Aberrometric Impact of High-Tech Intraocular Lenses
Aberrometric impact in post-cataract surgery patients with high-tech intraocular lenses
Dr. Arturo Iván Pérez Pacheco1, Dr. Miguel Ángel Ibáñez Hernández1,Dra. Beatriz Alvarado Castillo1,
OPEN ACCESS
PUBLISHED: 30 June 2025
CITATION: PACHECO, Dr. Arturo Iván Pérez; HERNÁNDEZ, Dr. Miguel Ángel Ibáñez; CASTILLO, Dra. Beatriz Alvarado. Aberrometric impact in post-cataract surgery patients with high-tech intraocular lenses. Medical Research Archives, [S.l.], v. 13, n. 6, june 2025.Available at: <https://esmed.org/MRA/mra/article/view/6621>.
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i6.6621
ISSN 2375-1924
ABSTRACT
Introduction
Premium intraocular lenses have captured the vision of the most demanding users around the world, however, aberrometric phenomena are the most responsible for patient discomfort when we talk about the quality of life.
Objective
The objective is to evaluate pre surgical high order aberrations and their impact on post-surgical outcome, after cataract surgery with high-tech lenses.
Methods
We present an original, single-center, retrospective, and descriptive study, performed at “Puerta de Hierro” Hospital in Guadalajara, Jalisco, Mexico. Between January 2024 to December 2024, we obtained a total of 43 patients, of which 64 eyes corresponded, whether they had cataract surgery on one or both eyes and with an intraocular premium lens, performed by the same surgeon.
Results
The results consist of 64 eyes, of which 43 patients were evaluated for this study. The demographic distribution was 21 men and 22 women with a mean age of 62.98 ± 4.808 years. The mean pupil diameter in pre-operative surgery conditions in photopic conditions was 3.67 ± 0.64 mm and pre-operative surgery in mesopic conditions was 5.25 ± 0.76 mm. The mean pupil diameter in the post-operative photopic conditions was 3.36 ± 0.54 mm and the post-operative mesopic conditions was 4.63 ± 0.69 mm.
Conclusion
In conclusion the lack of consensus or real or specific information regarding corneal aberrations in premium lenses, motivates this type of study to be possible. The quality of vision compared to previous years was evaluated subjectively, today it can be objectified and promote true visual quality.
Keywords
- Aberrometry
- Cataract surgery
- Intraocular lenses
- High order aberrations
Introduction
Premium intraocular lenses have captured the vision of the most demanding users around the world, however, aberrometric phenomena are the most responsible for patient discomfort when we talk about the quality of life.
There are multiple artifacts or sensations of halos or glare, characterized by occurring in certain lighting conditions and a certain position of incidence, leading to this phenomenon. The values that are disregarded or overlooked in the calculations of different equipment’s, today we know, have a substantial impact on the final visual quality. Such measurements and information related to assessing the pre-surgical values of high-order aberrations (HOA), coma, trefoil, sphere, corneal surface regularity index (SRI), root mean square (RMS), chord m, pupillary dimensions under different conditions, as: mesopic, photopic and scotopic.¹²
Espaillat and colleagues¹¹, the better visual acuity at the time of surgery, the more likely they perceive halos and dysphotopic phenomena than those compared with worse visual acuity within 1 month and 6 months after cataract surgery. In addition to this, it is studied that with great influence, the HOA spherical type was the most prevalent at the time of pseudophakia concerning glare and halos. The documented ranges in microns with a lower incidence of HOA are proposed in values or parameters close to 0.200–0.399 mm, which after 1 month of cataract surgery, have fewer photopic events. Nevertheless, coma HOA, after 6 months was more associated with halos phenomena, that is, the lower the coma, the lower the probability at 6 months of perceiving halos with a proposed value of 0.000–0.199 mm.
On the other hand, an element that is not very associated and that impacts the visual quality, is chord m and its high value or presence (0.30 ± 0.15 mm) with 1 and 6 months of follow-up and the appearance of glare, being in world literature a cut-off value of >0.6 mm, however, not always in a practically measurable way.¹²
Corneal aberrations are defined as a wavefront false image, which derives from Snell’s law and by changing from one medium like water to air or another one and therefore do not constitute a real or true image.²⁶
Low-order corneal aberrations (LOA) are responsible for 85 % of the total aberrations, this means that the remaining 15 % are HOA which cannot be corrected by refractive surgery or spherocylindrical lenses. On the other hand, the most frequent HOA’s are coma and spherical ones. It is well known that the larger the pupil diameter, the larger the HOA’s are going to be. Furthermore, all HOA’s defects are dependent on pupil diameters in different light conditions. The interpretation of the models of the wave light of the light, through mathematics, allows the creation of polynomials, such as the case of the Zernike polynomials, which provide a precise description of these aberrations.¹³¹⁹
The modulation transfer function (MTF), which technological devices would represent, the contrast and sensitivity, allowing a high quality of image definition, in the eye depending on the cornea and providing the different details of an image. The point spread function (PSF), at the level of the occipital cortex, allows evaluation of the intensity of the wave coming from space through the optical system, from the cornea to the retina, thus measuring the final visual quality. Through RMS we can numerically measure the deviations of the light wave when compared with a perfect dioptric system.²⁰²³
The integration of all these elements and their correct interpretation not only allows us to get closer to an ideal visual result, but also to provide data that was not even considered before, which is why high-tech lenses today consider, evaluate and provide key information for the field performance of something more than a simple lens that delivers its dioptric power to see better.
The possibility of considering aberrations in patients who have previously undergone surgery or who have not undergone treatment also allows us to
understand the behavior of intraocular lenses, with a better understanding of their function in conditions that are often difficult even for performing a simple lens calculation.²⁴–²⁶
The objective is to evaluate pre-surgical high order aberrations and their impact on post-surgical outcome, after cataract surgery with high-tech lenses.
Methods
We present an original, single-center, retrospective, and descriptive study, performed at “Puerta de Hierro” Hospital in Guadalajara, Jalisco, Mexico. Between January 2024 to December 2024, we obtained a total of 43 patients, of which 64 eyes corresponded, whether they had cataract surgery on one or both eyes and with an intraocular premium lens, performed by the same surgeon.
The corneal aberrations were measured by the OPD-Scan III which measures corneal topography, wavefront aberrations, autorefraction, keratometry, pupillometry, and same-axis pupillography.
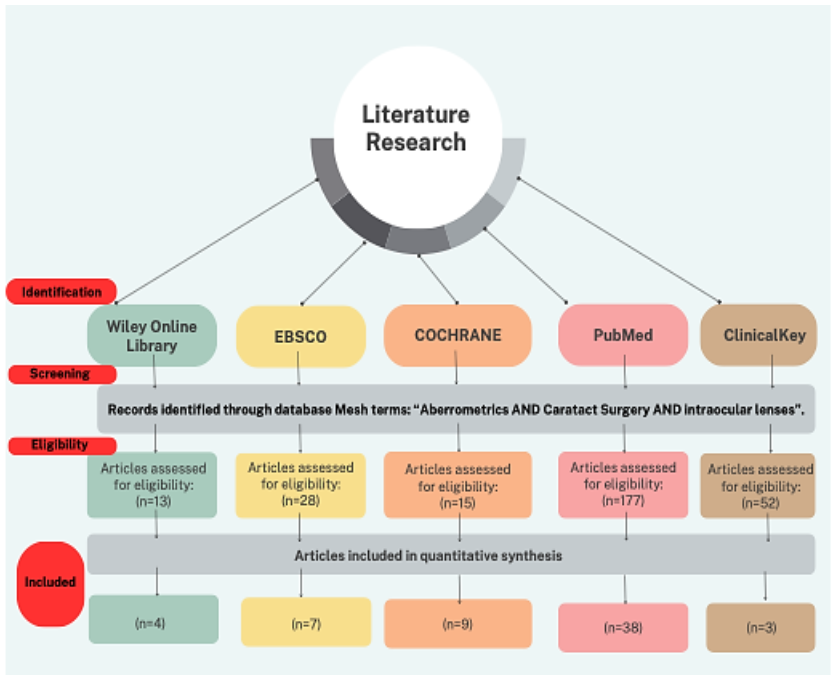
The execution of this original article was possible through metasearch engines like Wiley Online Library, EBSCO, Cochrane, ClinicalKey, and MEDLINE PubMed (National Library of Medicine, National Institutes of Health), to retrieve studies from January 2024 to December 2024, following PRISMA guidelines, with a special affinity to systematic reviews and meta-analysis. MeSH Terms associated with “Aberrometrics AND Cataract Surgery AND Intraocular lenses”. (Figure 1)
After this screening, eligibility criteria were followed according to the inclusion and exclusion criteria, where 13 were filtered from Wiley Online Library, to finally be included, 4. From the EBSCO database, 28 were chosen, to be entered 7. From Cochrane, 15 were chosen, to finally be entered 9. By the PubMed database, most were chosen with criteria but only 38 made the final selection. ClinicalKey with high participation of 52 proposed articles, however with final eligibility criteria of 3.
INCLUSION CRITERIA:
-
The patients with a previous diagnosis of cataract according to the LOCSIII classification criteria, aged 50 years and older.
EXCLUSION CRITERIA:
-
The patients with any corneal pathology, underlying diseases such as glaucoma, pseudoexfoliation, dry eye and retinal pathologies, as well as post-operative refractive surgery such as:
-
Laser-assisted in situ keratomileusis (LASIK)
-
Photorefractive keratectomy (PRK)
-
Small incision lenticule extraction (SMILE)
-
Radiated keratectomy. (Figure 1)
-
This study complies with the Declaration of Helsinki as well as informed consent form from each of the participants. Additionally approved by the ethics committee of the same hospital.
Results
STATISTICAL ANALYSIS:
The results consist of 64 eyes of which 43 patients were evaluated for this study. The demographic distribution was 21 men and 22 women with a mean age of 62.98 ± 4.808 years.
The mean pupil diameter in pre-operative surgery conditions in photopic circumstances was 3.67 ± 0.64 mm and pre-operative surgery in mesopic environment was 5.25 ± 0.76 mm. The mean pupil diameter in the post-operative photopic setting was 3.36 ± 0.54 mm and the post-operative mesopic circumstances was 4.63 ± 0.69 mm. (Table 1 and Figure 2)
On the other hand, the values were distributed not only by being before or after surgery, but also by age groups, as shown in (Table 2 and Figure 3).
The statistical analysis was also carried out by individual corneal aberration for greater precision. (Figure 3–6)
Finally, we compared pupil diameters in mesopic and photopic environments in different age groups. (Figure 7)
Results
| PRE-OPERATIVE SURGERY CONDITIONS | POST-OPERATIVE SURGERY CONDITIONS | |||||||
|---|---|---|---|---|---|---|---|---|
| PHOTOPIC PUPIL | MESOPIC PUPIL | |||||||
| MTF | 60.01 | 24.9 | 60.48 | 25.19 | 60.16 | 20.26 | 58.13 | 19.25 |
| RMS | 2.11 | 8.14 | 2.17 | 1.84 | 0.392 | 0.232 | 0.736 | 0.451 |
| COMA | 0.116 | 0.334 | 0.235 | 0.211 | 0.047 | 0.035 | 0.113 | 0.078 |
| TRI | 0.429 | 1.78 | 0.36 | 0.284 | 0.116 | 0.82 | 0.224 | 0.134 |
| AE | 0.136 | 0.768 | 0.095 | 0.082 | 0.28 | 0.036 | 0.071 | 0.082 |
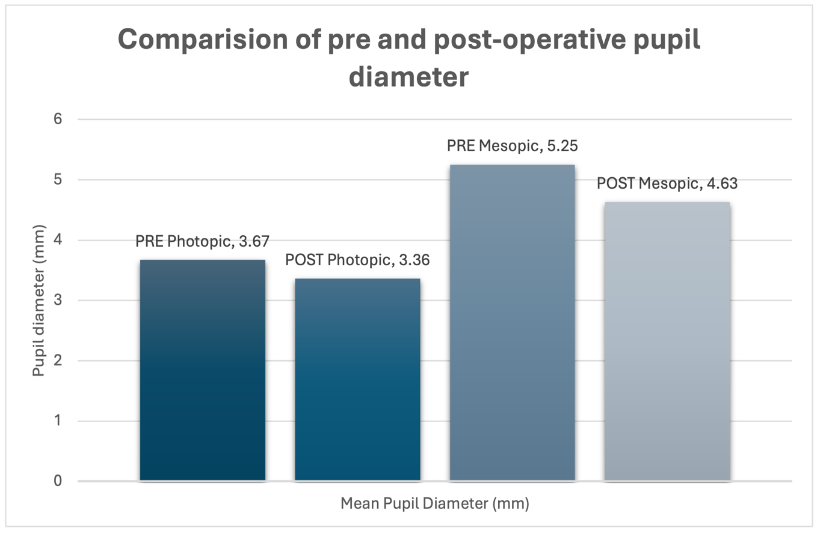
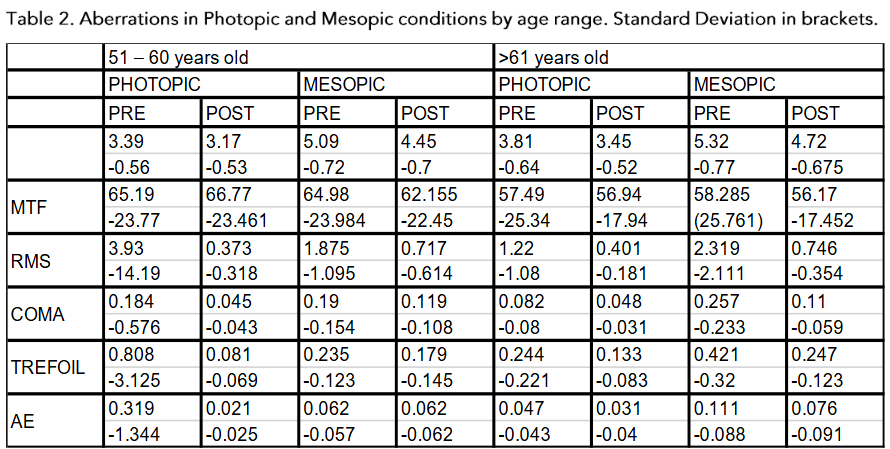
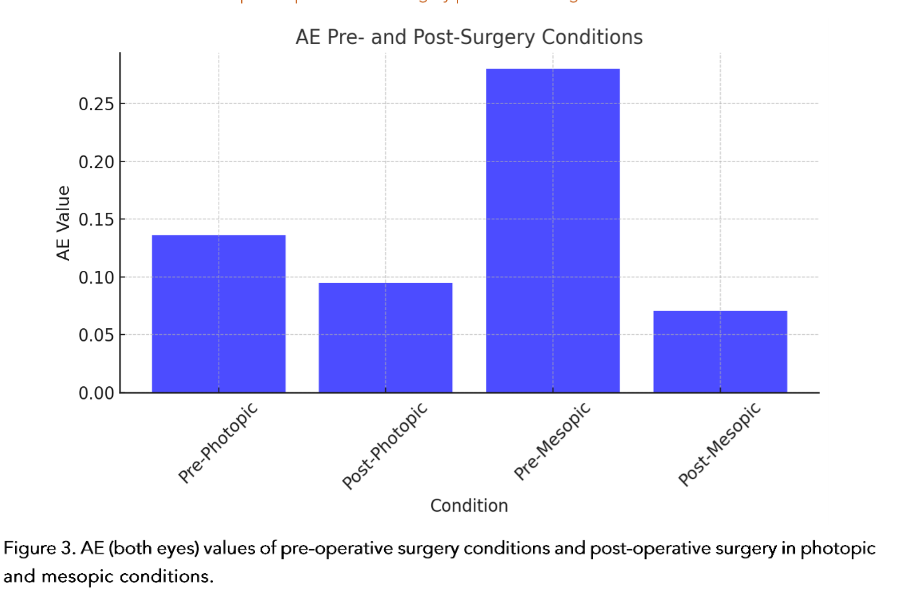
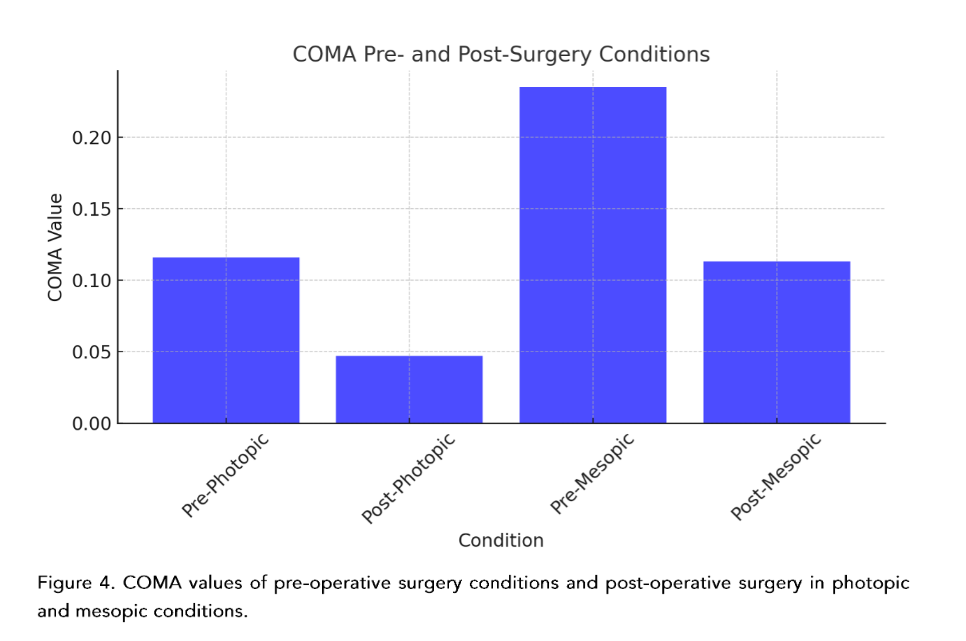
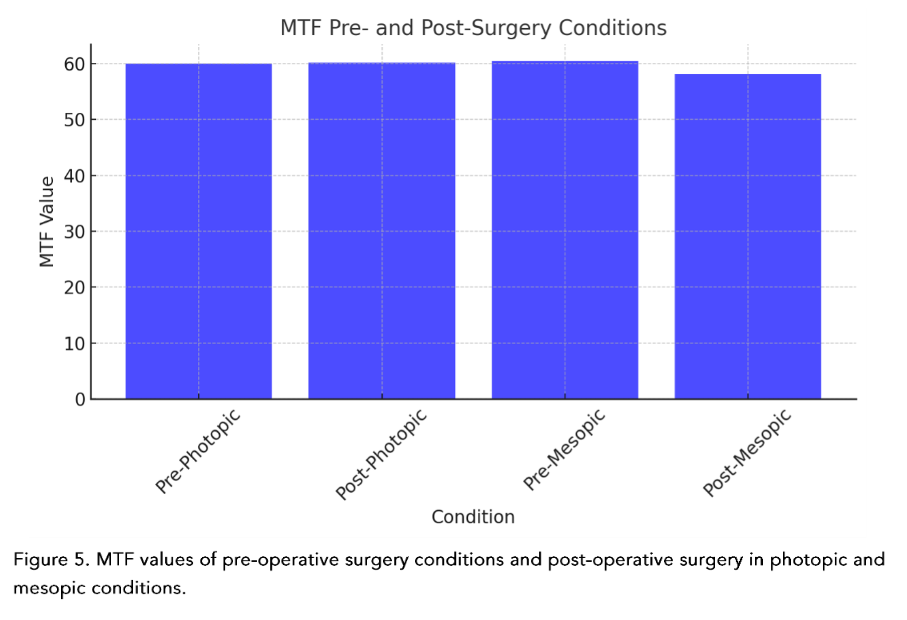
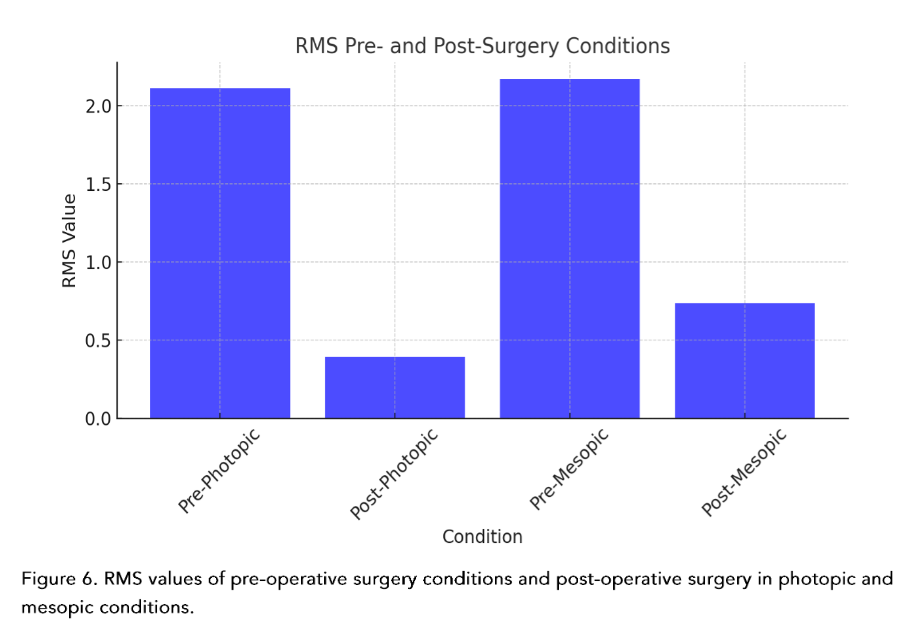
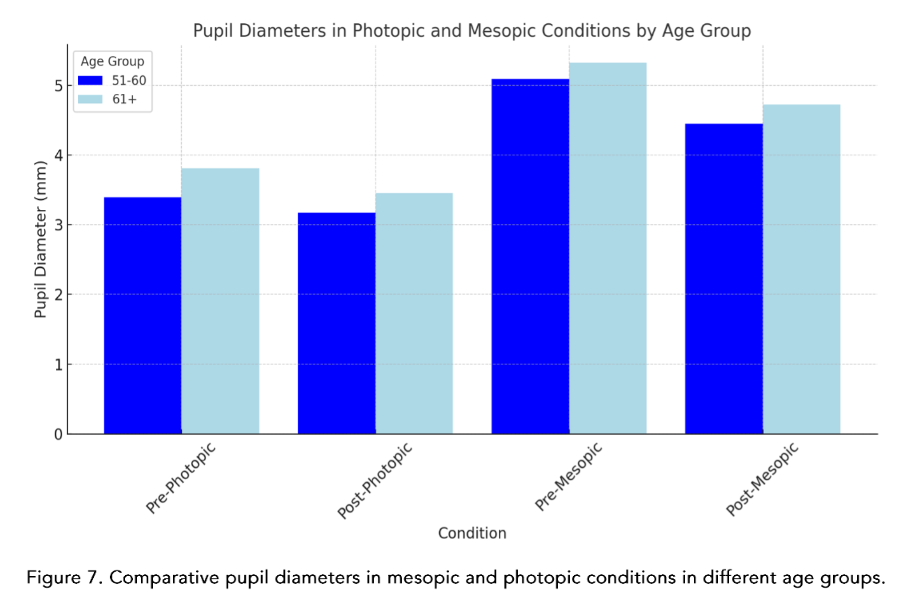
Table 3. Statistically significant P values in photopic and mesopic conditions pre and post-surgery and aberrometric evaluation.
| PHOTOPIC (Pre and Post Surgery Aberrations) | MESOPIC (Pre and Post Surgery Aberrations) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| P Value | MTF | RMS | COMA | TRIFOIL | AE | MTF | RMS | COMA | TRIFOIL | AE |
| 0.965 | 0 | 0.001 | 0.001 | 0.078 | 0.469 | 0 | 0 | 0.002 | 0.022 |
Discussion
Many of the corneal aberration studies consider results as global corneal aberrations. The value of breaking down each one of them allows a finer and more precise analysis. It is important to point out that: off-center shots of the corneal apex, in any of its quadrants, induce corneal aberrations that are not necessarily found in the patient.Since the aberrations are pupil-dependent, we observe that the pre-surgical values in photopic conditions behave differently in the age groups, especially those over 61 years of age. Furthermore, and on the contrary, there is a more stable relationship in post-surgical photopic conditions in relation to the binocular vision evaluation. Interesting description, because as we said previously, the conditions before and after surgery, but by age groups, are not usually united in the same study.²⁷–³³The behavior of coma, in accordance with the universal literature, behaved in an expected manner in photopic and mesopic pre-surgical conditions, where the less pre-surgical coma, the less post-surgical coma, thus benefiting the patient in being the greatest annoying elements in HOA’s.The values found for MTF, furthermore, present a practically linear relationship in the pre-surgical photopic and mesopic condition, and barely decreased in the post-surgical value in mesopic, not so for photopic, allowing to directly associate a stable behavior even after being operated, a notable element for a multifocal and extended-depth-of-focus (EDOF) lenses.³⁴–³⁹The EDOF lenses today have become inherent to a new non-diffractive technology, but they are nevertheless dependent on pupil size for near vision, hence the importance of measuring it, ectopic pupil evaluations and knowing which patients really could benefit from this type of technology.²³The light deviation that we present, evaluated by RMS, in photopic and mesopic pre-surgical conditions was distributed equally, however not for post-surgical conditions, better especially in mesopic conditions.⁴⁰–⁴³The comparison of pupils in diameter, by age group and in the different light conditions, showed to be greater in the group over 61 years of age, data of special attention for us refractive surgeons.One of the most important phenomena when measuring corneal aberrations is decentration and tilt. On the other hand, the same measurement instruments present discrepancies between the equipment when documenting the aberrations. Currently, there is a lack of reliable scientific data evidence about visual quality concerning tilt and decentration. After cataract surgery, the decentration can be 0.2 – 0.3 mm with a tilt of 2–3° degrees, 10% of patients who move more than 0.5 mm or 5° degrees. In vitro, studies of aspheric IOLs present greater decentration and tilt than those compared to spherical ones. In addition, it is completely correlated that the initial decentration or in pre-surgical studies is proportional to the result, and if from the beginning there is no centered IOL, the effective lens position (ELP) will not be accomplished.⁴¹The experimental models, evaluating a cataract surgery or a phaco refractive surgery also impact differently on the aberration wavefront, since in young patients, the positive spherical aberrations coming from the cornea are counteracted due to the aberrometric negative spherical power of the transparent natural lens, phenomenon that, on the contrary, occurs in cataracts in senile patients, leading to a final distortion of visual quality.⁴⁴–⁴⁶On the other hand, the dispersion of the material must be considered, since the manufacture of IOLs is usually under conditions of monochromatic green spectrum, it is necessary to introduce the measure of the Abbe number, allows the direct correlation that could be quantified, and result that the lower the Abbe number, the greater will be the dispersion color, translating this into a chromatic wavelength aberration. However, this longitudinal chromatic aberration induced by the lens itself allows us to describe the inability of the visual system to refract the propagation of light and the color spectrum to the same focal point.⁴⁷–⁵⁰The Femtosecond laser-assisted cataract surgery (FLACS), being able to guarantee the effective position of the intraocular lens during surgery is more precise today thanks to the application of these new technologies. It has been studied over the years, the substantial difference that exists in the immediate and long-term postoperative period, when performed conventionally phacoemulsification surgery. On the other hand, the HOA and spherical aberrations are lower in FLACS, in addition to contributing substantially to the lower amount of decentration and thus the tilt.⁵¹–⁵⁸The replicability capacity of FLACS made it objective, repetitive and forceful, the aberrations studied are in measurements of size, shape and position, comparable and therefore predictable. Thus, making a smaller sum of total aberrations at the end.⁵¹–⁵⁸ the aberration value and thus the final clinical behavior, allows us to globally anticipate its result.⁵⁹On the other hand, it seems that comparing trefoil vs spherical at 6 months, the trefoil aberration is higher at the end of this time. In addition, we find one more variable, which is little studied or documented when talking about HOA’s: it is the type of intraocular lens and its aspherical and spherical shape, the first being the one with the lowest aberration index.⁵⁹–⁶⁰Documenting the difference that exists between multifocal and monofocal intraocular lenses, in addition with the pupil diameter, interestingly allows us to distinguish that in FLACS there are higher MTF values than in conventional cataract surgery when starting from a pupil diameter of 4.5 mm. Thus, concluding that these patients are the ones who will clinically show better visual acuity.⁵⁶–⁵⁷As J. Miret³⁶ and colleagues said, positive spherical aberrations are produced by spherical surfaces, while with aspheric surfaces, they can be only controlled. There are elements that were previously explored as possible and today constitute a reality, such as the case of the design of trifocal lenses, whose diffractive base is curved but constitutes at the end a spherical surface.³⁶Another important element is that in all studies, the refractive target is suggested to be 0.5 D, however this is done by spherical equivalent, being this an area of opportunity because many sums could give that final refractive value, without this meaning truly good final visual acuity for the patients.¹The advancement of technology with respect to artificial intelligence has reached ophthalmology. The need to predict and alert errors has allowed it to be used to prevent refractive surprises. It was documented that when choosing the Barrett True K and Hill formula RBF (radial basis function) they are equiparable between each other as they are targeting a refractive target of 0.5 D.⁵In addition, like Alba-Bueno and cols¹, when comparing 5 diffractive IOL’s, it was demonstrated that the greater the addition of power to the lens, the greater the sensation and size of the halos reported by the patient. This is of great value since we can uniquely specify the need for an accurate calculation.For a long time throughout the development of intraocular lenses, the possibility raised that internal aberrations were typical of the IOL; however, today it has been shown that they do not actively participate in this light dispersion and therefore the HOA’s, spherical and coma, were not the most disabling.²²Personalized medicine is becoming more and more real in ophthalmology, where the visual needs of each patient are different. Knowing and having the best information available at the time of surgery allows having a direct and substantial impact, with the selected lens, according to each type of patient.⁵⁸–⁶¹
Conclusion
In conclusion the lack of consensus or real specific information regarding corneal aberrations in premium lenses, motivates this type of study to be possible. The quality of vision compared to previous years was evaluated subjectively; today it can be objectified and promote true visual quality. Knowing the specific characteristics of the IOL as well as its properties today constitutes a different starting point to understand their correction and explain the great world of corneal aberrations.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Alba-Bueno F, Garzón N, Vega F, Poyales F, Millán MS. Patient-Perceived and Laboratory-Measured Halos Associated with Diffractive Bifocal and Trifocal Intraocular Lenses. Current Eye Research. 2017;43(1):35-42. doi:10.1080/02713683.2017.13 79541.
2. Alio JL, D’Oria F, Toto F, et al. Retinal image quality with multifocal, EDoF, and accommodative intraocular lenses as studied by pyramidal aberrometry. Eye And Vision. 2021;8(1). doi:10.1186/s 40662-021-00258-y.
3. Alió JL, Kaymak H, Breyer D, Cochener B, Plaza‐Puche AB. Quality of life related variables measured for three multifocal diffractive intraocular lenses: a prospective randomised clinical trial. Clinical and Experimental Ophthalmology. 2017; 46(4):380-388. doi:10.1111/ceo.13084.
4. Ashena Z, Gallagher S, Naveed H, Spalton DJ, Nanavaty MA. Comparison of Anterior Corneal Aberrometry, Keratometry and Pupil Size with Scheimpflug Tomography and Ray Tracing Aberrometer. Vision. 2022;6(1):18. doi:10.3390/vis ion6010018.
5. Bhasin P, Sarkar D, Bhasin P, Dhanapal PP, Ubhal GN, Bhargava M. Visual performance and patient satisfaction with AcrySof® IQ Vivity® IOL: Experience from a tertiary care center in central India. Indian Journal of Ophthalmology. 2024;72 (4):554-557. doi:10.4103/ijo.ijo_1018_23.
6. Castillo RA, Hernández QE. Aberraciones corneales de alto orden. ¿Un método para graduar al queratocono? Rev Mex Oftalmol. 2008;82(6): 369-375.
7. Cerviño A, Esteve-Taboada JJ, Chiu YF, Yang CH, Tseng WC, Lee W. Tolerance to decentration of biaspheric intraocular lenses with refractive phase-ring extended depth of focus and diffractive trifocal designs. Graefe S Archive for Clinical and Experimental Ophthalmology. 2024; 262(8):2541-2550. doi:10.1007/s00417-024-06458-1.
8. Chen AJ, Long CP, Lu T, Garff KJ, Heichel CW. Accuracy of intraoperative aberrometry versus modern preoperative methods in post-myopic laser vision correction eyes undergoing cataract surgery with capsular tension ring placement. Graefe S Archive for Clinical and Experimental Ophthalmology. 2023;262(5):1545-1552. doi:10.100 7/s00417-023-06327-3.
9. Chen JL, Al-Mohtaseb ZN, Chen AJ. Criteria for premium intraocular lens patient selection. Curr Opin Ophthalmol. 2024;35(5):353-358. doi:10.1097/ ICU.0000000000001067.
10. Chuck RS, Jacobs DS, Lee JK, et al. Refractive Errors & Refractive Surgery Preferred Practice Pattern®. Ophthalmology. 2017;125(1):P1-P104. doi:10.1016/j.ophtha.2017.10.003.
11. Danzinger V, Schartmüller D, Schwarzenbacher L, et al. Clinical prospective intra-individual comparison after mix-and-match implantation of a monofocal EDOF and a diffractive trifocal IOL. Eye. 2023;38(2):321-327. doi:10.1038/s41433-023-02682-x.
12. Espaillat A, Coelho C, Batista MJM, Perez O. Predictors of Photic Phenomena with a Trifocal IOL. Clinical Ophthalmology. 2021;Volume 15: 495-503. doi:10.2147/opth.s282469.
13. Fernández J, Rodríguez-Vallejo M, Martínez J, Burguera N, Piñero DP. Prediction of visual acuity and contrast sensitivity from optical simulations with multifocal intraocular lenses. Journal of Refractive Surgery. 2019;35(12):789-795. doi:10.3928/1081597x-20191024-01.
14. Fu Y, Kou J, Chen D, et al. Influence of angle kappa and angle alpha on visual quality after implantation of multifocal intraocular lenses. Journal of Cataract & Refractive Surgery. 2019; 45(9):1258-1264. doi:10.1016/j.jcrs.2019.04.003.
15. Furlan WD, Martínez-Espert A, Montagud-Martínez D, Ferrando V, García-Delpech S, Monsoriu JA. Optical performance of a new design of a trifocal intraocular lens based on the Devil’s diffractive lens. Biomedical Optics Express. 2023; 14(5):2365. doi:10.1364/boe.487812.
16. García S, Salvá L, García-Delpech S, Martínez-Espert A, Ferrando V. Numerical analysis of the effect of decentered Refractive Segmented Extended Depth of Focus (EDOF) intraocular lenses on predicted visual outcomes. Photonics. 2023;10 (7):850. doi:10.3390/photonics10070850.
17. Garzón N, García-Montero M, López-Artero E, Poyales F, Albarrán-Diego C. Influence of trifocal intraocular lenses on standard autorefraction and aberrometer-based autorefraction. Journal of Cataract & Refractive Surgery. 2019;45(9):1265-1274. doi:10.1016/j.jcrs.2019.04.017.
18. Gatinel D, Rampat R, Dumas L, Malet J. An alternative wavefront reconstruction method for human eyes. Journal of Refractive Surgery. 2020; 36(2):74-81. doi:10.3928/1081597x-20200113-01.
19. Gatinel D, Rampat R, Malet J, Dumas L. Wavefront sensing, novel lower degree/higher degree polynomial decomposition and its recent clinical applications: A review. Indian Journal of Ophthalmology. 2020;68(12):2670. doi:10.4103/I jo.ijo_1760_20.
20. Huh J, Eom Y, Yang SK, Choi Y, Kim HM, Song JS. A comparison of clinical outcomes and optical performance between monofocal and new monofocal with enhanced intermediate function intraocular lenses: a case-control study. BMC Ophthalmology. 2021;21(1). doi:10.1186/s12886-021-02124-w.
21. Huang CY, Pu C, Hou CH. Premium intraocular lens adoption: Insights from a national health insurance analysis. J Formos Med Assoc. Published online August 7, 2024. doi:10.1016/j.j fma.2024.07.027.
22. Imburgia A, Gaudenzi F, Mularoni K, Mussoni G, Mularoni A. Comparison of clinical performance and subjective outcomes between two diffractive trifocal intraocular lenses (IOLs) and one monofocal IOL in bilateral cataract surgery. Frontiers in Bioscience-Landmark. 2022;27(2):041. doi:10.31083/j.fbl2702041.
23. Ishiguro N, Horiguchi H, Katagiri S, Shiba T, Nakano T. Correlation between higher-order aberration and photophobia after cataract surgery. PLoS ONE. 2022;17(9):e0274705. doi:10.1371/jour nal.pone.0274705.
24. Jameel A, Dong L, Lam CFJ, et al. Attitudes and understanding of premium intraocular lenses in cataract surgery: a public health sector patient survey. Eye. 2023;38(1):76-81. doi:10.1038/s41433-023-02633-6.
25. Jeon S, Choi A, Kwon H. Analysis of uncorrected near visual acuity after extended depth-of-focus AcrySof® VivityTM intraocular lens implantation. PLoS ONE. 2022;17(11):e0277687. doi:10.1371/journal.pone.0277687.
26. Kawamura J, Tanabe H, Shojo T, Yamauchi T, Takase K, Tabuchi H. Comparison of visual performance between diffractive bifocal and diffractive trifocal intraocular lenses. Scientific Reports. 2024;14(1). doi:10.1038/s41598-024-55926-5.
27. Kim JW, Eom Y, Bae SH, et al. Visual outcomes according to age after bilateral implantation of trifocal intraocular lenses. Journal of Refractive Surgery. 2024;40(4). doi:10.3928/1081597x-2024 0314-03.
28. La Cruz DZD, Garzón M, Pulido-London D, et al. Trifocal intraocular lenses versus bifocal intraocular lenses after cataract extraction. Cochrane Library. May 2017. doi:10.1002/14651858.cd012648.
29. Łabuz G, Güngör H, Auffarth GU, Yildirim TM, Khoramnia R. Altering chromatic aberration: how this latest trend in intraocular-lens design affects visual quality in pseudophakic patients. Eye And Vision. 2023;10(1). doi:10.1186/s40662-023-00367-w.
30. Łabuz G, Yan W, Baur ID, Khoramnia R, Auffarth GU. Comparison of Five Presbyopia-Correcting Intraocular Lenses: Optical-Bench Assessment with Visual-Quality Simulation. Journal of Clinical Medicine. 2023;12(7):2523. doi:10.339 0/jcm12072523.
31. Li LP, Yuan LY, Mao DS, Hua X, Yuan XY. Systematic bibliometric analysis of research hotspots and trends on the application of premium IOLs in the past 2 decades. International Journal of Ophthalmology. 2024;17(4):736-747. doi:10.18240/i jo.2024.04.19.
32. Liu X, Wu X, Huang Y. Laboratory evaluation of halos and Through-Focus performance of three different multifocal intraocular lenses. Journal of Refractive Surgery. 2022;38(9):552-558. doi:10.39 28/1081597x-20220802-02.
33. Ma DK, Fan YY, Sun CC, Chen HC. Photorefractive keratectomy for correcting residual refractive error following cataract surgery with premium intraocular lens implantation. Taiwan Journal of Ophthalmology. 2018;8(3):149. doi:10.4 103/tjo.tjo_51_18.
34. Ma J, El-Defrawy S, Lloyd J, Rai A. Prediction accuracy of intraoperative aberrometry compared with preoperative biometry formulae for intraocular lens power selection. Canadian Journal of Ophthalmology. 2021;58(1):2-10. doi:10.1016/j.j cjo.2021.06.024.
35. Markuszewski B, Wylęgała A, Szentmáry N, Langenbucher A, Markuszewska A, Wylęgała E. Comparative Analysis of the Visual, Refractive and Aberrometric Outcome with the Use of 2 Intraocular Refractive Segment Multifocal Lenses. Journal of Clinical Medicine. 2023;13(1):239. doi:10.3390/jcm13010239.
36. Miret JJ, Camps VJ, García C, Caballero MT, Gonzalez-Leal JM. Analysis and comparison of monofocal, extended depth of focus and trifocal intraocular lens profiles. Scientific Reports. 2022; 12(1). doi:10.1038/s41598-022-12694-4.
37. Ni S, Zhuo B, Cai L, et al. Visual outcomes and patient satisfaction after implantations of three types of presbyopia-correcting intraocular lenses that have undergone corneal refractive surgery. Scientific Reports. 2024;14(1). doi:10.1038/s41598-024-58653-z.
38. Niazi S, Gatzioufas Z, Dhubhghaill SN, et al. Correction to: Association of Patient Satisfaction with Cataract Grading in Five Types of Multifocal IOLs. Advances in Therapy. 2024;41(4):1774. doi:10.1007/s12325-024-02804-1.
39. Ning J, Zhang Q, Liang W, et al. Bibliometric and visualized analysis of posterior chamber phakic intraocular lens research between 2003 and 2023. Frontiers in Medicine. 2024;11. doi:10.3389/fmed.2024.1391327.
40. Palomino-Bautista C, Sánchez-Jean R, Carmona-Gonzalez D, Piñero DP, Molina-Martín A. Depth of field measures in pseudophakic eyes implanted with different type of presbyopia-correcting IOLS. Scientific Reports. 2021;11(1). doi:10.1038/s41598-021-91654-w.
41. Palomino-Bautista C, Sánchez-Jean R, Carmona-González D, Piñero DP, Molina-Martín A. Subjective and objective depth of field measures in pseudophakic eyes: comparison between extended depth of focus, trifocal and bifocal intraocular lenses. International Ophthalmology. 2019;40(2): 351-359. doi:10.1007/s10792-019-01186-6.
42. Pan RL, Tan QQ, Liao X, et al. Effect of decentration and tilt on the in vitro optical quality of monofocal and trifocal intraocular lenses. Graefe S Archive for Clinical and Experimental Ophthalmology. 2024;262(10):3229-3242. doi:10.10 07/s00417-024-06490-1.
43. Pedrotti E, Carones F, Talli P, et al. Comparative analysis of objective and subjective outcomes of two different intraocular lenses: trifocal and extended range of vision. BMJ Open Ophthalmology. 2020;5(1):e000497. doi:10.1136/b mjophth-2020-000497.
44. Pérez-Merino P, Aramberri J, Quintero AV, Rozema JJ. Ray tracing optimization: a new method for intraocular lens power calculation in regular and irregular corneas. Scientific Reports. 2023;13(1). doi:10.1038/s41598-023-31525-8.
45. Qu H, Abulimiti A, Liang J, et al. Comparison of short-term clinical outcomes of a diffractive trifocal intraocular lens with phacoemulsification and femtosecond laser assisted cataract surgery. BMC Ophthalmology. 2024;24(1). doi:10.1186/s1 2886-024-03440-7.
46. Rementería-Capelo LA, Contreras I, Morán A, Lorente-Hevia P, Mariñas L, Ruiz-Alcocer J. Visual Performance of Eyes with Residual Refractive Errors after Implantation of an Extended Vision Intraocular Lens. Journal of Ophthalmology. 2023; 2023:1-5. doi:10.1155/2023/7701390.
47. Salgado RMPC, Torres PF a. a. S, Marinho A a. P. Pupil versus 1st Purkinje capsulotomy centration with femtosecond laser: Long term outcomes with a sinusoidal trifocal lens. Journal of Biophotonics. 2024;17(5). doi:10.1002/jbio.20230 0446.
48. Seiler TG, Wegner A, Senfft T, Seiler T. Dissatisfaction after trifocal IOL implantation and its improvement by selective Wavefront-Guided LASIK. Journal of Refractive Surgery. 2019;35 (6):346-352. doi:10.3928/1081597x-20190510-02.
49. Sezenöz AS, Güngör SG, Doğan İK, Çolak MY, Gökgöz G, Altınörs DD. The effect of trifocal and extended-depth-of-focus intraocular lenses on optical coherence tomography parameters. Indian Journal of Ophthalmology. 2024;72(Suppl 3):S423-S428. doi:10.4103/ijo.ijo_1938_23.
50. Son HS, Labuz G, Khoramnia R, Merz P, Yildirim TM, Auffarth GU. Ray propagation imaging and optical quality evaluation of different intraocular lens models. PLoS ONE. 2020;15(2):e0228342. doi:10.1371/journal.pone.0228342.
51. Solli EM, Prescott CR. Impact of Patient Race/Ethnicity on Premium Intraocular Lens Utilization. Eye Contact Lens. 2024;50(9):406-409. doi:10.1097/ICL.0000000000001112.
52. Vidal Olarte R. Entendiendo e interpretando las aberraciones ópticas. Cienc Tecnol Salud Vis Ocul. 2011;(2): 105-122. https://ciencia.lasalle.edu.co/svo/vol9/iss2/10.
53. Villegas EA, Manzanera S, Lago CM, Hervella L, Sawides L, Artal P. Effect of crystalline lens aberrations on adaptive optics simulation of intraocular lenses. Journal of Refractive Surgery. 2019;35(2):126-131. doi:10.3928/1081597x-20181 212-02.
54. Wang JM, Che JB, Yuan XW, Zhang JB. [Effects of different types of intraocular lens implantation on patient’s visual quality and function after phacoemulsification]. PubMed. 2024;104(16): 1391-1396. doi:10.3760/cma.j.cn112137-20231125-01198.
55. Xiong J, Xu J, Zhou M, et al. Mesopic pupil indices as potential risk factors for glare disability after intraocular implantable collamer lens implantation: prospective study. Journal of Cataract & Refractive Surgery. 2024;50(6):565-571. doi:10.1097/j.jcrs.0000000000001420.
56. Xu J, Zheng T, Lu Y. Effect of decentration on the optical quality of monofocal, extended depth of focus, and bifocal intraocular lenses. Journal of Refractive Surgery. 2019;35(8):484-492. doi:10.392 8/1081597x-20190708-02.
57. Yan W, Łabuz G, Khoramnia R, Auffarth GU. Trifocal intraocular lens selection: predicting visual function from optical quality measurements. Journal of Refractive Surgery. 2023;39(2):111-118. doi:10.39 28/1081597x-20221207-02.
58. Zhong Y, Wang K, Yu X, Liu X, Yao K. Comparison of trifocal or hybrid multifocal-extended depth of focus intraocular lenses: a systematic review and meta-analysis. Scientific Reports. 2021;11(1). doi:10.1038/s41598-021-86222-1.
59. Zhong Y, Zhu Y, Wang W, Wang K, Liu X, Yao K. Femtosecond laser-assisted cataract surgery versus conventional phacoemulsification: comparison of internal aberrations and visual quality. Graefe S Archive for Clinical and Experimental Ophthalmology. 2021;260(3):901-911. doi:10.1007/s00417-021-05 441-4.
60. Zhou S, De Almeida Figueiredo AG, Abulimiti A, Hida WT, Chen X. Evaluation of Life Quality of Patients Submitted to Cataract Surgery with Implantation of Trifocal Intraocular Lenses. Journal of Personalized Medicine. 2023;13(3):451. doi:10.3390/jpm13030451.
61. Zvorničanin J, Zvorničanin E. Premium intraocular lenses: The past, present and future. Journal of Current Ophthalmology. 2018;30(4): 287-296. doi:10.1016/j.joco.2018.04.003.

