First Nations-Led COVID-19 Research Grant Program Insights
Describing a First Nations-led grant program for COVID-19 Research: The APPRISE-Ramsay First Nations COVID-19 grant program
Ms Kristy Crooks (Euahlayi) 1; Dr Miranda Smith 2; Professor Jaquelyne Hughes (Wagadagam) 3; Professor Adrian Miller (Jirrbal) 4
- Menzies School of Health Research, Charles Darwin University, Casuarina, Northern Territory, Australia
- Department of Infectious Diseases, University of Melbourne, at the Peter Doherty Institute for Infection and Immunity, Melbourne, Victoria, 3000, Australia
- College of Medicine and Public Health, Flinders University and Royal Darwin Hospital, Casuarina, Northern Territory, 0811, Australia
- Office of Indigenous Engagement, Centre for Indigenous Health Equity Research, Central Queensland University, Townsville, 4810 Australia
OPEN ACCESS
PUBLISHED: 30 November 2024
CITATION: Crooks, K., Smith, M., et al., 2024. Describing a First Nations-led grant program for COVID-19 Research: The APPRISE-Ramsay First Nations COVID-19 grant program. Medical Research Archives, [online] 12(11). https://doi.org/10.18103/mra.v12i11.5872
COPYRIGHT: © 2024 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v12i11.5872
ISSN 2375-1924
Abstract
We describe the establishment of a First Nations governed grant program that built on an existing Australian research collaboration during the height of the COVID-19 pandemic in 2020. Following a generous philanthropic donation, a process was initiated to centre and privilege First Nations perspectives and governance in the grant dissemination process. Decision-making was driven by First Nations people, including setting research principles and priorities, eligibility and review criteria, and in overseeing the advertising and grant review. This led to a widely distributed and highly competitive application round and the funding of ten grants from diverse organisations addressing various aspects of the COVID-19 response. The resulting grant outputs were diverse and impactful, including academic publications, articles for general readership, internal reports, social and traditional media, and frameworks. The principles from the grant round have underpinned the more recent formation of the ongoing First Nations Research preparednesS neTwork (FIRST), to further embed the important principles of First Nations self-determination for ongoing and future pandemic research.
Keywords
- First Nations
- COVID-19
- grant program
- research
- self-determination
Introduction
The COVID-19 pandemic swept across Australia, as it did across the world, throwing light on inequalities and inequities in health status and access to services. Aboriginal and Torres Strait Islander people across Australia (hereafter respectfully referred to as First Nations people), comprising about 3.8% of the population, braced for impact. Previous pandemics, such as the 2009 H1N1 Influenza pandemic, had hit First Nations people hard. The long legacy of colonisation continues to impact First Nations communities in Australia at every level. This includes in health, with often elevated levels of chronic disease and lower access to preventive health measures such as vaccination. Since the 1970s however, Aboriginal Community Controlled health organisations, including primary care and outreach services, have been built by First Nations communities to provide holistic and culturally appropriate health care. This self-determined, community-centred and community-governed model has transformed primary health care access for First Nations people. This is a result of their trust-building community governance model, focus on the social determinants of health, and the provision of high quality, culturally appropriate healthcare.
The promotion of health equity is particularly critical in pandemic response, since the impacts of co-morbidities, distance and structural racism are amplified during pandemics. With some careful lessons learned from the 2009 H1N1 pandemic, First Nations peoples and the First Nations community-controlled health sector was ready when COVID-19 hit, despite specific omissions from national pandemic preparedness plans. The community-controlled health sector response to COVID-19 in Australia was rapid, adaptive, and hugely successful, with First Nations communities experiencing significantly lower rates of infection and death than the rest of the Australian population, particularly in the first two years.
Working within the adjacent research sector, we sought to develop similar community-controlled principles for pandemic research that would be led by and work with First Nations communities to address COVID-19 specific research questions. The Australian Partnership for Preparedness Research on Infectious disease Emergencies (APPRISE) is a national research collaboration established in 2016 and initially funded by the Australian National Health and Medical Research Council. Centred within Western research institutions, APPRISE had supported the Privileging Aboriginal Voices project as a critical component in pandemic preparedness. This project focused on the adaptation of empowering and deliberative consultative practices to address pandemic-related questions with First Nations communities. A philanthropic donation to APPRISE from the Paul Ramsay Foundation in 2020 provided an opportunity to establish a grant program that put community-controlled principles into action to elevate the leadership of First Nations researchers in the COVID-19 response, and to fund research projects that inform First Nations responses to COVID-19.
Here, we detail the establishment, process, and impact of the grant program and explore the legacy of implementing the principles for ongoing pandemic preparedness.
Establishing the grant program
GOVERNANCE ARRANGEMENTS
Establishing First Nations-led governance arrangements was the first priority for the program. Authors Crooks and Miller, both First Nations people, invited eight other prominent First Nations researchers to join the First Nations COVID-19 Research Council to advise on the research principles, COVID-19 research priorities, principles to guide the grant application and evaluation process, and strategies for maximising the impact of the $AUD2 million donation from the Paul Ramsay Foundation.
A Grant Recommendation Panel was also established, comprising four Research Council members and one non-First Nations member of the APPRISE Executive to provide accountability to the grant-receiving body (APPRISE) and administering institution (The University of Melbourne). The Grant Recommendation Panel oversaw the grant application and advertising process, selected grant reviewers, allocated reviewers to applications and selected grants for funding once the reviews were compiled.
GRANT PRIORITIES AND PRINCIPLES
The First Nations COVID-19 Research Council was rapidly established and met four times in April and early May 2020 to decide the parameters of the grant program. The Research Council agreed on a set of key principles and priorities for the program, including that projects should be led by First Nations researchers; project teams should comprise at least 50% First Nations researchers; enabling applications from a wide range of research settings (not just universities and research institutes); and ensuring applications addressed cultural safety, community governance and engagement and Indigenous data sovereignty. Funding across the preparedness, response and recovery phases were explicitly sought. Flexibility was prioritised too, enabling applications for larger ($AUD250-400k) and smaller ($AUD20-100k) projects; new projects and extensions of existing projects, and projects that addressed a broad range of topics and disciplines.
ADMINISTERING THE GRANT PROGRAM
The grant guidelines and application form were adapted from those previously used for small grants within the broader APPRISE network. Specific sections were added to the application form to ensure the grant principles could be evaluated. This included formal declaration of Aboriginal and/or Torres Strait Islander status for all team members; a cultural safety statement, asking applicants to explain how cultural safety for both communities and study participants would be provided; and a statement on community governance and engagement, asking applicants to address community involvement in study decisions and data collection and how community concerns would be addressed.
The evaluation criteria were also established, with formal criteria to establish eligibility (complete and on-time application led by an Aboriginal and/or Torres Strait Islander researcher) and five weighted criteria for evaluation. These were:
- Demonstration of excellence (including methodological details, project governance, community engagement and data sovereignty) (60%);
- Addressing an unmet need aligning with the identified research priorities (10%);
- Promotion of equity (through a strengths-based approach) (10%);
- Cultural safety (no burden for frontline health staff, partnership approach with community; cultural safety training for non-First Nations researchers) (10%); and
- Feasibility (10%).
The call for applications was distributed widely through existing First Nations networks, assisted by the First Nations COVID-19 Research Council. Applications were open for 5 weeks from 29th June 2020 to 3rd August 2020. Fourteen reviewers were recruited, mostly First Nations researchers (including Council and Grant Recommendation Panel members), with some non-First Nations reviewers selected where their expertise matched the grant applications. All applications were reviewed by two reviewers, at least one of whom was a First Nations researcher. Grant allocations started with applications ranked by review scores, but also considering the other grant program principles and priorities, including how budgets were allocated, the type of organisation the lead applicant belonged to, the seniority of the lead researcher and geographical spread.
SUCCESSES OF THE GRANT PROGRAM
The urgency of the pandemic situation in 2020, combined with a sense of heightened anticipation for its impact on First Nations communities, meant that the Paul Ramsay Foundation donation was a timely and critical opportunity. Its importance was reflected in the generosity with which many First Nations academics were willing to participate in discussion, design and process for the grant program, despite facing great uncertainty and increased workload at the time.
The First Nations COVID-19 Research Council articulated core principles and priorities for grant funding, including the need for a First Nations lead applicant, the requirement for >50% of the research team to be First Nations researchers, encouraging applications from community-controlled organisations, and ensuring that funding, where possible, was directed towards salaries and support for First Nations staff.
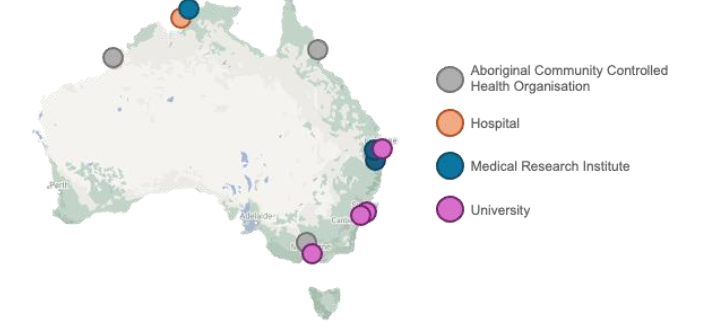
At the close of the 5-week application period, 29 applications had been received from across Australia. As hoped, applications were made by researchers of varied levels of experience and from a variety of settings, including universities, research institutes and community-controlled organisations. Fourteen reviewers were recruited, each reviewing between 2 and 6 grants. Eleven grants were funded, covering a wide geographic spread and diversity of organisation types.
The funded grants covered a range of topics, as outlined in Table 1. One grant was unable to proceed, with the funds returned towards the end of the grant period which enabled us to host a 2-day symposium. The table lists outcomes such as presentations, reports and publications; however, all grants had additional, less quantifiable impacts in documenting and opening new conversations, and in shedding light on issues and concerns of relevance within communities.
After the grants were announced, grant recipients participated in online meetings to share project progress. These meetings also provided an opportunity to learn how others were experiencing the unintended consequences of the public health response to COVID (including movement restrictions, concern for Elders, disruption to services, spread of misinformation etc.). These meetings forged collegiality and shared encouragement which were reflected in the shared knowledge and value of the completed research presented at the symposium in 2023.
Table 1: Completed grants and their outcomes
| Grant Details | Outputs |
|---|---|
| Developing a culturally responsive trauma-informed public health emergency response framework for First Nations families and communities during COVID-19 Professor Catherine Chamberlain; The University of Melbourne |
|
| Preventing COVID transmission by equipping frail dialysis patients with culturally appropriate COVID-safe practices to avoid unplanned hospitalisations in the Top End Professor Jaquelyne Hughes; Ms Onika Paolucci; Top End Renal Service, Menzies School of Health Research & Flinders University |
|
| A culturally-specific overcrowding guideline for COVID-19 pandemic planning, response and recovery in remote Kimberley communities Mr Ray Christophers; Nirrumbuk Aboriginal Corporation |
|
| Aboriginal Community Controlled Health Services and Aboriginal and Torres Strait Islander People’s responses to the COVID-19 Pandemic Dr Margaret Raven, Professor Ilan Katz; University of New South Wales |
|
| TeleHealth use in Cape York Communities- in response to COVID-19 travel restrictions Professor Yvonne Cadet-James; Apunipima Cape York Health Council |
|
| First Nations COVID-19 Pandemic Response: Harnessing the evidence from an urban First Nations health ecosystem to inform ongoing response, recovery and health system adaptation Professor James Ward; University of Queensland |
|
| Using systems thinking to better understand risks and protective factors at play for urban Indigenous peoples during COVID-19 Professor Bronwyn Fredericks; University of Queensland |
|
| Pandemic health messaging for Indigenous peoples during COVID-19 Mr Shea Spierings; University of Queensland |
|
| Revisiting the ‘Gambling Bug’ during COVID isolation: Developing and evaluating a holistic Aboriginal public health awareness strategy to improve service access and wellbeing in a rural and urban Australian setting. Dr Paul Saunders; Western Sydney University |
|
| The experiences of using telehealth in rural and regional Victorian ACCOs during COVID-19: perspectives from health service managers, clinic staff and patients. Mr Dallas Widdicombe; Bendigo & District Aboriginal Co-operative |
|
The grant teams came together for a collegial, uplifting and educational two-day Research Symposium at the beginning of March 2023. Day 1 of the symposium featured presentations from the grant teams, highlighting the strengths of the First Nations-led principles that underpinned the program overall. Additionally, the diverse research questions that were addressed and the different methods and approaches taken provided a rich opportunity for learning and reflection.
The symposium not only provided an opportunity for First Nations researchers to network, but also enabled discussion of how the momentum created through the grant program could be captured for the future. Day 2 included a facilitated discussion on the principles of pandemic research with First Nations communities and desirable features for an ongoing network on First Nations pandemic research preparedness. Reflections from discussions about the possibility of an ongoing First Nations pandemic research network was captured by a graphic recorder.

In late 2023, APPRISE launched the First Nations Research preparednesS neTwork (FIRST) to put the principles learnt and articulated through the grant program into action. FIRST has a Governance Group of eleven First Nations people, and seeks to continue the culture of enabling culturally appropriate, safe and inclusive research for pandemic issues.
Reflections and discussion
The First Nations-led and governed grant program established during the COVID-19 pandemic is a demonstration of what is possible when First Nations perspectives and priorities are centred and privileged in research funding processes. Embedding a process whereby the entire grant program from advertising, reviewing, and selection, was driven by First Nations governance, principles and priorities, successfully demonstrates that First Nations leadership can lead to culturally appropriate, meaningful and impactful research outcomes.
All projects were led by First Nations researchers from academic and community-led organisations, with diverse project focuses and outcomes. The funded projects covered a diverse range of issues relating to COVID-19, from telehealth to culturally informed, appropriate and responsive pandemic frameworks. The diversity of research topics explored highlights the flexibility of the grant program to support and address community-driven needs and priorities.
Good governance underpinned by First Nations perspectives was fundamental in the program’s success. The program structure centred respectful and meaningful engagement processes which enabled the development of principles that could inspire future similar research funding efforts.
While there are challenges in finding suitable reviewers in academic publishing generally, the review of projects for this grant program was done with an excellent, engaged group of First Nations and non-First Nations reviewers with relevant experience who appreciated the importance of the opportunity. Transparency was an important part of the governance to ensure that application review was shared, and the burden did not rely on a few individuals. This was particularly relevant given the increased demand of First Nations peoples during the COVID-19 pandemic and for those working directly in public health and pandemic response.
The entire grant process embedded First Nations priorities and values from start to end. The requirement for all projects to be led by First Nations peoples and for at least 50% of the research team to be First Nations, encouraged a broader definition of who could be considered a ‘researcher’. This included not just academics within research institutions, but also community health workers and health practitioners from community-based organisations. This priority enabled on-the-ground and connected community health workers and practitioners to participate in and contribute to research, which was reflected on with pride at the research symposium. There was a sense, tangible at the symposium, that while all grantees were competing with COVID, they were collaborating with, supporting and celebrating each other.
The grant program revealed a broad range of activity led by Aboriginal and Torres Strait Islander people across Australia focussed on preparedness and response. The scheme was highly time responsive, with the first funding contracts signed within 6 weeks of the application deadline. The symposium event in March 2023 enabled a reflection on what was learned, promoting preparedness for the next pandemic. The full extent of impact of the program is still emerging as additional research outputs are forthcoming.
The principles outlined in this grant program could be applied in additional contexts. The model of First Nations governance, prioritising First Nations leadership and privileging community engagement and data sovereignty, as well as ensuring grant flexibility, could be adapted in other settings where trusted relationships, adequate resources and motivation coincide.
Conclusions
This First Nations-led grant initiative highlights the impactful and community focused outcomes that are possible when First Nations peoples are enabled, trusted and resourced to direct research. As public health emergencies, including pandemics, continue to emerge, it is important to continue to invest in and prioritise these culturally appropriate governance structures with grant funding programs. Privileging First Nations ways of being and doing in both research and grant distribution approaches provides a strong and genuine, empowered base for future infectious disease challenges.
Conflicts of Interest Statement
The authors have no conflicts of interest to declare.
Funding Statement
This work was made possible by a donation from the Paul Ramsay Foundation to the Australian Partnership for Preparedness Research on Infectious disease Emergencies (APPRISE), a Centre of Research Excellence funded by the Australian National Health and Medical Research Council (NHMRC), Application ID1116530. JH was supported by an NHMRC Fellowship (GNT1174758).
Acknowledgments
We gratefully acknowledge the expertise and generosity of the First Nations researchers who joined the First Nations COVID-19 Research Council in addition to authors Crooks, Hughes and Miller. These were (in alphabetical order): Professor Alex Brown, Professor Sandra Eades, Ms Charlee Law, Dr Simon Graham, Mr Mark Mayo and Professor James Ward.
We also acknowledge the support and advocacy of the APPRISE Executive in securing the grant, enabling the First Nations Council and supporting the decisions of the Grant Recommendation Panel – Professor Ross Andrews, Professor Sharon Lewin, Professor Jodie McVernon and Professor Tania Sorrell.
Finally, we pay respects to the grantees and their teams who conducted research on the unceded lands of First Nations communities within Australia.
References
References
1. Australian Bureau of Statistics. Estimates and Projections, Aboriginal and Torres Strait Islander Australians. Accessed 12 September, 2024. https://www.abs.gov.au/statistics/people/aboriginal-and-torres-strait-islander-peoples/estimates-and-projections-aboriginal-and-torres-strait-islander-australians/2011-2031
2. Flint SM, Davis JS, Su JY, et al. Disproportionate impact of pandemic (H1N1) 2009 influenza on Indigenous people in the Top End of Australia’s Northern Territory. Med J Aust. May 17 2010;192(10):617-22. Doi:https://doi.org/10.5694/j.1326-5377.2010.tb03654.x
3. Rudge S, Massey PD. Responding to pandemic (H1N1) 2009 influenza in Aboriginal communities in NSW through collaboration between NSW Health and the Aboriginal community-controlled health sector. NSW Public Health Bull. 2010;21(2) Doi:https://dx.doi.org/10.1071/NB09040
4. Gall A, Law C, Massey P, Crooks K, Andrews R, Field E. Outcomes Reported for Australian First Nation Populations for the Influenza A(H1N1) 2009 Pandemic and Lessons for Future Infectious Disease Emergencies: a Systematic Review. Global Biosecurity. 07/10 2020;2(1) Doi:https://doi.org/10.31646/gbio.76
5. Thurber KA, Barrett EM, Agostino J, et al. Risk of severe illness from COVID‐19 among Aboriginal and Torres Strait Islander adults: the construct of ‘vulnerable populations’ obscures the root causes of health inequities. Australian and New Zealand Journal of Public Health. 2021/12/01/ 2021;45(6):658-663.
Doi:https://doi.org/10.1111/1753-6405.13172
6. Yashadhana A, Pollard-Wharton N, Zwi AB, Biles B. Indigenous Australians at increased risk of COVID-19 due to existing health and socioeconomic inequities. The Lancet Regional Health – Western Pacific. 2020;1 Doi:https://doi.org/10.1016/j.lanwpc.2020.100007
7. Pearson O, Schwartzkopff K, Dawson A, et al. Aboriginal community controlled health organisations address health equity through action on the social determinants of health of Aboriginal and Torres Strait Islander peoples in Australia. BMC Public Health. Dec 4 2020;20(1):1859. Doi:https://doi.org/10.1186/s12889-020-09943-4
8. Weightman M. The role of Aboriginal Community Controlled Health Services in Indigenous Health. Australian Medical Student Journal. 2013;4(1):49-52.
9. Trauer JM, Laurie KL, McDonnell J, Kelso A, Markey PG. Differential effects of pandemic (H1N1) 2009 on remote and indigenous groups, Northern Territory, Australia, 2009. Emerg Infect Dis. Sep 2011;17(9):1615-23. Doi:https://doi.org/10.3201/eid1709.101196
10. Miller A, Durrheim AD, Aboriginal and Torres Strait Islander Community Influenza Study Group. Aboriginal and Torres Strait Islander communities forgotten in new Australian National Action Plan for Human Influenza Pandemic: “Ask us, listen to us, share with us”. Med J Aust. Sep 20 2010;193(6):316-7. Doi: https://doi.org/10.5694/j.1326-5377.2010.tb03939.x
11. Crooks K, Casey D, Ward JS. First Nations peoples leading the way in COVID-19 pandemic planning, response and management. Med J Aust. Aug 2020;213(4):151-152 e1. Doi:https://doi.org/10.5694/mja2.50704
12. Stanley F, Langton M, Ward J, McAullay D, Eades S. Australian First Nations response to the pandemic: A dramatic reversal of the ‘gap’. Journal of Paediatrics and Child Health. 2021/12/01 2021;57(12):1853-1856. Doi: https://doi.org/10.1111/jpc.15701
13. The Australian Partnership for Preparedness Research on Infectious Disease Emergencies. Privileging Aboriginal voices in infectious disease emergencies. Accessed 12 September, 2024. https://www.apprise.org.au/project/privileging-aboriginal-voices-in-infectious-disease-emergencies/
14. Crooks K, Massey PD, Taylor K, Miller A, Campbell S, Andrews R. Planning for and responding to pandemic influenza emergencies: it’s time to listen to, prioritize and privilege Aboriginal perspectives. Western Pac Surveill Response J. Winter 2018;9(5 Suppl 1):5-7. Doi: https://doi.org/10.5365/wpsar.2018.9.5.005
15. Crooks K, Taylor K, Law C, Campbell S, Miller A. Engage, understand, listen and act: evaluation of Community Panels to privilege First Nations voices in pandemic planning and response in Australia. BMJ Glob Health. Aug 2022;7(8) Doi:https://doi.org/10.1136/bmjgh-2022-009114
16. Crooks K, Taylor K, Burns K, et al. Having a real say: findings from first nations community panels on pandemic influenza vaccine distribution. BMC Public Health. Nov 30 2023;23(1):2377. Doi:https://doi.org/10.1186/s12889-023-17262-7
17. Chamberlain C, Heris CL. Developing a culturally responsive trauma-informed public health emergency response framework for First Nations families and communities during COVID-19. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
18. Heris CL, Kennedy M, Graham S, et al. Key features of a trauma-informed public health emergency approach: A rapid review. Front Public Health. 2022;10:1006513. Doi:https://doi.org/10.3389/fpubh.2022.1006513
19. Graham S, Kamitsis I, Kennedy M, et al. A Culturally Responsive Trauma-Informed Public Health Emergency Framework for Aboriginal and Torres Strait Islander Communities in Australia, Developed during COVID-19. International Journal of Environmental Research and Public Health. 2022;19(23). Doi:https://doi.org/10.3390/ijerph192315626
20. Kennedy M, Bright T, Graham S, et al. “You Can’t Replace That Feeling of Connection to Culture and Country”: Aboriginal and Torres Strait Islander Parents’ Experiences of the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2022;19(24). Doi: https://doi.org/10.3390/ijerph192416724
21. Heris CL, Chamberlain C, Woods C, et al. 10 Ways we can better respond to the pandemic in a trauma-informed way. The Conversation. 2021. https://theconversation.com/10-ways-we-can-better-respond-to-the-pandemic-in-a-trauma-informed-way-168486
22. Kamitsis I, Jones KA, Bright T, et al. Developing a culturally responsive traumainformed public health emergency response framework for First Nations families and communities during COVID-19: Workshop Report. 2021. https://mspgh.unimelb.edu.au/__data/assets/pdf_file/0003/4084185/APPRISE-Workshop-Report-20220315.pdf
23. Chamberlain C, Bright T. “You Can’t Replace That Feeling of Connection to Culture and Country” Aboriginal and Torres Strait Islander Parents’ Experiences of the COVID-19 Pandemic. Presented at: Population Health Congress; 2022; Adelaide, South Australia, Australia.
24. Atkinson C. In the Eye of the Storm: Community-led Indigenous informed responses during a natural disaster. Accessed 12 September, 2024. https://mspgh.unimelb.edu.au/centres-institutes/onemda/research-group/indigenous-health-equity-unit/research/apprise-grant/activities/northern-rivers-community-healing-hub
25. Modderman R, Hughes JT. Live Strong, COVID-Safe and Frailty Free after starting dialysis: an Aboriginal and Torres Strait Islander renal care perspective. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
26. Modderman R, Paolucci O, Zabeen S, et al. Physiotherapy-led restorative care enabling improved frailty measures in adults after starting dialysis in Northern Territory of Australia: The ‘Frailty-to-Fit’ pilot study. The Lowitja Journal. 2024/01/01/ 2024;2:100020. Doi:https://doi.org/10.1016/j.fnhli.2024.100020
27. Zabeen S, Eades A-M, Paolucci O, et al. Evaluation of an innovative Live Strong COVID-mitigating healthcare delivery for adults after starting dialysis in the Northern Territory: A qualitative study. The Lowitja Journal. 2023/01/01/ 2023;1:100001. Doi:https://doi.org/10.1016/j.fnhli.2023.100001
28. Adams F. New Bus for Renal Patients. NT News. Accessed 12 September 2024. https://www.menzies.edu.au/icms_docs/325957_New_bus_for_renal_patients.jpg
29. Hughes JT. Transition Models of Care for Adults Starting Dialysis. Presented at: Renal Society of Australasia Annual Conference; 2022; Darwin, Northern Territory, Australia.
30. Modderman R. Informing the Evidence-Practice Gap About Frailty Support for Aboriginal and Torres Strait Islander People with End Stage Kidney Disease: The ‘Frailty to Fit’ Pilot Study. Presented at: Australian New Zealand Society of Nephrology Annual Scientific Meeting; 2022; Sydney, NSW, Australia.
31. Modderman R. Informing the Evidence-Practice Gap about Fraility Detection Measures Among Adult Aboriginal and Torres Strait Islander People with Advanced Kidney Disease: The Live Strong, COVID-Safe, Frailty Free After Starting Dialysis Project. Presented at: Australian New Zealand Society of Nephrology Annual Scientific Meeting; 2021; Online.
32. Poelina R, Hoy C, Clements C. A culturally-specific overcrowding guideline for COVID-19 pandemic planning, response and recovery in remote Kimberley communities. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
33. Clements C, Hoy C, Bin-Maarus L, Morris S, Christophers R. Aboriginal peoples’ lived experience of household overcrowding in the Kimberley and implications for research reciprocity in COVID-19 recovery. Aust N Z J Public Health. 2023;47(6) Doi: https://doi.org/10.1016/j.anzjph.2023.100104
34. Hoy C, Clements C, Christophers R. Principles of Engaging with Community. Presented at: Kimberley Aboriginal Health Research Alliance Forum; 2022; Broome, Western Australia, Australia.
35. Morris S, Christophers R. Aboriginal Environmental Health Conference; 2021; Perth, Western Australia, Australia
36. Clements C, Ward J. Learning more about people’s experiences of overcrowding in the Kimberley. Presented at: 13th National Aboriginal and Torres Strait Islander Environmental Health Conference; 2022; Darwin, Northern Territory, Australia.
37. Ward J. Aboriginal-led development of a culturally-specific overcrowding guideline for COVID19 planning. Presented at: Preventive Health Conference; 2021; Perth, Western Australia, Australia.
38. Raven M, Jopson W, Katz I. Aboriginal Community Controlled Health Services and Aboriginal and Torres Strait Islander People’s responses to the COVID-19 Pandemic. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
39. Cadet-James Y. Telehealth Use in Cape York Communities in response to COVID-19 travel restrictions. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
40. Pascua K. First Nations COVID-19 Pandemic Response: Harnessing the evidence from an urban First Nations health ecosystem to inform ongoing response, recovery and health system adaptation. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
41. Fredericks B, McAvoy S. Using systems thinking to better understand risks and protective factors at play for urban Indigenous peoples during COVID-19. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
42. Fredericks B, Bradfield A, Ward J, et al. ‘We know what our communities need’: What the Indigenous health sector reveals about pandemic preparedness in urban Indigenous communities in Australia. The Lowitja Journal. 2024/01/01/ 2024;2:100019. Doi:https://doi.org/10.1016/j.fnhli.2024.100019
43. Fredericks B, Bradfield A, McAvoy S, et al. Responding to COVID-19: How group model building can assist the health and well-being of urban Indigenous communities in Australia. Australian Journal of Social Issues. 2024/06/01 2024;59(2):462-486. Doi:https://doi.org/10.1002/ajs4.303
44. Fredericks B, Bradfield A, McAvoy S, et al. The Burden of the Beast: Countering Conspiracies and Misinformation within Indigenous Communities in Australia. M/C Journal. 02/21 2023;25(1) Doi: https://doi.org/10.5204/mcj.2862
45. Fredericks B, Bradfield A, Ward J, et al. Mapping pandemic responses in urban Indigenous Australia: Reflections on systems thinking and pandemic preparedness. Aust N Z J Public Health. 2023;47(5) Doi: https://doi.org/10.1016/j.anzjph.2023.100084
46. Fredericks B, Bradfield A, Ward J, et al. Tackling conspiracies and misinformation within Aboriginal and Torres Strait Islander communities. Croakey Health Media. 2022. Accessed 12 September 2024. https://www.croakey.org/tackling-conspiracies-and-misinformation-within-aboriginal-and-torres-strait-islander-communities/
47. Fredericks B, Ward J, McAvoy S, et al. Innovative research explores responses to COVID-19 among Indigenous communities in Brisbane. Croakey Health Media. 2021. Accessed 12 September 2024. https://www.croakey.org/innovative-research-explores-responses-to-covid-19-among-indigenous-communities-in-brisbane
48. Fredericks B, Ward J. Understanding health responses to COVID-19 in urban Indigenous communities in Brisbane. Croakey Health Media. 2021. Accessed 12 September 2024. https://www.croakey.org/understanding-health-responses-to-covid-19-in-urban-indigenous-communities-in-brisbane/
49. Fredericks B. What the urban Indigenous health sector reveals about systemic responses to COVID-19. Presented at: Native American and Indigenous Studies Association Conference Regional Gathering; 2022; Brisbane, Queensland, Australia.
50. Spierings S. Pandemic health messaging for Indigenous peoples during COVID-19. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
51. Spierings S. Pandemic health messaging for Indigenous peoples. Presented at: 2nd Australasian COVID-19 Conference; 2022; Sydney, NSW, Australia.
52. Saunders P. Revisiting the ‘Gambling Bug’ during COVID isolation: Using Participatory Action Research to inform a holistic Aboriginal gambling awareness strategy in a regional and urban setting. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
53. McCarthy S, Widdicombe D. The experiences of using telehealth in rural and regional Victorian ACCOs during COVID-19: perspectives from health service managers, clinic staff and patients. Presented at: First Nations COVID-19 Research Symposium; 2023; Brisbane, Queensland, Australia.
54. The Australian Partnership for Preparedness Research on Infectious Disease Emergencies. FIRST Governance Group. Accessed 12 September, 2024. https://www.apprise.org.au/people/people-category/first-governance-group/




