Endodontic Microsurgery with Biphasic Calcium Sulfate
Treatment of a Root Cyst of the Maxilla with Endodontic Microsurgery and Grafting Using Biphasic Calcium Sulfate Hardening Cement: A Case Study
Damian Dudek¹,², Oliwia Warmusz², Kurtzman Gregori³, Edyta Reichman-Warmusz²
- Artmedica Outpatient Oral Surgery and Implantology Clinic, Torun, Poland
- Silesian Nanomicroscopy Center, Silesia Lab Med-Research and Implementation Centre, Medical University of Silesia, Katowice, Poland
- Implant Cosmetic Dental Center, Silver Spring, Maryland, USA
OPEN ACCESS
PUBLISHED:30 November 2024
CITATION:Dudek, D., Warmusz, O., et al., 2024. TITLE HERE. Medical Research Archives, [online] 12(11).https://doi.org/10.18103/mra.v12i11.5701
COPYRIGHT: © 2024 European Society of Medicine.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v12i11.5701
ISSN 2375-1924
Abstract
Introduction: Many lesions of endodontic origin require surgical management, often due to the possible diagnosis of odontogenic cysts and tumors in the jaw bones. A root cyst is a benign inflammatory lesion, typically presenting as either a painful or painless, slow-growing, expansile mass that appears well-demarcated with an osteosclerotic shell on radiographic imaging. After treatment, large osseous defects often remain, and the use of a graft to fill the void can accelerate healing and prevent complications from failure to fill by the host tissue.
Case Presentation: A 65-year-old female patient with multiple chronic cardiac conditions underwent endodontic microsurgery and bone grafting to treat a root cyst in the anterior right maxilla. The cyst, which caused damage to both cortical plates, was treated in a single step. A retrograde fill of the apex was performed, followed by grafting with biphasic calcium sulfate (Bond Apatite®) to regenerate the osseous defect.
Clinical Discussion: Histologically, the root cyst consisted of multilayered epithelium and connective tissue containing areas rich in inflammatory cells with some fibrotic fragments. Surgical removal of the cyst, followed by curettage of the surrounding bone and defect grafting, provided predictable healing and satisfactory clinical results. The use of biphasic calcium sulfate allowed for tenting of the surgical area without the need for a membrane, simplifying the procedure and reducing the risk of soft tissue ingrowth during healing. The material gradually converted to host bone over a period of 3 to 6 months.
Conclusion: This case, along with supporting literature, suggests that biphasic calcium sulfate is an effective graft material for repairing osseous defects following the removal of cysts and tumors in the jaw. Its use eliminates the need for resorbable membranes, simplifying procedures and reducing costs without compromising clinical outcomes.
Keywords: apicoectomy, biphasic calcium sulfate, guided bone regeneration, root cyst
Introduction
A significant percentage of patients in oral surgery departments require treatment for odontogenic cysts and benign jaw tumors. These lesions, which are often of various etiologies, frequently require surgical intervention. Among these, the root cyst—a chronic inflammatory condition—accounts for over 60% of odontogenic cysts and over 50% of bone cysts. Benign tumors, while less common, may mimic cysts in their early stages on radiographic imaging. Of reported lesions, 54.6% were radicular cysts, 20.6% were dentigerous cysts, and 11.7% were keratocystic odontogenic tumors. Studies indicate that 92.9% of cystic lesions are odontogenic, emphasizing their endodontic origin.
Surgical management of these cysts can range from conservative to radical approaches. One-step procedures, such as endodontic microsurgery, have become an effective option, thanks to advances in microtools, optical instruments, and modern materials. Ultrasonic devices and new filling materials allow precise preparation and backfilling of resected canals. Additionally, a variety of bone substitutes can be used to augment bone cavities.
Bond Apatite® is a notable biomaterial used in bone surgery. It consists of fine-grained biphasic calcium sulfate and synthetic hydroxyapatite. Packaged in a sterile syringe, it can be activated with saline to form a hardening cement without releasing thermal energy. This material does not require barrier membranes, simplifying procedures and minimizing risks associated with wound exposure.
This case report presents the one-step treatment of a root cyst in the anterior right maxilla using Bond Apatite® for bone regeneration.
Case Report
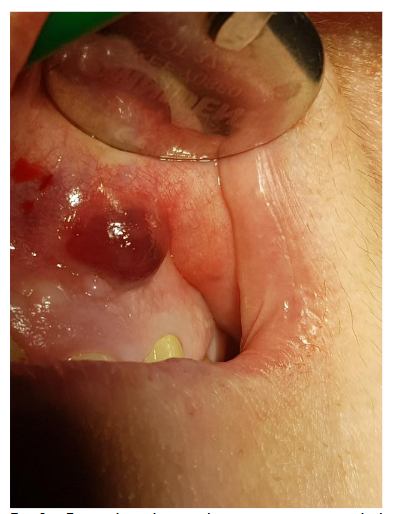
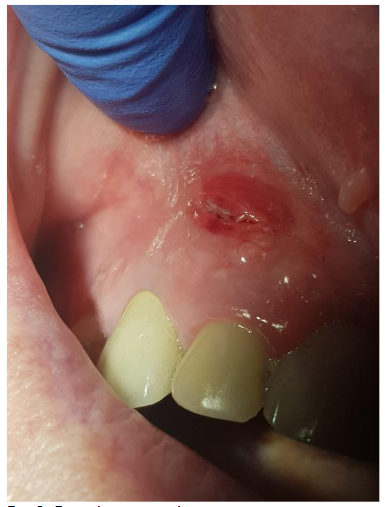
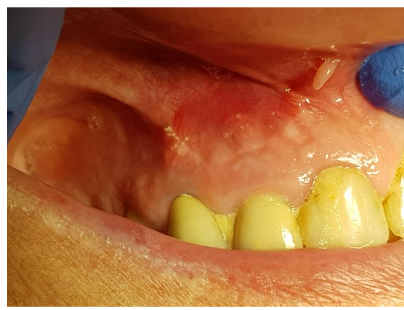
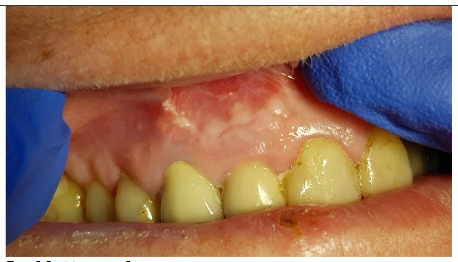
A 65-year-old female patient with multiple medical conditions, including diabetes, a history of heart infarction (treated with PCI), hypertension, atrial fibrillation, and chronic anticoagulant therapy (dihydroxycoumarin and antiplatelet drugs), presented with a root cyst. The lesion appeared four years after successful endodontic and prosthetic treatment. The first clinical symptom was an abscess.
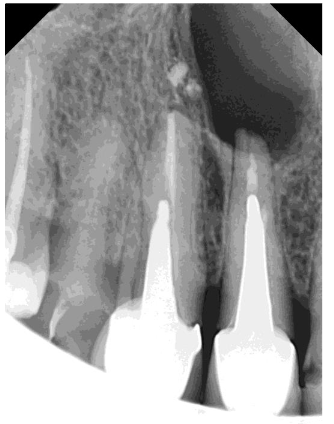
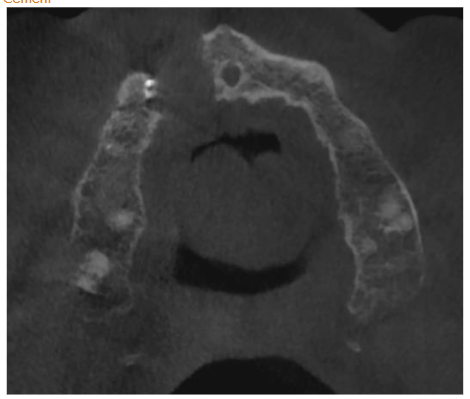
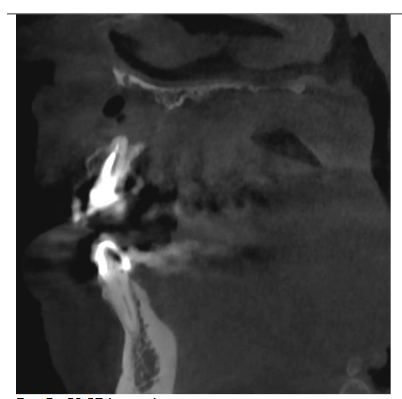
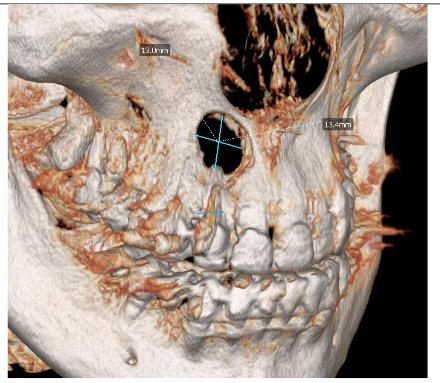
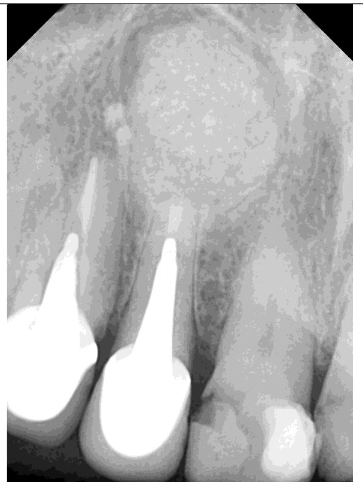
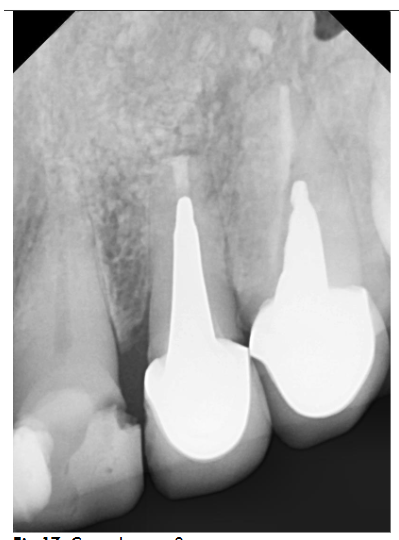
Radiographic examination revealed necrosis around the apex of tooth 12, with CBCT scans showing damage to both the buccal and palatal cortical plates. A decision was made for one-step treatment, and anticoagulant therapy was not interrupted.
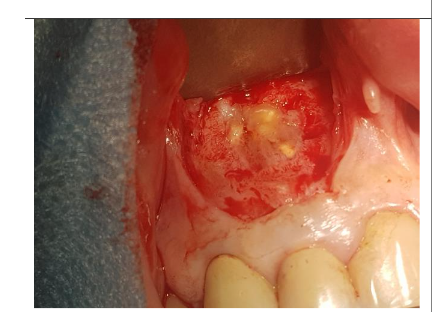
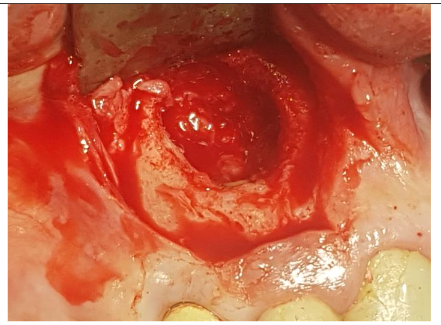
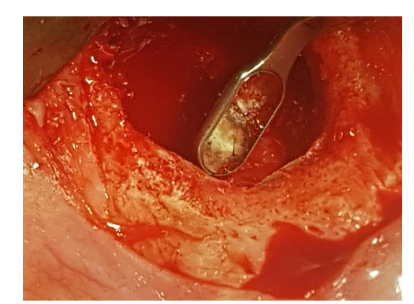
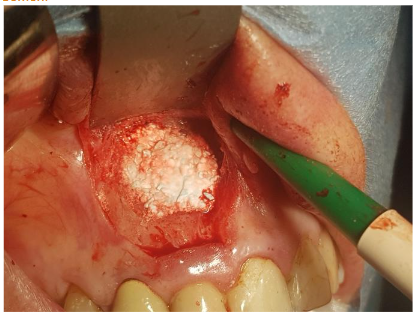
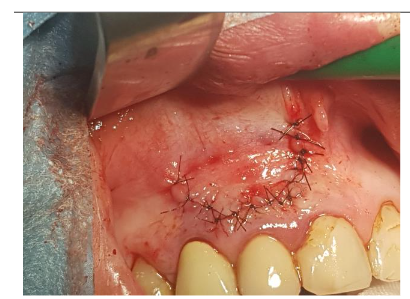
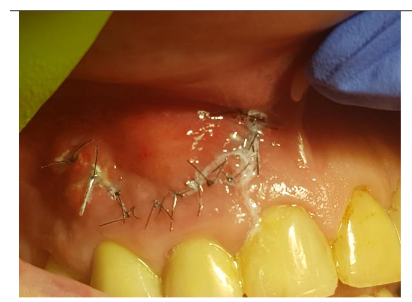
Under local anesthesia (4% articaine with adrenaline), a trapezoidal incision was made, and extensive damage to the external lamina was observed. The cyst was carefully removed and sent for histopathology, which confirmed an inflammatory root cyst. A 3 mm apicoectomy was performed on tooth 12, and the root canal was filled with MTA. The bone defect was filled with 2 cc of Bond Apatite®, and the flap was closed without a membrane.
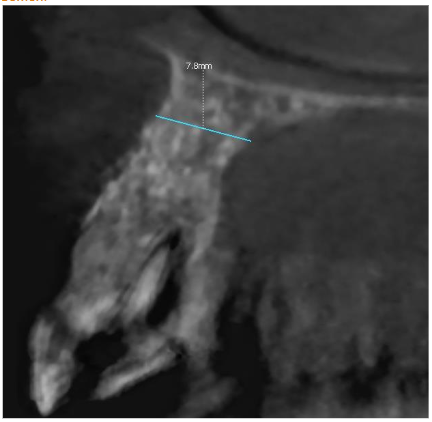
The patient experienced moderate discomfort in the first two days post-surgery. Sutures were removed after seven days, and follow-up radiographs showed satisfactory healing. After six months, CBCT scans revealed significant bone remodeling and regeneration of both cortical plates. No symptoms were reported during a two-year follow-up.
Histological Examination
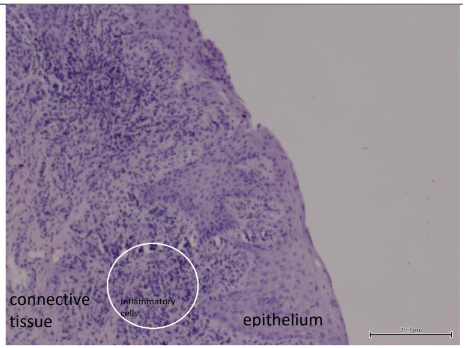
The biopsy, fixed in 10% formalin, was processed using standard histological techniques. Hematoxylin and eosin staining revealed multilayered epithelium and connective tissue with areas rich in inflammatory cells. This histological appearance correlated with the radiographic findings of an inflammatory root cyst.
Discussion
Apical lesions often arise from pulpal issues, and while many resolve after endodontic treatment, larger cysts may require surgical removal. Complete excision of the lesion, combined with grafting, can enhance healing and maintain ridge contours. While grafting may not always be necessary, it can prevent the collapse of buccal ridges and accelerate osseous regeneration.
Various graft materials, including biphasic calcium sulfate, have demonstrated effective conversion to host bone over time. Histological studies have shown that most hydroxyapatite particles are encased in new bone within six months.
Conclusions
This case supports the use of biphasic calcium sulfate (Bond Apatite®) as an effective graft material for treating osseous defects. Its simplicity, cost-effectiveness, and lack of need for resorbable membranes make it a viable option for both practitioners and patients. At six-month follow-up, the material showed high clinical effectiveness and comparable outcomes to other graft materials.
Ethical Approval
This case was treated in a private practice, and the authors are reporting the completed treatment.
Informed Consent
Written informed consent was obtained from the patient for publication of this case report.
Sources of Funding
No funding was received for this study.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Kaczmarzyk T, Stypułkowska J, Tomaszewska R. Torbiele Obszaru Szczękowo-twarzowego. Quintessence. Warsaw, Poland. 2009.
- Morgan PR. Cysts and cystic lesions of the jaws. Current Diagn Pathol 1995; 2: 86-93.
- Brenda L. Nelson, Billy J. Phillips. Benign Fibro-Osseous Lesions of Head and Neck. Head Neck Pathol 2019; 3: 466-475.
- Bertolini F et al. Multiple ossifying fibromas of the jaws: a case report. J Oral Maxillofac Surg 2002; 60: 225-229.
- Y Liu, H Wang, M You, Z Yang, J Miao, K Shimizutani, T Koseki. Ossifying Fibromas of the jaw bone: 20 cases. Dentomaxillofac Radiol 2010; 1: 57-63.
- Pick E, Schäfer T, Al-Haj Husain A, Rupp NJ, Hingsammer L, Valdec S. Clinical, Radiological, and Pathological Diagnosis of Fibro-Osseous Lesions of the Oral and Maxillofacial Region: A Retrospective Study. Diagnostics (Basel) 2022 Feb; 12(2): 238. Published online 2022 Jan 19. doi: 10.3390/diagnostics12020238.
- Azim AA, Albanyan H, Azim KA, et al. The buffalo study: outcome and associated predictors in endodontic microsurgery- a cohort study. Int Endod J 2021;54:301–18.




