Staphylococcal Scalded Skin Syndrome in Elderly Patients
Staphylococcal Scalded Skin Syndrome in an Elderly Patient: A Rare and Life-Threatening Case Report
Sofia Camões 1, Nídia Oliveira 1, Beatriz Silva 1, Hugo Ventura 1, Filipa Reis 1, Fabiola de Almeida Figueiredo 1, Catarina Oliveira 1, Margarida Rato 2, Rita Cabral 2, Edite Nascimento 1
- Internal Medicine, Unidade Local de Saúde Viseu- Dão Lafões
- Dermatology, Unidade Local de Saúde Viseu- Dão Lafões
OPEN ACCESS
PUBLISHED: 28 February 2026
CITATION: Camões, S., Oliveira, N., et al., 2026. Staphylococcal Scalded Skin Syndrome in an Elderly Patient: A Rare and Life-Threatening Case Report. Medical Research Archives, [online] 14(2).
COPYRIGHT: © 2026 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
ISSN 2375-1924
Abstract
Staphylococcal scalded skin syndrome (SSSS) is a toxin-mediated exfoliative dermatosis that predominantly affects neonates and young children. Adult cases are rare and associated with high morbidity and mortality, particularly among elderly patients with comorbidities. We report the case of an 85-year-old woman admitted with sepsis secondary to a urinary tract infection who developed acute diffuse erythema, superficial desquamation, and a positive Nikolsky sign during hospitalization. Histopathological examination revealed intraepidermal acantholysis, consistent with SSSS. Prompt initiation of targeted antimicrobial therapy and supportive care resulted in complete clinical recovery. This case highlights the importance of considering SSSS in the differential diagnosis of acute exfoliative dermatoses in adults. Early recognition, differentiation from Stevens–Johnson syndrome, and timely multidisciplinary management are essential to improve outcomes in this high-risk population.
Keywords:
- Staphylococcal scalded skin syndrome
- Elderly
- Exfoliative toxins
- Stevens–Johnson syndrome
- Case report
Introduction
Staphylococcal scalded skin syndrome (SSSS) is an acute exfoliative skin disorder caused by exfoliative toxins A and B produced by specific strains of Staphylococcus aureus. These toxins induce cleavage at the granular layer of the epidermis by targeting desmoglein-1, leading to widespread superficial blistering and desquamation. This syndrome predominantly affects neonates and young children due to immature renal clearance of circulating toxins and lack of protective antibodies. In contrast, adult SSSS is rare and typically occurs in patients with underlying conditions such as chronic kidney disease, diabetes mellitus, malignancy, or immunosuppression. Adult cases are associated with significantly higher mortality rates, reported to reach 50–60%, largely due to delayed diagnosis and comorbidities. Differentiation from other severe exfoliative dermatoses, particularly Stevens–Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), is critical, as management and prognosis differ substantially. These factors contribute to diagnostic uncertainty and may negatively impact prognosis in adult patients. Although SSSS is well recognized in pediatric populations, its occurrence in adults is uncommon and often associated with delayed diagnosis and poor outcomes. Elderly patients are particularly vulnerable due to comorbidities and impaired renal clearance of exfoliative toxins. Adult mortality has been reported to be substantially higher than in children. Given the clinical overlap with other severe cutaneous adverse reactions, such as Stevens–Johnson syndrome and toxic epidermal necrolysis, early recognition of adult SSSS remains challenging but crucial. We present a rare case of SSSS in an elderly patient with favorable outcome, aiming to highlight key diagnostic features, therapeutic considerations, and the importance of multidisciplinary management in adult patients.
Case Presentation
An 85-year-old woman was admitted to the emergency department with a two-day history of fever and generalized asthenia. She had been previously treated at a private clinic with two doses of ceftriaxone and a non-steroidal anti-inflammatory drug for a presumed urinary tract infection. Subsequently, she developed oliguria, dysuria, polyuria, and erythematous skin lesions on the neck. Her medical history included insulin-treated type 2 diabetes mellitus, recurrent urinary tract infections, obesity, arterial hypertension, and hypothyroidism. She had a known allergy to amoxicillin.
On admission, she was hemodynamically stable but febrile (38.4 °C). Physical examination revealed a generalized erythematous rash, more prominent in the cervical region. Laboratory tests showed leukocytosis with neutrophilia, elevated C-reactive protein, and stage 2 acute kidney injury according to KDIGO criteria. Urinalysis demonstrated marked leukocyturia, hematuria, and positive nitrites. Renal and bladder ultrasonography revealed no significant abnormalities.
A septic workup was initiated, and empirical antibiotic therapy with ciprofloxacin was started. Urine cultures isolated extended-spectrum beta-lactamase–producing Escherichia coli, sensitive to ertapenem, gentamicin, and nitrofurantoin; blood cultures were negative. Antibiotic therapy was therefore adjusted to ertapenem for seven days.
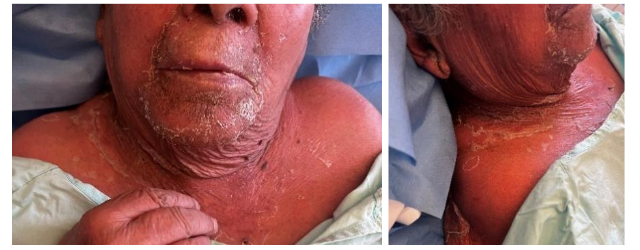
On the first day of hospitalization, the patient developed a diffuse exanthem with superficial dermal desquamation involving the perioral, periorbital, and cervical regions, along with a positive Nikolsky sign on the neck.
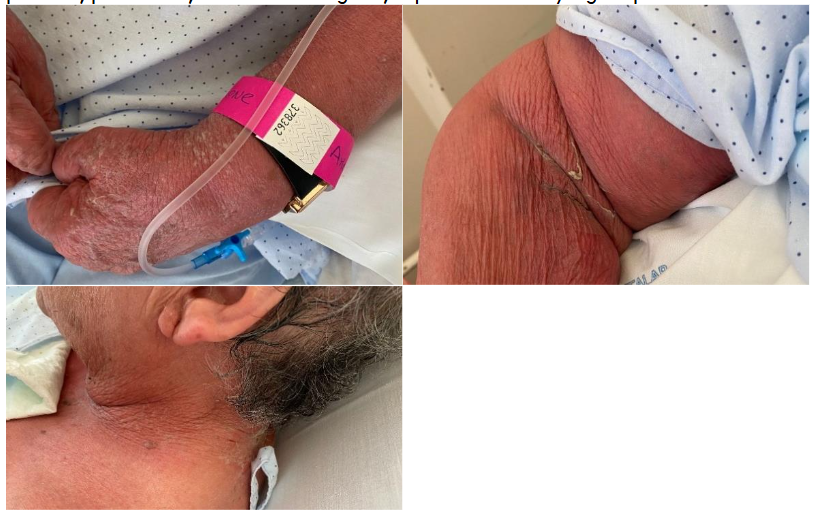
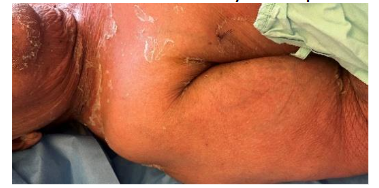
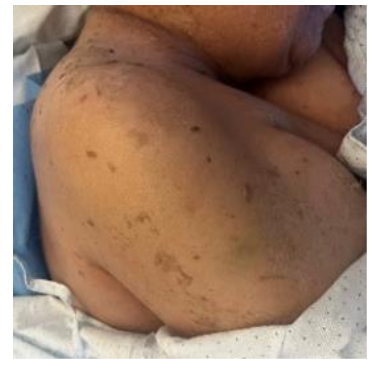
Figure 1 A-C. Diffuse exanthem with superficial desquamation, observed on the first day of hospitalization, involving the perioral, periorbital, and cervical regions; a positive Nikolsky sign is presente on the neck.
Dermatology consultation raised suspicion of SSSS. The patient was transferred to an isolation room for protective care, and bladder catheterization was performed to prevent skin contamination. Intravenous vancomycin was added and continued for ten days, in line with recommendations for suspected adult SSSS. Skin swab cultures isolated Enterococcus faecalis and Escherichia coli, both sensitive to gentamicin. A skin biopsy revealed intraepidermal acantholysis without full-thickness epidermal necrosis, findings consistent with SSSS. Although Stevens–Johnson Syndrome could not be completely excluded histologically, the absence of mucosal involvement and the rapid clinical improvement without corticosteroid therapy strongly supported the diagnosis of SSSS. Due to periorbital involvement, ophthalmological evaluation was performed. Artificial tears and topical antibiotics were prescribed. No ocular or other mucosal involvement was identified.
The patient showed progressive clinical and analytical improvement, with complete resolution of skin lesions and recovery of renal function. She was discharged with full restoration of skin integrity.
The patient returned to the emergency department four months after the initial hospitalization due to a urinary tract infection caused by Escherichia coli. The patient was readmitted and treated with intravenous antibiotic therapy, with no complications during the hospital stay. Approximately one year after the initial hospitalization, the patient died of natural causes in the community. No similar episodes were reported following discharge.
Discussion
Staphylococcal scalded skin syndrome is predominantly a pediatric disease, with adult cases representing a rare but clinically significant entity. In contrast to children, adult SSSS is frequently associated with severe underlying conditions, including renal dysfunction, diabetes mellitus, malignancy, and immunosuppression, which impair toxin clearance and contribute to worse outcomes. Adult cases remain poorly represented in the literature, largely limited to case reports and small series, which may further contribute to delayed recognition in clinical practice. Reported mortality rates in adults range from 50% to 60%, markedly higher than those observed in pediatric populations. The present case is therefore noteworthy not only due to the advanced age of the patient, but also because of the favorable clinical outcome despite multiple risk factors.
The diagnostic challenge in adult SSSS lies primarily in its clinical overlap with other acute exfoliative dermatoses, particularly Stevens–Johnson syndrome and toxic epidermal necrolysis. Accurate differentiation is essential, as management strategies and prognoses differ substantially. In SSSS, epidermal cleavage occurs superficially at the granular layer due to desmoglein-1 disruption, resulting in fragile bullae, superficial desquamation, and a positive Nikolsky sign, while mucous membranes are typically spared. In contrast, SJS/TEN is characterized by full-thickness epidermal necrosis and prominent mucosal involvement, often accompanied by systemic deterioration.
In the present case, the absence of mucosal involvement, the histopathological finding of intraepidermal acantholysis without keratinocyte necrosis, and the rapid clinical improvement without immunosuppressive therapy strongly supported the diagnosis of SSSS over SJS/TEN. The temporal association between systemic infection and the onset of cutaneous manifestations further reinforces a toxin-mediated mechanism. This highlights the importance of maintaining a high index of suspicion for SSSS in adult patients presenting with acute exfoliative skin findings, particularly in the context of sepsis or renal dysfunction.
Management of adult SSSS relies on prompt initiation of effective anti-staphylococcal antimicrobial therapy, eradication of the infectious focus, and meticulous supportive care. Supportive measures, including fluid and electrolyte management, temperature control, pain management, and prevention of secondary infections, are essential and parallel those employed in burn care units. Early dermatology consultation and a multidisciplinary approach are crucial to optimize outcomes, particularly in elderly patients with multiple comorbidities. The favorable evolution observed in this high-risk patient underscores the potential impact of early diagnosis, appropriate antimicrobial selection, and comprehensive supportive management. Although adult SSSS remains a rare diagnosis, increased awareness among clinicians may facilitate earlier recognition and reduce associated morbidity and mortality. This case contributes to the limited body of literature on adult SSSS and reinforces the importance of considering this diagnosis in elderly patients presenting with acute exfoliative dermatoses.
Conclusion
This case illustrates a rare presentation of staphylococcal scalded skin syndrome in an elderly patient and reinforces the importance of maintaining a high index of suspicion for SSSS in adults presenting with acute exfoliative dermatoses. Early recognition, accurate differentiation from Stevens–Johnson syndrome, and timely initiation of appropriate antimicrobial and supportive therapy are crucial to improving outcomes and reducing mortality.
Informed Consent
Written informed consent was obtained from the patient’s legal representative for the publication of this case report. All identifying information has been removed to ensure patient anonymity.
Ethics Statement, Conflicts of Interest and Funding
This study was conducted in accordance with the principles of the Declaration of Helsinki. The authors declare no conflicts of interest. No external funding was received for the preparation of this manuscript.
References
- Ladhani S. Understanding the mechanism of action of the exfoliative toxins of Staphylococcus aureus. FEMS Immunol Med Microbiol. 2003;39(2):181–189.
- Handler MZ, Schwartz RA. Staphylococcal scalded skin syndrome: diagnosis and management in adults and children. J Eur Acad Dermatol Venereol. 2014;28(11):1418–1423.
- Lyell A. A review of the staphylococcal scalded skin syndrome. Br J Dermatol. 1988;118(2):181–186.
- Patel GK, Finlay AY. Staphylococcal scalded skin syndrome: an update. Dermatology. 2003;207(4):329–334.
- Melish ME, Glasgow LA. The staphylococcal scalded skin syndrome. N Engl J Med. 1970;282(20):1114–1119.
- Cribier B, Piemont Y, Grosshans E. Staphylococcal scalded skin syndrome in adults. Br J Dermatol. 1994;130(5):653–658.
- Lamand V, et al. Staphylococcal scalded skin syndrome in adults: a clinical and prognostic study. Clin Infect Dis. 2013;56(12):e164–e170.
- Mockenhaupt M. Severe cutaneous adverse reactions. J Dtsch Dermatol Ges. 2010;8(10):803–813.
- Bukowski JA, et al. Adult staphylococcal scalded skin syndrome: a clinicopathological review. Am J Med. 2020;133(6):e323–e330.
- Klein R, et al. Adult staphylococcal scalded skin syndrome: diagnostic pitfalls. Dermatology. 2022;238(6):1049–1056.
- Patel N, et al. Adult staphylococcal scalded skin syndrome: a rare but severe disease. IDCases. 2024;36:e01985.
- Harr T, French LE. Stevens–Johnson syndrome and toxic epidermal necrolysis. Chem Immunol Allergy. 2012;97:149–166.
- Ladhani S, et al. Management of staphylococcal scalded skin syndrome. Arch Dis Child. 2010;95(10):819–824.
- Patel GK, Finlay AY. Staphylococcal scalded skin syndrome: diagnosis and management. Clin Dermatol. 2019;37(4):331-336.
- Creamer D, Walsh SA, Dziewulski P, et al. U.K. guidelines for the management of Stevens–Johnson syndrome/toxic epidermal necrolysis in adults 2016. Br J Dermatol. 2016;174(6):1194-1227.
- Haveman LM, Fleer A, van Dijk MR, et al. Adult staphylococcal scalded skin syndrome: clinical features, outcomes, and prognostic factors. J Am Acad Dermatol. 2017;76(2):278-284.




