Emerging Technologies in Aging Face Assessment
Emerging Technologies for Assessing Anthropometric and Dental Variables in the Aging Face – A Scoping Review
Panagiota Chatzidou¹, Olga Naka², Nikolaos Kokolantonakis³ and Vassiliki Anastassiadou⁴
- Research Fellow, Department of Prosthodontics, School of Dentistry, Aristotle University of Thessaloniki, Greece
- Associate Professor of Prosthodontics, Aristotle University of Thessaloniki, Greece
- Undergraduate Student, School of Dentistry, Aristotle University of Thessaloniki, Greece
- Professor of Prosthodontics and Geriatric Dentistry, Aristotle University of Thessaloniki, Greece
OPEN ACCESS
PUBLISHED: 30 September 2025
CITATION: Chatzidou, P., Naka, O., et al., 2025. Emerging Technologies for Assessing Anthropometric and Dental Variables in the Aging Face – A Scoping Review. Medical Research Archives, [online] 13(9).
https://doi.org/10.18103/mra.v13i9.6898
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i9.6898
ISSN 2375-1924
Abstract
Age-related changes in craniofacial morphology—such as skeletal resorption, soft tissue volume loss, altered occlusion, and progressive tooth loss—profoundly affect the vertical dimension and overall aesthetic balance of the ageing face. For plastic surgeons seeking comprehensive facial rejuvenation, these anatomical alterations present both challenges and opportunities. Traditional assessment methods, including two-dimensional imaging and manual anthropometry, often fall short in capturing the complex, three-dimensional interplay between facial structures and dentition. Recent advances in digital technologies—such as three-dimensional facial scanning, cone-beam computed tomography, digital intraoral scanning, and artificial intelligence-driven morphometric analysis—offer high-resolution, reproducible, and non-invasive alternatives for evaluating these variables with greater accuracy. This scoping review examined how such technologies enhance the assessment of craniofacial and dental parameters in adults aged, with a focus on optimizing vertical dimension and facial aesthetics. Using the Patient Intervention Comparison Outcome framework, relevant studies (n = 70) were identified through a structured search and evaluated for methodological rigor and clinical relevance. The findings from n=21 studies were synthesized using Bloom’s Taxonomy as a cognitive framework, enabling a deeper understanding of how these tools contribute to knowledge acquisition, clinical application, and innovation in aesthetic planning. The review highlighted the diagnostic and planning benefits of integrating digital dental data into facial aesthetic procedures, thereby promoting interdisciplinary collaboration between prosthodontists and plastic surgeons. Ultimately, this study emphasized the significance of emerging technologies in enabling personalized, evidence-based approaches to facial rejuvenation in aging populations, with a specific focus on restoring vertical dimension and attaining harmonious aesthetic results.
Keywords
Ageing face, vertical dimension, facial aesthetics, digital anthropometry, prosthodontic rehabilitation, 3D facial scanning, interdisciplinary rejuvenation
List of Abbreviations
| Abbreviation | Meaning |
|---|---|
| 2D | Two-Dimensioned |
| 3D | Three-Dimensioned |
| AI | Artificial Intelligence |
| ANOVA | Analysis of Variance |
| CAD/CAM | Computer-Aided Design / Computer-Aided Manufacturing |
| CBCT | Cone-Beam Computed Tomography |
| DD | Duplicate Dentures |
| DIOS | Digital Intraoral Scanning |
| DOI(s) | Digital Object Identifier(s) |
| EED | Eye-ear distance |
| FTUs | Functional Tooth Units |
| G-SP | Glabella-Soft Pogonion |
| ICCs | Intra-class Correlation Coefficients |
| ICD | Intercondylar Distance |
| IOS | Intraoral Scanning |
| MeSH | Medical Subject Headings |
| OBJ | Object Files |
| OR | Occlusion Rims |
| OVD | Occlusal Vertical Dimension |
| PS | Primescan |
| Sn-Gn | Distance between the septum of the nose [Sn] and the tip of the chin [Gn] |
| Sn-Me | Subnasal to menton |
| SN-SP | Subnasal-Soft Pogonion |
| SPSS | Statistical Package for the Social Sciences |
| STL | Standard Triangle/Tessellation Language |
| VD | Vertical Dimension |
| VDO | Vertical Dimension of Occlusion = OVD |
1.0 Introduction
The global demographic profile is shifting toward a significantly older population, creating unique challenges for healthcare systems, particularly in the field of prosthodontics. With age, individuals experience progressive craniofacial changes including skeletal resorption, facial soft tissue atrophy, and dental deterioration, which compromise both aesthetics and function. Moreover, reductions in facial volume and alterations in occlusal vertical dimension (OVD) are frequently observed in ageing adults, with direct repercussions for prosthetic treatment planning. Classical approaches such as manual anthropometry and two-dimensional cephalometry, have been widely applied to assess these changes. However, they suffer from poor reproducibility, low spatial resolution, and failure to accurately capture three-dimensional anatomical complexities. Yiallouridou et al demonstrated that while extraoral anthropometric measurements change with age and sex, they often poorly correlate with intraoral variables, highlighting limitations in conventional measurement tools. Similarly, Srinivasan et al revealed significant discrepancies between analog and 3D vertical dimension measurements in edentulous patients, raising questions about the accuracy and reliability of current digital registration methods. Accurate OVD restoration is especially critical in edentulous rehabilitation. Goldstein et al highlighted the absence of a consensus gold standard for OVD determination, underscoring the clinical importance of reliable and reproducible methods. As an alternative, Morata et al introduced a craniometry-based predictive model using stable skull landmarks to estimate OVD, although its applicability to geriatric populations with craniofacial asymmetry remains unclear. Notably, a recent verification study in older patients confirmed that while craniometric models may offer a starting point, they require further validation across diverse populations.
Recent advances in digital technologies offer promising solutions to these diagnostic challenges. Three-dimensional (3D) facial scanning, cone-beam computed tomography (CBCT), digital intraoral scanning, and artificial intelligence (AI)-driven morphometric analysis provide high-resolution, non-invasive, and reproducible tools for assessing craniofacial and dental structures. These technologies enable a comprehensive evaluation of both hard and soft tissue morphology, allowing for dynamic visualization and quantitative analysis of the ageing face. Importantly, they offer the potential to integrate facial and dental data into a unified digital environment, enhancing the precision of prosthodontic treatment planning. Together, these technologies represent a paradigm shift in geriatric dental care, allowing clinicians to diagnose, plan, and deliver prosthodontic treatment with greater accuracy and individualized attention. Swift et al highlighted the ‘inside-out’ process of facial aging, demonstrating how bone resorption, changes in fat distribution, and soft tissue thinning collectively lead to facial volume reduction and misalignment of skeletal landmarks. High-resolution 3D imaging can capture these changes and facilitate precise mapping of facial, skeletal, and dental structures. For example, face scanners enable digital OVD measurement with intra-class correlation coefficients (ICCs) sufficiently high to detect subtle vertical changes. Nonetheless, digitized measurements consistently showed systematic differences from analog records, indicating a lack of clinical equivalence.
Beyond the technical domain, there is limited literature on how clinicians cognitively engage with emerging digital tools. Bloom’s Taxonomy provides a robust framework for examining how practitioners acquire knowledge, interpret morphometric data, apply it in planning, evaluate prosthetic designs, and ultimately create individualized digital workflows. Understanding these cognitive transitions is central to integrating AI-enabled digital diagnostics into routine geriatric practice. Despite advances in digital imaging and landmark-based predictive models, their applicability in older adults remains underexplored. Existing studies primarily involve younger or mixed-age cohorts, with limited reports addressing age-specific anatomical variability. Furthermore, digital tools often yield conflicting measurements compared to analog methods, highlighting a gap in validating their clinical reliability in older, edentulous populations. There is also a knowledge gap in mapping clinician decision-making and adoption processes through cognitive frameworks, such as Bloom’s Taxonomy.
This scoping review aimed to evaluate the role of emerging digital technologies in assessing craniofacial and dental variables, with particular emphasis on OVD, in adults, and to compare them with conventional analog methods. The objectives of the present study were to catalogue key digital technologies—3D facial scanning, cone-beam computed tomography (CBCT), digital intraoral scanning (IOS), and AI-based morphometric analysis—utilized in geriatric craniofacial and dental assessment; to evaluate their diagnostic accuracy and reliability relative to conventional anthropometric and cephalometric methods, focusing on vertical dimension, skeletal resorption, and facial volume loss; to assess their clinical impact on prosthodontic treatment planning, restoration design, and patient outcomes; to apply Bloom’s Taxonomy in analyzing clinicians’ cognitive progression in adopting these technologies; and to identify existing evidence gaps while recommending future research directions to enhance validation, standardization, and clinical translation of digital tools in ageing patient care.
2.0 Materials and Methods
The present scoping review employed a rigorous methodology guided by the PRISMA framework to evaluate the integration of emerging digital technologies in craniofacial and dental assessment among older adults (Figure 1). The study protocol was structured using the PICO framework to ensure methodological clarity: Population (human participants adults with various ages), Intervention (advanced digital technologies including 3D facial scanning, cone-beam computed tomography (CBCT), digital intraoral scanners, and artificial intelligence-based morphometric analysis), Comparison (conventional anthropometric and two-dimensional imaging methods), and Outcomes (diagnostic accuracy, reliability, clinical utility, and contributions to prosthodontic and aesthetic treatment planning).
A comprehensive search strategy was developed and executed across key electronic databases including PubMed, Embase, Scopus, Web of Science, and the Cochrane Library. Controlled vocabulary (MeSH terms) and keywords such as “ageing face,” “digital dentistry,” “3D imaging,” “CBCT,” “intraoral scanner,” “artificial intelligence,” and “prosthodontics” were combined using Boolean operators. The search was limited to peer-reviewed articles published in English from 2000 onwards. Additionally, relevant articles were selected through hand-searching.
The study selection process involved a two-stage screening procedure conducted independently by two reviewers. Titles and abstracts were initially screened using predefined inclusion and exclusion criteria based on the PICO framework, followed by a full-text review of studies deemed potentially eligible. Discrepancies were resolved through discussion or consultation with a third reviewer. A standardized data extraction form was used to gather study characteristics, participant demographics, intervention details, and outcome measures from 70 included studies.
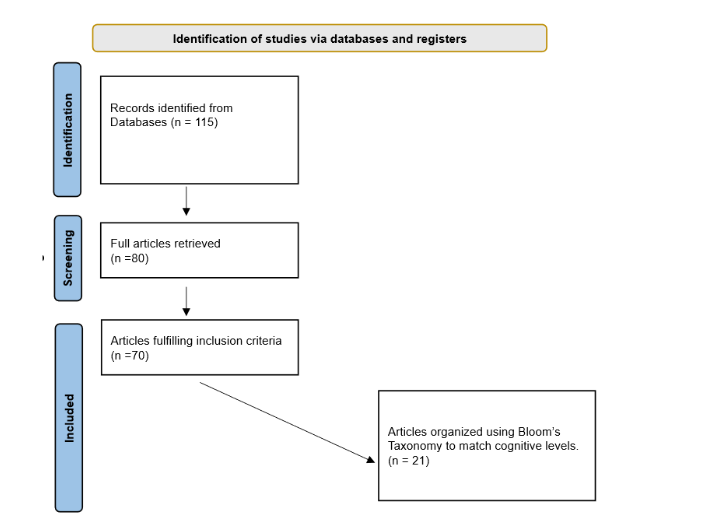
Data synthesis (from 21 studies) was structured using Bloom’s Taxonomy as a cognitive framework, categorizing evidence according to the levels of knowledge acquisition, comprehension, application, analysis, evaluation, and creation. Foundational studies elucidating biological and morphological changes with ageing were classified at the lower cognitive levels “Remembering and Understanding”. In contrast, clinical validation and implementation studies of digital technologies were assigned to the “Applying” and “Analyzing” levels. Studies addressing clinical decision-making, technology integration, and innovation were mapped to the higher-order “Evaluation and Creation” levels (Figure 2).

Quality assessment and transparent reporting were guided by PRISMA standards, ensuring methodological rigor and comprehensive documentation from study identification through evidence synthesis. This approach facilitated a thorough exploration of how digital assessment tools improve diagnostic precision and clinical outcomes in geriatric prosthodontics, highlighting current research gaps and informing future innovation.
3.0 Results
3.1 A CATALOGUE OF KEY DIGITAL TECHNOLOGIES
Advancements in digital technologies have revolutionized the assessment and management of craniofacial and dental conditions in geriatric populations. Key innovations, including three-dimensional (3D) facial scanning, cone-beam computed tomography (CBCT), digital intraoral scanning (DIOS), and artificial intelligence (AI)-based morphometric analysis, have enhanced diagnostic precision and treatment planning, particularly in prosthodontics.
3D facial scanning utilizes structured light, laser triangulation, or photogrammetry to generate highly accurate surface models of the face, capturing detailed facial contours, symmetry, volume loss, and vertical dimension changes crucial for aesthetic and functional prosthodontic planning. In older adults, this technology facilitates the evaluation of age-related volume loss and midface flattening, monitors perioral structural changes during denture use, aids in determining the occlusal vertical dimension (OVD), and supports virtual smile design and facially driven restorations. The method is non-invasive, rapid, reproducible, and free of ionizing radiation, making it suitable for clinical use. Srinivasan et al demonstrated the reliability of 3D facial scanning in measuring OVD in edentulous patients, while Gibelli validated its accuracy compared to CBCT, confirming its diagnostic value.
CBCT offers high-resolution, three-dimensional imaging of hard tissues, including bone and teeth, with significantly lower radiation exposure compared to conventional computed tomography. It is indispensable for assessing alveolar ridge resorption, sinus pneumatization, and mandibular morphology in the elderly. Clinically, CBCT enables precise evaluation of alveolar ridge resorption prior to implant placement, assessment of skeletal asymmetries and resorptive patterns, planning implant-supported overdentures in atrophic jaws, and determination of bone volume for facial support in full-mouth rehabilitation. Jacobs et al emphasized the utility of CBCT in geriatric implant planning, and Schuster et al employed CBCT to quantify bone resorption patterns in edentulous patients.
Digital intraoral scanning (IOS) captures detailed impressions of the dentition and soft tissues in real-time, replacing traditional impression materials. IOS offers enhanced patient comfort, instantaneous 3D visualization, and streamlined clinical workflows. In geriatric populations, IOS is used to capture residual ridge anatomy, monitor prosthetic fit and mucosal changes, facilitate digital denture design with CAD/CAM integration, and detect occlusal wear and prosthetic misalignments. Bilgin et al confirmed the feasibility and accuracy of IOS in scanning edentulous arches, while Srivastava et al demonstrated its effectiveness in elderly patients with partial edentulism.
AI-based morphometric analysis leverages machine learning and deep learning algorithms to analyze large datasets from 3D imaging technologies. These models automate pattern recognition, landmark detection, and predictive modeling, augmenting prosthodontic diagnostics and treatment planning. Applications include the automated detection of facial landmarks critical for OVD estimation, the prediction of age-related morphological changes, personalized denture design that accounts for facial symmetry and volume loss, and enhanced diagnostics in cases of facial collapse or asymmetry. AI enables rapid data processing, reduces inter-operator variability, and offers scalability. Kavousinejad et al applied morphometric AI to detect age- and gender-related craniofacial changes, and Myer et al demonstrated AI-driven predictive facial aging models for reconstructive planning. Kim et al employed deep learning for the automated identification of facial landmarks in prosthetic planning.
Collectively, these digital technologies (Table 1) offer a comprehensive and multidimensional approach to geriatric craniofacial and dental assessment. Their integration enhances diagnostic accuracy and reliability, and improves treatment outcomes by enabling precise, individualized prosthodontic interventions tailored to the complex anatomical changes associated with aging patients.
| Soft Tissue Technologies | Technology Overview | Clinical Applications in Older Adults | Advantages | Key References (with DOIs) |
|---|---|---|---|---|
| Two and Three-Dimensional (3D) Facial Scanning | Uses structured light, laser triangulation, or stereophotogrammetry to capture detailed surface anatomy of the ageing face. | – Assess perioral tissue loss, midface flattening, and VDO. – Support aesthetic design of prostheses. – Monitor facial changes post-therapy. |
Non-invasive, radiation-free, high-resolution, real-time, reproducible. | Yiallouridou et al, 2023 https://doi.org/10.3390/app131910860 Srinivasan et al, 2024 https://doi.org/10.1016/j.jdent.2024.105016 |
| Artificial Intelligence (AI)-Based Morphometric Analysis | Applies machine learning and neural networks to analyze 3D facial and cranial data for automated diagnostics and predictive modelling. | – Detect craniofacial ageing patterns. – Automate OVD estimation and landmark identification. – Optimize facial symmetry in planning. |
Automated, reduces operator variability, supports population-level modeling, and integrates with imaging tools. | Swift et al, 2021 https://doi.org/10.1093/asj/sjaa339 |
3.2 EMERGING DIGITAL TECHNOLOGIES IN GERIATRIC CRANIOFACIAL AND DENTAL ASSESSMENT
This review synthesized findings from 21 recent clinical studies that investigated various analog and digital technologies for measuring and assessing the occlusal vertical dimension (OVD) in prosthodontic rehabilitation. The studies collectively demonstrate advances in accuracy, reliability, and clinical applicability of these methods, emphasizing the growing role of digital technologies alongside traditional approaches. The results are organized according to cognitive domains of Bloom’s Taxonomy—Remembering, Understanding, Applying, Analyzing, and Evaluating—to highlight the progression of knowledge and clinical practice development. Bloom’s taxonomy provides a hierarchical framework for categorizing cognitive skills, which can be applied to analyze the levels of clinician engagement with digital technologies in geriatric craniofacial and dental assessment.
The foundational level, “Remembering”, involves basic recall and recognition of knowledge like summarizing evidence or consensus on digital diagnostic tools. “Understanding” requires a deeper grasp of concepts, such as explaining digital evaluation processes of aesthetics or interpreting workflow protocols for imaging devices. At “Applying”, clinicians use information practically, such as implementing scanning devices, using anthropometric predictors, or operating specialized software for treatment planning. “Analyzing” involves examining data, comparing diagnostic methods, identifying correlations, or conducting clinical evaluations to discern nuances in patient outcomes. “Evaluating” is a higher skill where clinicians judge the reliability, accuracy of digital tools, patient satisfaction, or expert consensus. Although “Creating”, the highest domain, is less common in current literature—focused more on evaluation rather than innovation—it remains an important goal for future progress (Tables 2-5).
“Remembering and Understanding”: Basic recall of digital diagnostic tools and understanding of evaluation processes and workflow interpretation
Basic knowledge of digital diagnostic tools involves recognizing different technologies like 3D scanners, intraoral cameras, and imaging software used in clinical assessments. Explaining their evaluation processes requires understanding how these tools collect and analyze data, as well as the workflow protocols that guide their application. This foundational understanding helps clinicians follow standard procedures accurately, ensuring consistent data collection and seamless integration of digital technologies into patient diagnosis and treatment planning (Table 2). A study by Chou et al examined how increasing occlusal vertical dimension (OVD) affects smile dynamics in 30 dental students aged 21–30. Using occlusal registrations of +0, +2, +4, +6, and +8 mm, posed smile images were analyzed. Results showed significant increases in interlabial gap height, incisal edge-to-lower lip distance, and display zone area with increased OVD (P < .001), while the smile index (width-to-height ratio) significantly decreased (P < .001). No significant changes were observed in intercommissural width or incisal edge-to-upper lip distance. These findings suggest that increasing OVD alters vertical smile dimensions and aesthetic proportions, without affecting smile width or upper lip positioning.
A clinical study by Imani et al explored a fully digital workflow that integrated intraoral and extraoral facial scanning for complete-mouth implant-supported rehabilitation in 10 edentulous patients. By utilizing digital scans to generate virtual tooth arrangements aligned with 3D facial scans, CAD-CAM technology enabled the milling of interim prostheses that functioned effectively for at least six months. This approach not only streamlined the clinical process but also contributed to more precise facial reconstruction, supporting improved aesthetics and patient satisfaction.
Building on this, Kouveliotis et al highlighted the efficiency and reproducibility of CAD-CAM complete denture workflows, emphasizing how digital technologies in prosthodontics facilitate more predictable facial support and rejuvenation outcomes. The report presented a streamlined digital workflow for fabricating a complete maxillary denture opposing an implant-retained mandibular overdenture. Using a three-visit protocol, the technique enables the accurate digital articulation of edentulous arches without the need for traditional impressions. Wax rims on relined trays recorded occlusion at the correct vertical dimension. Laboratory scans enabled precise virtual articulation of intraoral scans. The prostheses were digitally designed and milled, improving efficiency and patient comfort, with all steps documented.
Sun et al demonstrated that digitally increasing the occlusal vertical dimension (OVD) improves lower facial form and aesthetics, counteracting the sunken appearance in aged or collapsed faces. Their study increased (OVD) by 3, 6, and 9 mm, finding significant increases in lower facial height, facial height ratio, lip height, and nasolabial angle, while lip width decreased. Even a 3 mm OVD increase was noticeable, with the original OVD rated most aesthetic. Minor OVD changes can impact aesthetics, even if they met functional needs. Restoring the correct OVD via prosthodontics can create a younger, balanced face. Collectively, these findings reinforce the importance of prosthodontic rehabilitation not only in functional restoration but also in reestablishing youthful facial proportions, preventing the pseudo–Class III profile often associated with aging and loss of vertical support. Together, these studies provide a strong theoretical and conceptual foundation for subsequent practical applications, emphasizing the role of digital innovations while respecting traditional clinical wisdom.
| Authors | Technology/Method Compared | Objective | Key Findings/Outcomes | Notes | Bloom’s Taxonomy Level and Study Type |
|---|---|---|---|---|---|
| Chou et al, 2014 | Effect of increasing OVD (+0, +2, +4, +6, +8 mm) on smile dynamics | Examine how increasing OVD affects smile aesthetics in young adults | Interlabial gap height, incisal edge-to-lower lip distance, and display zone area increased significantly with OVD (P<.001); smile index (width/height ratio) decreased significantly (P<.001); no significant changes in intercommissural width or incisal edge-to-upper lip distance (P>0.05) | Showed vertical smile dimensions altered by OVD increases; aesthetic proportions affected | Understanding / Experimental Study |
| Imani et al, 2022 | Fully digital workflow integrating intraoral & extraoral facial scanning; CAD-CAM milling | Explore fully digital workflow for complete-mouth implant-supported rehabilitation in edentulous patients | Digital scans combined with 3D facial scans allowed precise virtual tooth arrangement; interim prostheses milled via CAD-CAM worked effectively for ≥6 months; streamlined process, improved facial reconstruction and patient satisfaction | Pilot clinical study with 10 patients | Understanding / Clinical Pilot Study |
| Kouveliotis et al, 2022 | CAD-CAM complete denture workflow; digital articulation of edentulous arches without traditional impressions | Demonstrate efficiency and reproducibility of digital denture workflows for facial support and rejuvenation | Three-visit protocol for full maxillary denture opposing implant overdenture; wax rims recorded occlusion at correct OVD; prostheses digitally designed and milled; improved efficiency and patient comfort | Emphasized reproducibility and documentation of digital workflow | Understanding / Clinical Case Report |
| Sun et al, 2021 | Digital increase of occlusal vertical dimension (OVD) by 3, 6, 9 mm | Assess impact of increasing OVD on lower facial form and aesthetics | Lower facial height (P<.001), facial height ratio (P<.01), lip height (P<.01), nasolabial angle (P<.001) significantly increased; lip width significantly decreased (P<.05); even 3 mm OVD increase was visibly noticeable; original OVD rated most aesthetic | Demonstrated minor OVD changes impact aesthetics; functional and aesthetic importance of VD restoration | Understanding / Quantitative Clinical Study |
“Applying”: Clinical use of scanning devices and software alongside anthropometric predictors for effective treatment planning.
A growing body of research highlights the importance of digital tools and anthropometric techniques in enhancing prosthodontic rehabilitation. These methods are especially valuable for restoring the correct facial vertical dimension (VD), which is essential for maintaining youthful facial proportions and preventing the pseudo–Class III profile often associated with aging (Table 3). A clinical study by Zhou et al compared a digitally manufactured simple intraoral Gothic arch-tracing device (T1) with a traditional device (T2) for determining centric relation in complete denture patients (n= 10). T1 significantly reduced clinical time (41.90 ± 2.64 min) compared to T2 (57.50 ± 2.37 min; P < .01). Maximum position deviations between T1 and T2 were within 0.5 mm: midline mandibular region—0.32 ± 0.14 mm (labial-lingual), 0.40 ± 0.23 mm (vertical); molar region—0.35 ± 0.23 mm (buccal-lingual), 0.33 ± 0.20 mm (vertical). No midline deviation or occlusal instability was observed. The digital device demonstrated time efficiency and comparable accuracy to traditional methods.
Rutkūnas et al showed that incorporating reference objects during intraoral scanning significantly enhances the accuracy of virtual occlusal records, enabling more precise alignment of prosthetic components and achieving balanced facial symmetry. Kaffaf and Şakar validated anthropometric measurements as a non-invasive method for predicting OVD, providing clinicians with a practical tool for restoring facial height and preserving natural contours, thereby avoiding the flattened mid-face appearance commonly associated with aging. They studied 271 adults (136 women, 135 men; mean age, 30.4), recording 36 measurements, including 4 OVDs, 24 facial parameters, and eight hand parameters using digital calipers. Pearson correlation and regression analysis revealed several strongly correlated variables (r ≥ 0.6), including pupil-to-cheilion, sellion-to-stomion, stomion-to-pogonion, and 4-finger width. Regression formulas were created from these, indicating that facial and hand dimensions can reliably predict OVD, offering a practical, non-invasive method for prosthodontics.
Figueras-Alvarez et al tested open-source software for assessing interarch space in denture wearers, providing clinicians with reliable digital tools to plan prostheses restoring vertical proportions. They proposed a digital protocol using open-access software and intraoral scanning in edentulous patients with complete dentures. The method involved 360° extraoral scans of dentures, antagonist arches, and intermaxillary records. STL files were imported into free software to measure interarch space, aiding implant-supported prosthesis planning. This workflow offers a cost-effective, efficient, and accurate alternative to traditional methods. The study demonstrated that digital assessment with accessible tools can enhance clinical decision-making, particularly in vertical space and aesthetic evaluation.
Satin et al compared occlusal vertical dimension (OVD) transfer accuracy in CAD-CAM dentures using two workflows: duplicate dentures (DD) and occlusion rims (OR), each with 15 samples. Scanned, mounted edentulous casts were analyzed in 3D. The OR group had greater deviation (0.72 ± 0.13 mm) than the DD group (0.45 ± 0.23 mm), with 98.9% showing increased OVD. A two-way ANOVA revealed significant differences between workflows (p < 0.0001), but no significant differences across measurement points. Although DD was more accurate, both methods are likely to stay within clinically acceptable limits. Collectively, these studies demonstrated that integrating digital and anthropometric strategies into prosthodontic workflows can reliably restore facial volume, improve aesthetic outcomes, support soft tissues, and promote a youthful appearance in edentulous patients.
| Authors | Technology/Method Compared | Objective | Key Findings/Outcomes | Notes | Bloom’s Taxonomy Level and Study Type |
|---|---|---|---|---|---|
| Zhou et al, 2023 | Digitally manufactured intraoral Gothic arch-tracing device (T1) vs. traditional device (T2) for centric relation | Compare efficiency and accuracy of digital vs traditional centric relation devices in complete denture patients (n=10) | T1 reduced clinical time significantly: 41.90 ± 2.64 min vs. T2: 57.50 ± 2.37 min (P < .01); max positional deviations ≤0.5 mm (midline mandibular: 0.32 ± 0.14 mm labial-lingual, 0.40 ± 0.23 mm vertical; molar: 0.35 ± 0.23 mm buccal-lingual, 0.33 ± 0.20 mm vertical); no midline deviation or occlusal instability observed. Digital device time-efficient and accurate | Sample size small; pilot clinical comparison | Applying / Clinical Comparative Study |
| Rutkūnas et al, 2023 | Use of reference objects in intraoral scanning to improve accuracy of virtual occlusal records | Enhance precision in virtual occlusal records for balanced prosthetic alignment and facial symmetry | Incorporation of reference objects improved accuracy of virtual occlusal records; enabled precise alignment of prosthetic components and balanced facial symmetry | Demonstrates practical improvement in digital scanning accuracy | Applying / Technical Improvement Study |
| Kaffaf and Şakar, 2024 | Anthropometric measurements (facial and hand) to predict occlusal vertical dimension (OVD) | Validate non-invasive anthropometric predictors for OVD restoration | Sample: 271 adults (136 women, 135 men; mean age 30.4); 36 measurements recorded; Pearson correlation coefficients r ≥ 0.6 for pupil-to-cheilion, sellion-to-stomion, stomion-to-pogonion, and 4-finger width; regression formulas developed to reliably predict OVD from these variables | Provides practical non-invasive clinical tool for VD estimation | Applying / Observational Analytical Study |
| Figueras-Alvarez et al, 2022 | Open-source software combined with intraoral and extraoral scanning to assess interarch space in denture wearers | Test a digital protocol for measuring interarch space to aid prosthesis planning and vertical proportion restoration | Utilized 360° extraoral scans of dentures and antagonist arches with STL file analysis in free software; protocol proved cost-effective, efficient, accurate alternative to traditional methods; enhanced clinical planning for vertical space and aesthetics | Demonstrates accessible digital workflow for prosthodontic assessment | Applying / Technical Protocol Validation Study |
| Satin et al, 2024 | Two CAD-CAM denture workflows for OVD transfer accuracy: duplicate dentures (DD) vs occlusion rims (OR) | Compare accuracy of two CAD-CAM workflows for transferring OVD in denture fabrication (n=15 per group) | OR group had greater deviation: 0.72 ± 0.13 mm vs DD: 0.45 ± 0.23 mm; 98.9% samples showed increased OVD; two-way ANOVA: significant difference between workflows (p < 0.0001), no significant difference across measurement points; both methods within clinically acceptable limits | Highlights trade-off between accuracy and workflow in CAD-CAM denture fabrication | Applying / Experimental Comparative Study |
“Analyzing”: Analyzing data, comparing diagnostics, identifying correlations, and performing detailed evaluations for accurate assessment.
A growing body of research has progressively refined our understanding of how digital technologies and anatomical relationships can be used to restore facial occlusal vertical dimension (OVD) in prosthodontic rehabilitation—an outcome with clear implications for facial aesthetics and rejuvenation. Proper OVD reestablishment contributes to balanced lower facial proportions, enhances soft tissue support, and reduces the aged, pseudo–Class III appearance. This makes such interventions increasingly relevant not only in dental settings but also in collaborative facial aesthetic planning with plastic surgeons (Table 4).
In 2023, Khan et al conducted a randomized controlled trial with 80 edentulous patients to evaluate the relationship between index finger length (2D) and occlusal vertical dimension (OVD), measured from subnasale to menton (Sn-Me). Participants were divided into control and experimental groups, and satisfaction was assessed one week later using a Visual Analog Scale. A significant positive correlation was observed between finger length and OVD in both genders, with males having longer finger lengths. Notably, 97% of the experimental group reported satisfaction. The study concluded that index finger length is a simple, quick, and reliable method for OVD determination.
That same year, Bhat et al conducted a study on 258 dentate individuals aged 18–30 to assess the correlation between intercondylar distance (ICD) and occlusal vertical dimension (OVD). ICD was measured with Denar reference points and calipers, while OVD was assessed using a Willis gauge. The mean ICD was 133.5 mm and OVD was 55.4 mm. Pearson analysis showed a significant positive correlation (R = 0.619, P < .001). The study concluded OVD can be predicted from ICD with a regression model, aiding edentulous rehabilitation and helping prosthodontists optimize facial proportions.
In 2023, Tian et al conducted an in vitro study to evaluate how mandibular distal extension edentulism affects OVD accuracy using two IOSs: Primescan and Trios 4. They scanned a typodont model with four missing teeth and implants, assessing accuracy with marker-based measurements. Both trueness and precision were significantly influenced by marker position and scanner type (P < 0.001). PS showed superior trueness and precision in most cases. Both IOSs underestimated occlusal dimensions in edentulous areas, highlighting the importance of selecting the correct scanner and protocol for digital restorations. The study provided key clinical insights for selecting scanning technology to ensure accurate OVD reconstruction, especially in complex cases.
In 2024, Srinivasan et al assessed the reliability of facial scanners for OVD measurement, reporting high intra- and inter-operator consistency—an essential validation of digital scanning’s reproducibility for facial dimension analysis. They evaluated the reliability of a face scanner in measuring the vertical dimension of occlusion (OVD) in 20 fully dentate participants. Clinical and digital measurements were compared at maximal intercuspation and at 2, 4, and 6 mm increased OVD. Using 3D mesh-processing software and anatomical landmarks, 120 measurements were analyzed. Strong correlations (r > 0.93, P < 0.001) and excellent intra-class correlation coefficients (ICC) indicated high reliability. Mean differences between methods were minimal (0.054–0.203 mm), and no significant proportional bias was found. The study concluded that face scanning provides a reliable, accurate method for OVD assessment in digital prosthodontics.
El-Sabbagh et al found that high-resolution digital imaging aids in evaluating the 3D maxillary dentition inclination and facial landmarks, which are essential for restoring a youthful facial appearance. Their study of 81 patients used 3D analysis of intraoral and facial scans to compare the maxillary occlusal plane with Camper’s plane and the ala-tragus line. They found that the superior and middle Camper’s planes, as well as the superior ala-tragus line, aligned closely with the occlusal plane, while the Fox plane showed high variability. The findings support digital methods for reliable occlusal plane assessment in restorative dentistry procedures.
In 2024, Skomina et al used stereophotometric 3D photogrammetry to assess facial soft-tissue changes following denture rehabilitation. Their study identified subtle but significant improvements in facial dimensions, directly linked to enhanced VD and denture function. They conducted a survey assessing facial changes in 102 edentulous older adults (>65 years) after complete denture rehabilitation, compared with 30 dentate controls. Using 3D stereophotometric scans, 16 facial parameters and 11 regional changes were analyzed. Dentures improved perioral features, a wider mouth, a longer upper lip, and a more protruding profile. Unexpectedly, fuller cheeks were observed post-rehabilitation, though not directly linked to denture use. Compared to dentate individuals, edentulous faces with dentures appeared shorter, more retruded, and in females, had narrower vermilions and flatter profiles. The study highlights both aesthetic improvements and residual facial deficiencies post-rehabilitation. These findings demonstrated how prosthodontic interventions can impact facial aesthetics in ways that align with the goals commonly pursued in facial plastic surgery.
| Authors | Technology/Method Compared | Objective | Key Findings/Outcomes | Notes | Bloom’s Taxonomy Level and Study Type |
|---|---|---|---|---|---|
| Khan et al, 2023 | Index finger length (2D) vs. occlusal vertical dimension (OVD) | Evaluate correlation between 2D finger length and OVD in edentulous patients | RCT with 80 edentulous patients; there is a significant positive correlation between finger length and OVD in both genders. Males had longer fingers. The experimental group showed 97% satisfaction using the finger length method. Finger length is a simple, quick, reliable way to determine OVD. | RCT; use of Visual Analog Scale for satisfaction; simple anthropometric proxy | Analyzing / Randomized Controlled Trial |
| Bhat et al, 2023 | Intercondylar distance (ICD) vs. occlusal vertical dimension (OVD) | Assess correlation between ICD and OVD in dentate young adults | 258 participants aged 18–30; mean ICD: 133.5 mm, mean OVD: 55.4 mm; Pearson correlation R = 0.619, P < .001; regression model predicts OVD from ICD, aiding edentulous rehabilitation and facial proportion optimization | Observational analytical study with regression model development | Analyzing / Observational Analytical Study |
| Tian et al, 2024 | IOS scanners Primescan (PS) vs Trios 4 for mandibular distal extension | Evaluate accuracy (trueness, precision) of IOS scanners in scanning edentulous areas | In vitro typodont model with implants and 4 missing teeth; trueness and precision significantly influenced by marker position and scanner type (P < 0.001); PS showed superior trueness and precision; both IOSs underestimated occlusal dimensions in edentulous areas; highlights importance of scanner and protocol choice for VD reconstruction | Controlled in vitro design; clinical implications for digital workflow | Analyzing / Experimental Study |
| Srinivasan et al, 2024 | Facial scanner reliability for VDO measurement | Assess intra- and inter-operator reliability of face scanning for OVD in dentate adults | 20 participants; 120 measurements at various OVD increments; strong correlations r > 0.93, p < 0.001; excellent ICC; mean differences 0.054–0.203 mm; no significant proportional bias; confirms reliability and accuracy of face scanning for OVD assessment in prosthodontics | Validates digital scanning reproducibility; clinical relevance for prosthodontic measurements | Analyzing / Reliability Study |
| El-Sabbagh et al, 2024 | 3D digital imaging analysis of maxillary occlusal plane vs reference planes | Assess alignment of occlusal plane with facial planes for 81 patients; 3D analysis showed superior and middle Camper’s planes and superior ala-tragus line closely aligned with occlusal plane; Fox plane showed high variability; supports digital methods for accurate occlusal plane evaluation | Analyzing / Observational Study |
“Evaluating and Creating”: Assessing digital tool accuracy and developing innovative methodologies for improved assessments
Evaluation studies emphasize the importance of accurate vertical dimension OVD assessment in prosthodontic rehab for facial harmony and aesthetics. As the lower face significantly affects age and attractiveness, these insights aid plastic surgeons in restoring youthful proportions (Table 5).
Mosier et al conducted a clinical observational comparison between analog and digital VD measurement methods. In that observational study, they compared rest vertical dimension (RVD) and occlusal vertical dimension (OVD) measurements obtained manually with calipers and digitally using a facial scanner (Face Camera Pro, Bellus3D) in 30 participants. Distances between facial landmarks were measured in both analog and digital formats (OBJ and STL files). Results showed no significant differences between manual and digital measurements, regardless of file format (p > .05). Inter- and intra-operator reliability was high (Cronbach’s alpha, .994–.997). The study concluded that digital facial scanning is as accurate and consistent as conventional methods for measuring vertical dimensions. This improved reliability enables more precise reconstruction of facial height, leading to better soft tissue support and a more youthful appearance, outcomes highly sought after in aesthetic treatment planning.
In 2022, Vinnakota et al conducted a multicenter, randomized trial comparing patient satisfaction with complete dentures made using conventional methods and those made using cephalometric angular reconstruction for occlusal vertical dimension. Participants were randomly assigned, and satisfaction was rated on a scale of 1 to 5. Results showed no significant difference in vertical dimension accuracy (P = 0.465) or satisfaction (P = 0.943). Confounding factors and dentist quality did not affect satisfaction. The study concluded that cephalometric angular reconstruction is as effective as conventional methods for denture fabrication. Using skeletal landmarks in vertical assessment enhances functional restoration and facial esthetics, reducing aging-related facial features.
Strajnić et al compared face anthropometry and digital 2D-face photogrammetry to predict occlusal vertical dimension (OVD) in 90 Serbian adults. They measured 15 craniofacial distances, focusing on Sn-Gn (nose septum to chin tip) using a Boley gauge and digital software (Dr Ceph). The mean Sn-Gn values were almost identical between methods (63.55 mm vs. 63.56 mm). Multivariate regression showed Sn-Gn depended on various facial distances and sex for both methods. The study concluded that digital 2D facial photogrammetry was as reliable as traditional anthropometry for OVD prediction, with no significant differences found. By capturing volumetric data, 3D methods provide a more comprehensive understanding of facial form and symmetry, which are crucial factors in achieving aesthetic results that blend harmoniously with surrounding structures.
A pioneering cross-sectional study by Yialouridou et al examined the influence of age, sex, and dental variables on lower and middle facial aesthetics in 58 Caucasian dentate adults aged 26–79. Using 2D digital photography and intraoral measurements analyzed with ImageJ and SPSS, significant age-related changes were identified: the middle third was more prominent in females, the lower third in males, and pupil-to-orbital distance decreased with age. Dental variables also showed significant correlations with facial features. The findings offer valuable anthropometric data for the Greek population, highlighting the importance of considering age, sex, and dental factors in preoperative planning for dental restorations and facial surgeries.
In a 2025 study, Srinivasan compared the accuracy of two stationary face scanners using progressive capture (Obiscanner) and multi-view simultaneous capture (RAYFace) technologies. Forty dentate volunteers had facial landmarks measured manually with a caliper and digitally via the scanners. Digital measurements were consistently longer than clinical ones (p < 0.001). RAYFace showed greater variability in vertical measurements, while Obiscanner had more variation horizontally (p < 0.05). Inter-examiner reliability was high for digital measurements (ICC ≥ 0.99). The study highlighted the distinct strengths and limitations of each scanner in terms of facial measurement accuracy in prosthodontics.
Overall, these studies show that accurate OVD determination is essential not only for prosthodontic success but also for improving facial aesthetics. Restoring proportional facial height through evidence-based digital workflows enables collaboration, especially with facial aesthetic specialists, to achieve outcomes that are both functional and visually rejuvenating.
| Authors | Technology/Method Compared | Objective | Key Findings/Outcomes | Notes | Bloom’s Taxonomy Level and Study Type |
|---|---|---|---|---|---|
| Mosier et al, 2021 | Analog (calipers) vs digital facial scanner (Face Camera Pro, Bellus3D) | Compare accuracy and reliability of analog and digital VD measurements (RVD and OVD) | 30 participants; no significant differences between manual and digital measurements (p > .05); high inter- and intra-operator reliability (Cronbach’s alpha .994–.997); digital scanning as accurate and consistent as conventional methods; enables precise facial height reconstruction | Observational clinical study; OBJ and STL file formats analyzed; relevant for esthetic treatment planning | Evaluating / Observational Clinical Study |
| Vinnakota et al, 2022 | Conventional denture fabrication vs cephalometric angular reconstruction | Compare patient satisfaction and VD accuracy between conventional and cephalometric methods | Multicenter randomized trial; no significant difference in VD accuracy (P = 0.465) or satisfaction (P = 0.943); satisfaction unaffected by confounders; skeletal landmarks effective for functional and aesthetic restoration, reducing aging facial features | Patient satisfaction rated 1–5 scale; supports skeletal landmark use in denture fabrication | Evaluating / Creating Randomized Controlled Trial |
| Strajnić et al, 2024 | Face anthropometry vs digital 2D facial photogrammetry (Dr Ceph software) | Assess reliability of digital 2D photogrammetry compared to anthropometry | 90 adults; mean Sn-Gn values nearly identical (63.55 mm vs. 63.56 mm); multivariate regression showed Sn-Gn dependent on facial distances and sex; no significant differences found; 3D methods suggested for volumetric understanding of facial symmetry | Evaluating / Observational Comparative Study | |
| Yiallouridou et al, 2023 | 2D digital facial photography & intraoral assessment analyzed with ImageJ and SPSS | Evaluate age, sex, and dental variable impacts on lower and midfacial aesthetic proportions in dentate individuals | 58 adults aged 26–79; significant facial changes across ages; middle third more prominent in females, lower in males; negative correlation between age and pupil–orbital distance; intraoral dental factors significantly related to facial measures | Cross-sectional anthropometric study in Greek population; findings support planning for full-arch restorations and facial aesthetic treatments | Evaluating / Cross-Sectional Observational Study |
3.3 SUMMARY OF THE RESULTS
From the perspective of a plastic surgeon focused on achieving optimal aesthetic outcomes for the aging face, the reviewed literature underscores the growing relevance of digital prosthodontic technologies in facial rejuvenation. Precise reestablishment of vertical dimension (OVD) is essential for restoring balanced lower facial proportions, supporting perioral tissues, and reversing the pseudo–Class III appearance often caused by edentulism and age-related alveolar resorption. Digital intraoral and facial scanning technologies have demonstrated high accuracy, operator reliability, and reproducibility, making them suitable adjuncts to aesthetic facial interventions. Studies using facial scanners and software-based measurements confirm minimal deviations from analog methods, supporting their application in preoperative planning where precise facial proportions are critical. These technologies facilitate the planning of subtle enhancements, such as improved lip posture, nasolabial angle, and lower facial projection.
Anthropometric predictors, such as index finger length and facial measurements (e.g., stomion-to-pogonion, pupil-to-cheilion), offer non-invasive, reproducible estimates of OVD and can support surgical planning without the need for intraoral procedures. These correlations are especially valuable for multidisciplinary teams where dental impressions are impractical or unnecessary in the early stages of facial rejuvenation planning. CAD-CAM technologies and digital workflows further contribute to improved facial outcomes by enabling the precise restoration of lost vertical facial height and occlusal relationships. These techniques result in improved lower facial symmetry, enhanced soft tissue support, and rejuvenated perioral structures. Moreover, digital methods can be customized to optimize aesthetics, avoiding overtreatment and maintaining harmony with natural facial dynamics.
Nevertheless, device selection and workflow customization remain critical, as accuracy can vary significantly across scanners and clinical contexts. For instance, multi-view and progressive capture scanners show different strengths depending on the anatomical area and degree of edentulism. Digital workflows must be tailored to individual patients to ensure accuracy in transferring the occlusal vertical dimension and aligning facial landmarks. Collectively, the evidence suggests that digital prosthodontic methods, when integrated with aesthetic surgical planning, offer a comprehensive strategy for facial rejuvenation. These technologies provide quantifiable and reproducible data that can help achieve natural, youthful appearances with greater efficiency and increased patient satisfaction.
4.0 Discussion
Facial aging is a complex process involving progressive degeneration of the skin, subcutaneous tissues, fat compartments, muscles, and bones. While typical cosmetic procedures, such as facelifts, fillers, and laser treatments, primarily target the skin and surface tissues, they often overlook the more profound structural and occlusal changes that significantly impact facial appearance and function. Mendelson and Wong noted that skeletal remodeling—specifically, maxillary retrusion, mandibular posterior rotation, and alveolar bone loss—is the fundamental framework underlying soft tissue changes. Swift et al supported this view, calling for a shift in how we approach facial aging, understanding it as an inside-out process where changes in hard and deep soft tissue occur before surface signs.
The occlusal vertical dimension (OVD), traditionally viewed as a dental issue, has gained new attention among aesthetic practitioners due to its key role in supporting lower facial height, lip posture, and perioral aesthetics. Coleman et al argued that attempts to rejuvenate facial volume without addressing OVD collapse may lead to incomplete or short-term aesthetic improvements. The digitally guided restoration of OVD provides a structural base for both prosthodontic function and soft tissue balance, especially in the aging lower third of the face.
Recent progress in craniofacial modeling allows clinicians to more precisely and objectively assess OVD in both dentate and edentulous patients. Morata et al developed a cephalometric model based on craniometric landmarks to estimate OVD in the Spanish population. In contrast, Biascamano refined this method for the French population, incorporating factors such as eye–ear distance (EED), sex, and craniofacial type. Their results showed clinically acceptable accuracy, especially when intraoral references are missing.
Likewise, Avila-Vásquez et al and Kim et al compared anthropometric methods to the traditional Knebelman technique and reported similar predictive results, confirming the usefulness of extraoral references in prosthodontic diagnosis. Furthermore, a strong link between nose-to-chin distance and OVD was found, supporting its use as a non-invasive predictor. Also, the nose-to-chin distance was proved as a reliable indicator of OVD, aiding in more straightforward yet effective prosthetic planning.
Other studies have explored the relationship between facial measurements and OVD. Bhat et al found a statistically significant link between intercondylar distance and vertical dimension in dentate individuals, suggesting its use in edentulous rehabilitations. Kaffaf and Şakar emphasized the clinical significance of the stomion-to-pogonion distance, which remains consistent despite changes in soft tissue. Additionally, Jankowska et al and Sadry et al examined nasal morphology and philtral height concerning facial attractiveness and balance, providing benchmarks useful for both prosthodontic and surgical planning.
The impact of aging on facial angularity has also been documented. Schuster demonstrated that the naso-mental and columella-labial angles shift with age, resulting in a decrease in facial projection. Cobah et al employed 3D imaging techniques to investigate changes in nasal width and tip angle across various age groups, highlighting the significance of considering broader facial aging patterns in prosthetic rehabilitation.
Digital technologies have further improved diagnostic capabilities, enabling clinicians to better understand the complexity of craniofacial aging with greater accuracy. Stereophotogrammetry, cone-beam computed tomography (CBCT), and high-resolution surface scanning systems like the RAYFace and Obiscanner provide detailed three-dimensional facial mapping. Srinivasan et al demonstrated the reproducibility of 3D scans in capturing facial morphology and measuring vertical dimension in edentulous populations, with strong inter-operator reliability. However, Strajnić et al warned that accuracy may decrease in patients with significant soft tissue redundancy or facial asymmetry.
Volumetric imaging techniques have expanded clinicians’ ability to assess deep tissue loss and anatomical shifts. Jiang et al and other medical teams focusing on age rejuvenation used CT-based tools to quantify cheek fat depletion and midfacial volume loss, offering a consistent protocol to guide fat grafting or implant-based augmentation. Their results highlighted the usefulness of volumetric diagnostics as supplements to dental and surgical assessments.
The mandible contour significantly impacts facial appearance, shaping the lower facial silhouette. Redefining mandibular contour is essential for facial and neck rejuvenation. Research on facial aging across various age groups and genders remains limited. Hussein et al used artificial intelligence and advanced three-dimensional (3D) analysis to study mandibular aging patterns in both males and females. AI-powered 3D analysis of 280 CT scans (ranging from 20 to 79 years old) revealed subtle yet sex-specific changes in the mandible. The posterior mandibular height decreased in both sexes. Men showed more bone resorption and flattening of the antegonial notch, while women exhibited greater resorption of the symphysis. Both groups experienced increases in bigonial and intercondylar widths at the back. These findings highlighted the importance of skeletal support in facial rejuvenation planning.
Likewise, Zhang et al examined anterior maxillary osteotomy and its effects on both soft tissue advancement and hard tissue repositioning, demonstrating the dynamic interaction between skeletal modifications and aesthetic improvements. Maxillary advancement surgery can impact the aesthetics of the nasolabial region and result in specific changes to the surrounding soft tissues. Understanding these changes is essential to establishing realistic patient expectations and achieving optimal functional and aesthetic outcomes.
Artificial intelligence and statistical modeling have further pushed the frontier of personalized craniofacial assessment. Rames et al employed statistical shape modeling to map mandibular dimorphism across genders, enhancing sex-specific aesthetic planning. Zaheer et al validated semi-automated software tools for facial and musculoskeletal measurements, showing high interrater reproducibility. Nonetheless, advised caution, noting that over-reliance on algorithms may obscure individual variations and cultural norms in aesthetic perception.
The integration of prosthodontics with facial aesthetic surgery marks a shift from fragmented care toward a comprehensive, structural approach to rejuvenation. Strong correlations were found between dental arch shape and facial soft tissue projection, suggesting that dental treatments can influence facial harmony. El-Sabbagh et al also demonstrated that digitally planned prosthetic rehabilitation, particularly OVD correction, significantly enhances aesthetic outcomes in edentulous patients. Both the Camper’s plane and the horizontal reference plane can serve as initial reference points for oral rehabilitation. However, additional anatomical and aesthetic parameters are necessary to confirm an occlusal plane angle that is visually appealing.
Kamalakidis et al revealed a mastication pattern based on wear facets on maxillary first molars in denture wearers, emphasizing neuromuscular adaptation. The latter highlighted the importance of balanced occlusal design in maintaining occlusal vertical dimension (OVD). Strategic occlusal planning, especially in posterior areas, improves chewing and long-term prosthetic stability. Using advanced techniques, such as digital occlusal analysis, in treatment planning benefits functional outcomes and facial preservation, which are crucial for aging patients requiring aesthetic and prosthodontic care.
Although studies vary on the exact number of functional tooth units (FTUs) required, there is consensus, as noted by Naka et al, that chewing efficiency and consequently masticatory muscle volume is strongly influenced by both the number and distribution of remaining teeth. Preserving posterior teeth is essential for maintaining the vertical dimension of occlusion (OVD), which directly supports lower facial height and contributes to a youthful appearance. Strategic prosthetic restoration enhances both oral function and facial aesthetics. These principles should inform and refine predictive formulas, particularly those based on facial anatomical landmarks, to develop more accurate, logarithmic models for estimating the ideal individualized OVD. From a plastic surgeon’s perspective, OVD loss contributes significantly to facial aging. This review highlights how emerging technologies, such as 3D facial scanning and digital occlusal analysis, enable integrative, functional, and aesthetically driven care for aging patients.
Emerging digital technologies, such as 3D facial scanning, intraoral imaging, and anthropometric modeling, may offer precise assessment tools for evaluating dental and facial variables. By integrating these technologies, clinicians can develop targeted interventions that not only restore occlusal support and vertical dimension but also enhance structural facial harmony. Such interdisciplinary approaches are essential for advancing personalized, aesthetic, and functional care in geriatric oral rehabilitation.
Despite the increasing evidence supporting interdisciplinary approaches, their implementation remains limited by disciplinary silos. Collaborative frameworks and shared digital platforms among prosthodontists, oral surgeons, and plastic surgeons are essential for fully realizing these innovations. To support this, Bloom’s Taxonomy has been suggested as a cognitive framework to improve interdisciplinary training and decision-making. Including digital skills within Bloom’s higher order learning levels, allowing clinicians to integrate anatomical data, assess treatment plans, and work together on precise interventions.
5.0 Conclusion
This scoping review highlighted the crucial role of digital technologies in enhancing craniofacial assessment and aesthetic planning for aging populations. By integrating high-resolution, three-dimensional tools such as CBCT, facial scanning, AI-driven morphometrics, and digital intraoral impressions, clinicians can more accurately evaluate occlusal vertical dimension (OVD), skeletal support, and soft tissue dynamics. These technologies facilitate a more precise understanding of age-related facial changes, supporting a shift from superficial rejuvenation techniques to structurally informed, interdisciplinary interventions. The findings advocate deeper collaboration between prosthodontists and plastic surgeons, enhancing both functional and aesthetic outcomes through evidence-based, personalized treatment strategies.
Future research should focus on standardizing digital protocols across disciplines, validating age- and sex-specific normative data, and developing integrated assessment platforms that link facial scanning, dental occlusion, and volumetric analysis. Longitudinal studies examining outcomes of digitally guided OVD restoration and skeletal augmentation in facial rejuvenation are also warranted. Additionally, educational frameworks such as Bloom’s Taxonomy may be expanded to include digital literacy and collaborative competencies, thereby promoting more cohesive clinical training and decision-making. As aging populations continue to grow, these advances will be essential for delivering comprehensive and sustainable facial rehabilitation strategies rooted in precision medicine and digital innovation.
Disclaimer: The authors have no conflicts of interest to declare.
References
1. Swift A, Liew S, Weinkle S, Garcia JK, Silberberg MB. The facial aging process from the “inside out.” Aesthetic surgery journal. 2021;41(10):1107–1119. https://doi.org/10.1093/asj/sjaa339
2. Srinivasan M, Handel S, Bronzino I, Kamnoedboon P, McKenna G, Leles CR. Comparing analog and 3D measurements of vertical dimension in edentulous subjects. Journal of dentistry. 2025;154:105566. https://doi.org/10.1016/j.jdent.2025.105566
3. Yiallouridou I, Sarafidou K, Theocharidou A, Menexes G, Anastassiadou V. Anthropometric vs. dental variables of the ageing face: A clinical study. Applied Sciences. 2023;13(19):10860. https://doi.org/10.3390/app131910860
4. Srinivasan M, Berisha F, Bronzino I, Kamnoedboon P, Leles CR. Reliability of a face scanner in measuring the vertical dimension of occlusion. Journal of dentistry. 2024;146:105016. https://doi.org/10.1016/j.jdent.2024.105016
5. Kim SW, Ko KH, Huh YH, Cho LR, Park CJ. Evaluation of perceptual and anthropometrical facial changes according to increase in vertical dimension of occlusion. Journal of oral rehabilitation. 2025;52(6):833–839. https://doi.org/10.1111/joor.13937
6. Goldstein G, Goodacre C, MacGregor K. Occlusal vertical dimension: Best evidence consensus statement. Journal of prosthodontics: official journal of the American College of Prosthodontists. 2021;30(S1):12–19. https://doi.org/10.1111/jopr.13315
7. Morata C, Pizarro A, Gonzalez H, Frugone-Zambra R. A craniometry-based predictive model to determine occlusal vertical dimension. The Journal of prosthetic dentistry. 2020;123(4):611–617. https://doi.org/10.1016/j.prosdent.2019.05.009
8. Biascamano V, Chuy V, Srinivasan M, Morata C, Naveau A. Development of craniometry-based predictive model to determine occlusal vertical dimension by using the eye-ear distance in a French population. The Journal of prosthetic dentistry. 2025;134(1):207–213. https://doi.org/10.1016/j.prosdent.2023.09.006
9. Iwuchukwu M. Literature review and use of Benjamin Bloom’s taxonomy. Literature Review and Use of Benjamin Bloom’s Taxonomy. 2016;1(2). 2356-5926.
10. Tuma F, Nassar AK. Applying Bloom’s taxonomy in clinical surgery: Practical examples. Annals of medicine and surgery (2012). 2021;69:102656. https://doi.org/10.1016/j.amsu.2021.102656
11. Gibelli D, Dolci C, Cappella A, Sforza C. Reliability of optical devices for three-dimensional facial anatomy description: a systematic review and meta-analysis. International journal of oral and maxillofacial surgery. 2020;49(8):1092–1106. https://doi.org/10.1016/j.ijom.2019.10.019
12. Jacobs R, Salmon B, Codari M, et al. Cone beam computed tomography in implant dentistry: recommendations for clinical use. BMC Oral Health. 2018;18:88. https://doi.org/10.1186/s12903-018-0523-5
13. Schuster AJ, da Rosa Possebon AP, Schinestsck AR, Chagas-Júnior OL, Faot F. Circumferential bone level and bone remodeling in the posterior mandible of edentulous mandibular overdenture wearers: influence of mandibular bone atrophy in a 3-year cohort study. Clinical oral investigations. 2022;26(3):3119–3130. https://doi.org/10.1007/s00784-021-04294-9
14. Bilgin MS, Baytaroğlu EN, Erdem A, Dilber E. A review of computer-aided design/computer-aided manufacture techniques for removable denture fabrication. European journal of dentistry. 2016;10(2):286–291. https://doi.org/10.4103/1305-7456.178304
15. Srivastava G, Padhiary SK, Mohanty N, Molinero-Mourelle P, Chebib N. Accuracy of intraoral scanner for recording completely edentulous arches: a systematic review. Dentistry journal. 2023;11(10):241. https://doi.org/10.3390/dj11100241
16. Kavousinejad S, Dalaie K, Behnaz M, et al. Developing an artificial intelligence-based progressive growing GAN for high-quality facial profile generation and evaluation through Turing test and aesthetic analysis. Sci Rep. 2025;15:26611. https://doi.org/10.1038/s41598-025-11172-x
17. Myers M, Brown MD, Badirli S, et al. Long-term predictive modelling of the craniofacial complex using machine learning on 2D cephalometric radiographs. International dental journal. 2025;75(1):236–247. https://doi.org/10.1016/j.identj.2024.12.023
18. Kim E, Kuroda Y, Soeda Y, Koizumi S, Yamaguchi T. Validation of machine learning models for craniofacial growth prediction. Diagnostics (Basel, Switzerland). 2023;13(21):3369. https://doi.org/10.3390/diagnostics13213369
19. Chou JC, Thompson GA, Aggarwal HA, Bosio JA, Irelan JP. Effect of occlusal vertical dimension on lip positions at smile. The Journal of prosthetic dentistry. 2014;112(3):533–539. https://doi.org/10.1016/j.prosdent.2014.04.009
20. Imani M, Bani Hassan E, Vogrin S, et al. Validation of a semiautomatic image analysis software for the quantification of musculoskeletal tissues. Calcified tissue international. 2022;110(3):294–302. https://doi.org/10.1007/s00223-021-00914-4
21. Kouveliotis G, Tasopoulos T, Karoussis I, Silva NR, Zoidis P. Complete denture digital workflow: Combining basic principles with a CAD-CAM approach. The Journal of prosthetic dentistry. 2022;127(4):550–555. https://doi.org/10.1016/j.prosdent.2020.12.024
22. Sun J, Lin YC, Lee JD, Lee SJ. Effect of increasing occlusal vertical dimension on lower facial form and perceived facial esthetics: A digital evaluation. The Journal of prosthetic dentistry. 2021;126(4):546–552. https://doi.org/10.1016/j.prosdent.2020.07.013
23. Zhou TF, Yang X, Wang RJ, et al. [Title in Chinese]. Beijing da xue xue bao. Yi xue ban = Journal of Peking University. Health sciences. 2023;55(1):101–107. https://doi.org/10.19723/j.issn.1671-167X.2023.01.015
24. Rutkūnas V, Gedrimienė A, Al-Haj Husain N, et al. Effect of additional reference objects on accuracy of five intraoral scanners in partially and completely edentulous jaws: An in vitro study. The Journal of prosthetic dentistry. 2023;130(1):111–118. https://doi.org/10.1016/j.prosdent.2021.09.032
25. Kaffaf MB, Şakar O. Evaluation of various anthropometric measurements for the determination of the occlusal vertical dimension. The Journal of prosthetic dentistry. 2024;132(3):570–577. https://doi.org/10.1016/j.prosdent.2024.07.006
26. Figueras-Alvarez O, Clua-Palau A, Caponi LQ, Vidal-Ponsoda C. Interarch space assessment in edentulous patients rehabilitated with complete removable dentures using open-access software. Journal of dentistry. 2022;123:104127. https://doi.org/10.1016/j.jdent.2022.104127
27. Satin SR, Goodacre BJ, Masri R. Comparing the accuracy of occlusal vertical dimension transfer in CAD-CAM dentures. Journal of prosthodontics: official journal of the American College of Prosthodontists. 2024;33(3):239–245. https://doi.org/10.1111/jopr.13669
28. Khan SA, Raza Kazmi SM, Ahmed S, et al. Correlation of index finger length to vertical dimensions of occlusion for edentulous patients and their satisfaction: a randomized controlled trial. Sci Rep. 2023;13:7414. https://doi.org/10.1038/s41598-023-33722-x
29. Bhat VS, Shetty S, Khizer S. Correlation of intercondylar distance and occlusal vertical dimension in dentate individuals: A clinical study. The Journal of prosthetic dentistry. 2023;129(6):895.e1–895.e6. https://doi.org/10.1016/j.prosdent.2023.01.009
30. Tian J, Jung RE, Han Y, Mei Y, Di P. The impact of mandibular partial edentulous distal extension on virtual occlusal record accuracy when using two different intraoral scanners: An in vitro analysis. Journal of dentistry. 2024;150:105303. https://doi.org/10.1016/j.jdent.2024.105303
31. El-Sabbagh B, Seidel K, Sayahpour B, Güth JF. 3D evaluation of sagittal inclination of the maxillary dentition in relation to facial landmarks: A cohort study. Clinical implant dentistry and related research. 2024;26(5):913–921. https://doi.org/10.1111/cid.13351
32. Skomina Z, Kuhar M, Verdenik M, Ihan Hren N. Stereophotometric facial changes in edentulous older adults after rehabilitation with complete dentures. Gerodontology. 2025;42(1):100–109. https://doi.org/10.1111/ger.12774
33. Mosier M, Barmak BA, Gómez-Polo M, Zandinejad A, Revilla-León M. Digital and analog vertical dimension measurements: A clinical observational study. The International journal of prosthodontics. 2021;34(4): 419–427. https://doi.org/10.11607/ijp.7270
34. Vinnakota DN, Edamadaka N, Reddy PS, Duggineni CR. Comparison of patient satisfaction between complete dentures fabricated using “conventional” and “cephalometric angular reconstruction” vertical dimension procedures: A multicenter randomized clinical trial. Journal of Indian Prosthodontic Society. 2022;22(1):82–91. https://doi.org/10.4103/jips.jips_336_21
35. Strajnić L, Perić M, Živković N, et al. Comparison of Face Anthropometry and Digital 2D-Face Photogrammetry as Methods for Predicting Vertical Dimension of Occlusion. The International journal of prosthodontics. 2024; (3):282–292. https://doi.org/10.11607/ijp.8371
36. Wong CH, Mendelson B. . Changes in the facial skeleton with aging: implications and clinical applications in facial rejuvenation. Aesthetic plastic surgery. 2012;36(4):753–760. https://doi.org/10.1007/s00266-012-9904-3
37. Coleman S, Saboeiro A, Sengelmann R. A comparison of lipoatrophy and aging: volume deficits in the face. Aesthetic plastic surgery. 2009;33(1):14–21. https://doi.org/10.1007/s00266-008-9258-z
38. Avila-Vásquez F, Vergara-Sarmiento P, Crespo-Crespo C. Vertical Dimension of Occlusion: A comparative study between Anthropometric and Knebelman’s craniometric methods. Acta odontologica latinoamericana: AOL. 2021;34(1):43–49. https://doi.org/10.54589/aol.34/1/043
39. Kim SW, Ko KH, Huh YH, Cho LR, Park CJ. Evaluation of Perceptual and Anthropometrical Facial Changes According to Increase in Vertical Dimension of Occlusion. Journal of oral rehabilitation. 2025;52(6): 833–839. https://doi.org/10.1111/joor.13937
40. Alhajj MN, Khalifa N, Amran A. Eye-rima oris distance and its relation to the vertical dimension of occlusion measured by two methods: Anthropometric study in a sample of Yemeni dental students. European journal of dentistry. 2016;10(1):29–33. https://doi.org/10.4103/1305-7456.175689
41. Emam NM. Correlation Between Nose-to-Chin Distance and Other Measurements Used to Determine Occlusal Vertical Dimension. Cureus. 2024;16(5):e60443. https://doi.org/10.7759/cureus.60443
42. Basutkar N, Borham AM, AlGhamdi SA, Alderea EW, AlShammari MM, Sheikh KH. Reliability of anthropological measurements in determining vertical dimension of occlusion in Saudi population: A cross sectional study. The Saudi dental journal. 2021;33(7):568–573. https://doi.org/10.1016/j.sdentj.2020.08.006
43. Jankowska A, Janiszewska-Olszowska J, Grocholewicz K. Nasal Morphology and Its Correlation to Craniofacial Morphology in Lateral Cephalometric Analysis. International journal of environmental research and public health. 2021;18(6):3064. https://doi.org/10.3390/ijerph18063064
44. Sadry S, Eusmanaga E, Kayalar E. Nasal profile changes after orthodontic tooth extraction in Class II, Division 1 malocclusion patients: A retrospective study. Journal of stomatology, oral and maxillofacial surgery. 2024;125(5):101748. https://doi.org/10.1016/j.jormas.2023.101748
45. Çoban G, Yavuz İ, Demirbaş AE. Three-dimensional changes in the location of soft tissue landmarks following bimaxillary orthognathic surgery. Dreidimensionale Veränderungen der Lage von Weichgewebereferenzpunkten nach bimaxillärer orthognatischer Chirurgie. Journal of orofacial orthopedics = Fortschritte der Kieferorthopadie. 2021;82(4):257–265. https://doi.org/10.1007/s00056-021-00279-1
46. Zhang C, Lu T, Wang L, et al. Three-dimensional analysis of hard and soft tissue changes in skeletal class II patients with high mandibular plane angle undergoing surgery. Scientific reports. 2024;14(1):2519. https://doi.org/10.1038/s41598-024-51322-1
47. Choi JW, Lee JY, Oh TS, Kwon SM, Yang SJ, Koh KS. Frontal soft tissue analysis using a 3 dimensional camera following two-jaw rotational orthognathic surgery in skeletal class III patients. Journal of cranio-maxillo-facial surgery. 2014;42(3):220–226. https://doi.org/10.1016/j.jcms.2013.05.004
48. Chen YH, Baan F, Bruggink R, et al. Clockwise versus counterclockwise rotation in bimaxillary surgery: 3D analysis of facial soft tissue outcomes. Oral and maxillofacial surgery. 2024;28(2):693–703. https://doi.org/10.1007/s10006-023-01196-w
49. Jiang M, Shao H, Li Q. Analysis of Anatomy and Age-related Changes in Infraorbital Cheek Using Computed Tomography. Aesthetic plastic surgery. 2024;48:3061–3067. https://doi.org/10.1007/s00266-024-04093-z
50. Jiang M, Shao H, Li Q. A New and Validated Computed Tomography-Based Method for Measurement of Facial Fat Volume. Aesthetic plastic surgery. Published online 2025. https://doi.org/10.1007/s00266-025-04769-0
51. Tower J, Seifert K, Paskhover B. Longitudinal Analysis of Superficial Midfacial Fat Volumes Over a 10-Year Period. Aesthetic plastic surgery. 2018;42(4):995–1001. https://doi.org/10.1007/s00266-018-1134-x
52. Galanin I, Nicu C, Tower JI. Facial Fat Fitness: A New Paradigm to Understand Facial Aging and Aesthetics. Aesthetic plastic surgery. 2021;45(1):151–163. https://doi.org/10.1007/s00266-020-01933-6
53. Hussein SM, Rames JD, Shehab AA, et al. How Does the Mandible Age? Comprehensive Artificial Intelligence-Assisted Shape Analysis in the White Population. Plastic and reconstructive surgery. Global open. 2025;13(4):e6650. https://doi.org/10.1097/GOX.0000000000006650
54. Zhang D, Zhao F, Du L, Jin X. Soft and Hard Tissue Changes and Facial Rejuvenation of Anterior Maxillary Segmental Osteotomy: A Three-Dimensional Cephalometric Study. Aesthetic plastic surgery. 2023;47(1):271–281. https://doi.org/10.1007/s00266-022-03063-7
55. Li K, Chow W, Zhu Z, et al. Comparison of Effects between Total Maxillary Setback Osteotomy and Anterior Maxillary Segmental Osteotomy on Nasolabial Morphology. Plastic and reconstructive surgery. 2023;152(6):1076e–1087e. https://doi.org/10.1097/PRS.0000000000010447
56. Bıçkı T, Tosun E, Meral SE, Tüz HH, Avcı H. Maxillary advancement surgery with vertical component: Impact on the nasolabial aesthetics. Journal of cranio-maxillo-facial surgery : official publication of the European Association for Cranio-Maxillo-Facial Surgery. 2024;52(12):1415–1421. https://doi.org/10.1016/j.jcms.2024.08.011
57. Canbaz B, Yılancı H. Assessment of the Change in the Nasal Septum and Nasal Profile After Le Fort I With Cone Beam Computed Tomography. Annals of plastic surgery. 2024;93(3):331–338. https://doi.org/10.1097/SAP.0000000000004085
58. Rames JD, Hussein SM, Shehab AA, et al. Mandibular Gender Dimorphism: The Utility of Artificial Intelligence and Statistical Shape Modeling in Skeletal Facial Analysis. Aesthetic plastic surgery. 2024;48(21):4272–4279. https://doi.org/10.1007/s00266-024-04300-x
59. Zaheer R, Shafique HZ, Khalid Z, et al. Comparison of semi and fully automated artificial intelligence driven softwares and manual system for cephalometric analysis. BMC medical informatics and decision making. 2024;24(1):271. https://doi.org/10.1186/s12911-024-02664-3
60. Bor S, Ciğerim SÇ, Kotan S. Comparison of AI-assisted cephalometric analysis and orthodontist-performed digital tracing analysis. Progress in orthodontics. 2024;25(1):41. https://doi.org/10.1186/s40510-024-00539-x
61. Newberry I, Cerrati EW, Thomas JR. Facial Plastic Surgery in the Geriatric Population. Otolaryngologic clinics of North America. 2018;51(4):789–802. https://doi.org/10.1016/j.otc.2018.03.013
62. Sadeghi P, Meyers A. Novel Perspectives on the Facial Aging Process. Aesthetic surgery journal. 2022;42(4):NP263–NP264. https://doi.org/10.1093/asj/sjab403
63. Ocak I, Karsli N, Altug AT, Aksu M. Relationship between vertical facial morphology and dental arch measurements in class II malocclusion: a retrospective study. PeerJ. 2023;11:e16031. https://doi.org/10.7717/peerj.16031
64. Wang T, Nie K, Fan Y, et al. Network analysis of three-dimensional hard-soft tissue relationships in the lower 1/3 of the face: skeletal Class I-normodivergent malocclusion versus Class II-hyperdivergent malocclusion. BMC oral health. 2024;24(1):996. https://doi.org/10.1186/s12903-024-04752-2
65. Priest G, Wilson MG. An Evaluation of Benchmarks for Esthetic Orientation of the Occlusal Plane. Journal of prosthodontics : official journal of the American College of Prosthodontists. 2017;26(3):216–223. https://doi.org/10.1111/jopr.12524
66. Frugone-Zambra RE, Silva-Fontana O, Bianchi A, Jimenez-Silva A, Bortolini S. Stable cranial parameters to evaluate the occlusal plane orientation in the frontal plane: a systematic review. Minerva dental and oral science. 2023;72(4):185–194. https://doi.org/10.23736/S2724-6329.22.04659-9
67. Kingrungpetch S, Aunmeungtong W, Khongkhunthian P. The accuracy of anatomic landmarks on the occlusal plane: a comparative study between conventional and 3D image method. BMC oral health. 2024;24(1):1459. https://doi.org/10.1186/s12903-024-05132-6
68. Kamalakidis S, Stratos A, Tortopidis D, Forna N, Anastassiadou V. Investigating masticatory cycle parameters and functional wear characteristics in older removable complete denture wearers: a targeted literature review. Oral. 2025;5(2):34. https://doi.org/10.3390/oral5020034
69. Naka O, Anastassiadou V, Pissiotis A. Association between functional tooth units and chewing ability in older adults: a systematic review. Gerodontology. 2014;31(3):166–177. doi:10.1111/ger.12016
70. Janović A, Miličić B, Antić S, et al. Feasibility of using cross-sectional area of masticatory muscles to predict sarcopenia in healthy aging subjects. Sci Rep. 2024;14:2079. doi:10.1038/s41598-024-51589-4

