Coping Mechanisms and Health Disparities in Racial Groups
Coping Mechanisms and Health Outcomes: A Comparative Analysis of African American and Caucasian Communities
Dr. Clifton Addison 1,2; Dr. Brenda Jenkins 1; Dr. Monique White 1; Dr. Marinelle Payton 1,2
- Jackson State University (JSU) Jackson Heart Study (JHS) Graduate Training and Education Center (GTEC), College of Health Sciences
- Department of Epidemiology and Biostatistics, Jackson, Mississippi, U.S.A.
OPEN ACCESS
PUBLISHED:31 October 2025
CITATION:Addison, C., Jenkins, B., et al., 2025. Coping Mechanisms and Health Outcomes: A Comparative Analysis of African American and Caucasian Communities. Medical Research Archives, [online] 13(10).
https://doi.org/10.18103/mra.v13i10.7063
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i10.7063
ISSN 2375-1924
Abstract
Coping mechanisms—the behavioral and cognitive strategies used to manage stress—play a critical role in determining both mental and physical health outcomes. This study examines the relationship between coping styles and health disparities in African American and Caucasian communities in the United States. Drawing on literature from psychology, sociology, and public health, it highlights how cultural norms, structural inequities, and historical experiences shape stress responses and coping choices. Specifically, African American populations often rely on emotion-focused and spiritual coping rooted in collective resilience, whereas Caucasian populations tend to adopt more problem-focused and individual coping strategies. These differences influence outcomes such as hypertension, depression, and cardiovascular disease. Using a narrative review design, the study synthesizes evidence from the Jackson Heart Study and related epidemiologic data to demonstrate how coping mediates the impact of stress on health. The findings underscore the need for culturally tailored interventions that integrate spiritual, social, and psychological resources to promote adaptive coping and reduce health inequities.
Keywords: coping mechanisms, health disparities, African Americans, Caucasians, stress, health outcomes, resilience
Introduction
Racial and ethnic disparities in health outcomes remain persistent in the United States. African Americans experience disproportionately higher rates of hypertension, cardiovascular disease, and stress-related disorders compared to Caucasians. While structural inequities and access to care are major determinants, coping strategies represent a critical yet underexplored factor in understanding these disparities. Coping, as first conceptualized by Lazarus and Folkman, refers to the constantly changing cognitive and behavioral efforts to manage specific external and/or internal demands that are appraised as taxing or exceeding one’s resources. These strategies mediate how individuals respond to chronic stressors—such as illness, poverty, or discrimination—and consequently affect health trajectories.
Coping strategies offer one avenue through which one can understand how individuals respond to life stressors, including chronic illness, financial strain, and racism. Cultural background, historical context, and social support systems significantly shape these coping responses and their efficacy in maintaining health. The concept of coping was developed by Lazarus and colleagues and comprises the many practices that individuals utilize, when faced with a menacing situation, to mitigate the negative impact and reduce the possibility of impending psychological and physical harm. Coping implies two things: first, the existence of a real or imagined problem. In order to understand how individuals address the problems they face, researchers administer coping skills inventories to understand human responses to environmental frustrations and aggravations. The coping instruments used to gather information can serve as the inner voice that can inform researchers and individuals about their practices, thoughts, attitudes, and behaviors.
Understanding people’s responses will help public health and healthcare professionals, as well as the individuals themselves, to recognize the environmental cues and triggers that ultimately affect health and contribute to poor outcomes. Understanding these indicators can lead to implementation of prevention and intervention strategies that effectively address the prevalence of chronic diseases.
The aim of this paper is to compare coping mechanisms between African American and Caucasian populations and to examine their associations with mental and physical health outcomes. The scope includes a discussion of sociocultural influences, historical stressors, and resource accessibility that shape coping patterns across these two groups.
Study Design and Methodology
This paper employs a narrative literature review design, synthesizing peer-reviewed studies, national health surveys, and community-based research that focus on coping mechanisms and health disparities among African American and Caucasian populations. Data were drawn from large epidemiological studies such as the Jackson Heart Study (JHS), the National Survey of American Life, and the Stress in America Survey.
The JHS was established in 2000 as a collaborative partnership among Jackson State University, Tougaloo College, the University of Mississippi Medical Center, and the National Institutes of Health (NIH) through its National Heart, Lung, and Blood Institute (NHLBI) and the Office of Research on Minority Health. The primary objective of the JHS is to identify risk factors contributing to the development of cardiovascular disease (CVD) among African American men and women. Beyond traditional biomedical determinants, the study also examines how psychosocial factors and stressors influence cardiovascular health outcomes, recognizing that social and emotional contexts play a critical role in disease development and progression.
Complementing the JHS’s focus on psychosocial determinants of health, the American Psychological Association launched the Stress in America survey in 2007 as part of its Mind/Body Health campaign. Conducted annually, this nationwide survey provides valuable insight into the prevalence, sources, and perceived impacts of stress across the U.S. population. The Stress in America findings highlight how chronic stress—particularly related to financial strain, work, and discrimination—can have profound effects on both physical and mental well-being. These data offer a national perspective on the stress-related factors that may contribute to the disparities in CVD risk observed in studies such as the JHS.
In parallel, the National Survey of American Life (NSAL) expands understanding of the intersection between race, culture, and mental health. The NSAL was designed to examine the prevalence, severity, and impairment associated with mental disorders among nationally representative samples of Black and non-Hispanic White populations in the United States. Importantly, the study emphasizes diversity within the Black population by including African Americans, Afro-Caribbean immigrants, and U.S.-born individuals of Afro-Caribbean descent. Findings from the NSAL underscore the complex role of cultural identity, socioeconomic position, and social stressors in shaping psychological well-being and health outcomes.
Together, the JHS, Stress in America, and NSAL studies provide a multidimensional understanding of how psychosocial, cultural, and environmental factors intersect to influence cardiovascular and mental health. Integrating insights from these landmark studies allows for a more comprehensive examination of health disparities, emphasizing the need for continued research on the pathways through which chronic stress and social determinants affect both physical and mental health outcomes.
Building on this foundation, the current study explores the relationship between psychosocial stress, coping mechanisms, and cardiovascular risk among adults. The review focused on three main domains: (1) coping typologies (problem-focused, emotion-focused, avoidance-based); (2) sociocultural determinants influencing coping style selection; and (3) health outcomes associated with coping, including hypertension, depression, and cardiovascular risk.
Results and Discussion
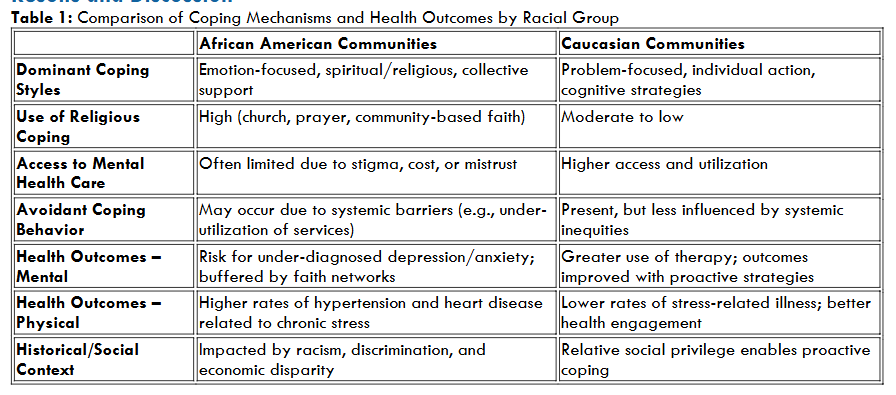
African American Communities
- Dominant Coping Styles: Emotion-focused, spiritual/religious, collective support
- Use of Religious Coping: High (church, prayer, community-based faith)
- Access to Mental Health Care: Often limited due to stigma, cost, or mistrust
- Avoidant Coping Behavior: May occur due to systemic barriers (e.g., under-utilization of services)
- Health Outcomes – Mental: Risk for under-diagnosed depression/anxiety; buffered by faith networks
- Health Outcomes – Physical: Higher rates of hypertension and heart disease related to chronic stress
- Historical/Social Context: Impacted by racism, discrimination, and economic disparity
Caucasian Communities
- Dominant Coping Styles: Problem-focused, individual action, cognitive strategies
- Use of Religious Coping: Moderate to low
- Access to Mental Health Care: Higher access and utilization
- Avoidant Coping Behavior: Present, but less influenced by systemic inequities
- Health Outcomes – Mental: Greater use of therapy; outcomes improved with proactive strategies
- Health Outcomes – Physical: Lower rates of stress-related illness; better health engagement
- Historical/Social Context: Relative social privilege enables proactive coping
Coping Typologies and Cultural Context
Coping strategies can be grouped into problem-focused, emotion-focused, and avoidance-based categories. Research indicates that Caucasian individuals, who often face fewer systemic barriers, are more likely to adopt problem-focused coping such as active problem-solving or planning. African Americans, conversely, rely heavily on emotion-focused and collective coping, including prayer, religious involvement, and family support. These patterns reflect cultural strengths rooted in spirituality and community solidarity that buffer against psychological stressors but may not fully mitigate physiological consequences of chronic stress.
Coping and Physical Health
African Americans exhibit higher rates of hypertension and cardiovascular disease, partly due to chronic exposure to racism and socioeconomic adversity. Emotion-focused coping, while effective for psychological relief, may not reduce biological stress markers such as cortisol and blood pressure. Conversely, problem-focused coping—more common among Caucasians—has been associated with improved cardiovascular health and treatment adherence.
Coping and Mental Health
Emotion regulation is central to mental well-being. Adaptive coping reduces the risk of depression and anxiety, whereas maladaptive coping—such as avoidance or substance use—increases psychological distress. African Americans may underutilize mental health services due to stigma or mistrust, relying instead on faith-based or familial support systems. Caucasians are more likely to access formal therapy or medication, which may explain differences in reported mental health outcomes.
Social and Structural Influences
Historical trauma and systemic racism have shaped coping cultures in African American communities, fostering resilience but also limiting access to structural supports. Collective coping serves as a cultural strength, yet health systems often overlook these practices. For Caucasians, relative privilege facilitates access to healthcare and psychological resources, enabling more proactive coping and engagement in preventive care.
Implications for Public Health Practice
Culturally informed interventions are necessary to bridge coping disparities. For African American populations, integrating spiritual leaders, peer support networks, and culturally relevant stress management programs can enhance coping efficacy. For Caucasians, strengthening self-regulation and behavioral coping through cognitive-behavioral therapy and mindfulness may yield additional benefits. Policymakers must also address structural inequities—such as healthcare access and discrimination—that shape stress exposure and coping capacity.
Conclusion
Coping mechanisms are pivotal in mediating the relationship between stress and health. African American and Caucasian populations demonstrate distinct coping profiles influenced by culture, history, and access to resources. Recognizing these differences is essential for designing equitable, culturally competent interventions. By integrating spiritual, social, and psychological components into health promotion, practitioners can foster resilience and reduce chronic disease disparities across racial groups.
Funding
The Jackson State University Jackson Heart Study Graduate Training and Education Center (JSU JHS GTEC), Jackson, Mississippi, USA, received external funding from the National Heart, Lung, and Blood Institute (NHLBI) and the National Institute of Minority Health and Health Disparity (NIMHD) of the National Institutes of Health (NIH) – Jackson State University Grant Number HHSN2682018000131.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Williams DR, Mohammed SA. Racism and health I: Pathways and scientific evidence. Am Behav Sci. 2013;57(8):1152-1173.
- Lazarus RS, Folkman S. Stress, Appraisal, and Coping. Springer; 1984.
- Taylor SE, Stanton AL. Coping resources, coping processes, and mental health. Annu Rev Clin Psychol. 2007;3:377-401.
- Brondolo E, Brady N, Ver Halen N, Pencille M, Beatty D, Contrada RJ. Coping with racism: a selective review of the literature and a theoretical and methodological critique. J Behav Med. 2009;32(1):64-88.
- Lewis TT, Cogburn CD, Williams DR. Self-reported experiences of discrimination and health. Annu Rev Clin Psychol. 2015;11:407-440.
- Addison CC, Campbell-Jenkins BW, Sarpong DF, et al. Psychometric evaluation of a Coping Strategies Inventory Short-Form (CSI-SF) in the Jackson Heart Study cohort. Int J Environ Res Public Health. 2007;4(4):289-295.
- Lazarus RS, Lanier R. Stress-related transactions between person and environment. In: Pervin LA, Lewis M, eds. Perspectives in Interactional Psychology. Plenum Press; 1978:287-327.
- Addison C, Jenkins B, White M. User manual for Coping Strategies Inventory Short Form (CSI-SF) – The Jackson Heart Study. Int J Environ Res Public Health. 2024;21(4):443.
- Sempos CT, Bild DE, Manolio TA. Overview of the Jackson Heart Study: A study of cardiovascular diseases in African American men and women. Am J Med Sci. 1999;317(3):142-146.
- Tajeu GS, Colvin CL, Hardy ST, et al. Prevalence, risk factors, and cardiovascular disease outcomes associated with persistent blood pressure control: The Jackson Heart Study. PLoS One. 2022;17(8):e0270675.
- Bhavsar NA, Davenport CA, Yang LZ, et al. Psychosocial determinants of cardiovascular events among Black Americans with chronic kidney disease. BMC Nephrol. 2021;22:375.
- American Psychological Association. Stress in America, United States, 2007-2023. Inter-university Consortium for Political and Social Research; 2025.
- Jackson JS, Torres M, Caldwell CH, et al. The National Survey of American Life: A study of racial, ethnic, and cultural influences on mental disorders and mental health. Int J Methods Psychiatr Res. 2004;13(4):196-207.
- Folkman S, Moskowitz JT. Coping: pitfalls and promise. Annu Rev Psychol. 2004;55:745-774.
- Chatters LM, Taylor RJ, Lincoln KD. Religious involvement and coping among African Americans. J Black Psychol. 2011;37(4):403-423.
- Levi M, Murphy B, O’Brien M. Problem-focused coping and treatment adherence. J Behav Med. 2016;39(4):563-572.
- Aldwin CM. Stress, Coping, and Development: An Integrative Perspective. Guilford Press; 2007.
- Ward EC, Wiltshire JC, Detry MA, Brown RL. African American men and women’s attitudes toward mental illness, perceptions of stigma, and preferred coping behaviors. Nurs Res. 2013;62(3):185-194.
- Utsey SO, Bolden MA, Lanier Y, Williams O. Spirituality and quality-of-life indicators among African Americans. J Black Psychol. 2015;41(4):370-391.

