Efficacy of ALIMFUS in Type II Diabetes Management
Evaluation of Airborne Low Intensity Multi Frequency Ultrasound, as an add-on Therapy in Type II Diabetic Patients: Self-controlled cross over study
Vyankatesh Shivane¹, Rohit Barnabas², Sanjay Tamoli³, Swapnali Mahadik³, Saba Samad Memon², Tushar Bandgar², Bharat Mehta⁴
Abstract
Background: Airborne Low Intensity Multi Frequency Ultrasound (ALIMFUS) is a novel add-on therapy mechanical therapy working on low intensity ultrasonography principle.
Materials and methods: This was an open label, self-controlled cross over, single centre, interventional, prospective clinical study, to study efficacy and safety of ALIMFUS in type II Diabetes using ambulatory glucose monitoring methods.
Results: After screening the subjects (n=48), 33 patients were included. There were 17 male (51.51%) and 16 female (48.48%) with mean age 52.39±9.39 years and duration of diabetes was 7.51±3.27 years. All the subjects were on 2/3 oral hypoglycemic agents with none being on insulin. 42.42% had dyslipidaemia and 33.33% had hypertension. There was an increase in time in range (65.96±19.72 to 66.73±19.92 mg/dL and time above range (26.40±22.51 to 27.21±21.01 mg/dL), there was reduction in time below range (7.64±11.66 to 6.06±12.33 mg/dL). There was significant reduction in Hba1C (8.07±0.90 % to 7.87±0.80 %, p 0.010), VLDL (31.07±18.13 to 28.54±14.52, p 0.001) and Total cholesterol: High density lipoprotein levels (3.64±0.75 to 3.45±0.67, p 0.010). Global assessment of overall efficacy by the investigator showed 68.74% had much improvement/no change. None had adverse events with good tolerability in all.
Conclusions: Airborne Low Intensity Multi Frequency Ultrasound showed significant HbA1C reduction and no significant change in ambulatory glucose monitoring parameters. ALIMFUS may be considered as an non-invasive, safe and well tolerated add-on novel technology in patients with uncontrolled glycemia.
Keywords: Type 2 diabetes, Airborne ultrasound, Glycemic control
Introduction:
Diabetes mellitus, a condition marked by elevated blood sugar levels and heightened cardiovascular risk, is becoming increasingly common, especially in developing nations. The metabolic characteristics of Asian Indians are distinct, having higher levels of abdominal obesity and visceral fat, with insulin resistance, dyslipidemia, and elevated inflammatory markers. All of these contribute to an increased risk of diabetes and early cardiovascular disease. The age of onset of type 2 Diabetes is also lower.
Current treatments for diabetes consist of dietary and lifestyle changes, as well as oral medications and injectable therapies, which can effectively manage the condition but may sometimes cause side effects like gastrointestinal discomfort, hypoglycaemia, weight gain, etc. Resistance to oral hypoglycaemic agents leading to therapeutic failure can evolve over the course of treatment. Research for effective and safer treatment options as monotherapy or as add-on is ongoing. Prevalence of usage of complementary and alternative therapies varies from 39 to 68% in India for treatment of diabetes. These alternative therapies are used in as an add on with conventional treatments rather than as replacements. In India, a wide range of herbal remedies, including Ayurvedic, Unani, Homeopathic, and Siddha preparations, are commonly utilized, but there is a lack of robust data on their effectiveness, and questions remain about their safety, especially heavy metal toxicity.
Yoga, acupuncture, biofeedback, aromatic therapy and hydrotherapy are physical therapy modalities which are used as alternatives to conventional therapies. Ultrasound is a promising modality as a form of physical therapy. Ultrasound consists of mechanical waves created by a piezoelectric crystal, with frequencies that exceed human hearing capabilities. The biological effects of therapeutic ultrasound differ according to the frequency and intensity of the waves used. High-intensity ultrasound tends to produce thermal effects, while low-intensity ultrasound primarily generates mechanical (compression) effects.
Airborne Low-Intensity Multi-frequency Ultrasound (ALIMFUS)-GLUCOSTIM operates on the principle of low-intensity ultrasound, generating sound waves between 20 kHz and 65 kHz using quartz crystals and advanced Vibron technology. It utilizes both thermal and non-thermal effects through mechanisms such as sonophoresis, sonoporation, and acoustic streaming.
HbA1C is conventionally used as a marker of glycaemic control and to monitor complications however it does not reflect glycaemic variability adequately. Ambulatory glucose monitoring (AGM) is being increasingly used to overcome the shortcomings of conventional measures. Measures such as time in range (TIR), time below range (TBR), time above range (TAR) gives a more accurate representation of glycaemic control, hypoglycaemic and hyperglycaemic events. American Diabetes Association (ADA) recommends TIR above 70% as a therapeutic goal.
A clinical trial assessing the efficacy and safety of ALIMFUS revealed a modest and statistically insignificant reduction in HbA1c, quality of life scores, and inflammation markers compared to the placebo group. However, there was a notable improvement in lipid profiles, as well as fasting and postprandial glucose levels in participants with HbA1c greater than 8%. Data on AGM in patients using ALIMFUS is scarce, we aimed to evaluate the efficacy and safety of ALIMFUS-GLUCOSTIM as an add-on therapy to OHAs in Type II Diabetic Patients using AGM.
Materials and Methods:
This was an open label, self-controlled cross over, single centre, interventional, prospective clinical study which was conducted after approval from Ethics Committee. The study was registered in the clinical trial registry of India (CTRI/2022/09/045734) and patients were enrolled between Nov 2022 to Jan 2023. Informed consent was obtained in writing from each participant prior to their inclusion in the study.
Patients: 18-70 year old Patients with uncontrolled Type 2 Diabetes with HbA1C 7-10% on stable dose of 2-3 OHAs for the last 8 weeks were screened for inclusion. The patients were excluded if they had renal disease, chronic kidney disease (estimated glomerular filtration rate <60 ml/min/1.73m2), active malignancy, tuberculosis, recent significant cardiovascular event in the last 12 weeks, acute complications of diabetes like ketoacidosis or hyperosmolar nonketotic hyperglycaemia, severe peripheral vascular disease, severe non-proliferative or proliferative diabetic retinopathy or macular edema, diabetic foot disease requiring treatment, human immunodeficiency virus (HIV), Hepatitis B or C, recent use investigational drug within one month, pregnancy and lactation. All those with known hypersensitivity to ultrasound or skin allergy.
Intervention: After recruiting the patients ambulatory glucose monitoring (AGM) was applied on the arm of the subject throughout study period (14 days). Subjects were allowed to continue their OHAs without exposing to “Glucostim” an ALIMFUS device being manufactured by maser electronics with exclusive authorization to aquatic remedies Pvt. Ltd. for the first 5 days. From the 6th day onwards to 14th Day subjects were called at the study site and exposure to ALIMFUS was given for 20 minutes as per the standard protocol for ALIMFUS therapy as follows.
- Select a quiet and peaceful place to sit with minimum disturbance.
- Sit on a chair at a distance of 5 feet, as shown in the below figure with your clothes on so that maximum part of your abdomen gets exposed to the sound waves.
- Plug the device – Glucostim at on standard 110/230 V AC electrical outlet, it will emit a ‘beep’ tone and the LED on the front panel will start blinking.
- Device will emit a start tune and the light emitting diode (LED) on the front panel will start blinking.
- After 20 minutes at the second beep sound, the unit will stop emitting any further sound waves.
- Close the device and perform your regular activities thereafter.
Assessment of efficacy and safety:
Primary objectives for evaluation of efficacy and safety, were percentage change in glycaemic control through evaluation of time in range (TIR), time below range (TBW), time above range (TAR) with 9 days of ALIMUS treatment and change in daily average blood sugars on day 5 + 2 days and day 14 + 2 days, HbA1c% from baseline to day 14. Secondary objectives were changes in Hemogram, CRP, Vitamin D, homocysteine and lipid profile before and after exposure to ALIMFUS. Global assessment of overall change after treatment, tolerability of ALIMFUS by investigator and subject and assessment of adverse events.
Statistical analysis:
SPSS version 25.0 (IBM, Armonk, NY) software was used for analysis. Quantitative measures were expressed as mean ± standard deviation, or median with range as applicable. Chi-Square test was used for categorical data and t-test was used for qualitative variables. Paired t-test was performed for the difference between baseline and post-intervention. Two-sided significance test was used for all p values, and all the statistical tests were interpreted at least up to 5% level of significance. Intention to treat population and per-protocol population analysis was used for the analysis of efficacy variables. Those who did not complete the study schedule, the values of the last visit were considered for final analysis (Last Observation Carry Forward) for intent to treat analysis. All patients who had received at least one exposure were conserved for safety analysis.
Results:
A total of 48 subjects were screened in the study of which 15 were screen failures and 33 subjects were recruited.
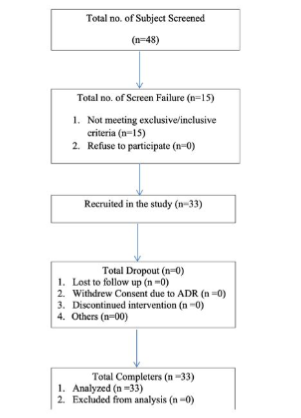
All 33 subjects completed the study and there were no drop-outs. All the cases that completed the study considered as “Per Protocol Population” as per protocol. Also, all the cases who had been exposed to ALIMFUS were considered as “safety population” and were evaluated. There were 17 male (51.51%) subjects and 16 female (48.48%). The mean (SD) age was 52.39 (9.39) years and mean (SD) duration of diabetes being 7.51 (3.27) years. All the subjects participating in the study were on 2 to 3 OHAs with none being on insulin. 42.42% patients had dyslipidaemia and 33.33% of patients had hypertension.
Table 1: Baseline Characteristics
| Parameter | No. of participant/Value |
|---|---|
| Total Participants | 33 |
| Mean Age in Years (SD) | 52.39 (9.39) (range 27-70 years) |
| Male | 17 (51.51%) |
| Female | 16 (48.48%) |
| Clinical features | |
| Systolic blood pressure, mean (SD) | 134.18 (15.35) |
| Diastolic blood pressure, mean (SD) | 81.90 (10.42) |
| Heart rate, mean (SD) | 85.09 (11.95) |
| Respiratory rate, mean (SD) | 13.72 (1.64) |
| Laboratory features | |
| Average Blood glucose levels, AGM, mean (SD) | 148.93 (38.29) |
| Hba1C, mean (SD) | 8.07 (0.90) |
| Haemoglobin, mean (SD) | 12.62 (1.75) |
| ESR, mean (SD) | 15.06 (11.62) |
| Diabetes history | |
| Average duration of Diabetes, mean (SD) | 7.51 (3.27) years |
| Type of Oral Antidiabetic Medications | |
| Dipeptidyl peptidase-4 inhibitor | 28/33 |
| Metformin | 24/33 |
| Sulphonyl urea | 23/33 |
| Thiazolidinedione | 9/33 |
| SGLT2 inhibitor | 5/33 |
| Alpha glucosidase inhibitor | 2/33 |
| Number of Oral Antidiabetic Medications | 1, 2, 3, 4, 5 |
| Co-morbidities | |
| Dyslipidemia | 14/33 (42.42%) |
| Hypertension | 11/33 (33.33%) |
Table 2: Outcomes of patients after treatment with ALIMFUS
| Primary outcomes | AGM Characteristics Before Treatment (BT) (n=33) | After Treatment (AT) (n=33) | P value |
|---|---|---|---|
| TIR, Mean (SD) | 65.96 (19.72) | 66.73 (19.92) | 0.766 |
| TBR, Mean (SD) | 7.64 (11.66) | 6.06 (12.33) | 0.172 |
| TAR, Mean (SD) | 26.40 (22.51) | 27.21 (21.01) | 0.7631 |
| BSL, Mean (SD) | 148.93 (38.29) | 149.11 (32.81) | 0.963 |
| HbA1c % , Mean (SD) | 8.07 (0.90) | 7.87 (0.80) | 0.011 |
| Secondary outcomes | Baseline (n=33) | End of study (14 Days) (n=33) | P value |
|---|---|---|---|
| Total cholesterol (mg/dL), Mean (SD) | 169.95 (40.80) | 164.78 (37.84) | 0.224 |
| Serum. Triglycerides (mg/dL), Mean (SD) | 155.35 (90.65) | 142.59 (72.67) | 0.214 |
| LDL (mg/dL), Mean (SD) | 106.51 (31.31) | 104.81 (30.50) | 0.537 |
| HDL (mg/dL), Mean (SD) | 47.41 (10.84) | 48.26 (8.91) | 0.431 |
| VLDL (mg/dL), Mean (SD) | 31.07 (18.13) | 28.54 (14.52) | 0.218 |
| TC: HDL, Mean (SD) | 3.64 (0.75) | 3.45 (0.67) | 0.012 |
| LDL: HDL, Mean (SD) | 2.27 (0.58) | 2.19 (0.57) | 0.130 |
| CRP (mg/L), Mean (SD) | 0.56 (0.69) | 0.46 (0.42) | 0.384 |
| Serum. Homocysteine (𝜇mol/L), Mean (SD) | 16.32 (7.22) | 15.97 (6.79) | 0.503 |
| Vitamin D3 (nmol/L), Mean (SD) | 25.67 (21.46) | 27.11 (25.21) | 0.308 |
Global assessment of overall efficacy by the investigator showed 13/32 subjects (40.62%) reported no change, 9/32 (28.12%) had improvement while 10/32 subjects (31.25%) had minimal worsening in their condition. None of the participants experienced any adverse events during the course of the study and showed no intolerance with exposure to ALIMFUS on global assessment of overall tolerability.
Discussion:
This present study conducted to evaluate efficacy and safety of ALIMFUS, as an add-on Therapy in Type II Diabetic Patients to oral hypoglycaemic agents using ambulatory glucose monitoring. ALIMFUS showed no statistically significant change in time in range (TIR), time below range (TBR), time above range (TAR) and daily average blood glucose level, however there was a significant reduction in HbA1C% after therapy. Secondary outcomes of Total Cholesterol (TC): High density lipoprotein (HDL) ratio reduced significantly with therapy. The therapy was safe with no device or intervention-related adverse events.
HbA1C used a primary tool used for assessment of glycaemic control can have limitations as it is an indirect measure and multiple non glycaemic factors can affect its measurement. Ambulatory glucose monitoring (AGM) is being increasingly used to overcome these, AGM parameter especially time in range (TIR) is associated with microvascular complications risk. Continuous glucose monitoring (CGM) is recommended to be used in type 1 and type 2 diabetic patients, especially those with multiple daily injections, which measures interstitial glucose. There can be variation in the accuracy of commonly used blood glucose monitoring devices. Previous studies using ALIMFUS have showed significant reduction in fasting and post prandial blood glucose, however ambulatory glucose monitoring (AGM) has been sparingly used. This study showed that there was no significant difference in ambulatory glucose monitoring (AGM) parameters after therapy.
The level of reduction in HbA1C with ALIMFUS used previously was comparable to that of SGLT2 inhibitors, α glucosidase inhibitors and DDP-4 inhibitors. However in the present study there was significant reduction in the Hba1C but to a lesser level, this could be due to shorter duration of follow up. HbA1C is a measure of average glycemia which has limitation, especially conditions which affect blood cell turnover, blood transfusions, kidney disease or pregnancy. Ethnic variations can also be seen. The possible mechanisms of ultrasound in improving glycaemic control proposed are increased insulin release from beta cells. Ultrasound exposure temporarily alters the cell membrane, causing calcium influx that triggers the exocytosis of insulin granules. This effect is reversible and short-lived. Mechano-transduction leads to activation of signalling pathways eventually leading to stimulation of mechano-sensitive membrane ion proteins. The other mechanisms are sonoporation where transient alteration of cell membrane leads to increased uptake of low and high molecular weight substances. Ultrasound therapy may also play a role in improving insulin resistance, gluconeogenesis and reducing glucagon secretion observed previously.
There was significant reduction was observed in TC/HDL ratio with ALIMFUS therapy, other parameters of lipid profile also showed a trend towards reduction as was observed in the previously. The mechanism for this is not clear, however ultrasonic lipolysis used in obese women showed improvement in blood cholesterol levels and abdominal fat.
Global assessment of overall efficacy by the investigator showed that majority of patients had no change or much improvement with therapy (68.75%). The device was well tolerated with no side effects in our study. Previous studies have shown improvement in diabetes symptom scores and quality of life scores.
The major limitations of our study was short duration of follow-up and small sample size, however the use of ALIMFUS as an add on therapy was safe with few side effects and improvement in HbA1C and lipid profile was noted. However larger studies are needed.
Conclusion:
Airborne Low Intensity Multi Frequency Ultrasound may be considered as an safe, non-invasive add-on novel technology in patients with uncontrolled glycemia. There was no significant change in ambulatory glucose monitoring parameters with significant HbA1C reduction. This was a safe therapy with good tolerability. However further long-term studies are needed to show its effective role as an add-on therapy.
Data availability statement:
Authors confirm that data supporting the findings of this study are available within the article.
Conflict of Interest:
None
Funding:
Aquatic Remedies Ltd, located at 1208e1211, Cabin B, 12th Floor, Universal Majestic, P. L. Lokhande Marg, Chembur (W), Mumbai 400043 and MASER Electronics PVT. LTD.
Disclosure Summary:
The authors have nothing to disclose.
Author contribution:
VS, RB, ST, SM, SSM, TB and BM designed the trial. VS, ST and SM performed the clinical trial. RB, VS, and SSM wrote the article. VS, RB and SSM analysed the data. All authors interpreted the data and revised the article. VS is the guarantor.
Consent for publication:
All the co-authors have consented to the publication of the study results.
Availability of data and material:
Authors confirm that data supporting the findings of this study are available within the article.
Acknowledgements:
None
References:
- Dagenais GR, Gerstein HC, Zhang X, et al. Variations in Diabetes Prevalence in Low-, Middle-, and High-Income Countries: Results From the Prospective Urban and Rural Epidemiological Study. Diabetes Care. 2016;39 (5):780-787. doi:10.2337/dc15-2338
- Shah VN, Mohan V. Diabetes in India: what is different? Curr Opin Endocrinol Diabetes Obes. 2015;22 (4):283-289. doi:10.1097/MED.0000000000000166
- Pandey A, Tripathi P, Pandey R, Srivatava R, Goswami S. Alternative therapies useful in the management of diabetes: A systematic review. J Pharm Bioallied Sci. 2011;3 (4):504-512. doi:10.4103/0975-7406.90103
- Vishnu N, Mini GK, Thankappan KR. Complementary and alternative medicine use by diabetes patients in Kerala, India. Glob Health Epidemiol Genom. 2017;2:e6. doi:10.1017/gheg.2017.6
- Misra A, Gulati S, Luthra A. Alternative medicines for diabetes in India: maximum hype, minimum science. Lancet Diabetes Endocrinol. 2016;4 (4):302-303. doi:10.1016/S2213-8587 (15)00515-X
- Milanese C, Cavedon V, Piscitelli F, Zancanaro C. Effect of low-intensity, low-frequency ultrasound treatment on anthropometry, subcutaneous adipose tissue, and body composition of young normal weight females. J Cosmet Dermatol. 2014;13 (3):202-207. doi:10.1111/jocd.12101
- Suarez Castellanos I, Jeremic A, Cohen J, Zderic V. Ultrasound Stimulation of Insulin Release from Pancreatic Beta Cells as a Potential Novel Treatment for Type 2 Diabetes. Ultrasound Med Biol. 2017;43 (6):1210-1222. doi:10.1016/j.ultrasmedbio.2017.01.007
- Yang C, Li Y, Du M, Chen Z. Recent advances in ultrasound-triggered therapy. J Drug Target. 2019;27 (1):33-50. doi:10.1080/1061186X.2018.1464012
- Shivane V, Pathak H, Tamoli S, et al. Effect of Airborne Low Intensity Multi frequency ultrasound (ALIMFUS) on glycemic control, lipid profile and markers of inflammation in patients with uncontrolled type 2 diabetes: A multicentre proof of concept, randomized double blind Placebo controlled study. Diabetes Metab Syndr. 2022;16 (5):102483. doi:10.1016/j.dsx.2022.102483
- American Diabetes Association Professional Practice Committee. 6. Glycemic Goals and Hypoglycemia: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47 (Suppl 1):S111-S125. doi:10.2337/dc24-S006
- American Diabetes Association Professional Practice Committee. 7. Diabetes Technology: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47 (Suppl 1):S126-S144. doi:10.2337/dc24-S007
- Brazg RL, Klaff LJ, Parkin CG. Performance variability of seven commonly used self-monitoring of blood glucose systems: clinical considerations for patients and providers. J Diabetes Sci Technol. 2013;7 (1):144-152. doi:10.1177/193229681300700117
- King F, Ahn D, Hsiao V, Porco T, Klonoff DC. A Review of Blood Glucose Monitor Accuracy. Diabetes Technol Ther. 2018;20 (12):843-856. doi:10.1089/dia.2018.0232
- Nathan DM, Buse JB, Davidson MB, et al. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2009;32 (1):193-203. doi:10.2337/dc08-9025
- Bergenstal RM, Gal RL, Connor CG, et al. Racial Differences in the Relationship of Glucose Concentrations and Hemoglobin A1c Levels. Ann Intern Med. 2017;167 (2):95-102. doi:10.7326/M16-2596
- Khosla L, Bhat S, Fullington LA, Horlyck-Romanovsky MF. HbA1c Performance in African Descent Populations in the United States With Normal Glucose Tolerance, Prediabetes, or Diabetes: A Scoping Review. Prev Chronic Dis. 2021;18:E22. doi:10.5888/pcd18.200365
- Selvin E. Are There Clinical Implications of Racial Differences in HbA1c? A Difference, to Be a Difference, Must Make a Difference. Diabetes Care. 2016;39 (8):1462-1467. doi:10.2337/dc16-0042
- ter Haar G. Therapeutic applications of ultrasound. Prog Biophys Mol Biol. 2007;93 (1-3):111-129. doi:10.1016/j.pbiomolbio.2006.07.005
- Lavrinenko YeE. Low-Frequency Ultrasound Therapy in Combination Treatment of Patients with Type 2 Diabetes Mellitus. Mìžnarodnij endokrinologìčnij žurnal. 2013; (3.51):30-34. doi:10.22141/2224-0721.3.51.2013.84315
- ElGendy MH, Mohamed AZ, Professor of Int. Medicine , Faculty of Medicine , Cairo University, Egypt., et al. Efficacy of ultrasonic lipolysis on blood cholesterol level in centrally obese women. IJPR. 2017;5 (4):2164-2170. doi:10.16965/ijpr.2017.163

