, Eichenlaub EK, Antonacci CL, Cuddiny L, Amin DB, Razo-Castaneda D, Orbach MR, McGuckin JP, Bucklen BS, Antonacci MD, Betz RR. An investigation of range of motion preservation in fusionless anterior double screw and cord constructs for scoliosis correction. Eur Spine J. 2023;32(4):1173-1186. DOI: 10.1007/s00586-023-07608-5
29. Parvaresh KC, Osborn EJ, Reighard FG, Doan J, Bastrom TP, Newton PO. Predicting 3D thoracic kyphosis using traditional 2D radiographic measurements in adolescent idiopathic scoliosis. Spine Deform. 2017;5(3):159-165. DOI: 10.1016/j.jspd.2016.12.002
30. Newton PO, Bartley CE, Bastrom TP, Kluck DG, Saito W, Yaszay B. Anterior spinal growth modulation in skeletally immature patients with idiopathic scoliosis: a comparison with posterior spinal fusion at 2 to 5 years postoperatively. J Bone Joint Surg Am. 2020;102(9):769-777. DOI: 10.2106/JBJS.19.01176
31. Ellinger F, Tropp H, Gerdhem P, Hallgren HB, Ivars K. Magnetically controlled growing rod treatment for early-onset scoliosis: analysis of 52 consecutive cases demonstrates improvement of coronal deformity. J Spine Surg. 2023;9(3):259-268. DOI: 10.21037;jss-22-70
32. Urbański W, Tucker S, Ember T, Nadarajah R. Single vs dual rod constructs in early onset scoliosis treated with magnetically controlled growing rods. Adv Clin Exp Med. 2020;29(10):1169-1174. DOI: 10.17218/acem/126289
33. Acaroglu E, Yazici M, Alanay A, Surat A. Three-dimensional evolution of scoliotic curve during instrumentation without fusion in young children. J Pediatr Orthop. 2002;22(4):492-496
34. Klemme WR, Denis F, Winter RB, Lonstein JW, Koop SE. Spinal instrumentation without fusion for progressive scoliosis in young children. J Pediatr Orthop. 1997;17:734-742
35. Moe JH, Kharrat K, Winter RB, Cummine JL. Harrington instrumentation without fusion plus external orthotic support for the treatment of difficult curvature problems in young children. Clin Orthop Relat Res. 1984;185:35-45
36. Harrington PR. Treatment of scoliosis. Correction and internal fixation by spine instrumentation. J Bone Joint Surg Am. 1962;44: 591-610

