Impact of Adult ADHD on Relationship Quality
Relationship difficulties: compounding effects of Adult Attention-Deficit/Hyperactivity Disorder (ADHD)
Anh-Luu Huynh-Hohnbaum, Ph.D., MSW¹ and S. M. Benowitz², MSW*
- Department of Social Work,
California State University, Los Angeles, Los Angeles, California, USA;
*Pacific Clinics
*Corr. author:
[email protected]
OPEN ACCESS
PUBLISHED: 28 February 2026
CITATION: Huynh-Hohnbaum, A.L. and Benowitz, S.M., 2026. Relationship difficulties: compounding effects of Adult Attention-Deficit/Hyperactivity Disorder (ADHD). Medical Research Archives, [online] 14(2).
COPYRIGHT: © 2026 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
ISSN 2375-1924
ABSTRACT
Once thought solely a childhood disorder, research on adult Attention-Deficit/Hyperactivity Disorder (ADHD) has become more prevalent since the condition’s recognition in the 1990s. However, information remains scarce about if and how it impacts functionality in relationships. Adults with Attention-Deficit/Hyperactivity Disorder can experience interpersonal relationship difficulties due to the disorder’s signature symptoms of hyperactivity, impulsivity, and inattentiveness, as well as due to their oft-observed dimension of emotional lability. Adults with Attention-Deficit/Hyperactivity Disorder tend to have more trouble navigating romantic relationships and are more likely to be divorced than adults without Attention-Deficit/Hyperactivity Disorder. The purpose of this paper is to perform a systematic literature review of empirically-based studies of integrative couples therapy wherein at least one partner struggles with adult Attention-Deficit/Hyperactivity Disorder. Future research, gaps in the literature, and practice implications also are discussed, including hope for focus on the positive aspects of ADHD for individuals and partnerships.
Keywords:
adult; attention deficit hyperactivity disorder; ADHD; relationship; couples therapy
Introduction
Although attention deficit hyperactivity disorder (ADHD) was regarded until the end of the 20th century to be only a childhood disorder, a growing body of research has found adult manifestations. Evidence suggests higher likelihood for childhood onset; however, differences in symptom expression e.g., by gender and age complicate timely diagnosis (Katzman et al., 2017; Posner et al., 2020). While in childhood the condition tends to present only with varying levels of its signature symptoms of inattention, impulsivity, and hyperactivity, adulthood hyperactivity usually resembles restlessness; also, adult ADHD tends to present with comorbidities e.g., obesity, insomnia, mood disorders, and addictive behaviours each with functional impairments (Katzman et al., 2017; Posner et al., 2020). Adult ADHD is associated with costs across domains including education, employment, and health; for example, health problems (such as obesity), substance use disorders, and mood disorders resulted in higher medical insurance claims for adults with ADHD versus without (Libutzki et al., 2019).
Meta-analyses of international research have found adult ADHD to extend into 57% of adults from childhood (Fayyad, 2017) and only 9.1% of young adults diagnosed w/ADHD as children showed sustained remission of symptoms 16 years after childhood diagnosis (Sibley, 2021), making it one of the most common mental health disorders in adulthood (Fayyad et al., 2017; Kessler et al., 2005; Posner et al., 2020). In fact, the CDC has recently identified adult ADHD as a public health issue, in addition to a mental health issue due to the lack of research and misinformation regarding adult ADHD (National Academies of Sciences, Engineering, and Medicine, 2024).
Attention-Deficit/Hyperactivity Disorder during adulthood can wreak havoc on personal relationships, particularly intimate ones. Partners with ADHD are more likely to be forgetful, disorganized, and distracted due to deficits in executive functioning, poor attention, and lack of impulse control, which can lead the other partner to feel frustrated and increase the likelihood that a marriage will fail (Hankin, 2001; Robin & Payson, 2002). Moreover, not only are individuals with mental health problems more likely to develop depressive, anxiety, and substance use disorders when there is conflict in their romantic relationships (Whisman & Baucom, 2012), couples where a partner has ADHD are more likely to suffer from anxiety, stress, and depression compared to couples without ADHD present (Ghahramanzadeh et al., 2021). The purpose of this paper is to perform a systematic review of the literature on empirically-based studies of integrative therapy to treat couples wherein at least one partner struggles with adult ADHD.
Effects of Adult ADHD on Intimate Relationships
DIVORCE
The presence of ADHD in at least one partner can contribute to intimate relationship problems. Adults with ADHD reported less satisfaction in, and more trouble navigating, romantic relationships, and were more likely to be divorced than adults without ADHD (Katzman et al., 2017; Klein et al., 2012; Michielsen et al., 2013; Wymbs et al., 2021). In a longitudinal study, adults diagnosed during childhood with ADHD were three times likelier to be divorced than adults in a comparison group (Klein et al., 2012), much as was the case in a study wherein the likelihood of lifetime singlehood or history of divorce among older adults with ADHD was three times higher than among those without the disorder (Michielsen et al., 2013).
LESS INTIMACY
Exploration into the effects of adult ADHD on intimate partnerships has revealed associations between ADHD symptoms and certain relationship elements. Spouses of partners with ADHD reported lower intimacy and less satisfaction in their marriages than spouses of non-ADHD partners (Ben-Naim et al., 2017). Severity of ADHD symptoms among college students was positively correlated with fear of intimacy, particularly in the context of reflection about past intimacy problems, and also positively correlated with cynicism about the possibility of ever being close with a partner; however, fear of intimacy was not associated with lowered self-assessment of relationship competence (e.g., communication skills, romantic appeal) the latter result, researchers noted, corresponded with research showing positive illusory bias in self-assessment among children with ADHD (Marsh et al., 2015). Also, increased ADHD symptomology, though linked with fear of intimacy, was nonetheless associated with risky sexual behavior (Marsh et al., 2015).
LACK OF EMPATHY AND AWARENESS
Attention-Deficit/Hyperactivity Disorder’s effect on empathy revealed deficits that would presume to hinder intimate relationships. A literature review cited a body of research demonstrating deficits in facial and vocal emotion recognition as well as in cognitive empathy among adults with ADHD (Bora & Pantelis, 2015). Roy et al. (2013) found that, in a sample of adults with ADHD, 15% were found to be on the autism spectrum (associated with deficits in emotional and cognitive empathy), versus 0.06% in the general population.
Of note is that researchers observed positive illusory bias in self-assessment of relationship skill by adults with ADHD, who rated themselves as more competent than was observed by their partners, friends, or family members; moreover, increased discrepancy between self-assessment and observed assessment of symptom severity predicted increased positive illusory bias (Jiang & Johnston, 2011). Similarly, Marsh et al. (2012) found that increased symptom severity was not associated with decreased self-assessment of relationship skills.
IMPULSIVITY
Other symptomalogical dimensions of adult ADHD have revealed assorted intimate relationship outcomes. Adults with primary hyperactivity symptoms of ADHD were more likely than those with primarily impulsivity or inattention symptoms to report divorce or dissatisfaction in their intimate relationships (Das et al., 2012 and Moyá et al., 2012, respectively). Canu et al. (2014) found that symptoms of impulsivity and hyperactivity combined with inattention (that is, the symptoms of the combined type of adult ADHD) were more likely to be associated with low conflict resolution and less relationship satisfaction than symptoms of the inattentive type or than absence of ADHD symptoms. College students with self-reported symptoms of combined type of ADHD reported lower romantic relationship quality than did students without ADHD symptoms (Bruner et al., 2015). Interestingly, among young adults, hyperactive/impulsive symptoms predicted past fear of intimacy, while inattentive symptoms predicted current pessimism about intimacy (Marsh et al., 2015). Both genders with combined-type ADHD tended to report lower relationship quality than did subjects with no ADHD symptoms; only for females, each type of ADHD symptom independently predicted lower reported relationship quality, mediated in each case by emotional dysregulation and hostile conflict (Bruner et al., 2015).
INTIMATE PARTNER VIOLENCE
Symptoms of ADHD have been associated with intimate partner violence (IPV), anger, hostile conflict, and low conflict resolution. Adult ADHD symptoms were risk factors for IPV among a sample of adults without other IPV risk factors (e.g., childhood maltreatment or substance use) (Wymbs et al., 2016). Romero-Martinez et al. (2018) identified adult ADHD’s impulsiveness and inattentiveness to be related to risk of IPV, especially regarding difficulties decoding facial expression and exercising cognitive flexibility, but a study examining links between adult ADHD and community violence found an association between IPV and hyperactivity (Gonzalez et al., 2013). Gonzalez et al. (2013), looking at associations between adult ADHD and violent behavior in the community, also found that severe and repetitive acts of violence, including against intimate partners, were linked with severe ADHD symptoms. Emotional lability was present among ADHD-affected adults without comorbidities, and anger was the emotion most related to antisocial behavior (Skirrow & Asherson, 2013). Likewise, Bruner et al. (2015) found that emotion dysregulation and hostile conflict mediated reports of low relationship quality among women with ADHD; and Canu et al. (2014) found low conflict resolution associated with reported dissatisfaction in relationship quality among couples where one partner had ADHD.
PARENTING DEFICITS
Johnston et al. (2012) posit that, parents with ADHD, due to deficits in their behavioral and emotional control, may introduce a chaotic environment, ineffective problem-solving, insubstantial child monitoring, and erratic or over-reactive discipline. In a parent training program, adults with ADHD were more likely than those without ADHD to go off-task or break rules while interacting with their children (Babinski et al., 2015). Parents with the impulsive/hyperactive type (versus the inattentive type) of ADHD tended to overestimate their competence in parenting compared to their observed competence – which, researchers noted, aligns with previous studies finding positive illusory bias in self-assessment by children with ADHD (Lui et al., 2013). Pharmacotherapy for adults with ADHD gradually resulted in less negative talk, fewer commands, and increased praise toward their children, yielding their children’s corresponding reduced negative behavior (Waxmonsky et al., 2014). These difficulties with parenting also stress the marriage and increase the likelihood for discord (Hankin, 2001).
Methodology
LITERATURE SEARCH STRATEGY
The methodology is based on Xiao & Watson’s (2019) guide for conducting systematic literature reviews. In June 2022, we performed a systematic search by using the following key words and search terms: adult adhd and couples therapy in the following three electronic databases: EbscoHost, PsycInfo, and OneSearch. In order to broaden the search, there were no time limits on the publication dates. For each article, preliminary relevance was determined by title and abstract. If the abstract discussed methodology, we obtained the full article for evaluation. Both researchers performed independent assessments of the manuscripts and any discrepancies were discussed and resolved.
INCLUSION AND EXCLUSION FACTORS
Studies were considered for inclusion if they met the following criteria: 1) participants age 18 and older; 2) one of the participants met the criteria for DSM-111-R, DSM-IV, or DSM-5 ADHD; 3) couples therapy wherein both individuals were present; 4) one of the goals of treatment was to reduce ADHD symptoms and thereby improve relationship quality; and 5) outcomes were measured at pre- and (at a minimum) post-treatment. Studies that were not empirically evaluating an intervention or were not peer-reviewed were excluded; this included book chapters, book reviews, single case studies, editorials, and conference abstracts/reports.
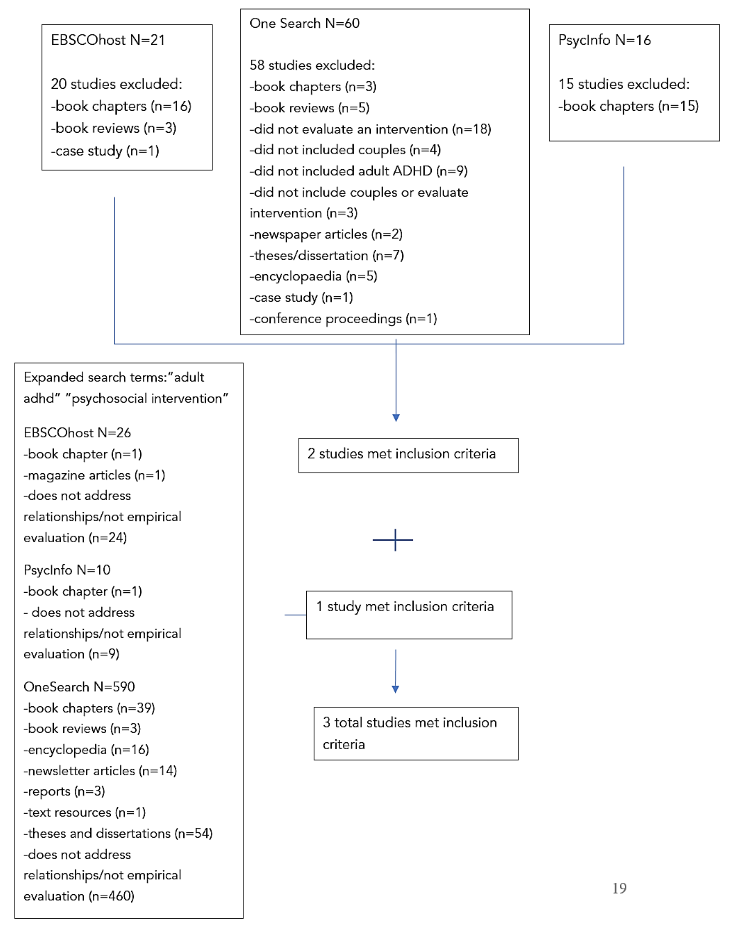
After doing the search, only two articles met the criteria. In order to expand the search, the authors included the following search terms: adult adhd and psychosocial intervention in the same three electronic databases: EbscoHost, PsycInfo, and OneSearch. Similar to the above search, there were no time restrictions.
For both searches, after reviewing the abstract for the predefined inclusion and exclusion criteria, we obtained the study for full-text screening. After combing through 626 results with the same inclusion and exclusion factors, one more study was found for a total of three articles (See Figure 1). These findings are consistent with Wymbs et al.’s (2021) finding that there is very limited empirical study of couples therapy for ADHD. Once the full-text article was obtained, the following information was extracted: research goal, study design, sample, study inclusion and exclusion factors, number of intervention sessions, outcomes, intervention modality, post-intervention outcomes, and any follow up outcomes.
Results
In sum, a total of three articles met the criteria of examining integrative couples therapy to improve relationship quality via traditional couples therapy approaches combined with interventions to reduce ADHD symptoms. Table 1 provides an overview of the included studies.
| Authors (Year) | Aim | Design / Sample | I/E Criteria | Sessions | Intervention | Measures | Key Outcomes |
|---|---|---|---|---|---|---|---|
| Buitelaar et al. (2019) | Examine whether ↓ ADHD symptoms associated with ↓ IPV frequency in offenders with ADHD | Longitudinal; N=209 male & female IPV offenders in forensic psychiatry; 4 follow-ups (8, 16, 24, 52 weeks) | (I) ADHD dx; 18 yrs; Dutch literacy; IPV within 8 wks pre-intake (E) Unable to complete ADHD-RS | Variable (risk-adjusted); 4 checkpoints over 1 yr | TAU for IPV + solution-focused or emotionally focused couples therapy (if indicated); ADHD psychoeducation + coaching; optional pharmacotherapy | Baseline: DIVA 2.0 (clinician). Outcomes: ADHD-RS (self-report), CTS2 (IPV self-report), MOAS (clinician-rated IPV), med compliance, session attendance | Significant ↓ in ADHD symptoms and IPV outcomes ↓ IPV primarily associated with ↓ ADHD symptoms |
| Hirvikoski et al. (2017) | Test feasibility, efficacy, effectiveness of PEGASUS psychoeducation for adults w/ ADHD & partners | Pragmatic multicenter RCT; N=179; TAU+PEGASUS (n=97) vs TAU only (n=82) | (I) Primary ADHD dx; 18 yrs; 1 adult significant other (E) SUD; IQ<70; ASD; psychosis; suicidality; severe psychosocial instability | 8 weekly group sessions (10-15 adults + partners) | Manualized psychoeducation (ADHD knowledge, support, self-management); multidisciplinary facilitators; partners included | Primary: ADHD knowledge (ADHD-20). Secondary: SWLS; HADS; relationship quality (QAFM); burden (BAS); self-esteem (RSES) | ↑ ADHD knowledge & life satisfaction No overall change in relationship quality ↓ partner criticism & burden ↑ self-esteem (ADHD adults) |
| Wymbs & Molina (2015) | Evaluate feasibility & acceptability of CBT + couples therapy group | Pilot open trial; non-randomized; N=15 couples (1 partner with elevated ADHD symptoms) | (I) 18-35 yrs; 6 mo relationship; elevated ADHD (ASRS); stable medication (E) Children | 6 weekly 1.5-hr sessions | CBT for adult ADHD + Relationship Distress Prevention Program | ASRS (self & partner); Treatment Satisfaction; Positive & Negative Relationship Quality Scale; Relationship Impact Checklist | No dropouts (high feasibility) Zero medium ADHD symptom improvement (gender differences) ↓ relationship negativity Small positive effects on conflict behaviors |
One of the studies was conducted in the United States (Pennsylvania) Wymbs and Molina, 2015) and two were international: one was in Sweden (Hirvikoski et al., 2017) and one was in the Netherlands (Buitelaar et al., 2019). Two studies were in psychiatric outpatient settings, while Wymbs and Molina (2015) recruited participants via flyers posted at bus stops and on Craigslist.com. Per the inclusion criteria, all studies included both the adult with ADHD and at least one partner. Wymbs and Molina (2015) had the smallest sample size with 15 couples, whereas the other two had 179 and 209 couples, respectively (Buitelaar et al., 2019; Hirvikoski et al., 2017). Buitelaar et al.’s (2019) participants were from a forensic psychiatric setting, and one of their requirements, in addition to adult ADHD, was that subjects had a history of IPV offending within the eight weeks prior to intake.
INTERVENTIONS
All three interventions were a form of integrative couples therapy to improve relationship quality via traditional couples therapy approaches combined with psychoeducation about ADHD. Wymbs and Molina (2015) combined evidence-based couples therapy with CBT for ADHD. Each week, core components of CBT for adult ADHD were integrated with an evidence-based relationship distress prevention program (see Markman et al., 2004). CBT for ADHD included psychoeducation; relationship-building skills practice; learning to distinguish, accept, and tolerate unchangeable ADHD-related behaviors; and reframing of differences as potential relationship strengths. Hirvikoski et al.’s (2017) intervention provided information about available support and treatment strategies for optional ADHD self-management to both the participant with ADHD and their significant others. Buitelaar et al. (2019) combined solution-focused or emotionally-focused couples therapy with IPV treatment, which included safety planning and enhanced communication skills. These interventions were also combined with ADHD psychoeducation for participants and their partners, with coaching for ADHD-related problems, if necessary. Additionally, participants with ADHD were offered ADHD pharmacotherapy.
Both Wymbs and Molina (2015) and Hirvikoski et al. (2017) held weekly sessions, whereas Buitelaar et al. (2019) provided a varying number of sessions, adjusted based on risk of recidivism over the course of the year, with four checkpoints throughout the year. Buitelaar et al. (2019) was the only study that included multiple timepoints. With respect to assignment of treatment, Hirvikoski et al. (2017) was the only study that used a control group: participants were randomly assigned to receive the 8-session psychoeducational treatment (PEGASUS) or the TAU, which was standard clinical services, including pharmacological and non-pharmacological interventions.
MEASUREMENTS
All three studies aimed at a decrease in ADHD symptoms and an increase in relationship satisfaction. Hirvikoski et al. (2017) measured ADHD knowledge for both the adult with ADHD and their significant others, and Buitelaar et al. (2019) and Wymbs and Molina (2015) measured symptom management by self and by partner. Regarding relationship outcomes, Buitelaar et al. (2019) looked specifically at a reduction in IPV through the self-reported Conflicts Tactic Scale 2 and clinician-rated Modified Overt Aggression Scale.
OUTCOMES OF INTERVENTIONS
Overall, findings supported the effectiveness of the interventions. Participants with ADHD reported less ADHD symptoms after treatment (Buitelaar et al., 2019), specifically inattention and hyperactivity/impulsivity (Wymbs and Molina, 2015); and participants with ADHD and their partners showed increased knowledge about ADHD, such as living with ADHD, ADHD in relationships, and structure and strategies in everyday life (Hirvikoski et al., 2017). With respect to the quality of relationships, couples reported reduced relationship negativity and fewer conflict-inducing behaviors (Wymbs and Molina, 2015) and all IPV outcomes were favorable, including reduction in minor and severe acts of aggression and observed overt aggression (Buitelaar et al., 2019). While Hirvikoski et al. (2017) did not find a change in general relationship quality, they did find that non-ADHD partners expressed fewer critical remarks to their partners with ADHD and reported decreased burden of care. Wymbs and Molina (2015) found that while participants with ADHD self-reported no effect of treatment on their conflict-inducing behaviors (e.g. doesn’t respond when spoken to, pays bills late, doesn’t remember being told things, takes out frustrations on me), their non-ADHD partners did find a small effect. Both studies findings (Hirvikoski et al., 2017; Wymbs & Molina, 2015) underscore the importance of including significant others in ADHD treatment to help corroborate assessments of ADHD symptom improvement.
Discussion
This literature review reveals a dearth of empirical research into integrative interventions for couples wherein at least one partner has adult ADHD – in fact, we only found three such studies. This gap in research is corroborated by Wymbs et al. (2021), who found only one empirical study (Wymbs & Molina, 2015 one of the three articles we examine in this paper) that evaluated treatment of adult ADHD in the context of couples therapy. Meanwhile, a body of non-empirical popular literature has ventured to fill the gap (e.g., Married to Distraction, co-authored in 2010 by psychiatrist Ned Hallowell, himself diagnosed with adult ADHD, and his wife, Sue Hallowell, a couples therapist). While adult intimate relationships was not the main focus on their paper, Cortese et al. (2025) stated that core ADHD adult symptoms that may impact relationships included starting relationships quickly, not being able to delay gratification, and emotional dysregulation that includes outbursts of anger.
Based on our review of the limited empirical literature available, several recommendations for couples therapists stand out. Practitioners must be able to identify the complicated and varied symptomalogical dimensions of adult ADHD and its potential effects on couples, and provide this psychoeducation to clients, especially given that many adults are unaware that ADHD can persist past childhood. Clinicians should model sensitivity regarding potential shame surrounding symptoms and attendant functional impairments in the partner with ADHD, as well as address emotional distress – born of the effects of ADHD on the relationship – for which the partner without ADHD may require treatment, while also assisting couples to identify strengths that ADHD may bring to the individuals and their partnership. Providers also must be on the lookout for psychiatric comorbidities of ADHD that may demand interventions alongside the ADHD itself. An integrated treatment approach that combines couples counseling techniques plus interventions for ADHD and its comorbidities could prove difficult (suggesting the need for consultation with other mental health professionals), but also potentially gratifying and successful for all involved.
The sparse amount of empirical research into interventions for couples affected by adult ADHD urges exploration in this area, which may further support integrative treatment and shed light on ways to help spare individuals, couples, and their families unnecessary conflict and dissolution – as well as emphasize and cultivate the positive aspects of living with ADHD.
Conclusion
Adult ADHD may negatively affect intimate partnerships, with potentially compounding effects. Further research is needed to confirm the compounding effects, as is awareness by couples therapy practitioners of the likely possibility that presenting problems could be partly or largely driven by adult ADHD in one or both partners in a distressed relationship. Integrative interventions that address ADHD may provide structure, relief, and hope for adult ADHD-impacted unions, as well as permit recognition of strengths ADHD brings to individuals and their unions.
Finally, the coronavirus-19 (COVID-19) pandemic has brought on many problems for individuals and personal relationships, including intimate ones. The restrictions of the lockdown during the pandemic caused significant levels of emotional distress for all individuals and some researchers have argued that adults with ADHD would have greater levels of stress during the pandemic (Adamou et al., 2020; Evren et al., 2021), as their perceived level of stress is often higher than adults with ADHD (Krause et al., 1998). Evren et al. (2021) found the higher levels of Covid-19 related anxiety was related to increased cigarette smoking and alcohol consumption in young adult males with ADHD.
As many adjust to stay-at-home-related realities such as working and schooling from home, many couples are now under significant amounts of stress. In addition to external stressors, such as possible job loss and health issues, there are also internal stressors, such as depression and anxiety, affecting individuals and their intimate relationships (Pietromonaco and Overall, 2020). For adults with ADHD and their partners, the stress of the pandemic may have exacerbated problems, including maladaptive behaviors and poor communication. Ultimately, given that this is a public health matter, the need to continue education, advocacy, and collaboration with therapists is needed to improve the lives of adults with Attention-deficient/hyperactivity disorder.
References
Adamou M, Fullen T, Galab N, Mackintosh I, Abbott K, Lowe D, et al. Psychological effects of the COVID-19 imposed lockdown on adults with attention deficit/hyperactivity disorder: cross-sectional survey study. JMIR Form Res.2020;4(12):e24430. doi:10.2196/24430
Babinski DE, Waxmonsky JG, Waschbusch DA, Pelham WE. Behavioral observations of parents with ADHD during parent training. J Atten Disord. 2015;22(13):1289-1296. doi:10.1177/1087054715580843
Ben-Naim S, Marom I, Krashin M, Gifter B, Arad K. Life with a partner with ADHD: the moderating role of intimacy. J Child Fam Stud. 2017;26(5):1365-1373. doi:10.1007/s10826-016-0653-9
Bora E, Pantelis C. Meta-analysis of social cognition in attention-deficit/hyperactivity disorder (ADHD): comparison with healthy controls and autistic spectrum disorder. Psychol Med. 2016;46(4):699-716. doi:10.1017/S0033291715002573
Bruner MR, Kuryluk AD, Whitton SW. Attention-deficit/hyperactivity disorder symptom levels and romantic relationship quality in college students. J Am Coll Health. 2015;63(2):98-108. doi:10.1080/07448481.2014.975717
Buitelaar NJ, Posthumus JA, Bijlenga D, Buitelaar JK. The impact of ADHD treatment on intimate partner violence in a forensic psychiatry setting. J Atten Disord. 2019;23:1087054719879502. doi:10.1177/1087054719879502
Canu WH, Tabor LS, Michael KD, Bazzini DG, Elmore AL. Young adult romantic couples conflict resolution and satisfaction varies with partner’s attention-deficit/hyperactivity disorder type. J Marital Fam Ther. 2014;40(4):509-524. doi:10.1111/jmft.12018
Cortese S, Bellgrove MA, Brikell I, Franke B, Goodman DW, Hartman CA, et al. Attention-deficit/hyperactivity disorder (ADHD) in adults: evidence base, uncertainties and controversies. World Psychiatry. 2025;24(3):347-371. doi:10.1002/wps.21374
Das D, Cherbuin N, Butterworth P, Anstey KJ, Easteal S. A population-based study of attention deficit/hyperactivity disorder symptoms and associated impairment in middle-aged adults. PLoS One. 2012;7(2):e31500. doi:10.1371/journal.pone.031500
Evren C. Alcohol- and cigarette-use-related behaviors across gender, dysfunctional COVID-19 anxiety, and the presence of probable ADHD during the pandemic: a cross-sectional study in a sample of Turkish young adults. Dusunen Adam J Psychiatry Neurol Sci. 2021. doi:10.14744/dajpns.2021.00161
Fayyad J, Sampson NA, Hwang I, Adamowski T, Aguilar-Gaxiola S, Al Hamzawi A, et al. The descriptive epidemiology of DSM-IV adult ADHD in the World Health Organization World Mental Health Surveys. Published 2017.
Ghahramanzadeh M, Mashhadi A, Shamloo ZS, Kimiaee SA. Comparing emotional disturbances and quality of life in couples with attention-deficit and hyperactivity disorder and ordinary couples. J Fundam Ment Health. 2021;23(1):41-48.
González RA, Kallis C, Coid JW. Adult attention deficit hyperactivity disorder and violence in the population of England: does comorbidity matter? PLoS One. 2013;8(9):e75575. doi:10.1371/journal.pone.0075575
Hallowell EM, Hallowell S, Orlov M. Married to distraction: how to restore intimacy and strengthen your partnership in an age of interruption. Ballantine Books; 2011.
Hankin CS. ADHD and its impact on the family. Drug Benefit Trends. 2001;13(suppl C):15-16.
Hirvikoski T, Lindström T, Carlsson J, Waaler E, Jokinen J, Bölte S. Psychoeducational groups for adults with ADHD and their significant others (PEGASUS): a pragmatic multicenter randomized controlled trial. Eur Psychiatry. 2017;44:141-152. doi:10.1016/j.eurpsy.2017.04.005
Johnston C, Mash EJ, Miller N, Ninowski JE. Parenting in adults with attention-deficit/hyperactivity disorder (ADHD). Clin Psychol Rev. 2012;32(4):215-228. doi:10.1016/j.cpr.2012.01.007
Jiang Y, Johnston C. The relationship between ADHD symptoms and competence as reported by both self and others. J Atten Disord. 2012;16(5):418-426. doi:10.1177/1087054710392541
Katzman MA, Bilkey TS, Chokka PR, Fallu A, Klassen LJ. Adult ADHD and comorbid disorders: clinical implications of a dimensional approach. BMC Psychiatry. 2017;17(1):302. doi:10.1186/s12888-017-1463-3
Kessler RC, Adler LA, Barkley R, Biederman J, Conners CK, Faraone SV, et al. Patterns and predictors of attention-deficit/hyperactivity disorder persistence into adulthood: results from the National Comorbidity Survey Replication. Biol Psychiatry. 2005;57(11):1442-1451. doi:10.1016/j.biopsych.2005.04.001
Klein RG, Mannuzza S, Olazagasti MA, Roizen E, Hutchison JA, Lashua EC, et al. Clinical and functional outcome of childhood attention-deficit/hyperactivity disorder 33 years later. Arch Gen Psychiatry. 2012;69(12):1295-1303. doi:10.1001/archgenpsychiatry.2012.271
Libutzki B, Ludwig S, May M, Jacobsen R, Reif A, Hartman C. Direct medical costs of ADHD and its comorbid conditions on basis of a claims data analysis. Eur Psychiatry. 2019;58:38-44. doi:10.1016/j.eurpsy.2019.01.019
Lui JH, Johnston C, Lee CM, Lee-Flynn SC. Parental ADHD symptoms and self-reports of positive parenting. J Consult Clin Psychol. 2013;81(6):988-998. doi:10.1037/a0033490
Markman HJ, Stanley SM, Blumberg SL, Jenkins NH, Whiteley C. 12 hours to a great marriage: a step-by-step guide for making love last. Jossey-Bass; 2004.
Marsh LE, Norvilitis JM, Ingersoll TS, Li B. ADHD symptomatology, fear of intimacy, and sexual anxiety and behavior among college students in China and the United States. J Atten Disord. 2015;19(3):211-221. doi:10.1177/1087054712453483
McGough JJ. Treatment controversies in adult ADHD. Am J Psychiatry. 2016;173(10):960-966. doi:10.1176/appi.ajp.2016.15091207
Michielsen M, Comijs HC, Aartsen MJ, Semeijn EJ, Beekman ATF, Deeg DJH, et al. The relationships between ADHD and social functioning and participation in older adults in a population-based study. J Atten Disord. 2015;19(5):368-379. doi:10.1177/1087054713515748
Moyá J, Stringaris AK, Asherson P, Sandberg S, Taylor E. The impact of persisting hyperactivity on social relationships. J Atten Disord. 2014;18(1):52-60. doi:10.1177/1087054712436876
National Academies of Sciences, Engineering, and Medicine. Adult attention-deficit/hyperactivity disorder: diagnosis, treatment, and implications for drug development: proceedings of a workshop. National Academies Press; 2024.
Pachado MP, Scherer JN, Guimarães LS, von Diemen L, Pechansky F, Kessler FH, et al. Markers for severity of problems in interpersonal relationships of crack cocaine users from a Brazilian multicenter study. Psychiatr Q. 2018;89(4):923-936. doi:10.1007/s11126-018-9590-7
Pietromonaco PR, Overall NC. Applying relationship science to evaluate how the COVID-19 pandemic may impact couples relationships. Am Psychol. 2021;76(3):438-450. doi:10.1037/amp0000714
Posner J, Polanczyk GV, Sonuga-Barke EJS. Attention-deficit hyperactivity disorder. Lancet. 2020;395(10222):450-462. doi:10.1016/S0140-6736(19)33004-1
Robin A, Payson E. The impact of ADHD on marriage. ADHD Rep. 2002;10:9-13.
Romero-Martínez Á, Lila M, Moya-Albiol L. The importance of impulsivity and attention switching deficits in perpetrators convicted for intimate partner violence. Aggress Behav. 2019;45(2):129-138. doi:10.1002/ab.21802
Skirrow C, Asherson P. Emotional lability, comorbidity and impairment in adults with attention-deficit hyperactivity disorder. J Affect Disord. 2013;147(1-3):80-86. doi:10.1016/j.jad.2012.10.011
Waxmonsky JG, Waschbusch DA, Babinski DE, Humphrey HH, Alfonso A, Crum KI, et al. Does pharmacological treatment of ADHD in adults enhance parenting performance? Results of a double-blind randomized trial. CNS Drugs.2014;28(7):665-677. doi:10.1007/s40263-014-0165-3
Whisman MA, Baucom DH. Intimate relationships and psychopathology. Clin Child Fam Psychol Rev. 2012;15(1):4-13. doi:10.1007/s10567-011-0107-2
Wymbs BT, Canu WH, Sacchetti GM, Ranson LM. Adult ADHD and romantic relationships: what we know and what we can do to help. J Marital Fam Ther. 2021;47(3):664-681. doi:10.1111/jmft.12475
Wymbs BT, Dawson AE, Suhr JA, Bunford N, Gidycz CA. ADHD symptoms as risk factors for intimate partner violence perpetration and victimization. J Interpers Violence. 2017;32(5):659-681. doi:10.1177/0886260515586371
Wymbs BT, Molina BSG. Integrative couples group treatment for emerging adults with ADHD symptoms. Cogn Behav Pract. 2015;22(2):161-171. doi:10.1016/j.cbpra.2014.06.008
Xiao Y, Watson M. Guidance on conducting a systematic literature review. J Plan Educ Res. 2019;39(1):93-112. doi:10.1177/0739456X17723971




