Critical Insights on Cerebral Palsy Treatment Approaches
Cerebral Palsy: a critical approach to theories and treatment plans
Reinald Brunner1, Stephanie Jünemann 2
OPEN ACCESS
PUBLISHED: 28 Febuary 2025
CITATION: BRUNNER, Reinald; JÜNEMANN, Stephanie. Cerebral Palsy: a critical approach to theories and treatment plans. Medical Research Archives,. Available at: <https://esmed.org/MRA/mra/article/view/6112>.
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i2.6112
ISSN 2375-1924
Abstract
The treatment strategies are based on hypotheses about the aetiology of the pathology. These hypotheses remain unchanged, even if our treatment does not always bring the desired success. The cause of these less satisfactory results is often not investigated. New findings from modern literature can also go unnoticed for a long time. We should question our traditional concepts more often and be open to new and novel possibilities. As examples, we describe the treatment of hamstrings in squatting gait, femoral osteotomy in internal hip rotation during walking and the importance of spasticity. The problem of outdated working hypotheses also calls into question clinical evidence-based papers on outcome.
Keywords
- Cerebral Palsy
- Spasticity
- Treatment Strategies
- Hamstrings
- Osteotomy
Introduction
In medical school and later during residency we learn how to approach a patient, take a history, make a diagnosis and treat. Treatment is based on theories, pathophysiological aspects, practical experience and Level 1-4 recommendations. Outpatient clinic is busy, time for the patient limited, and the pile of bureaucracy is rising. Standard thinking, standard theories, and known procedures are often convenient. Too often too little time or effort to ask, rethink treatments and question clinical everyday life.
Cerebral palsy is a good example of existing theories on aetiology, symptomatic treatment and therapies. The most common form is the spastic form with in the last decades established treatments (such as selective dorsal rhizotomy, intrathecal Baclofen, intramuscular Botulinum Toxin) of the symptom spasticity expecting functional improvement of the motor abilities. But in recent years there are increasingly discussions not just on the concept of spasticity (measurement, necessity for function, weakness below) but a step further on the concept of Cerebral Palsy, its aetiology in terms of CP-mimics (genetic or metabolic causes), characterisation and missing knowledge on for example impairments in the spinal cord. Modern literature questions our hypotheses on aetiology and pathomechanics, which still serve as the basis for our treatment concepts. We explain this problem using a few examples and encourage you to reconsider and correct the hypotheses that form the basis for our treatment concepts. Patients come to see us because they have a problem. We on our side understand that they seek for a solution which should be quick, efficient, and sustainable. We analyse the present situation in order to set up a and base our decision on the momentaneous clinical findings which may include imaging or other diagnostic tools. We combine our findings with what we have learned, our experience and the publications of successful outcomes from the literature, and we determine a treatment plan. We feel secured as we rely on the evidence base criteria to qualitatively judge the respective reference papers, searched for help in textbooks written by experts in the field, and see the good outcome in our patients. Nevertheless, we are hardly aware that we lack a firm knowledge on aetiology and pathomechanics, and most of our concepts base on hypotheses which never have been proven but have been passed on for years. These hypotheses are so well accepted and constantly repeated that we have difficulties to allow for critical views and other new hypotheses. Although a critical approach does not necessarily change our current treatment, it does allow a more precise understanding and offers the inclusion of different and new treatment measures.
Anatomy, Measurements and Function: Is there a correlation?
In case of a fracture, we base our decision of treatment on x-rays. Asking about the circumstances during the incidence provides information about possible additional problems and risks for our treatment which then may be adapted. Osteoarthritis of the hip is best and most easily treated by joint replacement. Repairing the defect corrects the problem. Little thought is given to why the osteoarthritis has developed, as it has no bearing on the decision at the time.
Our concept of treatment is that repairing the defect which causes pain and reduces the use of the limb, results automatically in a restitution of function. This concept is certainly valid for localised problems, and we also apply this assumption to complex diseases such as cerebral palsy. In principle, we assume normal anatomy of the musculoskeletal system as a guarantee of normal function. We carry out a clinical examination with the patient lying on a table or standing statically in front of us and list the abnormalities by comparing the patient’s values with the normative standards. We recommend lengthening of short muscle-tendon systems, osteotomies to correct abnormally shaped bones and ligament reconstruction or joint fusion for instability. We treat leg length discrepancies of a few centimetres to prevent scoliosis or cure back pain. We assume that spasticity hinders function and treat it in order to reach a situation close to healthy people.
Is normality really the basis for optimal function? We all know that Usain Bold won the marathon with flat feet and Cristiano Ronaldo became a fantastic and famous soccer player despite his flat feet. On the other hand, club feet were treated with an extensive decomposition of the hind and midfoot known as Cincinnati approach. Indeed, x-rays proved a good and anatomical position of the foot bones after surgery, but the feet not uncommonly got stiff and painful in later life. The manipulation approach by Ponseti in contrast results in superior function despite the risk for a poorer correction of the skeletal malposition. Normal function hence can be reached in spite of skeletal abnormalities, although usually to a mild degree. Further, normalcy has a wide range. We usually consider only the mean as this is easy to remember, and if we are good, we add the standard deviation. If we look at the Gauss curve, however, we must realise that all this still concerns only part of the whole range. On the other hand, there are people, who still have difficulties to perform normally although they do not present any musculoskeletal deformity. Neuromuscular control is at least as important as anatomical shape, and motor learning enables to develop compensations for skeletal deformities in order to reach at least close to normal function. This is where another bias of the treating person comes into play: We imagine how a particular movement problem affects function, and we use that imagination to recommend treatment. We imagine the importance of a leg length discrepancy but ignore, that we seldom stand on both legs fully extended or walk on even pavement. We may use improvement of back pain after leg length equalisation as an argument for the correctness of treatment but it is more probable that the different position of the pelvis changes the load on the spine muscles and relaxes the tense muscles. We are not all absolutely the same, but we have nevertheless learnt to function in the same way. Mistakes and failures are necessary to learn that an attempted movement strategy does not lead to the desired result, which helps to compensate for anatomical differences. So we need to allow mistakes for motor learning, but help with persistent failure. We therefore do not have to correct every current error immediately and must be open to other, but successful movement strategies.
We must further consider that anatomical especially during growth, the reorientation of the growth plate helps to correct posttraumatic deformities if they lay in the movement direction of a joint. Hence, before we consider a deformity as primary, we should reason whether there could be a functional cause.
Primary and secondary deformities
In patients with cerebral palsy, we distinguish between primary deformities arriving as a consequence of the deranged motor control and secondary deformities which develop due to compensations over time. Secondary deformities may disappear spontaneously if the causing primary deformity is corrected. Although this analytic concept sounds logical, it is often difficult to make this distinction in a given situation. For example: does hamstring shortness develop on the base of spasticity (abnormally high muscle tone or hyperreflexia), or may there be other reasons, e.g. overuse? In a clinic situation, we see a patient who walks with flexed knees which means knee flexion in stance phase. We find short hamstrings on the couch and spasticity. Our interpretation may be that the spasticity of the hamstrings impedes an adequate knee extension during gait; and due to spasticity these muscles become short. The use of gait analysis, where muscle length for the individual can be computed for any moment in time during the gait cycle, is seldom used. It still says nothing about muscle tension and force, but it would at least avoid erroneous lengthenings. Although it was shown that in the majority of patients the hamstrings are not short during gait, the concept of spasticity as the main cause for knee flexion in stance phase of gait persists. Hamstring weakening by injecting botulinum toxin or hamstring lengthening are still widely used to correct knee flexion. We also experience an increase of pelvic anterior tilt and hip flexion after these procedures. It surprises that we do not question the concept of hamstring pathology in front of such undesirable side effects. The main problem with the current hypothesis is that spasticity during walking has never been detected or can be measured. We infer the presence of spasticity during walking from the situation on the couch, guided by the impression of stiffness or muscle shortening. We neglect the lack of evidence. Could there possibly be other hypotheses that explain the hamstring pathology?
New hypotheses should be based on the facts we know about the gait pattern: A near vertical tibial position is essential for knee extension. Under load, the hamstrings work primarily as hip extensors. If the knee has lost extension during the stance phase of gait due to the forward tilt of the tibia, the knee extensors, especially the vasti, are overloaded. This knee extensor overloaded can be reduced by an anterior trunk tilt which shifts the centre of mass forward at the expense of the hip extensors, which are required for sagittal pelvic and trunk control. In addition to the gluteus maximus, the hamstrings also come into play in this situation. As knee flexion increases, the lever arm for the hamstrings to flex the knee increases, which in turn requires a counteraction from the vasti and increases the load on the knee extensors. The constant and increased load on the hamstrings can be seen as a good reason for the muscle shortening found during the examination on the couch. This history explains the patient’s situation as well as the findings in the clinical examination, but does not require spasticity as a causal argument. The hypothesis is based on anterior tibial tilt and its consequences. Possible causes are weak plantar flexors or a short lever arm due to a foot deformity during stance, both of which are known to occur in patients with cerebral palsy. Another reason is insufficient knee extension during terminal swing. Possible causes include insufficient acceleration during pre-swing, insufficient time to complete the swing phase due to instability of the opposite leg, or hamstring spasticity. In fact, all of these causes can be present in individual patients, even in combination. The hypothesis with increased load of the hamstrings leads to the conclusion that the hamstrings should be treated more carefully and that the knee extensor weakness is becoming more important, which is already reflected in the procedures for shortening the patellar ligament.
The original publication on the development of crouch gait reasons even on the cause of foot deformities which lead to poor control on the tibia position. A concept for the development of gait disorders is presented, where sensory problems and the mental reaction to it are seen as the primary cause, and the development of the gait patterns is explained by a chain of compensations which use muscles and joint positions in an abnormal way on a purely mechanical basis. In brief, foot equinus results from a perception of insecurity when posture is controlled. While initially the equinus helps to keep the knee extended, the development of a foot deformity withdraws this positive effect and the knee becomes flexed with the consequence of knee extensor overload, trunk forward lean and hamstring overuse and shortness as described above. Surprisingly, spasticity is not an important factor, and the concept fits with patients with other diseases such as spina bifida as well. Although this explanation may not represent the truth, it offers a new different view and novel approaches. Further, and this is important, it also shows the possibility of preventive means which may be of impact in the future. If the foot deformity is prevented and the foot is kept in line with the leg and the direction of gait, the competence to control tibial advancement is maintained and the mechanical failure resulting in crouch is stopped. Providing stability is an essential factor for improvement and prevention of deterioration, and keeping control of knee extension is one part. These facts are not new, and many of us would describe them as therapeutic goals. However, this must not be concealed, that insufficient knee extension at terminal swing remains an unsolved problem. The concept of the development of gait deformities only provides a possible background for treatment decisions. It explains how deformities require compensations and how this creates new deformities. Understanding this chain of causal connections enables the treater to correct not only a given deformity but also to define and correct the causing factors in order to prevent recurrency. As it puts the mechanical factors into a larger context, it helps to understand at least partially, that motor experience and competence are other important factors and that deficits in these areas make it impossible to reach normality.
Internal rotation gait
Another example is internal rotation gait. We check the various components which add up internal rotation during gait and correct the torsion of the foot, the tibia, and the femur. We see the cause for an increased femoral anteversion in a lack of spontaneous normal reduction of anteversion and correct it to the midpoint of hip rotation (that external rotation equals internal rotation). The outcome reports are satisfying but not really reliable and long lasting in an individual. Especially if corrected early, anteversion relapses. We thus should consider the femoral anteversion a result of bony adaptation at the forces resulting from daily use, and should evaluate the factors which lead to internal rotation at the hip. We know that toe walking can be one component, midfoot break another, and we see rocking on an internally rotated foot as a further component. If the foot is more than about 30 degrees internally rotated, rocking on this foot twists the foot and indirectly the leg internally until push off. In asymmetric internal rotation as in unilateral cerebral palsy, hip internal rotation is often combined with pelvic retraction on the same side. A common still hypothetical explanation is that the better leg takes the functional lead which would require excellent motor control as the difference must be perceived. Modelling rocking on an equinus foot, however, provides a simple mechanical passive reaction as an explanation. In a patient with sensational and motor control deficits, this second explanation is at least as attractive. The consequence of accepting that anteversion is secondary, is that the causing factors need to be addressed as well when femoral torsion is corrected. An indication for the soundness of this concept is that correcting toe walking into a heel toe gait prevents the development of hip internal rotation deformity.
A second problem arises by focussing on femoral anteversion as the origin: The movement of the hip is normally not limited by bony structures but by ligaments, capsule, and muscles. These tissues adapt faster than bone. If recurrent internal rotation deformity is treated by repetitive derotation osteotomies, there is a risk for uncovering the femoral head on the posterior part.
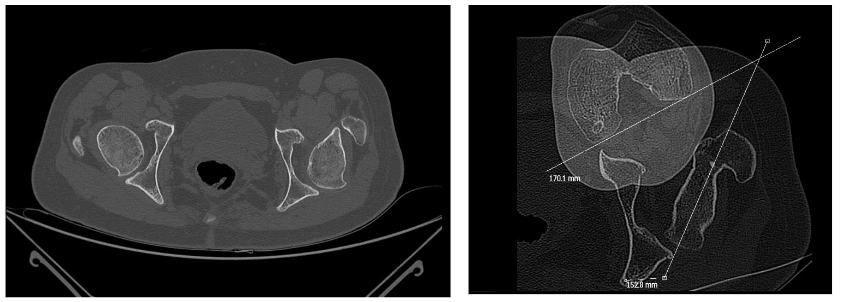
On the other hand, the forces that act on the proximal femur and shape the anteversion occur not only during walking, but during all activities during the day, including sitting. We do not yet have clear data about these forces. Nevertheless, we should broaden the field of vision of our concept and also include indirect, causal and new factors in our treatment.
Spasticity, motor control
We can feel neither gravity nor inertia. This tempts us to think of movement as muscle-driven. The muscles certainly play an important role, but they have to cope with external forces. Unusual segmental positions in space require muscle activity that deviates from the norm, but this can be well controlled in view of the situation. Part of our functional efficacy is due to the way how we control the external forces for keeping posture and moving forward. While we profit from external forces when we keep our body segments in favourable positions, we lose this effect in other usually more bent positions. Nevertheless, unimpaired individuals seem to use a more complex motor control in a more favourable body position when walking than impaired individuals with their gait abnormalities. As only patients with brain damage (cerebral palsy, stroke) were analysed it does not surprise that less complex motor control in impaired patients coincides with spasticity. However, a causal link was not described. In a recent paper, spasticity was not found to be a factor affecting gross motor function. In contrast to such reports, spasticity treatment for functional improvement is still part of daily practice. We imagine that spasticity hinders function. It may be surprising that a large study on patients with cerebral palsy found no difference in function with or without spasticity treatment, and only speed to a mild degree and spasticity itself were affected. Such information should stimulate critical thinking. In a case diagnosed of spasticity, we have a tendency to ascribe all abnormal muscle activity and even movement to spasticity. We neglect the fact, that there is no report of spasticity during gait, and no method for diagnosing spasticity during function is described. We still see spasticity as the cause for foot equinus even during swing phase of gait as the foot is plantarflexed in the second part of swing phase in most of the patients with spastic cerebral palsy. However, spasticity requires a fast stretch against resistance. There is no resistance for the foot in swing. Once the foot hits the floor with the toes, it would be possible to activate pathological reflexes. Again, there are no clear signs in dynamic EMG nor in kinetics. We have a tendency to believe more our eyes and imagination than proper data, and excuse this contradiction by the lack of proper measuring facilities; and continue to treat spasticity to improve function. The presence of spasticity during function is an unproven hypothesis, and the report on poor effect of spasticity treatment for functional improvement puts the hypothesis in question. Many other hypotheses are possible in the case of foot equinus: it can compensate for an even only functional leg length discrepancy, it can prevent the tibia from falling forward with the danger of losing control on knee extension in case of equilibrium incompetence in stance phase, it can be a remnant from poor motor learning with the persistence of immature motor patterns, and maybe there are even more possibilities. Instead of considering plantarflexion as caused by spasticity, it could be seen as an erroneous means to manage body control during gait. The only option to correct the drop foot position in swing is an AFO. Spasticity treatment with the effect of weakening the plantar flexors in contrast is of little help.
The problem with evidence
These considerations show that we rarely scrutinise the basic concept of our treatment decision. We focus on the presentation of the problems of the patient at the moment of the visit on the basis of what we learned, experienced, and accepted. Our thinking tends to find causal connections, which also influences the hypotheses we have created and still use. This has also a consequence for scientific research: we assume that our basic background for our decision is generally accepted and valuable. We do not describe the details in our papers. We take any improvement as proof for the correctness of our action. We are seldom aware of the complex interaction of the various interventions and the reasons, and the result is still unclear. We should far more concentrate on the concept underlying our treatment activities, and we should more often compare the outcome of mildly different treatment concepts, such as in the paper of Niklasch et al. where different details of decision making for femoral derotation were studied. A prospective study setup would have been superior, however. It questions the basic background. Such questions finally bring us to the point where we need to reflect what we understand under more a complex of symptoms than an actual disease itself, and that it may occur in the context of various affections. However, the focus remains on motor symptoms with uncontrolled and spastic muscle activity as a major factor for the clinical picture. MacWilliams et al. showed in a paper on large cohorts that the effect of spasticity treatment is marginal. Botulinum toxin is increasingly questioned. Such reports should stimulate more a critical examination of our basic treatment concepts. Brandenburg et al. focus on the contradiction that the diagnosis of cerebral palsy bases on the clinical picture independent of the verification of any brain pathology. They further discuss the spasticity symptoms as a spinal cord problem which lost sight of. Rosenbaum questions the concept of the current understanding of cerebral palsy in a wider range of multiple contributing factors in a recent editorial. The report on regular and severity depending lesions also of the sensory tracts offers a further concept which can explain the motor symptoms as well as the developmental retardation. We need to understand that we lack clear explanations of at least some parts of what we understand as cerebral palsy. We need to step away from the narrow focus on motor function, motor pathways in the brain, and cerebral motor control and open the view to a more complex picture on interacting factors and a deeper understanding of the pathomechanisms. We need to draw conclusions from the modern literature and adapt our bases for the treatment regimen.
Conclusion
We can identify a gap between information in the modern literature and the hypotheses where our treatment bases on. We need to incorporate this new information and adapt our hypotheses on aetiology and pathomechanics, and possibly even develop new concepts. This approach includes also considering contributing factors such as motor learning, integrity of senses, IQ, and even the environment.
Conflict of Interest:
None.
Funding Statement:
There were no funding for this project.
Acknowledgements:
None.
References:
- Zwick, E.B., et al., Comparison of Ponseti versus surgical treatment for idiopathic clubfoot: a short-term preliminary report. Clin Orthop Relat Res, 2009. 467(10): p. 2668-76.
- Wolff, J., Die Lehre von der functionellen Knochengestalt. Archiv für pathologische Anatomie und Physiologie und für klinische Medicin, 1899. 155(2): p. 256-315.
- Arnold, A.S., et al., The role of estimating muscle-tendon lengths and velocities of the hamstrings in the evaluation and treatment of crouch gait. Gait Posture, 2006. 23(3): p. 273-81.
- Frigo, C., E.E. Pavan, and R. Brunner, A dynamic model of quadriceps and hamstrings function. Gait Posture, 2010. 31(1): p. 100-3.
- Brunner, R., The Evolution of Knee Flexion during Gait in Patients with Cerebral Palsy, in Cerebral Palsy, F. Miller, et al., Editors. 2018, Springer International Publishing: Cham. p. 1-14.
- Kay, R.M., et al., Comparison of proximal and distal rotational femoral osteotomy in children with cerebral palsy. J Pediatr Orthop, 2003. 23(2): p. 150-4.
- Boyer, E.R., et al., Long-term functional outcomes after an external femoral derotation osteotomy in individuals with cerebral palsy. Gait Posture, 2021. 87: p. 184-191.
- Dreher, T., et al., Long-term outcome of femoral derotation osteotomy in children with spastic diplegia. Gait Posture, 2012. 36(3): p. 467-70.
- Ounpuu, S., et al., Long-term effects of femoral derotation osteotomies: an evaluation using three-dimensional gait analysis. J Pediatr Orthop, 2002. 22(2): p. 139-45.
- Brunner, R. and J.U. Baumann, Long-term effects of intertrochanteric varus-derotation osteotomy on femur and acetabulum in spastic cerebral palsy: an 11- to 18-year follow-up study. J Pediatr Orthop, 1997. 17(5): p. 585-91.
- Brunner, R., et al., Effects of plantarflexion on pelvis and lower limb kinematics. Gait Posture, 2008. 28(1): p. 150-6.
- Gaston, M.S., et al., Transverse plane rotation of the foot and transverse hip and pelvic kinematics in diplegic cerebral palsy. Gait Posture, 2011. 34(2): p. 218-21.
- Brunner, R., W.R. Taylor, and R.M.S. Visscher, Restoration of Heel-Toe Gait Patterns for the Prevention of Asymmetrical Hip Internal Rotation in Patients with Unilateral Spastic Cerebral Palsy. Children (Basel), 2021. 8(9).
- Steele, K.M., A. Rozumalski, and M.H. Schwartz, Muscle synergies and complexity of neuromuscular control during gait in cerebral palsy. Dev Med Child Neurol, 2015.
- MacWilliams, B.A., et al., Causal factors affecting gross motor function in children diagnosed with cerebral palsy. PLoS One, 2022. 17(7): p. e0270121.
- MacWilliams, B.A., et al., Long-term effects of spasticity treatment, including selective dorsal rhizotomy, for individuals with cerebral palsy. Dev Med Child Neurol, 2021.
- Marsden, J., V. Stevenson, and L. Jarrett, Treatment of spasticity. Handb Clin Neurol, 2023. 196: p. 497-521.
- Gourdine-Shaw, M.C., et al., Equinus deformity in the pediatric patient: causes, evaluation, and management. Clin Podiatr Med Surg, 2010. 27(1): p. 25-42.
- Brunner, R. and G.-N. K., A critical view on the importance of treating spasticity and new options to improve function in patients with cerebral palsy GMFCS I-III. Medical Research Archives, 2023. 11(4).
- Mathevon, L., et al., Adjunct therapies to improve outcomes after botulinum toxin injection in children: A systematic review. Ann Phys Rehabil Med, 2019. 62(4): p. 283-290.
- Milne, N., M. Miao, and E. Beattie, The effects of serial casting on lower limb function for children with Cerebral Palsy: a systematic review with meta-analysis. BMC Pediatr, 2020. 20(1): p. 324.
- Mills, P.B., et al., Systematic review of adjunct therapies to improve outcomes following botulinum toxin injection for treatment of limb spasticity. Clin Rehabil, 2016. 30(6): p. 537-48.
- Niklasch, M., et al., Superior functional outcome after femoral derotation osteotomy according to gait analysis in cerebral palsy. Gait Posture, 2015. 41(1): p. 52-6.
- Multani, I., et al., Botulinum Toxin in the Management of Children with Cerebral Palsy. Paediatr Drugs, 2019. 21(4): p. 261-281.
- Kim, H. and K. Kolaski, Is botulinum toxin type A more effective and safer than other treatments for the management of lower limb spasticity in children with cerebral palsy? A Cochrane Review summary with commentary. NeuroRehabilitation, 2021. 49(1): p. 161-164.
- Brandenburg, J.E., M.J. Fogarty, and G.C. Sieck, A Critical Evaluation of Current Concepts in Cerebral Palsy. Physiology (Bethesda), 2019. 34(3): p. 216-229.
- Rosenbaum, P., Cerebral palsy: is the concept still viable? Dev Med Child Neurol, 2017. 59(6): p. 564.
- Brunner, R. and W. Strobl, Sensory function in CP: an overview and considerations for consequences. Medical Research Archives, 2023. 11(12).
- Alves-Pinto, A., M. Emch, and R. Lampe, Effects of Piano Training in Unilateral Cerebral Palsy Using Probabilistic and Deterministic Tractography: A Case Report. Front Hum Neurosci, 2021. 15: p. 622082.
- Trivedi, R., et al., Correlation of quantitative sensorimotor tractography with clinical grade of cerebral palsy. Neuroradiology, 2010. 52(8): p. 759-65.
- Yoshida, S., et al., Quantitative diffusion tensor tractography of the motor and sensory tract in children with cerebral palsy. Dev Med Child Neurol, 2010. 52(10): p. 935-40.

