Biomedical Engineering’s Impact on Pediatric Care
The Role of Biomedical Engineering in the Life of a Paediatrician
Pieter Rousseau Fourie
Paediatric Consultant at Rustenvrede Optima Psychiatric Hospital, Biomedical Engineer Innovus Stellenbosch University, South Africa.
Johanna J. Koen
Research Assistant to Dr. Fourie. South Africa.
OPEN ACCESS
PUBLISHED: 31 July 2025
CITATION Fourie, R., P., Koen, J., J., The Role of Biomedical Engineering in the Life of a Paediatrician. Medical Research Archives, [online] 13(7). https://doi.org/10.18103/mra.v13i8.6816
COPYRIGHT © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i8.6816
ISSN 2375-1924
ABSTRACT
As in many scientific fields, the increased benefit of biomedical engineering has brought a paradigm shift in the manner in which physicians, and in particular paediatricians, are able to support their patients. The tempo of new applications being introduced, especially with the introduction of artificial intelligence to support diagnosis, has skyrocketed and the end is still not in sight. This is exciting times and for the paediatrician it brings a number of support systems to enhance diagnostic accuracy and improved management. This article highlights some of the rapid developments in biomedical engineering including microelectronics, AI-supported diagnostics, organ transplantation and advances in cancer treatment to name a few.
Keywords
- Biomedical Engineering
- Paediatrics
- Artificial Intelligence
- Diagnostics
- Microelectronics
- Organ Transplantation
- Cancer Treatment
Introduction
Over the past 2000 years, the science of medicine has progressed with leaps and bounds especially since the introduction of electricity, the discovery of micro-organisms and the development of pharmacological agents. The last three decades have been specifically noted for the influence of computers, micro-electronics as well as the internet and recently the advent of artificial intelligence (AI), which have opened up unlimited information made available to the physician to assist in reaching a definitive diagnosis, managing the disease via a multitude of therapeutic modalities and monitoring progress effectively. Nowhere has this become more apparent than in the paediatric practice where the outcome of any result would not only affect the quality of child’s life, but also that of the close family and caretakers. This article will highlight the various fields of medical science and how bioengineering has changed and sculpted the present-day paediatric practice as well as a view on what the future will hold. Although not directly involved, such as cancer treatment and heart transplants, the paediatrician is indirectly involved in managing these cases on a day-to-day basis. Refer to Table 1.
Before we venture into the future let us allow ourselves to have a look at a day in the life of a paediatrician. The mobile phone has replaced the stand-alone phone and pagers making it easy to receive calls and respond to emergency cases. More so, it allows the user to have direct access to emails and documents which can be rerouted to colleagues and associates. Patient files can be accessed via a dedicated hospital, or government platform as well as clinical information such as blood and other laboratory results and include radiographic information, e.g., X-rays and MRI reports. Prescriptions can be sent via a security mobile phone app. The cost saving regarding waiting time required is significant. The most important benefit is to the patient who does not have to wait long hours before results or special investigations can be discussed and acted upon. Obviously, the paediatrician has more time available to focus on reaching a diagnosis as well as shortening the time before the patient can be treated.
Table 1. Technology Available to Paediatricians
| Technology | Present | Future |
|---|---|---|
| Cardiovascular | Holter monitoring | Skin patch embedded sensors |
| Respiratory | Stethoscope | Micro-electronics |
| EEG | Contact electrodes | Intra-ear EEG |
| Diabetes | Glucose monitoring and insulin delivery | AI optimisation |
| Hearing | Bionic devices | AI informatics |
| Pharmacology | Pharmacogenomics | Patient-specific drug design |
| Radiology | X-ray, ultrasound, CT scan, MRI | AI diagnostics and mobile MRI |
| Vision | Computer assist devices | Bionic vision |
| Metabolic disorders | Blood analysis | CRISP/Cas9 |
| Oncology | Genetic profiling drug delivery | Immunotherapy, CAR-T |
| Transplant | Heart, lung, kidney | Artificial organs |
| Neuropathology | Biofeedback, IR monitoring | Intracranial monitoring and diagnostics |
Biomedical Engineering Technology
At the present moment, paediatricians will rely mostly on auscultation to detect any respiratory or cardiac abnormalities. The latest in stethoscope development allows the user to amplify and filter heart and breathing sounds as well as real-time electrocardiogram (ECG) information, download the data via Bluetooth to a web-based app and then email to a colleague for further assessment. Standard ECG registration and Holter monitoring and Loop recording are presently readily available and includes built in diagnostic capabilities. Future stethoscope development will include advanced AI diagnostic reports especially with regard to respiratory sounds and heart murmurs, again allowing the paediatrician to make real time decisions regarding further management. Holter monitors will be replaced with a skin patch that incorporates embedded micro-electronics.
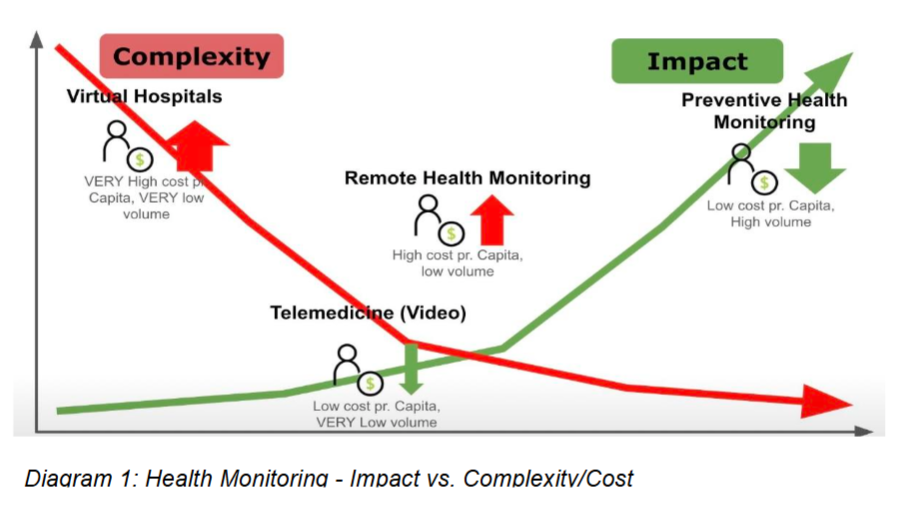
AI has entered the arena of special investigations acting in the background of laboratory results as well as radiographic screening and interpretation but now also moving into everyday applications such as auscultation for heart murmurs, dysrhythmias and lung sounds and assisting medical personnel to make an early and preliminary diagnosis without having to transfer the patient to a tertiary care centre. The application of data science on a broader level will benefit a significant number of applications of which its predictive capacity is probably the most exciting. Heart rate variability has already been demonstrated to operate as an “early warning” signal that will alert the paediatrician of an impending infection or crisis long before the patient presents with symptoms. See Diagram 1 below indicating the financial benefit of remote monitoring as a preventative technological support.
Bionic Cochlear implants are now standard in cases of extreme deafness. The future will include devices with more electrodes as well as AI supported sound and volume adaptation with frequency filtering whilst moving from a quiet room to a meeting or conference with all round noise impacting on the ability to identify the voice of the speaker. The quantum jump will be in the commercialization of bionic eyes. A number of options are presently being investigated including AI driven miniature cameras attached to glasses with an auditory output warning the user of an obstacle, intraocular charged coupled devices (CCD) implantation with stimulation of the ocular nerve and intracranial sensors placed on the visual cortex.
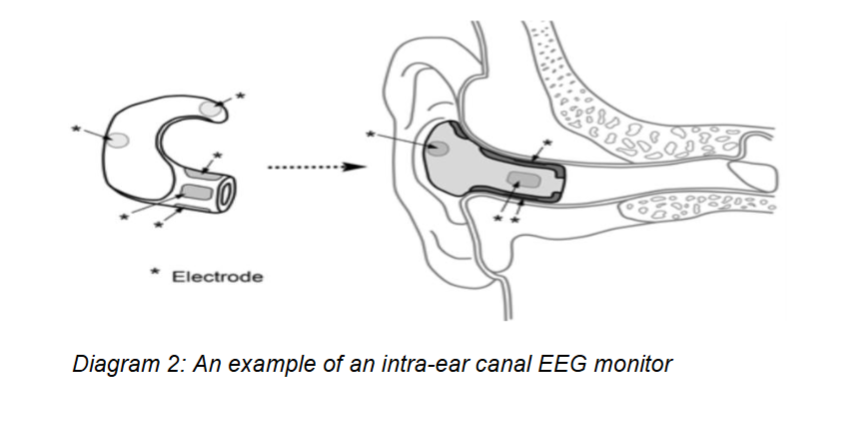
Electroencephalogram (EEG) monitoring has come a long way since the previous century. Mobile EEG monitoring is now standard and can be ordered from a reputable electrophysiologist. However, it is still a cumbersome procedure with the electrodes having to be attached to the scalp and results in quite a messy clean-up afterwards. Contactless electrodes are available, but signal detection is often hindered due to bulky hair styles. Intra-ear EEG monitoring applying Fast Fourier transform (FFT) analysis has demonstrated to be accurate in detecting cortical EEG activity. Although not as accurate in localization compared to the standard array of EEG electrodes, it has the advantage of being highly comfortable, aesthetically acceptable and will allow the user to be monitored during sleep, anaesthesia as well as during work and school hours. It can also detect sedation, drowsiness, drug overdose, tiredness and act as an early warning signal for convulsions, epilepsy and mood derangements.
Especially in the field of neurodiversity, patients are often on multiple drugs for various reasons. These may include stimulants such as methylphenidate or Lizdexamphetamine to improve concentration, anti-epileptic medications such as sodium valproate or lamotigine as a mood stabilizer, antidepressants i.e. selective serotonin reuptake inhibitors (SSRI’s) or mono-amine oxidase inhibitors (MOI) e.g. Sertraline or Ethipramine to lessen anxiety, or anti-psychotics such as Respiridone or Ziprasidone to modify behaviour. Until recently the paediatrician or psychiatrist had to gauge the response based on feedback from the patient or guardian and if the patient complained of specific side-effects, the paediatrician had to work through a conglomerate of side-effects potentially related to each drug as well as the interaction the drugs would have on each other. Often, he/she would then have to trial and error hoping to find the ideal combination for the individual patient. The recent introduction of pharmacogenomics, where all the drugs used by the patient are matched against the patient’s genetic profile, has made this conundrum significantly easier and will lead to less side-effects, improved efficacy and patient compliance. The future will be even more promising leading to patient specific drug design and profiling.
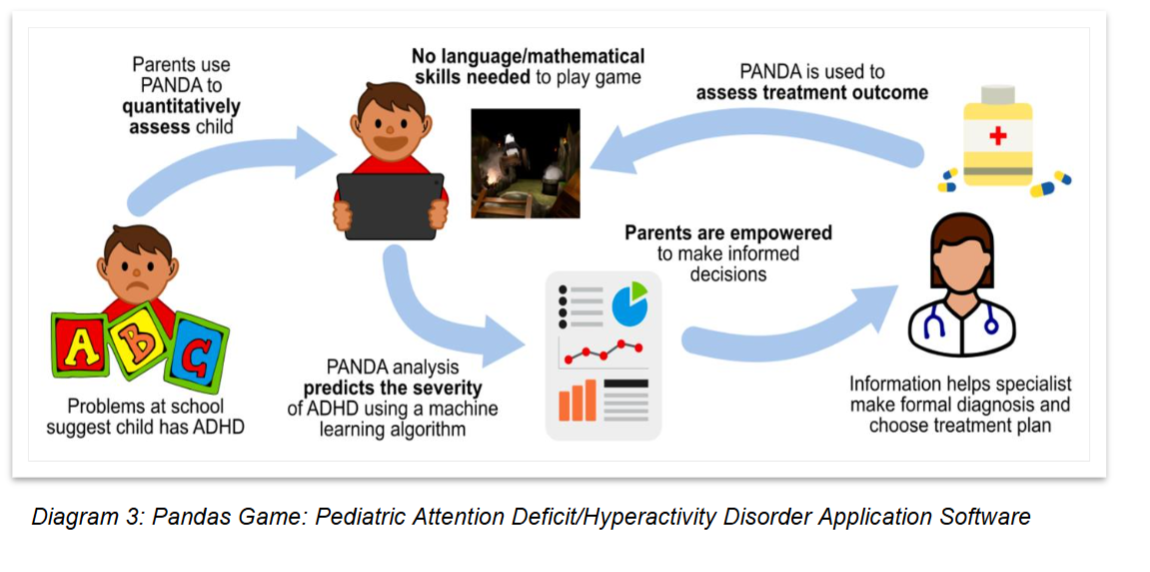
The diagnosis of patients with attention deficit hyperactivity disorder (ADHD) is still complex, costly and subjective where the diagnosis is made after an extensive review of a psychological assessment, and reports such as the Swan and Snap IV. In the developing world, these patients often go undetected adding to the financial burden of a government to support them throughout their academic and working career. Simple and accurate AI driven alternatives are emerging which will not only support the paediatrician in making a quick and objective assessment but will aid in the monitoring and response to medication.
Maybe the brightest future lies in the area of transplant technology. Not only the potential of genetically modified animal organs to negate the possibility of rejection, but the growth of stem cell derived organs as well as mechanical artificial hearts, lungs, kidneys, pancreas β-cells and liver organs.
Biofeedback applying EEG or infrared (IR) analysis, a technique to improve concentration or mood modification, has been available for a decade or two. Intracranial implants to stabilize epilepsy has become a safe and effective method to control recalcitrant convulsions. Transcranial stimulation has recently been added to the treatment armamentarium as an option to treat depression. The advent of brain-computer interface has opened up an unlimited potential of applications. The more obvious application is in assisting quadriplegic patients to communicate effectively. However, the support in modifying behavior in neurodiverse patients, decreasing the need for mood stabilizers such as anti-psychotics, deep neural stimulation in anxiety and depression are some of the benefits that brain-computer interface will hold.
Metabolic disorders include a wide range of genetic abnormalities that affect metabolic pathways between organs such Phenylketonuria (PKU) and Insulin Dependent Diabetes Mellitus (IDDM) as well as within cells such as mitochondrial disorders e.g., Leigh syndrome. Till recently the management has focused mainly on supporting the patient with dietary modifications and physical support, e.g., occupational and physiotherapy. Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR) is a gene-editing technology that allows scientists to modify DNA sequences in living cells and organisms. It is based on a bacterial immune system that uses CRISPR and CRISPR-associated protein 9 (Cas9) to defend against viruses. This technology has revolutionized biomedical research and has potential applications in treating genetic diseases and developing new therapies.
Although not directly involved in oncology, the paediatrician is often confronted with a patient undergoing chemotherapy or radiotherapy. Nowhere in medical science has there been such a paradigm shift as here, moving away from standard diagnostic techniques and chemotherapy to pharmacogenomics and chimeric antigen receptors (CAR T-Cell). The “CAR” is the engineered receptor on the T cells that allows them to bind to a specific protein on cancer cells. CAR T-cell therapy is a type of immunotherapy, meaning it uses the body’s own immune system to fight cancer. It involves genetically modifying a patient’s T cells, a type of white blood cell, to better recognize and attack cancer cells.
Conclusion
If anything, the future for paediatric management looks bright leading to a more efficient and satisfying day to day interaction with patients. The sustainability of future AI-driven general practice support hinges on balancing its transformative potential with responsible implementation. While AI offers numerous benefits like improved efficiency, resource optimization, and personalized care, its environmental impact, ethical considerations, and potential for exacerbating existing inequalities need careful management. A sustainable approach requires integrating AI strategies within broader sustainability initiatives, focusing on eco-design, responsible data management, and continuous monitoring.
Conflict of Interest:
None.
Funding Statement:
None.
Acknowledgements:
None.
References:
- Bertucci, P. (2007). Therapeutic Attractions: Early Applications of Electricity to the Art of Healing. In: Whitaker, H., Smith, C.U.M., Finger, S. (eds) Brain, Mind and Medicine: Essays in Eighteenth-Century Neuroscience. Springer, Boston, MA. https://doi.org/10.1007/978-0-387-70967-3_20
- Demain, A., Sanchez, S. Microbial drug discovery: 80 years of progress. J Antibiot 62, 5–16 (2009). https://doi.org/10.1038/ja.2008.16
- Indrio F, Pettoello-Mantovani M, Giardino I, Masciari E. The Role of Artificial Intelligence in Pediatrics from Treating Illnesses to Managing Children’s Overall Well-Being. J Pediatr. 2024 Dec;275:114291. doi: 10.1016/j.jpeds.2024.114291. Epub 2024 Sep 4. PMID: 39242077.
- Can Demirbaş K, Yıldız M, Saygılı S, Canpolat N, Kasapçopur Ö. Artificial Intelligence in Pediatrics: Learning to Walk Together. Turk Arch Pediatr. 2024 Mar;59(2):121-130. doi: 10.5152/TurkArchPediatr.2024.24002. PMID: 38454219; PMCID: PMC11059951.
- Javaid, Mohd & Haleem, Abid & Singh, Ravi. (2024). Health informatics to enhance the healthcare industry’s culture: An extensive analysis of its features, contributions, applications and limitations. Informatics and Health. 1. DOI: 10.1016/j.infoh.2024.05.001.
- Gutmann, E. Pathologists and Patients: Can We Talk?. Mod Pathol 16, 515–518 (2003). https://doi.org/10.1097/01.MP.0000068260.01286.AC
- Hussain S, Mubeen I, Ullah N, Shah SSUD, Khan BA, Zahoor M, Ullah R, Khan FA, Sultan MA. Modern Diagnostic Imaging Technique Applications and Risk Factors in the Medical Field: A Review. Biomed Res Int. 2022 Jun 6;2022:5164970. doi: 10.1155/2022/5164970. PMID: 35707373; PMCID: PMC9192206.
- Odukoya OK, Chui MA. E-prescribing: a focused review and new approach to addressing safety in pharmacies and primary care. Res Social Adm Pharm. 2013 Nov-Dec;9(6):996-1003. doi: 10.1016/j.sapharm.2012.09.004. Epub 2012 Oct 11. PMID: 23062769; PMCID: PMC3709012.
- Wang SJ, Middleton B, Prosser LA, Bardon CG, Spurr CD, Carchidi PJ, Kittler AF, Goldszer RC, Fairchild DG, Sussman AJ, Kuperman GJ, Bates DW. A cost-benefit analysis of electronic medical records in primary care. Am J Med. 2003 Apr 1;114(5):397-403. doi: 10.1016/s0002-9343(03)00057-3. PMID: 12714130.
- Seah JJ, Zhao J, Wang Y, Lee HP. Review on the Advancements of Stethoscope Types in Chest Auscultation. Diagnostics (Basel). 2023 Apr 25;13(9):1545. doi: 10.3390/diagnostics13091545. PMID: 37174938; PMCID: PMC10177339.
- Galli A, Ambrosini F, Lombardi F. Holter Monitoring and Loop Recorders: From Research to Clinical Practice. Arrhythm Electrophysiol Rev. 2016 Aug;5(2):136-43. doi: 10.15420/AER.2016.17.2. PMID: 27617093; PMCID: PMC5013174.
- Ruchonnet-Métrailler I, Siebert JN, Hartley MA, Lacroix L. Automated Interpretation of Lung Sounds by Deep Learning in Children With Asthma: Scoping Review and Strengths, Weaknesses, Opportunities, and Threats Analysis. J Med Internet Res. 2024 Aug 23;26:e53662. doi: 10.2196/53662. PMID: 39178033; PMCID: PMC11380063.
- Zhang T, Wang Y, Feng X, Zuo Y, Yu H, Bao H, Jiang F, Jiang S. Flexible electronics for cardiovascular monitoring on complex physiological skins. iScience. 2024 Aug 12;27(9):110707. doi: 10.1016/j.isci.2024.110707. PMID: 39262772; PMCID: PMC11387687.
- Garbern SC, Mamun GMS, Shaima SN, Hakim N, Wegerich S, Alla S, Sarmin M, Afroze F, Sekaric J, Genisca A, Kadakia N, Shaw K, Rahman ASMMH, Gainey M, Ahmed T, Chisti MJ, Levine AC. A novel digital health approach to improving global pediatric sepsis care in Bangladesh using wearable technology and machine learning. PLOS Digit Health. 2024 Oct 30;3(10):e0000634. doi: 10.1371/journal.pdig.0000634. PMID: 39475844; PMCID: PMC11524492.
- Bird M, Carter N, Lim A, Kazmie N, Fajardo C, Reaume S, McGillion MH. A Novel Hospital-to-Home System for Children With Medical Complexities: Usability Testing Study. JMIR Form Res. 2022 Aug 12;6(8):e34572. doi: 10.2196/34572. PMID: 35969456; PMCID: PMC9419046.
- Adam J, Rupprecht S, Künstler ECS, Hoyer D. Heart rate variability as a marker and predictor of inflammation, nosocomial infection, and sepsis: a systematic review. Auton Neurosci. 2023;249:103116. doi:10.1016/j.autneu.2023.103116
- Aliyeva A. Transhumanism: Integrating Cochlear Implants With Artificial Intelligence and the Brain-Machine Interface. Cureus. 2023 Dec 12;15(12):e50378. doi: 10.7759/cureus.50378. PMID: 38213340; PMCID: PMC10782474.
- Zhang G, Chen R, Ghorbani H, Li W, Minasyan A, Huang Y, Lin S, Shao M. Artificial intelligence-enabled innovations in cochlear implant technology: Advancing auditory prosthetics for hearing restoration. Bioeng Transl Med. 2025 Jan 9;10(3):e10752. doi: 10.1002/btm2.10752. PMID: 40385537; PMCID: PMC12079510.
- Makawi A, Shah VA, Kim LA, Akkara JD, Firl KC, Tang PH, Montezuma SR. Retinal Prosthesis. American Academy of Ophthalmology. EyeWiki. 2025 Mar 6. Online: https://eyewiki.org/Retina_Prosthesis
- Long Z, Qiu X, Chan CLJ, Sun Z, Yuan Z, Poddar S, Zhang Y, Ding Y, Gu L, Zhou Y, Tang W, Srivastava AK, Yu C, Zou X, Shen G. A neuromorphic bionic eye with filter-free color vision using hemispherical perovskite nanowire array retina. Nat Commun. 2023 Apr 8;14(1):1972. doi: 10.1038/s41467-023-37581-y. PMID: 37031227; PMCID: PMC10082761.
- Suvvari, Tarun Kumar & Madhu, Mansi & Nagendra, Sowmyashree. (2021). Bionic Eye: An Iconic Innovation. TNOA Journal of Ophthalmic Science and Research. 59. 52-55. 10.4103/tjosr.tjosr_168_20.
- Zhang, Hongxin & Lee, Suan. (2024). Advancing the Robotic Vision Revolution: Development and Evaluation of a Bionic Binocular System for Enhanced Robotic Vision. Biomimetics. 9. 371. 10.3390/biomimetics9060371.
- Lau-Zhu A, Lau MPH, McLoughlin G. Mobile EEG in research on neurodevelopmental disorders: Opportunities and challenges. Dev Cogn Neurosci. 2019 Apr;36:100635. doi: 10.1016/j.dcn.2019.100635. Epub 2019 Mar 8. PMID: 30877927; PMCID: PMC6534774.
- Hajare, Raju & Kadam, Sanjana. (2021). Comparative Study Analysis of Practical EEG sensors in Medical Diagnoses. Global Transitions Proceedings. 2. 10.1016/j.gltp.2021.08.009.
- A-Fahoum AS, Al-Fraihat AA. Methods of EEG signal features extraction using linear analysis in frequency and time-frequency domains. ISRN Neurosci. 2014 Feb 13;2014:730218. doi: 10.1155/2014/730218. PMID: 24967316; PMCID: PMC4045570.
- Mihai AS, Geman O, Toderean R, Miron L, SharghiLavan S. the Next Frontier in Brain Monitoring: A Comprehensive Look at In-Ear EEG Electrodes and Their Applications. Sensors 2025, 25(11), 3321; https://doi.org/10.3390/s25113321
- Joyner M, Hsu SH, Martin S, Dwyer J, Chen DF, Sameni R, Waters SH, Borodin K, Clifford GD, Levey AI, Hixson J, Winkel D, Berent J. Using a standalone ear-EEG device for focal-onset seizure detection. Bioelectron Med. 2024 Feb 7;10(1):4. doi: 10.1186/s42234-023-00135-0. PMID: 38321561; PMCID: PMC10848360.
- Setati, T., Perold, W., Fourie, P.R. Withey, D. (2022). Comparing Closed-loop Control of Drug Infusion using MPC and PID. In Proceedings of the 15th International Joint Conference on Biomedical Engineering Systems and Technologies (BIOSTEC 2022) – Volume 1: BIODEVICES; ISBN 978-989-758-552-4, SciTePress, pages 126-133. DOI: 10.5220/0010783700003123.
- Moumane H, Pazuelo J, Nassar M, Juez JY, Valderrama M, Le Van Quyen M. Signal quality evaluation of an in-ear EEG device in comparison to a conventional cap system. Front Neurosci. 2024 Sep 10;18:1441897. doi: 10.3389/fnins.2024.1441897. PMID: 39319310; PMCID: PMC11420159.
- Kaveh R, Schwendeman C, Pu L, Arias AC, Muller R. Wireless ear EEG to monitor drowsiness. Nat Commun. 2024 Aug 2;15(1):6520. doi: 10.1038/s41467-024-48682-7.
- Maniram J, Oosthuizen F, Karrim SBS. An Overview of Pharmacotherapy in the Management of Children with Autism Spectrum Disorder at a Public Hospital in KwaZulu-Natal. Child Psychiatry Hum Dev. 2024 Dec;55(6):1655-1663. doi: 10.1007/s10578-023-01514-z. Epub 2023 Mar 22. PMID: 36944778; PMCID: PMC11485179.
- Popow C, Ohmann S, Plener P. Practitioner’s review: medication for children and adolescents with autism spectrum disorder (ASD) and comorbid conditions. Neuropsychiatr. 2021 Sep;35(3):113-134. doi: 10.1007/s40211-021-00395-9. Epub 2021 Jun 23. PMID: 34160787; PMCID: PMC8429404.
- Manter MA, Birtwell KB, Bath J, Friedman NDB, Keary CJ, Neumeyer AM, Palumbo ML, Thom RP, Stonestreet E, Brooks H, Dakin K, Hooker JM, McDougle CJ. Pharmacological treatment in autism: a proposal for guidelines on common co-occurring psychiatric symptoms. BMC Med. 2025 Jan 7;23(1):11. doi: 10.1186/s12916-024-03814-0. PMID: 39773705; PMCID: PMC11705908.
- Alonso, Herculano & Heimer, Mônica & Calado, Rafael & Silva, João & Lamenha-Lins, Renata & Romão, Dayse & Pugliesi, Daniela & Junior, Valdeci. (2024). Sedation and its Potential Risks in Children with Autism Spectrum Due to Drug Overlaps: A Critical Review. Pesquisa Brasileira em Odontopediatria e Clínica Integrada. 24. 10.1590/pboci.2024.053.
- Goodson R, Wagner J, Sandritter T, Staggs VS, Soden S, Nadler C. Pharmacogenetic Testing in Patients with Autism Spectrum Disorder Evaluated in a Precision Medicine Clinic. J Dev Behav Pediatr. 2023 Oct-Nov 01;44(8):e505-e510. doi: 10.1097/DBP.0000000000001215. Epub 2023 Oct 6. PMID: 37807195; PMCID: PMC10564071.

