Fentanyl’s Neuroscience: Impacts on Crime and Health
A Review on Fentanyl and The Neuroscientific Roots of Criminal Behaviour: Forensic and Legal Reflections
F. Posa¹, A. Porfilio¹, C. Trussardi¹, V. Colmenares Pulido¹, M. Posa¹, V. Vener¹
- NeuroIntelligence, Institute for Ethical Criminological Research, Via Volta 6, 21100 Varese, Italy
OPEN ACCESS
PUBLISHED: 30 November 2025
CITATION: Posa, F. , Porfilio, A., et al., 2025. A Review on Fentanyl and The Neuroscientific Roots of Criminal Behaviour: Forensic and Legal Reflections. Medical Research Archives, [online] 13(11).
https://doi.org/10.18103/mra.v13i11.0000
COPYRIGHT © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i11.0000
ISSN 2375-1924
Abstract
Background: The global diffusion of illicitly manufactured fentanyl represents a critical intersection between neuroscience, law, and public health. Originally developed as a potent analgesic in the XX century, fentanyl’s low production cost, chemical adaptability, and high lethality have enabled its rapid proliferation through transnational criminal networks. While North America remains the epicenter of the crisis, with synthetic opioids accounting for the majority of overdose deaths, recent evidence indicates the gradual expansion of fentanyl and its analogues into Europe, where emerging threats include nitazenes and xylazine-adulterated compounds.
Methods: This study adopts a multidisciplinary approach combining neuroscientific, criminological, and legal perspectives to analyze the roots and repercussions of fentanyl use and distribution. Through a systematic review of biomedical and legal literature, the research outlines the neurobiological mechanisms underlying opioid dependence, particularly the role of craving and impaired reward circuitry involving the mesolimbic dopaminergic system.
Results: These findings reveal structural and functional brain alterations that significantly affect volitional control, thereby challenging the traditional legal assumption of free will as a prerequisite for culpability. Epidemiological data from 2019–2025 demonstrate a continuous rise in fentanyl-related mortality, particularly among adolescents and first-time users exposed to adulterated substances.
Conclusions: Although harm-reduction strategies, such as naloxone distribution, fentanyl test strips, and medication-assisted treatment, have yielded measurable benefits, they remain insufficient to counter the evolving complexity of synthetic opioid markets. Overall, the findings underscore the urgent need to align legal and criminal policy frameworks with neuroscientific evidence, promoting a balanced paradigm that integrates public health, justice, and human rights in addressing the global fentanyl crisis.
Keywords
Fentanyl, opioid dependence, neuroscience, criminal behavior, public health, harm reduction.
Introduction
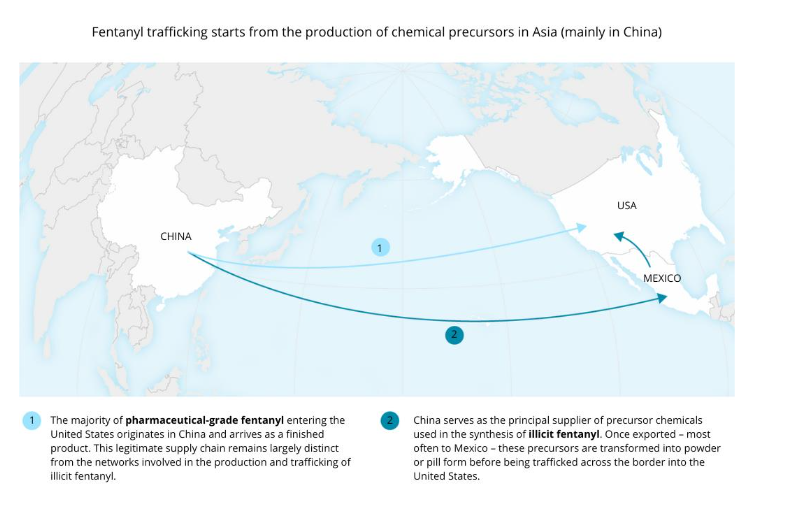
In the last two decades, the spread of Illicitly Manufactured Fentanyl (IMF) and other synthetic opioids has generated one of the most serious health and social crises in the recent history of the United States and North America. Fentanyl and its derivatives are starting to appear in the European drug market as well. 25 kg of fentanyl precursors were confiscated in the Netherlands in December 2024. In Italy, fentanyl smuggling is often associated with stolen medications from public hospitals. With analgesic potency 50 to 100 times greater than that of morphine, fentanyl was initially developed for clinical use in hospital settings, but its extreme effectiveness, ease of synthesis, and low production cost have favored its rapid expansion in the illegal drug market. Starting from the 2010s, fentanyl has progressively supplanted heroin as the main cause of overdose deaths in the United States, contributing to an escalation that exceeded 109,000 deaths in 2023 alone. This phenomenon, commonly defined as the “opioid crisis”, is now configured as a true multifactorial epidemic, in which economic, political, health, and criminal dynamics converge on a global scale. Compared to other substances, fentanyl trafficking exhibits distinctive characteristics: it is based on a fragmented and transnational value chain, which starts from the production of chemical precursors in Asia (mainly in China), continues with synthesis and distribution in Mexico, and concludes with capillary distribution in the United States, and increasingly in Canada as well. Investigations conducted by federal agencies and international organizations highlight how Asian criminal networks and Mexican cartels collaborate steadily, exploiting regulatory gaps and the high market value of the finished product. Artificial Intelligence plays a crucial role in the development of new drugs. It is used not only by Chinese laboratories to design innovative chemical synthesis processes, but also by inexperienced dealers who leverage it to quickly learn the principles necessary for processing substances using legally obtained materials and equipment. This contribution aims to analyze, through a multidisciplinary approach, the origins, trajectories, and implications of the fentanyl phenomenon, with particular attention to geopolitical dynamics, transformations in production and distribution models, as well as impacts on public health and the social fabric. Furthermore, emerging risks for Europe and Italy will be examined, where the phenomenon has so far remained marginal but is potentially expanding. In light of current evidence, strengthening international cooperation and rethinking policies for combating, preventing, and treating synthetic opioid addictions is essential.
THE ROLE OF CRAVING IN DRUG USE
In psychiatric literature, craving is defined as an intense, impulsive, and obsessive desire to consume a substance or engage in a particular behavior to which one is addicted; as defined in the Diagnostic and Statistical Manual of Mental Disorders (5th ed.) “craving (Criterion 4) is manifested by an intense desire or urge for the drug that may occur at any time but is more likely when in an environment where the drug previously was obtained or used.” Craving represents a genuine psychophysical urge that compels individuals to engage in behaviors that are often counterproductive, if not outright harmful to themselves. This multifaceted phenomenon encompasses affective, cognitive, and behavioral dimensions. The affective component involves emotional distress and dysphoria in the absence of the substance, while the cognitive dimension manifests as intrusive thoughts, preoccupation, and attentional bias toward drug-related stimuli. Behaviorally, craving drives persistent drug-seeking activities despite awareness of negative consequences. From a neurobiological perspective, craving involves the dysregulation of reward circuitry, particularly the mesolimbic dopaminergic system, which becomes hypersensitive to drug-associated cues while showing diminished response to natural rewards. Neuroimaging studies have demonstrated that exposure to drug-related stimuli activates the prefrontal cortex, amygdala, and nucleus accumbens, regions implicated in motivation, emotional processing, and reward anticipation. As mentioned by Schembri in the research conducted in 2018, “Chronic exposure to fentanyl results in the downregulation and desensitization of opioid receptors in key brain regions, such as the thalamus and amygdala. Over time, these changes contribute to structural and functional alterations in the white matter of the frontal and temporal lobes, resulting in cognitive and emotional impairments.” The literature distinguishes between reward craving, driven by positive reinforcement expectations; relief craving, motivated by withdrawal symptom alleviation; and cue-induced craving, triggered by environmental contexts associated with previous use. The intensity and persistence of craving episodes represent critical predictors of relapse vulnerability, making craving management a central therapeutic target in addiction treatment.
THE EMERGENCE OF NEW SYNTHETIC OPIOIDS IN EUROPE: FENTANYL AND RELATED SUBSTANCES
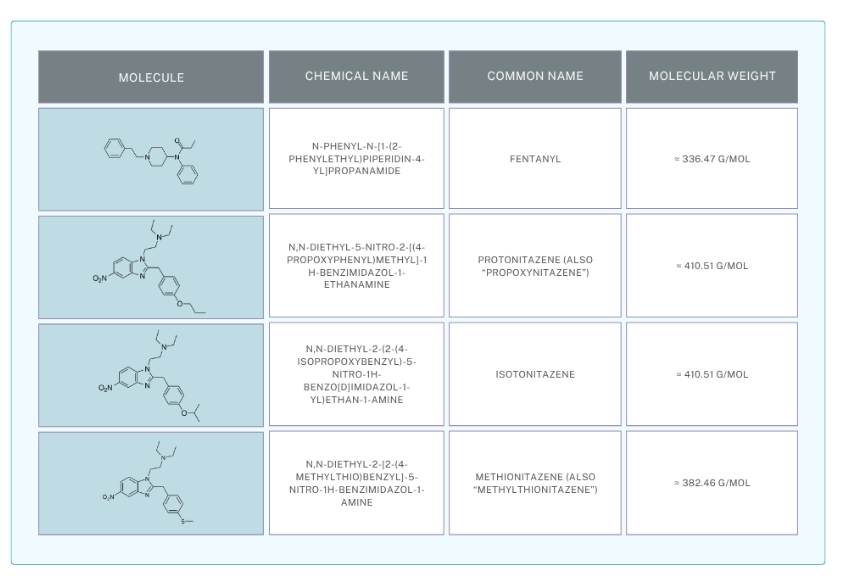
While fentanyl remains the most prominent synthetic opioid associated with overdose deaths in North America, its diffusion in Europe has been more limited and heterogeneous. In several European countries, seizures and toxicological reports indicate sporadic but concerning episodes of fentanyl circulation, often involving diverted medical preparations rather than large-scale illicit production. However, other synthetic opioids, either structurally related or pharmacologically comparable, have begun to appear more frequently across the continent. A key example is nitazenes, a class of highly potent benzimidazole-derived opioids first synthesized in the mid-20th century but recently re-emerging on the illicit drug market. Nitazenes, substances such as isotonitazene, metonitazene, and protonitazene, have been detected in forensic casework and linked to fatal intoxications in countries including Sweden, Germany, and the United Kingdom. Their extreme potency, in some cases exceeding that of fentanyl, raises significant challenges for both public health systems and law enforcement agencies. Alongside these developments, buprenorphine, a semi-synthetic opioid widely prescribed for opioid substitution therapy, has also been subject to diversion and misuse. Although less lethal than fentanyl or nitazenes, non-medical use of buprenorphine has been reported across Scandinavia, France, and Central Europe, sometimes in combination with benzodiazepines or alcohol, thereby increasing overdose risks. It is evident from these trends that Europe’s opioid landscape is shaped not only by the threat of fentanyl but also by the growing availability of alternative cheap synthetic opioids. By 2024, new nitazenes were more commonly reported than new fentanyl analogues by Member States to UNODC and accounted for almost 50 percent of all reported opioid NPS (New Psychoactive Substances). In 2024, the most frequently identified nitazenes in forensic institutes worldwide were protonitazene (38 percent), followed by N-pyrrolidino protonitazene (24 percent), N-desethyl isotonitazene (10 percent) and metonitazene (8 percent).

WHEN VOLITION BECOMES COMPULSION
Opioid use disorder can be partly categorized as a decision-making disorder, among other things. The role of decision-making in fentanyl addiction has been examined thoroughly by several academic studies. Two major, and opposing, theoretical perspectives have emerged: the habit theory and the relative value theory. According to the former, addiction erodes the capacity to exercise one’s free will, while for the supporters of the latter, PWUD (people who use drugs) are still able to choose and exercise their free will, but they disproportionately favor drugs over healthier choices. This mechanism has been explored extensively in a 2023 thesis by T. Shaver. The study investigated whether escalated fentanyl intake alters decision-making processes by contrasting habit theory with relative value theory. Using an allomorphic concurrent choice task in Sprague-Dawley rats, the authors observed that extended (6-hour) access to fentanyl led to clear escalation of intake, while limited (1-hour) access did not. Despite this escalation, choice behavior between drug and food rewards remained stable across groups, and model comparisons indicated that value-based rather than habitual processes best accounted for the observed data. These findings suggest that even under conditions of escalated opioid use, decision-making capacities remain intact, thereby challenging habit theory and supporting the relative value framework. Obviously, these findings have important legal repercussions; given that the capacity to exercise free will remains intact, fentanyl users convicted of a crime would have to face the full consequences of their actions.
NEUROSCIENTIFIC CONSIDERATIONS
The neurobiological impact of fentanyl extends beyond its well-documented effects on pain modulation and reward to include profound cognitive and structural brain alterations. Acute and chronic opioid exposure produces converging patterns of neurotoxicity, neurovascular compromise, and functional dysregulation across cortical and subcortical systems. Acute hippocampal injury following non-fatal overdose has been consistently associated with deficits in episodic and working memory, yet chronic opioid use disorder (OUD) produces a broader constellation of neuropsychological impairments. A comprehensive meta-analysis by Wollman et al. (2019) demonstrated significant reductions in cognitive flexibility, verbal working memory, verbal fluency, decision-making, attention, and processing speed in chronic OUD patients, suggesting widespread disruption of fronto-parietal and limbic networks critical for executive functioning. These deficits parallel findings from imaging studies show altered prefrontal–striatal connectivity and blunted neural responsivity to reward-related cues.
STRUCTURAL AND FUNCTIONAL ALTERATIONS
Evidence of structural compromise has been directly observed in individuals with a history of opioid overdose. An exploratory whole-brain voxel-based morphometry analysis revealed reduced gray matter volume in parietal and temporal regions among individuals with prior non-fatal overdoses. These cortical reductions may reflect hypoxic–ischemic injury following repeated respiratory depression episodes, consistent with the neuropathological profile of opioid toxicity. The parietal and temporal cortices, regions involved in spatial awareness, sensory integration, and episodic recall, are particularly susceptible to hypoxic injury. Functional neuroimaging studies conducted on primates further support dysregulation in reward and salience networks, depending on substance use frequency, genetics, sex, and other factors. Positron emission tomography (PET) studies have identified fentanyl-associated decrease in regional cerebral blood flow (rCBF) within the thalamus and altered metabolic activity in the anterior cingulate cortex and striatum, regions central to arousal, pain regulation, and reinforcement learning. These abnormalities align with the motivational deficits and impaired risk evaluation commonly observed in chronic opioid users.
MECHANISTIC BASIS: BRAIN HYPOXIA AND CELLULAR STRESS
At the physiological level, fentanyl’s potent µ-opioid receptor activation triggers pronounced respiratory depression, reducing cerebral oxygen availability. Experimental work by Solis and colleagues demonstrated a dose-dependent decrease in brain oxygen with ~30-second latency, reaching nadir within 90 seconds and accompanied by parallel declines in glucose metabolism. These hypoxic events were most pronounced in the nucleus accumbens (NAc), a hub of the mesolimbic reward circuit, and the amygdala, both critical to emotional regulation and reinforcement processing. Chronic cycles of hypoxia and hyperglycemia may lead to neuronal oxidative stress, mitochondrial dysfunction, and glial activation, providing a plausible biological substrate for enduring cognitive deficits. Human studies corroborate these physiological mechanisms. Tamargo et al. found that individuals using heroin and fentanyl exhibited marked cognitive impairments across multiple domains, supporting the notion that fentanyl-induced brain hypoxia contributes to lasting neuropsychological dysfunction.
GENETIC SUSCEPTIBILITY AND NEUROPHARMACOGENOMICS
Molecular evidence indicates that interindividual variability in fentanyl neurotoxicity is strongly mediated by genetic polymorphisms influencing receptor sensitivity, metabolism, and transport. As detailed by Barletta et al. (2025), variants in CYP3A4 and CYP3A5 modulate the rate of fentanyl clearance, while the OPRM1 A118G polymorphism affects µ-opioid receptor binding affinity and downstream signaling efficacy. Individuals carrying the GG genotype exhibit decreased receptor sensitivity, potentially requiring higher doses for analgesic efficacy but simultaneously exposing the brain to greater hypoxic and excitotoxic stress. Further, ABCB1 (P-glycoprotein) gene variants alter blood–brain barrier transport efficiency, influencing fentanyl’s central bioavailability, while COMT Val158Met modulates dopaminergic tone and executive control. These genetic factors may partially explain the heterogeneity in cognitive outcomes and vulnerability to addiction observed among fentanyl users.
NEURAL CIRCUITRY AND BEHAVIORAL CORRELATES
Chronic fentanyl use results in functional reorganization across the thalamic–striatal–cingulate circuitry, which governs alertness, reward valuation, and pain perception. Alterations in dopaminergic and glutamatergic transmission within the NAc and prefrontal cortex compromise reinforcement learning and impulse control, favoring habitual over goal-directed behavior. The convergence of neurohypoxia, receptor desensitization, and synaptic remodeling generates a neurobiological milieu conducive to compulsive drug-seeking and cognitive rigidity, hallmarks of advanced OUD. Taken together, neuroscientific data reveal that fentanyl’s neurotoxicity arises from intertwined molecular, vascular, and genetic mechanisms. Acute respiratory depression induces transient yet cumulative hypoxic injuries, while chronic exposure drives receptor downregulation, white matter degradation, and dopaminergic imbalance. The resultant cognitive and emotional disturbances not only perpetuate addiction but also hinder recovery potential. Future neuroimaging and longitudinal studies are warranted to clarify the temporal progression of these alterations and to identify potential neuroprotective strategies.
Methods
A comprehensive literature search was conducted to identify relevant studies on fentanyl. The search strategy employed a systematic exploration of multiple databases to ensure thorough coverage of the available biomedical literature. The primary databases searched included PubMed and Ovid MEDLINE, which were selected for their extensive coverage of peer-reviewed biomedical and clinical research. These databases were queried using a combination of Medical Subject Headings (MeSH) terms and keywords related to fentanyl. The keywords used included, but were not limited to, “fentanyl”, “fentanyl use”, “opioid”, “opioid use disorder”, “crime”, “antisocial behavior”. To supplement the biomedical database search and capture additional grey literature, conference proceedings, and interdisciplinary research, Google Scholar was also utilized as a secondary search engine, using the same list of keywords. This approach enabled the identification of studies that may not be indexed in traditional biomedical databases, thereby enhancing the comprehensiveness of the literature review. The search was limited to articles published in English. No restrictions were placed on publication date to ensure a complete historical perspective on fentanyl research. All database searches were performed between July and October 2025, and duplicate records were removed prior to screening. The search results were systematically screened and evaluated according to predetermined inclusion and exclusion criteria to identify studies relevant to the research objectives of this paper. The study was conducted at the headquarters of NeuroIntelligence – Institute for Ethical Criminological Research, situated in Varese, Italy.
Results
EPIDEMIOLOGICAL AND FORENSIC FINDINGS
The analysis of recent review and modeling studies reveals a complex and evolving landscape of opioid overdose prevention, highlighting both the effectiveness and limitations of current public health strategies. Data collected between 2019 and 2025 indicate an alarming rise in synthetic opioid–related mortality, particularly among adolescents and young adults, and underscore the need for integrated, community-based interventions. According to Calihan et al. (2024), opioid overdose is now the third leading cause of death among adolescents in the United States. Between 2010 and 2021, adolescent overdose deaths increased by 121%, primarily due to the infiltration of fentanyl and its analogues into the illicit drug market. Notably, 65% of adolescents who died between 2019 and 2021 had no prior history of opioid use, and naloxone was administered in only 33% of fatal cases. This evidence suggests that overdose fatalities are no longer confined to chronic opioid users but increasingly affect naïve or experimental users exposed to fentanyl-adulterated substances. Thus, fentanyl can be particularly fatal especially in first-time users. The review identified several barriers limiting youth access to naloxone, including pharmacy restrictions, provider stigma, and insufficient training among pediatricians. Although most pediatricians recognize overdose prevention as part of their clinical responsibility, only 10% report ever prescribing naloxone, and fewer than 15% of pediatric emergency physicians provide it after an opioid-related visit. Such findings point to critical systemic gaps in early intervention and harm reduction for young populations. Recent legislative efforts have begun addressing these deficiencies. In 2024, 36 U.S. states allowed schools or school staff to store and administer naloxone on campus, while a smaller subset mandates its availability in all high schools. Proposed bills such as the School Access to Naloxone Act (2023) and the Helping Educators Respond to Overdoses (HERO) Act aim to expand these initiatives nationally. Preliminary pilot programs, including Safety First and Rx for Addiction and Medication Safety (RAMS), demonstrated improvements in student knowledge, confidence in using naloxone, and understanding of overdose risk factors. However, evidence-based evaluations of their long-term effectiveness remain limited. Zang et al. (2024) conducted a simulation study in Rhode Island using the PROFOUND (Prevention and Rescue of Fentanyl and Other Opioid Overdoses Using Optimized Naloxone Distribution Strategies) model to forecast the effects of opioid settlement–funded naloxone distribution. Their projections estimated that distributing an additional 50,000 naloxone kits per year could reduce annual opioid overdose deaths (OODs) by up to 9% under an optimized demand-based approach. More strikingly, the model predicted that increasing the proportion of witnessed overdoses by 60%, for example, through supervised consumption sites or social-use interventions, could further reduce annual OODs by 37%. When combined, these interventions were projected to achieve a synergistic reduction of over 30% in total fatalities. These findings suggest that while naloxone expansion remains essential, its full potential depends on addressing solitary drug use, a growing contributor to fatal overdoses. Complementary to these trends, recent forensic and toxicological evidence indicates a steady rise in fentanyl-adulterated polysubstance mixtures, often involving xylazine or nitazene analogues. In 2023, 20 different nitazenes were reported by 28 countries to the UNODC Early Warning Advisory on New Psychoactive Substances (NPS), 12 of which are now under international control. Such combinations have been associated with partial or delayed response to naloxone, raising concerns about the limitations of traditional overdose reversal protocols. Preliminary reports from emergency departments across North America show an increasing proportion of overdoses resistant to standard naloxone doses, necessitating repeated administrations or adjunctive respiratory support. Harm-reduction research has also highlighted the growing utility of fentanyl test strips (FTS). In a 2025 multicenter study, Vickers-Smith et al. demonstrated that individuals who received positive FTS results were significantly more likely to engage in overdose risk-reduction behaviors, such as using smaller doses, avoiding solitary use, and keeping naloxone nearby. However, FTS utilization did not significantly reduce the incidence of non-fatal overdoses, suggesting that behavioral changes, though beneficial, require complementary structural interventions. The Network for Public Health Law (2023) further documented similar behavioral adaptations among PWUD including discarding contaminated supplies and using drugs in the presence of others. According to the World Drug Report 2025, opioids continue to represent the most lethal class of substances globally, accounting for over 70% of all overdose deaths in 2023. Fentanyl and its analogues dominate this category, with North America responsible for nearly 84% of fatalities. Notably, poly-substance use involving stimulants or sedatives was present in approximately half of all overdose cases, further reducing the effectiveness of naloxone reversal. In North America, Fentanyl accounts for a large number of drug-related deaths, where 48,422 deaths in the United States of America in 2024 were estimated (data published 13 June 2025) to be related to synthetic opioids (fentanyl). In Canada in 2023, fentanyl was involved in 7,057 deaths, and fentanyl analogues were involved in 3,356 deaths. Nonetheless, in both the United States and Canada, there were initial signs of a decrease in the number of deaths resulting from fentanyl in the second half of 2023 and in 2024. In Mexico, by contrast, fentanyl use has been associated with a significant increase in the number of individuals entering treatment and care for drug use disorders between 2018 and 2023. Global surveillance data also highlight an alarming 500% increase in fentanyl-related mortality among adolescents since 2015, largely attributed to counterfeit pills and non-medical consumption. In parallel, the trafficking of synthetic opioid precursors surged by 80% between 2020 and 2023, underscoring the growing transnational dimension of the crisis. Collectively, these figures contextualize the modeling and clinical data presented by Calihan et al. (2024) and Zang et al. (2024), confirming that while naloxone and harm-reduction programs remain indispensable, they are insufficient to counter the expanding fentanyl supply and evolving patterns of drug consumption. Despite notable progress in policy and community engagement, the evidence suggests that fentanyl-related mortality continues to rise, driven by the diffusion of synthetic analogues, limited bystander presence, and systemic barriers to naloxone accessibility.
LEGAL OUTCOMES
The comparative analysis of national and international legal responses to fentanyl trafficking and misuse reveals persistent reliance on punitive, prohibitionist frameworks with limited deterrent effectiveness. In several jurisdictions, particularly in North America, stricter penalties and “drug-induced homicide” laws have not reduced opioid-related deaths but have instead contributed to systemic inequities, racial disparities in arrests, and elevated post-incarceration overdose risk. Conversely, evidence from harm-reduction and treatment-based initiatives, such as diversion programs and the application of Medication for Opioid Use Disorder (MOUD) in correctional settings, indicates more positive outcomes in terms of rehabilitation and public health protection. In Italy, where large-scale fentanyl trafficking has not yet emerged, legislative action is focused on prevention and monitoring. The inclusion of fentanyl analogues in Table I of controlled substances (Decree of 28 July 2020) and the adoption of the National Prevention Plan Against the Misuse of Fentanyl and Other Synthetic Opioids (2024–2025) mark a strategic effort to strengthen early detection, interinstitutional coordination, and international cooperation.
Discussion
CRIMINOLOGICAL AND LEGAL PERSPECTIVES: INTRODUCTORY CONTEXT
In the international context, the phenomenon of fentanyl consumption and illicit trafficking is situated within a complex framework that presents significant legal and criminological implications. The spread of this substance – highly potent and inexpensive to produce – is sustained by a dense network of illicit trafficking orchestrated by increasingly sophisticated criminal organizations, technologically advanced and capable of adapting to the shifting dynamics of the global market. Within this framework, European ports, now true strategic hubs of international smuggling, constitute a key logistical fulcrum for the clandestine trade of fentanyl and its derivatives. This trade is fueled by dynamic maritime and air routes, as well as by digital tools such as the dark web and drones used for anonymous retail delivery. Faced with such a transnational threat, legislative responses often remain anchored to anachronistic prohibitionist models – heirs to the repressive strategies of North American origin developed between the 19th and 20th centuries – whose limits, in terms of deterrent effectiveness and containment capacity, are widely documented. The adoption of a purely repressive paradigm, moreover, reinforces circuits of systemic violence, intensifying the criminogenic dynamics inherent in illicit drug markets. A shift in approach is therefore necessary: the fight against fentanyl trafficking cannot disregard the implementation of multilevel strategies grounded in international cooperation, the regulation of chemical precursors, particularly in key production areas such as China, India, and Türkiye, and preventive measures aimed at curbing demand in destination countries such as those in Europe. In this regard, the role of supranational bodies such as the United Nations Office on Drugs and Crime (UNODC) and the Commission on Narcotic Drugs could prove crucial in harmonizing both repressive and preventive efforts. At the same time, criminological analysis suggests that the violence connected to synthetic opioid markets is an inevitable by-product of a system removed from any form of legal control. In this sense, the dimension of drug-related violence represents the most visible symptom of an underground ecosystem that thrives precisely because of the illegality of the market itself.
A LOOK AT THE NATIONAL AND INTERNATIONAL LEGAL LANDSCAPE
For scholars and researchers operating in Italy, the analysis of national data has served as a starting point for extending research to the international level. In Italy, fentanyl abuse has become an emerging public concern. Between 2018 and 2023, law enforcement agencies seized quantities of fentanyl powder equivalent to thousands of lethal doses, along with tablets and other formulations. Acknowledging the seriousness of the issue, a decree enacted on 28 July 2020 included structural analogues and derivatives of fentanyl in Table I of controlled and psychotropic substances under Presidential Decree 309/90, specifying their structural characteristics to facilitate identification, prevention, and enforcement efforts. As of October 2025, an update meeting was held at the headquarters of the Italian Government concerning the implementation of the National Prevention Plan Against the Misuse of Fentanyl and Other Synthetic Opioids, initially presented in March 2024. The Plan was designed to implement an integrated and multidisciplinary strategy involving the active cooperation of several ministries and institutions through a coordinated series of actions. From a research and policy standpoint, particular attention has been devoted to criminal policy strategies aimed at prevention and enforcement. Among the activities implemented under the Plan are: the acquisition of data to monitor illicit fentanyl and precursor trade, as well as new opioid adulterants (including xylazine and nitazenes); the engagement of poison control centers and forensic toxicology professionals in training healthcare workers and promoting fentanyl screening; inspections by the Ministry of Health and enforcement actions by the Carabinieri’s NAS units, which have resulted in seizures and precautionary measures across various provinces; prevention campaigns in schools; professional training for law enforcement personnel; and the strengthening of analytical capacities for the identification of synthetic opioids, supported also by international collaboration. International experience underscores the importance of anticipating the problem, particularly since Italy has not yet experienced large-scale fentanyl trafficking, through targeted preventive strategies adaptable to the rapid evolution of the phenomenon. Indeed, at the international level, while the misuse of fentanyl has been documented since its discovery, its abuse has reached alarming proportions due to illegal trafficking and its replacement of traditionally common opioids such as heroin.
In the United States alone, fentanyl-related deaths numbered approximately 70,000 in 2022. Globally, preventive and enforcement measures have become inevitable; however, the proliferation of fentanyl analogues, often capable of evading current regulations due to chemical variability, continues to complicate law enforcement efforts. While numerous studies have analyzed the relationship between criminalization, substance use, and overdose, few have conducted qualitative research to examine the perspectives of communities directly affected by substance use, research that is in fact a necessary precursor for designing interventions and policies aimed at disrupting the cycle of criminal justice involvement among people who use drugs. Beyond the preventive and enforcement measures mentioned above, it is worth recalling the introduction of laws increasing penalties for opioid use and possession, although such criminalization strategies have predictably failed to achieve the desired outcomes. For example, several U.S. states have introduced harsh sanctions for the production and distribution of fentanyl (including the Wisconsin Legislature, 2021), for its transportation across state lines (Kentucky Legislature, 2022), or for supplying fentanyl to individuals who subsequently experience fatal overdoses (Mississippi Legislature, 2022). Similarly, in 2023, the U.S. House of Representatives approved Bill HR 467, which placed all fentanyl-based substances in Schedule I of the Controlled Substances Act, thereby enabling the imposition of harsher criminal penalties. Empirical evidence shows, however, that a predominantly punitive criminal law approach has not led to a reduction in fentanyl use but has instead resulted in increased racial profiling in arrests – disproportionately affecting the African American community – and consequent prison overcrowding. Moreover, incarceration itself has been shown to heighten the risk of overdose upon release, with rates up to 40 times higher than those observed in the general population. Nonetheless, several alternatives to incarceration have demonstrated positive outcomes. For instance, diversion programs and the application of Medication for Opioid Use Disorder (MOUD) in correctional facilities help mitigate, though not completely offset, the rise in mortality and imprisonment rates.
DRUG ADDICTION AND FREE WILL: BETWEEN SCIENCE AND LAW
The debate on free will represents «the most discussed question in all of metaphysics», as Hume aptly maintained. In the field of criminal law, following the well-known opposition between the Classical School and the Positivist School, legal doctrine has progressively converged toward an intermediate position between determinism and indeterminism. This stance acknowledges that, although an absolute freedom of self-determination does not exist, a relative or conditioned form of freedom nonetheless serves the regulatory purposes of criminal law. Law, in fact, does not assume freedom of will as an ontological given, but rather as a practical prerequisite indispensable for social coexistence. Such an approach, however, risks reducing the concept of freedom to a mere legal fiction, detached from any empirical foundation. Given the problematic nature of this issue, legal scholars have frequently questioned the implications of conceiving criminal law as an instrument grounded in a purely hypothetical notion of freedom: an instrument that, in effect, constitutes the mechanism through which society legitimizes the use of coercion. Consequently, within the judicial system, numerous “legal fictions” have been constructed to justify the attribution of culpability and, therefore, the imposition of punishment upon offenders who have, albeit not accidentally, placed themselves in a state of incapacity, such as that resulting from chronic intoxication by narcotic substances. Such a legal model appears entirely anachronistic and misaligned with the scientific and naturalistic frameworks that conceptualize substance abuse as a behavioral disorder. The discussion becomes even more complex when one considers that, from a clinical, symptomatological, anatomopathological, and psychological perspective, there exists a substantial difference between alcohol intoxication and intoxication caused by narcotic substances. As observed by the most authoritative scientific literature, in contrast to alcohol abuse, where the somatic, neurological, and psychiatric pathologies exhibit permanent characteristics and remain readily observable even after cessation of consumption, acute and chronic psychotic disorders resulting from substance abuse are difficult and controversial to classify. These latter conditions, though capable of affecting volitional capacity by diminishing or excluding it, do not necessarily produce permanent and/or irreversible effects, except in particular cases (for instance, those associated with heroin or morphine abuse). It follows that substance addiction does not fall within the normative parameters that allow for the exclusion of criminal responsibility. Such exclusion would apply in cases of chronic intoxication, but, as noted, this is difficult to ascertain, since it is rare to identify the kind of “permanent psychic alterations” necessary to establish it. These normative provisions have been the subject of criticism, particularly concerning their inconsistency with the principle of personal responsibility and with the rehabilitative purpose of punishment.
INTEGRATION OF HABIT THEORY AND RELATIVE VALUE THEORY
The present findings align more closely with relative value theory than with habit theory. Although extended fentanyl access produced clear escalation of intake, choice behavior remained sensitive to changes in magnitude and reward probability. According to habit theory, such prolonged exposure should have yielded rigid, stimulus–response behavior independent of outcome valuation. Instead, rats continued to allocate responding in accordance with relative reinforcement rates, consistent with the predictions of the generalized matching law and supporting the notion that decision-making remained value-based despite escalation. This preservation of value sensitivity parallels prior findings that individuals with opioid use disorder still adjust behavior according to reinforcer magnitude and delay. These results suggest that chronic exposure alters what is valued rather than abolishing valuation altogether, a view we find compatible with the incentive sensitization theory of addiction. Heightened salience of opioid-related cues may amplify the perceived relative value of the drug, driving compulsive use without eliminating goal-directed processes. Recent translational data reinforce this interpretation. Zang et al. (2024) demonstrated that interventions modifying contextual contingencies, such as naloxone distribution and peer presence, significantly reduced overdose mortality, while Calihan et al. (2024) emphasized early reinforcement of non-drug alternatives through education. Together, these studies highlight that even under high levels of drug exposure, choice remains dynamically governed by comparative reward structures. In summary, integrating both theories suggests that fentanyl addiction involves not the replacement of valuation by habit, but a pathological re-weighting of values within an intact decision system. This implies that therapeutic strategies, behavioral, pharmacological, or social, should aim to recalibrate the reward hierarchy rather than merely suppress habitual behavior.
PREVENTION AND POLICY INTEGRATIONS
This rapidly ascending use of fentanyl, or of its associated compounds, leads to the urgent need for preventive measures, which are aimed at reducing risk, incidence of substance use/overdose, or harm. One of the most common preventive measures is the ongoing OEND (Overdose Education Naloxone Distribution) training. This program aims to implement short courses and provide continuous updates on overdose recognition and naloxone use (OEND – Overdose Education and Naloxone Distribution). Additionally, it focuses on educating law enforcement on the risks associated with exposure to even minimal amounts of the substance and establishing protocols for the safe use of naloxone in the community. Another strategy would be to ensure broad and proactive naloxone distribution within law enforcement and emergency response services. Since the decision-making models indicate that targeted increases in naloxone availability can reduce deaths by up to ~9%, with even greater impact in scenarios involving witnessed overdoses, it would be optimal to expand naloxone distribution quantities and channels, ensuring the availability of operational kits across all police forces, emergency posts, and mobile emergency units. Simultaneously, incorporate neurophysiological education modules regarding the action of naloxone and the importance of timely intervention in relation to the duration of cerebral anoxia. Nowadays, the distribution of Fentanyl Test Strips (FTS), with usage training, is one of the most widespread preventive methods. FTS should be provided with practical instructions and harm reduction messages; legislative frameworks should be reviewed and updated to remove barriers to distribution (de-paraphernalization). Nonetheless, FTS use is associated with safer consumption behaviors and reduced overdose risk, while clear regulatory frameworks facilitate broader access and adoption.
Limitations and future directions
Several limitations regarding this work must be acknowledged. The limited inclusion of genetic, sex-based, and environmental variability may underestimate the heterogeneity of fentanyl’s behavioral and neurobiological effects. It is crucial to further assess the difference in fentanyl usage and consequences in various populations. As fentanyl is primarily a major issue in North America only, most research efforts were concentrated in this specific area. Methodologically, the use of value-based decision tasks provides insight into choice behavior but does not encompass the broader motivational and affective components of drug seeking. The absence of direct neural or molecular data also restricts mechanistic interpretation, particularly concerning the modulation of corticostriatal circuits implicated in habit formation. Future research integrating behavioral paradigms with electrophysiological or imaging techniques could help clarify these processes. Additional studies are required on the relation between neural pathways and fentanyl/opioid use. Future studies should also extend beyond fentanyl to include other emerging synthetic opioids such as isotonitazene, metonitazene, and protonitazene, whose pharmacodynamic profiles differ in duration and receptor affinity. Comparative approaches could reveal whether the escalation-induced transition from goal-directed to habitual control generalizes across opioid classes. Translational research combining preclinical evidence with human neuroimaging and behavioral studies will be essential to test the applicability of theoretical models to clinical opioid use disorder (OUD). Finally, at the public health level, the growing presence of ultra-potent opioids underscores the urgency of combining neurobehavioral findings with educational and preventive initiatives. As highlighted by Calihan and colleagues in 2024, implementing school-based overdose education and naloxone distribution (OEND) programs may help mitigate mortality among young populations increasingly exposed to synthetic opioids. Integrating laboratory and population-level research represents a crucial next step toward bridging neuroscience and prevention.
Conclusions
The findings of this review highlight fentanyl as a paradigmatic case in which neuroscientific, forensic, and legal domains converge on a global public health emergency. Evidence from neuroimaging and molecular studies demonstrates that fentanyl induces profound alterations in brain structure and function, including cortical atrophy, disrupted fronto–striatal connectivity, and persistent hypoxic injury. These pathophysiological mechanisms underlie impaired executive control, emotional regulation, and decision-making, yet experimental evidence suggests that volitional capacity is not entirely lost, challenging the deterministic assumptions of habit theory. From a policy standpoint, simulation modeling and epidemiological data confirm that the effectiveness of harm-reduction strategies, such as naloxone distribution and punitive approaches, depends on their integration with interventions addressing solitary use, early education, and community supervision. At the legal and criminological level, current punitive frameworks appear inadequate to contain the complexity of synthetic opioid markets and their neurobehavioral consequences. The evidence supports a paradigm shift toward prevention, and treatment-oriented governance, informed by neuroscientific insights into addiction and decision-making. Aligning criminal policy with empirical knowledge, through the expansion of OEND programs, youth-targeted education, and neuro-informed rehabilitation models, offers a pragmatic path to reducing mortality and recidivism. Ultimately, the fentanyl crisis requires an integrated response that reconciles the principles of justice, ethics, and public health, recognizing addiction as both a neurobiological disorder and a societal responsibility.
Acknowledgements
The authors acknowledge the temporary access to OVID MEDLINE, provided under a one-month trial license, which facilitated part of the literature search.
Conflicts of Interest: The authors have no conflicts of interest to declare.
Funding: None.
References:
- Han Y, Yan W, Zheng Y, Khan MZ, Yuan K, Lu L. The rising crisis of illicit fentanyl use, overdose, and potential therapeutic strategies. Transl Psychiatry. 2019;9(1):282. doi:10.1038/s41398-019-0625-0
- Jobski K, Bantel C, Hoffmann F. Abuse, dependence and withdrawal associated with fentanyl and the role of its (designated) route of administration: an analysis of spontaneous reports from Europe. Eur J Clin Pharmacol. 2023;79(2):257-267. doi:10.1007/s00228-022-03431-x
- Reuters. Dutch seize large shipment of core fentanyl ingredient. https://www.reuters.com/world/europe/dutch-seize-large-shipment-core-fentanyl-ingredient-2024-12-09/. 2024.
- Savona EU, Dugato M, Riccardi M. Theft of Medicines from Hospitals as Organised Retail Crime: The Italian Case. In: Ceccato V, Armitage R, eds. Retail Crime. Springer International Publishing; 2018:325-353. doi:10.1007/978-3-319-73065-3_13
- Stanley TH. The history and development of the fentanyl series. Journal of Pain and Symptom Management. 1992;7(3):S3-S7. doi:10.1016/0885-3924(92)90047-L
- Zhu DT, Cano M. Fentanyl-xylazine overdose deaths in the USA, 2018-2023. Inj Prev. Published online April 2, 2025:ip-2024-045596. doi:10.1136/ip-2024-045596
- Stoecker WV, Bosworth KT, Rottnek F. Missouri’s Fentanyl Problem: The China Connection. Mo Med. 2020;117(4):362-369.
- McDermott J. Mapping and Profiling the Most Threatening Criminal Networks in Latin America and the Caribbean. EL PACCTO 2.0.; 2025. https://elpaccto.eu/wp-content/uploads/2025/02/ENG_Mapping-and-profiling-HRCN_LAC_Vpages.pdf
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-5. 5th edition. American Psychiatric Association; 2013.
- Vafaie N, Kober H. Association of Drug Cues and Craving With Drug Use and Relapse: A Systematic Review and Meta-analysis. JAMA Psychiatry. 2022;79(7):641-650. doi:10.1001/jamapsychiatry.2022.1240
- Kronberg G, Goldstein RZ. An fMRI marker of drug and food craving. Nat Neurosci. 2023;26(2):178-180. doi:10.1038/s41593-022-01246-8
- Barletta C, Di Natale V, Esposito M, et al. The Rise of Fentanyl: Molecular Aspects and Forensic Investigations. IJMS. 2025;26(2):444. doi:10.3390/ijms26020444
- Schembri E. Are Opioids Effective in Relieving Neuropathic Pain? SN Compr Clin Med. 2019;1(1): 30-46. doi:10.1007/s42399-018-0009-4
- Karila L, Marillier M, Chaumette B, Billieux J, Franchitto N, Benyamina A. New synthetic opioids: Part of a new addiction landscape. Neurosci Biobehav Rev. 2019;106:133-140. doi:10.1016/j.neubiorev.2018.06.010
- European Monitoring Centre for Drugs and Drug Addiction. Relazione europea sulla droga 2022: tendenze e sviluppi. Publications Office; 2022. Accessed October 27, 2025. https://data.europa.eu/doi/10.2810/138286
- Pereira JRP, Quintas A, Neng NR. Nitazenes: The Emergence of a Potent Synthetic Opioid Threat. Molecules. 2025;30(19):3890. doi:10.3390/molecules30193890
- Ahmed S, Bhivandkar S, Lonergan BB, Suzuki J. Microinduction of Buprenorphine/Naloxone: A Review of the Literature. Am J Addict. 2021;30(4):305-315. doi:10.1111/ajad.13135
- Håkansson A, Widinghoff C, Abrahamsson T, Gedeon C. Correlates of Nine-Month Retention following Interim Buprenorphine-Naloxone Treatment in Opioid Dependence: A Pilot Study. Journal of Addiction. 2016;2016:1-8. doi:10.1155/2016/6487217
- Crime UNO on D and. World Drug Report 2025 (Set of 3 Booklets). 1st ed. United Nations Research Institute for Social Development; 2025.
- Shaver T. The effects of escalated fentanyl intake on decision-making dynamics. Published online 2023. doi:10.13023/ETD.2023.182
- Hogarth L, Field M. Relative expected value of drugs versus competing rewards underpins vulnerability to and recovery from addiction. Behav Brain Res. 2020;394:112815. doi:10.1016/j.bbr.2020.112815
- Han Y, Cao L, Yuan K, Shi J, Yan W, Lu L. Unique Pharmacology, Brain Dysfunction, and Therapeutic Advancements for Fentanyl Misuse and Abuse. Neurosci Bull. 2022;38(11):1365-1382. doi:10.1007/s12264-022-00872-3
- Kiyatkin EA, Choi S. Brain oxygen responses induced by opioids: focus on heroin, fentanyl, and their adulterants. Front Psychiatry. 2024;15:1354722. doi:10.3389/fpsyt.2024.1354722
- Todaro DR, Volkow ND, Langleben DD, Shi Z, Wiers CE. Collateral Damage: Neurological Correlates of Non-Fatal Overdose in the Era of Fentanyl-Xylazine. J Exp Neurosci. 2024;19:26331055241247156. doi:10.1177/26331055241247156
- Wollman SC, Hauson AO, Hall MG, et al. Neuropsychological functioning in opioid use disorder: A research synthesis and meta-analysis. The American Journal of Drug and Alcohol Abuse. 2019;45(1):11-25. doi:10.1080/00952990.2018.1517262
- Upadhyay J, Maleki N, Potter J, et al. Alterations in brain structure and functional connectivity in prescription opioid-dependent patients. Brain. 2010;133(7):2098-2114. doi:10.1093/brain/awq138
- Dolinak D. Opioid Toxicity. Academic Forensic Pathology. 2017;7(1):19-35. doi:10.23907/2017.003
- Lankhuijzen LM, Ridler T. Opioids, microglia, and temporal lobe epilepsy. Front Neurol. 2024;14:1298489. doi:10.3389/fneur.2023.1298489
- Withey SL, Cao L, de Moura FB, et al. Fentanyl-induced changes in brain activity in awake nonhuman primates at 9.4 Tesla. Brain Imaging Behav. 2022;16(4):1684-1694. doi:10.1007/s11682-022-00639-4
- Adler LJ, Gyulai FE, Diehl DJ, Mintun MA, Winter PM, Firestone LL. Regional brain activity changes associated with fentanyl analgesia elucidated by positron emission tomography. Anesth Analg. 1997;84(1):120-126. doi:10.1097/00000539-199701000-00023
- Comer SD, Cahill CM. Fentanyl: Receptor pharmacology, abuse potential, and implications for treatment. Neurosci Biobehav Rev. 2019;106:49-57. doi:10.1016/j.neubiorev.2018.12.005
- Solis E, Cameron-Burr KT, Shaham Y, Kiyatkin EA. Fentanyl-Induced Brain Hypoxia Triggers Brain Hyperglycemia and Biphasic Changes in Brain Temperature. Neuropsychopharmacol. 2018;43(4): 810-819. doi:10.1038/npp.2017.181
- Tamargo JA, Campa A, Martinez SS, et al. Cognitive Impairment among People Who Use Heroin and Fentanyl: Findings from the Miami Adult Studies on HIV (MASH) Cohort. J Psychoactive Drugs. 2021;53(3):215-223. doi:10.1080/02791072.2020.1850946
- Keady J, Charnigo R, Shaykin JD, et al. Behavioral and genetic markers of susceptibility to escalate fentanyl intake. bioRxiv. Published online January 29, 2025:2024.12.06.627259. doi:10.1101/2024.12.06.627259
- Takashina Y, Naito T, Mino Y, Yagi T, Ohnishi K, Kawakami J. Impact of CYP3A5 and ABCB1 gene polymorphisms on fentanyl pharmacokinetics and clinical responses in cancer patients undergoing conversion to a transdermal system. Drug Metab Pharmacokinet. 2012;27(4):414-421. doi:10.2133/dmpk.dmpk-11-rg-134
- Zhu PF, Wang X, Nie B, et al. A neural circuit from paratenial thalamic nucleus to anterior cingulate cortex for the regulation of opioid-induced hyperalgesia in male rats. Neurobiology of Disease. 2024;203:106745. doi:10.1016/j.nbd.2024.106745
- Fields HL, Margolis EB. Understanding opioid reward. Trends Neurosci. 2015;38(4):217-225. doi:10.1016/j.tins.2015.01.002
- Taylor JL, Samet JH. Opioid Use Disorder. Ann Intern Med. 2022;175(1):ITC1-ITC16. doi:10.7326/AITC202201180
- Wakeman SE. Opioid Use Disorder Diagnosis and Management. NEJM Evid. 2022;1(4):EVIDra2200038. doi:10.1056/EVIDra2200038
- Calihan JB, Carney BL, Schmill DM, Bagley SM. The Call for a School-Based Approach to Opioid Overdose Prevention. Am J Public Health. 2024;114(12):1305-1308. doi:10.2105/AJPH.2024.307849
- Kuehn BM. Fentanyl Drives Startling Increases in Adolescent Overdose Deaths. JAMA. 2023;329(4): 280-281. doi:10.1001/jama.2022.23563
- McKnight C, Weng CA, Reynoso M, Kimball S, Thompson LM, Jarlais DD. Understanding intentionality of fentanyl use and drug overdose risk: Findings from a mixed methods study of people who inject drugs in New York City. International Journal of Drug Policy. 2023;118:104063. doi:10.1016/j.drugpo.2023.104063
- Pilarinos A, Bromberg DJ, Karamouzian M. Access to Medications for Opioid Use Disorder and Associated Factors Among Adolescents and Young Adults: A Systematic Review. JAMA Pediatr. 2022;176(3):304-311. doi:10.1001/jamapediatrics.2021.4606
- Zang X, Skinner A, Krieger MS, et al. Evaluation of Strategies to Enhance Community-Based Naloxone Distribution Supported by an Opioid Settlement. JAMA Netw Open. 2024;7(5):e2413861. doi:10.1001/jamanetworkopen.2024.13861
- Messinger JC, Beletsky L, Kesselheim AS, Barenie RE. Moving Naloxone Over the Counter Is Necessary but Not Sufficient. Ann Intern Med. 2023;176(8):1109-1112. doi:10.7326/M23-0852
- Rife T, Tat C, Jones J, Pennington DL. An initiative to increase opioid overdose education and naloxone distribution for homeless veterans residing in contracted housing facilities. J Am Assoc Nurse Pract. 2021;34(1):188-195. doi:10.1097/JXX.0000000000000577
- Wang N, Ou Y, Wang Y, Huang Z, Hu Y, Zhao S. Xylazine-Adulterated Fentanyl-Induced Brain Toxicity: Mechanism Elucidation via Network Toxicology and Molecular Docking Approaches. J Appl Toxicol. Published online August 23, 2025. doi:10.1002/jat.4902
- Vickers-Smith RA, Gelberg KH, Childerhose JE, et al. Fentanyl Test Strip Use and Overdose Risk Reduction Behaviors Among People Who Use Drugs. JAMA Netw Open. 2025;8(5):e2510077. doi:10.1001/jamanetworkopen.2025.10077
- Fornili KS. International Control Efforts to Curb the Global Production and Trafficking of Fentanyl and Other Synthetic Opioids. J Addict Nurs. 2019;30(1):71-76. doi:10.1097/JAN.0000000000000269
- Liem M, Moeller K. Revisiting Goldstein’s Drugs-Violence Nexus: Expanding the Framework for the Globalized Era. Int Criminol. Published online March 4, 2025. doi:10.1007/s43576-025-00160-w
- Ghose R, Forati AM, Mantsch JR. Impact of the COVID-19 Pandemic on Opioid Overdose Deaths: a Spatiotemporal Analysis. J Urban Health. 2022;99(2):316-327. doi:10.1007/s11524-022-00610-0
- LeMasters K, Nall SK, Jurecka C, et al. Criminal legal penalties, substance use, and overdose: a concept mapping study examining Colorado’s criminal legal penalties. BMC Glob Public Health. 2025;3(1):1. doi:10.1186/s44263-024-00117-7
- Savinkina A, Jurecka C, Gonsalves G, Barocas JA. Mortality, incarceration and cost implications of fentanyl felonization laws: A modeling study. Int J Drug Policy. 2023;121:104175. doi:10.1016/j.drugpo.2023.104175
- Evans EA, Wilson D, Friedmann PD. Recidivism and mortality after in-jail buprenorphine treatment for opioid use disorder. Drug Alcohol Depend. 2022;231:109254. doi:10.1016/j.drugalcdep.2021.109254
- Greco L. Hume on free will. Università degli studi di Sassari. Preprint posted online 2023. doi:10.14275/2465-2334/20230.GRE
- Everitt BJ, Robbins TW. Drug Addiction: Updating Actions to Habits to Compulsions Ten Years On. Annu Rev Psychol. 2016;67(1):23-50. doi:10.1146/annurev-psych-122414-033457
- Baum WM. On two types of deviation from the matching law: bias and undermatching. J Exp Anal Behav. 1974;22(1):231-242. doi:10.1901/jeab.1974.22-231
- Banks ML, Negus SS. Preclinical Determinants of Drug Choice under Concurrent Schedules of Drug Self-Administration. Adv Pharmacol Sci. 2012;2012:281768. doi:10.1155/2012/281768
- Robinson TE, Berridge KC. Review. The incentive sensitization theory of addiction: some current issues. Philos Trans R Soc Lond B Biol Sci. 2008;363(1507):3137-3146. doi:10.1098/rstb.2008.0093
- Razaghizad A, Windle SB, Filion KB, et al. The Effect of Overdose Education and Naloxone Distribution: An Umbrella Review of Systematic Reviews. Am J Public Health. 2021;111(8):e1-e12. doi:10.2105/AJPH.2021.306306
- Ahmed SH, Koob GF. Transition from moderate to excessive drug intake: change in hedonic set point. Science. 1998;282(5387):298-300. doi:10.1126/science.282.5387.298

