Enhancing Medical Education Through Drawing Techniques
Enhancing Medical Education Through Drawing: A Pathway to Deeper Understanding and Retention
Valerie Weiss¹, Vanessa Kinley¹, Nicola Khalaf¹, Rob Sillevis¹
- Florida Gulf Coast University, Fort Myers, Florida
OPEN ACCESS
PUBLISHED: 30 April 2025
CITATION: Weiss, V., Kinley, V., et al., 2025. Enhancing Medical Education Through Drawing: A Pathway to Deeper Understanding and Retention. Medical Research Archives, [online] 13(4). https://doi.org/10.18103/mra.v13i4.6501
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i4.6501
ISSN 2375-1924
Abstract
N/A
Keywords
- Medical Education
- Drawing
- Active Learning
- Retention
- Anatomy
Introduction
Medical education is known for its rigorous demands, requiring students to develop a comprehensive understanding about the human body. Likewise, excelling in the pre-requisites needed for medical school admission is equally challenging due to the required intensive, content-heavy nature of required courses. Despite the evolution of pedagogical approaches, traditional teaching methods—such as didactic lectures and extensive note-taking—remain the predominant approach in these settings. As a result, students often resort to rote memorization to meet high-stake exam deadlines, while educators focus on covering large volumes of materials efficiently. Yet, do these passive learning strategies truly support long-term comprehension and retention?
Recognizing these challenges, researchers have explored alternative methods to encourage active learning and deeper understanding. For instance, Luscombe and Montgomery examined medical students’ experiences in large lectures and found that students perceived learning primarily occurred outside the lecture environment, highlighting the need for more interactive pedagogy. Similarly, Challa et al conducted a systematic review of modern teaching and learning techniques in medical education, underscoring the limitations of lecture-based instruction while advocating for other methods that foster active engagement and critical thinking. Further reinforcing this perspective, Mishra et al. compared the effectiveness of didactic lectures versus activity-based learning in teaching anatomy to first-year medical students. Their findings concluded that a blended approach—combing lectures with activity-based learning—yields better outcomes, particularly in terms of retention and conceptual understanding.
Despite the growing body of evidence supporting active learning, many medical school curricula continue to rely on traditional instructional strategies, often overlooking newer research-based instructional design principals. Dr. Levinson, Professor and Chair of health Sciences Educational Research and Instructional Development at McMaster University, highlights this gap, emphasizing that while theories of multimedia learning and cognitive load have been extensively studied by Mayer, their implementation in medical education remains limited. Levinson suggests that many medical school lectures run contrary to best instructional design practices, frequently leading to cognitive overload and reduced learning efficiency. Addressing these limitations requires not only adopting innovative teaching techniques but also ensuring that medical educators are trained in evidence-based instructional design.
Building on these insights, we propose that drawing may serve as a valuable supplementary tool for reinforcing anatomical learning. This editorial explores the role of drawing in medical education, its impact on student learning, and how integrating visual strategies may shape future physicians’ understanding of the human body.
Enhancing Memory and Learning via Drawing
Research by Fernandes et al. at the University of Waterloo in Ontario, Canada, reinforces the age-old proverb that “a picture is worth a thousand words,” suggesting that drawing may be a powerful tool for aiding learning. Across several studies, Fernandes and her colleagues established the drawing effect, essentially comparing the effectiveness of drawing as a memory aid in comparison to other methods. Their research demonstrates that drawing significantly improves memory retention and recall—outperforming traditional study strategies such as note-taking, listening to lectures, or viewing pre-existing images. Notably, the benefits of drawing persist regardless of artistic ability, making it an accessible and effective learning strategy for all students.
Beyond establishing the drawing effect, Fernandes and her colleagues established the Integrated-Trace Hypothesis, which explains why drawing benefits memory. According to this hypothesis, drawing engages multiple cognitive processes, including visual, semantic, and motor functions, embedding information more deeply into one’s memory compared to other strategies for learning and remembering.
Integrating Drawing into Medical Education
Fernandes et al.’s Integrated-Trace Hypothesis, in which multiple cognitive processes are engaged, has profound implications for medical education. Its implications for medical education are substantial, as mastering human anatomy and physiology extends beyond mere memorization. Instead, students must cultivate a comprehensive understanding of the body’s complex systems to effectively apply their knowledge in clinical practice.
A study by Beach et al. at the University of Vermont Medical Center in 2023 further supports the value of drawing in medical education. The study examined first-year medical students learning spinal anatomy through three different approaches: 1) drawing 2) clay modeling and 3) viewing a 3-dimensional anatomy application (control group). Results showed that students in the drawing group experienced significantly greater improvement in test scores (+11%) compared to the other groups. Clay modeling showed some improvement, but not to a statistically significant degree, while the control group showed no improvement at all. These findings reinforce the Integrated-Trace Hypothesis, demonstrating that actively engaging multiple cognitive pathways (visual, motor, and semantic) enhances student learning outcomes.
Boosting Engagement and Comprehension in Medical Education
Historically, drawing has played a crucial role in anatomical education, dating back to Renaissance artists such as Michelangelo and Leonardo da Vinci, who meticulously illustrated human dissections to advance anatomical knowledge. Adding to this perspective, Kumar and Rajprasath emphasize the historical connection between anatomical drawing and medical education. They highlight that, traditionally, students would dissect cadavers and touch/feel structures and then use drawings or atlases to depict and remember their observations.
Modern research supports the continued relevance of the role of drawing in learning. Joewono et al. investigated the impact of drawing in a first-year medical school anatomy course, finding that it significantly improved students’ comprehension of musculoskeletal anatomy. Their study suggests that drawing is not merely an artistic exercise but an effective educational tool—one that fosters deeper engagement, reinforces structural relationships, and enhances long-term retention.
Additionally, Liou et al. provide another compelling argument in favor of integrating drawing into medical education through structured clinical sketching workshops. Their study found that medical students, regardless of artistic ability, could learn to use basic medical illustration techniques to organize their thoughts, clarify anatomical relationships, and enhance patient communication. In their workshop, students engaged in structured exercises such as simplifying complex anatomical diagrams, illustrating blood circulation pathways, and visually summarizing laparoscopic surgeries in just a few key sketches. These exercises forced students to identify the most critical aspects of a procedure, which improved their ability to synthesize and communicate medical information efficiently—skills that extend beyond illustration into clinical practice.
Another study by Borrelli et al. adds a further dimension by quantitatively measuring the impact of anatomy drawing workshops. Their study found that students who attended structured drawing sessions showed a 22.5% statistically significant improvement in anatomical knowledge and a 43.2% increase in confidence in drawing anatomy. They designed a series of anatomy drawing workshops covering upper limb, lower limb, thorax, and head & neck anatomy, integrating whiteboard drawing demonstrations with cadaveric illustrations. Students reported that this two-part method, which transitioned from conceptual drawings to real-life cadaveric structures, enhanced their ability to visualize and retain anatomical relationships. A notable finding in Borrelli et al.’s research was that students identified “time constraints” as the primary barrier to incorporating drawing into their revision strategies. Despite this, qualitative feedback from students overwhelmingly suggested that drawing should be integrated into the core medical curriculum rather than being an optional or extracurricular activity.
Fostering Creativity and Problem-Solving in Today’s Learner
With the growing prevalence of digital resources and multimedia learning, students today may require a different approach to education. Kumar and Rajprasath suggest that modern learners, accustomed to interactive technology, will tend to be less engaged with traditional drawing techniques. However, Kumar and Rajprasath argue that drawing remains crucial because it forces students to construct a “mental model” of anatomical structures, requiring them to actively recall and organize information—key metacognitive skills that are often neglected in passive learning strategies.
For example, as illustrated in Figure 1, a student’s drawing of the four layers of the gastrointestinal tract demonstrates the application of problem-solving and creativity. By arranging the digestive mucosa, submucosa, muscularis, and serosa in the correct sequence, the student actively engages with the material, reinforcing their understanding of anatomical structures and their relationships rather than passively absorbing information.
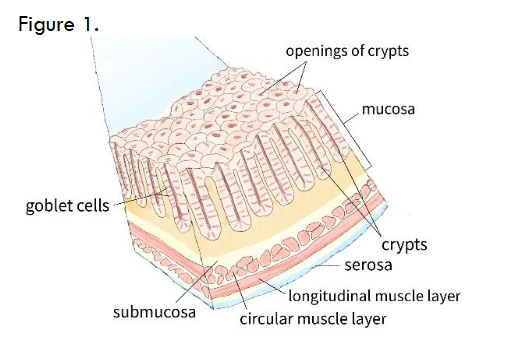
From a student’s perspective, drawing remains an underutilized learning tool. Traditional studying methods, such as reading through textbooks, writing extensive notes, and listening to oral lectures, are important but often stimulate passive learning. Conversely, the motion of drawing allows students to observe, process, and duplicate anatomical structures, promoting increased retention and active learning of complex information. This has become increasingly important to address with the exponential student usage of artificial intelligence. Hand drawing stands as one of the final reliable study methods to ensure student engagement.
Sketching grants students with the opportunity to navigate and better understand the three-dimensional nature of the human body. The action of illustrating stimulates students to visualize structures and enhance their spatial awareness, providing a firmer foundation for the implementation of physiological information. This skillset is crucial for future medical professionals, such as surgeons, dentists, and radiologists, who are challenged with accurately identifying and interpreting anatomical positioning every day. Additionally, illustrating increases memory retention through active recall. Some may be hesitant due to a lack of artistic confidence, but research confirms that drawing benefits memory and comprehension regardless of skill level. As opposed to passively attending lectures and writing notes to describe anatomical positions and organ systems, drawing enables students to retrieve and reproduce anatomical structures, address their weaknesses, and reinforce their knowledge. Beyond its educational benefits, illustrating can also provide students with a stress-relieving pathway between their rigorous academic requirements, promoting healthy and desired learning. Through the integration of creative approaches into learning routines, burnout levels can be mitigated while also promoting a healthy mental environment for students.
Promoting Wellness and Reducing Stress through Creative Learning
Medical training is rigorous, and stress and anxiety are common among this population. A significant benefit of incorporating drawing into medical education is its positive impact on student well-being. Students enrolled in Weiss’ medical illustration course during the COVID-19 pandemic described the drawing-based learning as “therapeutic, especially while self-isolating.” This supportive atmosphere was especially valuable during pandemic lockdowns, but its benefits extend to any high-stress academic setting. Thompson et al. highlight how integrating creative work, such as drawing, in medical education fosters emotional intelligence, improving students’ ability to connect with patients and navigate the complexities of medical practice. By encouraging artistic expression, medical schools can cultivate well-rounded practitioners better equipped to understand and respond to their patients’ experiences.
From an educator’s perspective, incorporating drawing into the curriculum enhances student engagement, promotes active learning, and boosts confidence. Instead of passively absorbing information, students who draw actively process and reinterpret complex concepts in a way that is both personal and meaningful. Research by Weiss et al. supports this approach, showing that integrating reading, discussion, and drawing significantly improves student confidence in learning anatomy and physiology. This interdisciplinary method creates a more memorable learning experience by transforming abstract ideas into tangible knowledge.
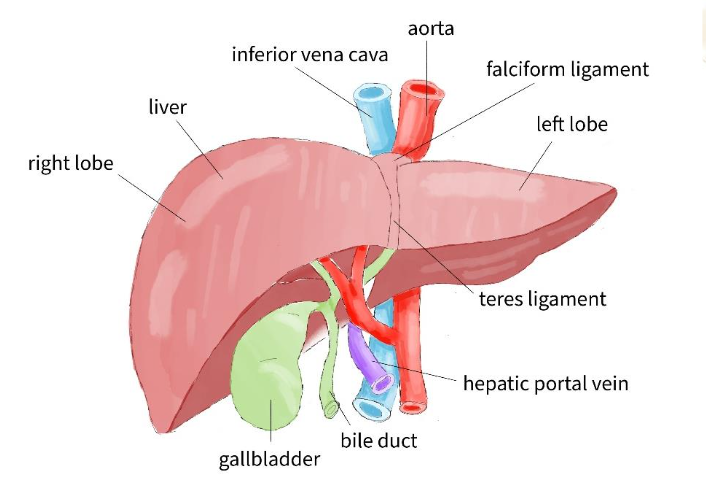
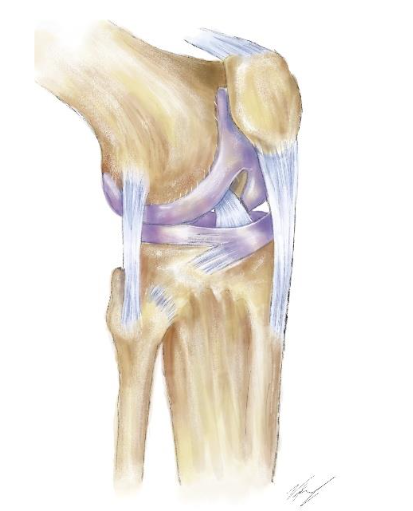
Conclusion
As medical education continues to evolve, adopting innovative teaching methods that promote comprehension and enhance retention is essential. Research supports drawing as an effective learning strategy, not only for retention but also for developing spatial understanding, fostering creativity, and reducing stress. Moreover, drawing transforms learning into an engaging, active process that encourages curiosity and deeper cognitive processing. The key benefits of integrating drawing into medical education are summarized in Figure 4.
In conclusion, by incorporating drawing into medical curricula, both students and educators can benefit from a richer, more effective learning experience—one that ensures knowledge is not merely memorized but truly understood.
Key Benefits of Integrating Drawing into Medical Education
- Enhanced Memory and Retention
- Deeper Understanding of Complex Anatomy
- Active Learning with Increased Engagement
- Enhanced Creativity and Problem-Solving Skills
- Promoting Wellness and Reducing Stress
References
- Slotnick HB. How doctors learn: education and learning across the medical-school-to-practice trajectory. Acad Med. 2001;76(10):1013-1026. doi:10.1097/00001888-200110000-00008
- Dienstag JL. Relevance and rigor in premedical education. N Engl J Med. 2008;359(3):221-224. doi:10.1056/NEJMp0803098
- Challa KT, Sayed A, Acharya Y. Modern techniques of teaching and learning in medical education: a descriptive literature review. MedEdPublish (2016). 2021;10:18. Published 2021 Jan 21. doi:10.15694/mep.2021.000018.1
- Das NK, Khan S, Patil R, Mukhida S. Is PowerPoint killing the art of medical teaching and is the interactive board way forward? Sri Ramachandra Journal of Health Sciences. 2024;4:4-5. doi:10.25259/srjhs_37_2023
- Ghaleb BDS. Effect of Exam-Focused and Teacher-Centered education systems on students’ cognitive and psychological competencies. International Journal of Multidisciplinary Approach Research and Science. 2024;2(02):611-631. doi:10.59653/ijmars.v2i02.648
- Luscombe C, Montgomery J. Exploring medical student learning in the large group teaching environment: examining current practice to inform curricular development. BMC Med Educ. 2016;16:184. Published 2016 Jul 19. doi:10.1186/s12909-016-0698-x
- Mishra D, Singh S, Khan AZ, Kumar S, Dwivedi P. Comparison of Didactic Lectures and Activity-Based Learning for teaching First-Professional MBBS students in the subject of anatomy. Cureus. Published online December 26, 2023. doi:10.7759/cureus.51106
- Mayer RE. Applying the science of learning to medical education. Med Educ. 2010;44(6):543-549. doi:10.1111/j.1365-2923.2010.03624.x
- Mayer RE. Applying the science of learning to multimedia instruction. In: The Psychology of Learning and Motivation/The psychology of Learning and Motivation.; 2011:77-108. doi:10.1016/b978-0-12-387691-1.00003-x
- Levinson AJ. Where is evidence-based instructional design in medical education curriculum development?. Med Educ. 2010;44(6): 536-537. doi:10.1111/j.1365-2923.2010.03715.x
- Fernandes MA, Wammes JD, Meade ME. The surprisingly powerful influence of drawing on memory. Current Directions in Psychological Science. 2018;27(5):302-308. doi:10.1177/0963721418755385
- Wammes JD, Meade ME, Fernandes MA. Creating a recollection-based memory through drawing. J Exp Psychol Learn Mem Cogn. 2018;44(5):734-751. doi:10.1037/xlm0000445
- Wammes JD, Meade ME, Fernandes MA. The drawing effect: Evidence for reliable and robust memory benefits in free recall. Q J Exp Psychol (Hove). 2016;69(9):1752-1776. doi:10.1080/17470218.2015.1094494
- Wammes JD, Jonker TR, Fernandes MA. Drawing improves memory: The importance of multimodal encoding context. Cognition. 2019;191:103955. doi:10.1016/j.cognition.2019.04.024
- Meade ME, Wammes JD, Fernandes MA. Drawing as an Encoding Tool: Memorial Benefits in Younger and Older Adults. Exp Aging Res. 2018;44(5):369-396. doi:10.1080/0361073X.2018.1521432
- Wammes JD, Meade ME, Fernandes MA. Learning terms and definitions: Drawing and the role of elaborative encoding. Acta Psychol (Amst). 2017;179:104-113. doi:10.1016/j.actpsy.2017.07.008
- Beach IR, D’Agostino EN, Thakrar R, Lunardini DJ. Learning by drawing and modeling: Teaching modalities for spinal anatomy in medical students. Anat Sci Educ. 2023;16(6):1041–1045. doi:10.1002/ase.2313
- Naicker J. Medical illustration in anatomy. In: Graphic Medicine, Humanizing Healthcare and Novel Approaches in Anatomical Education [3, 1 Ed.]; 2023:63-83. doi:10.1007/978-3-031-39035-7_4
- Kumar D, Rajprasath R. Drawing skills in anatomy education and the millennial learner: A cognitive and metacognitive viewpoint. Research and Development in Medical Education. 2019;8(1):58-60. doi:10.15171/rdme.2019.010
- Joewono M, Karmaya INM, Wirata G, Yuliana N, Widianti IGA, Wardana ING. Drawing method can improve musculoskeletal anatomy comprehension in medical faculty student. Anatomy & Cell Biology. 2018;51(1):14. doi:10.5115/acb.2018.51.1.14
- Liou KT, George P, Baruch JM, Luks FI. Clinical sketches: teaching medical illustration to medical students. Med Educ. 2014;48(5):522-548 doi:10.1111/medu.12450
- Borrelli MR, Leung B, Morgan MCB, Saxena S, Hunter A. Should drawing be incorporated into the teaching of anatomy? J Contemp Med Educ. 2018;6(2):34-48. doi:10.5455/jcme.20180411105347
- Dhawan S, Batra G. Artificial intelligence in higher education: promises, perils, and perspective. Expand Knowl Horiz OJAS. 2020;11:11-22.
- Engel T, Gowda D, Sandhu JS, Banerjee S. Art Interventions to Mitigate Burnout in Health Care Professionals: A Systematic Review. Perm J. 2023;27(2):184-194. doi:10.7812/TPP/23.018
- Mirza AA, Baig M, Beyari GM, Halawani MA, Mirza AA. Depression and Anxiety Among Medical Students: A Brief Overview. Adv Med Educ Pract. 2021;12:393-398. Published 2021 Apr 21. doi:10.2147/AMEP.S302897
- Weiss V, Casazza K. Leveraging the art of medical illustration to enhance anatomy instruction. In: Stephen JS, Kormpas G, Coombe C, eds. Global Perspectives on Higher Education. Vol 11. Knowledge Studies in Higher Education. Springer; 2023. doi:10.1007/978-3-031-31646-3_15
- Thompson T, Lamont-Robinson C, Younie L. ‘Compulsory creativity’: rationales, recipes, and results in the placement of mandatory creative endeavour in a medical undergraduate curriculum. Med Educ Online. 2010; 15:10.3402/meo.v15i0.5394. Published 2010 Nov 26. doi:10.3402/meo.v15i0.5394
- Weiss V, Khalaf N, Sillevis R. The Influence of an Interdisciplinary Approach on Student Confidence in Undergraduate Anatomy and Physiology. HAPS Educator Journal. 2024;28(2). doi:10.21692/haps.2024.012

