Impact of COVID-19 on Youth Athletes’ Health
Implications of the COVID-19 Pandemic on the Current & Future Health of Youth Athletes via the Ecological Model for Health Promotion
Justin S. DiSanti, PhD 1; Joseph Janosky, DrPH, MSc, PT, ATC 2; Gretchen Oliver, PhD, FACSM, ATC, CES 3; David Bazett-Jones, PhD, AT, ATC, CSCS4; Sophia Ulman, PhD5,6
OPEN ACCESS
PUBLISHED:30 November 2024
CITATION: Disanti, JS., Janosky, J., et al., 2024. Implications of the COVID-19 Pandemic on the Current & Future Health of Youth Athletes via the Ecological Model for Health Promotion. Medical Research Archives, [online] 12(11). https://doi.org/10.18103/mra.v12i11.5937
DOI https://doi.org/10.18103/mra.v12i11.5937
ISSN 2375-1924
ABSTRACT
The participation limitations and experiential challenges stemming from the COVID-19 pandemic threatened the potential for youth sport participation to positively impact the multidimensional development of adolescent athletes. As society moves on from the novel conditions of the pandemic, it is important to take stock of the deficits that adolescent athletes and their supporting stakeholders experienced during this time, while also planning productive steps to learn and grow from this experience. Thus, the purpose of this paper was to conduct an evidence-based review of existing literature of this topic, purposefully organized through the lens of the Ecological Model for Health Promotion. By identifying emerging trends, gaps, and interactions of between each level of this model (i.e., intrapersonal, interpersonal, organizational, community, public policy) in relation to literature related to youth experiences during the COVID-19 pandemic, several promising avenues for future research inquiry and practical application are proposed. Through this approach, the paper aims to assist in better embodying a systematic approach that targets areas of deficit and needs that were uncovered or exacerbated by the pandemic.
Keywords: Sports/athletics; physical activity; psychosocial development; mental health; family relationships; COVID-19 pandemic
Introduction
The COVID-19 pandemic has disrupted all levels of society and added, or exacerbated, threats to multiple domains of health and quality of life. Accumulating research has identified declining physical health (e.g., increase in sedentary behavior, lower physical competency, heightened risk of injury)1-3 as well as psychosocial health (e.g., rise in anxiety and depression, social isolation, professional burnout)4-6 both for those who have tested positive for COVID-197,8 and as a general population.9-11 One notable context in which this impact has been uniquely experienced is that of youth sports, which has traditionally served as a key cog in the physical, emotional, and social development of young people.12-14
As the COVID-19 pandemic unfolded, sport programs of all levels were faced with difficult decisions about whether to cancel, reschedule, or continue their training and competitions.10,15,16 Restrictions for physical distancing implemented by schools, businesses, and institutions explicitly prohibited, or limited opportunities for sport engagement.15,17,18 While efforts were made to adjust safety regulations and program logistics to eventually resume sport activities among the pandemic – especially at the professional and collegiate levels19,20 – the novel circumstances of the pandemic were especially challenging to youth programs that did not possess the resources, personnel, and infrastructure to execute the plans and protocols of more professionalized organizations.21,22
Youth sport stakeholders and pediatric medical practitioners emphasize an evidence-based approach to structuring sport participation;23-25 however, what can be done when existing evidence does not accurately reflect the current state of society? This question was posed to youth sport researchers and practitioners during the pandemic, and led to a wave of published reviews,26-28 perspective pieces,29-31 and original empirical research2,32 to take stock of the health of pediatric athletes amidst the pandemic. However, the next step for integrating and applying this knowledge is through the use of existing theory and conceptual frameworks to understand and plan future steps for structuring youth sport systems to deliver well-rounded, health-promoting experiences for young athletes.
One such model that has been utilized in this regard – and which is well suited to the interactive, complementary levels of society that have been impacted by the pandemic – is the Ecological Model for Health Promotion (EMHP).33 Therefore, this paper aims to collate and describe the current state of literature related to the COVID-19 pandemic’s impact on the health of pediatric athletes, framed through the constructs of the EMHP. Through this approach, the purpose of this evidence-based, integrative review is to identify trends and gaps in research and clinical knowledge as mapped onto this model. Applying these findings, practical initiatives to promote the health of pediatric athletes as we learn from the unique circumstances imposed by the COVID-19 pandemic will also be proposed.
The Ecological Model for Health Promotion
Ecological models are utilized in the public health domain to develop health improvement and promotion strategies. Historically, ecological models depict factors that influence health promotion behaviors, and also to describe relationships between factors associated with a specific health issue. The assumption that multiple factors influence health-promotion behaviors (HPBs) and associated outcomes is common among all ecological models. One of these models – the Ecological Model for Health Promotion (EMHP) was first introduced by a group of public health and health education experts from the United States in 1988,33 as a variation of previously developed ecological models more broadly related to the social sciences and youth development.34-36 The EMHP was developed to categorize factors that specifically influence health-related behaviors at the intrapersonal (individual), interpersonal, organizational, community, and public policy levels33 (See: Figure 1).
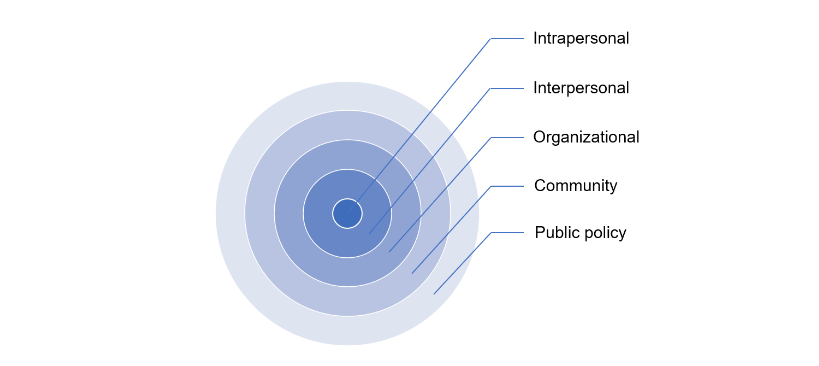
This method of categorizing individual and socioenvironmental factors uniquely supports the systematic development of interventions that can favorably influence health.33
The five levels of the EMHP are rooted in the assumption that health promotion interventions are derived from beliefs, understandings, and theories related to behavioral determinants. When assessing the process and evaluation outcomes of health promotion strategies, such as sport participation, there can be an overwhelming sense of complexity. However, the unique factors of influence identified at each level of the EMPH allow for systematic and organized evaluations of HPBs.
First, many of the factors identified at the intrapersonal level of the EMPH were derived from the assumption that the factors leading to health behaviors and the strategies used to change those behaviors are inherent to the individual, rather than part of the social environment.33 These factors position the individual at the center of the model and include their personal characteristics such as knowledge, attitudes, behavioral intentions, existing behaviors, skills and abilities, and the developmental history of the individual. Health promotion interventions designed to elicit behavior change through knowledge transfer or skill acquisition for individuals are often based on intrapersonal level factors.
Second, interpersonal relationships between an individual and their friends, colleagues, family members, and neighbors can serve as the source of factors that promote or dissuade HPBs. The formal and informal networks that grow from these interpersonal relationships are essential components of an individual’s social identity and may shape their health-related beliefs and outcomes. Health promotion interventions designed to foster behavior change through the influences of social norms are often based on interpersonal level factors.
Third, relationships between an individual and organizations or institutions can influence HPBs. Influences generated by rules, regulations, and guidelines within organizations can impact the implementation and adoption of HPBs, including investment in activities that achieve organizational change and the leveraging of organizational structures to disseminate health promotion interventions. While most organization-based interventions are designed with the support of an organization in mind, some interventions facilitate support and influence from organizations to foster behavioral change, while others rely on the structure within an organization to help distribute or socialize interventions.
Communities comprise the fourth layer of the EMHP. Under the EMHP, a community is defined as a collection of organizations or institutions within a defined area that are composed of individuals who interact face-to-face, and function under the jurisdiction of one or more power structures.33 HPBs can be impacted by community-level relationships associated with geographic proximity and mediation frameworks, while power structures can influence health behaviors of individuals through cultural and other norms.
Public policy is the fifth and most distal level of the EMHP. This policy level includes laws, regulations, ordinances, and mandates enacted at the local, regional, state, and/or federal level to promote or inhibit health behaviors.33 The use of regulatory policy has long been used to successfully ensure public health and can be restrictive, regulatory, or facilitating in nature. This level is strongly influenced by the mediating ability of communities and often promotes health behaviors that are most beneficial for the most people.
Ecological Model of Health Promotion: Application to COVID-19 Pandemic Literature
To develop a thorough understanding of existing evidence related to pediatric athletes and the COVID-19 pandemic, our first step was to conduct a literature review to identify key findings, trends, and gaps. The findings of this search were then mapped onto the EMPH framework, and are categorized by each respective level below:
INTRAPERSONAL
The EMBP starts by placing the individual at the center of the model, detailing intrapersonal factors such as the person’s perceptions, attitudes, behaviors, abilities, and history of development are incorporated.33,37 Broadly, there is accumulating evidence that the pediatric athlete population experienced multifaceted deficits to domains of their health at the intrapersonal level. Examples of these deficits include physical deficits (e.g., decreased cardiovascular fitness, higher sedentary behavior),3,5,37 mental health challenges (e.g., loneliness, increased hyperactivity and inattention),4,28 and shifts in their attitudes and behaviors related to sport and physical activity.3, 14, 38
Perhaps the most obvious domain because of the limitations in accessing physical sport spaces during the pandemic, physical health deficits were a common area of inquiry in taking stock of the pandemic’s impact on developing athletes. Unsurprisingly, the disruption to organized sport opportunities was associated with the physical deconditioning of athletes, as well as a higher rate of sport-related injuries upon returning to sport participation.16 However, individual sports may have been more protected from this injury rate spike, with a study of youth runners finding no significant difference in running-related injuries between pre- and post-pandemic measurements.39
It is also important to examine how pandemic-related changes at the intrapersonal level have impacted the behaviors, and behavioral intentions, of pediatric athletes. Associated with the physical space and activity limitations imposed at the height of the pandemic, youth athletes of various ages indicated that their sport-specific training time decreased.40 Most evidence related to levels of physical activity indicated a general decline during the pandemic.27,38,39,41 However, this finding was not universal depending on the way “physical activity” was operationalized, with one study finding that exercise and unstructured play may have actually increased, as well as time spent outside.40
There is also evidence to suggest that the underlying attitudes related to sport participation may have been influenced by the pandemic, with one study finding that between 10-20% of youth athletes changed their athletic goals, specifically in setting goals viewed as less ambitious, compared to their pre-pandemic goals.40 Degree of motivation to participate also seems to have been impacted, with one study of youth distance runners reporting lower overall motivation to run, and less enjoyment when they did so.42 Another qualitative examination of youth athletes’ experiences indicated that the pandemic served as a time of reflection for youth sport stakeholders regarding “what matters most” in their participation – both in examining the aspects they would like to change, as well as the positive benefits that may have been taken for granted.43 Further research is necessary to determine if these attitudes will rebound as sporting opportunities stabilize, or if these attitudinal shifts will persist.
Another intrapersonal domain that has come under the microscope is that of mental health, generally illustrating challenges that youth athletes faced during this time period.3,44 For example, the conditions of the pandemic exacerbated feelings of loneliness45,47 and elevated symptoms of depression and anxiety.6, 42, 45,47 One study found that adolescents who were isolated from peers showed higher levels of hyperactivity and inattention than those who were able to connect virtually with their friend groups.45 Interestingly, there is evidence that members of the pediatric population who were active in athletics experienced a lesser degree of psychological disruption than those who were not participating.2,32,48 It was found that high school athletes who had been active in a sport during the Fall 2020 season were less likely to report moderate or severe symptoms of anxiety and depression, while indicating a significantly higher overall health-related quality of life (HRQOL) than their peers who were not active in a fall sport.2 However, pediatric athletes were still vulnerable to intrapersonal mental health challenges, as one study found that 22-28% of their sample showed at least mild symptoms of anxiety or depression.40 Another indicated that adolescent athletes were three times more likely to report moderate or severe symptoms of anxiety and depression in comparison to data collected prior to the declaration of COVID-19 as a global pandemic.2 A study which tracked adolescent mental health over multiple years demonstrated that pandemic-related mental health deficits have begun to rebound as society has approached a higher degree of normality,49 though still not to their pre-pandemic levels. There is also evidence linking sport and sociodemographic characteristics to different mental health experiences during the pandemic, including higher rates of severe anxiety in female athletes, higher depression in team sports compared to individual-based sports,40 and lower HRQOL for those living in high poverty areas.2
Research related to the pediatric population’s intrapersonal health has begun to take stock of the multidimensional health impact of the COVID-19 pandemic. At an intrapersonal level, various physiological markers,3,5,38 health-related behaviors,18,42,49 and psychosocial constructs4,6,16 have indicated a decrease in quality of health. While there is evidence that sport participation may have mediated some of these psychosocial deficits in relation to the general pediatric population,2,32 further questions remain in understanding ongoing trajectories of these variables, and the degree to which they will return to normal in the coming years.
INTERPERSONAL
To better understand how the challenges faced by pediatric athletes during the pandemic were influenced by those around them, it is vital to take stock of how the numerous interpersonal, between-individual factors influenced their health and well-being. Factors that were hypothesized to contribute to the observed decrease in adolescents’ HRQOL were limited socialization, increased family strain, and reduced access to support services typically provided by schools.2 These explanations align with findings indicating more positive mental health profiles, higher perceptions of well-being, and a smaller decline in athletic identity by team sport athletes in comparison to those who could not receive this interpersonal connection through sport.2,49,50 Further underscoring this interpersonal importance, athletes who lacked social connection through school sports were more likely to report moderate to severe anxiety or depression even after adjusting for age, sex, school instruction type, and socioeconomic status.49 This lack of association implies that while physical activity has traditionally been beneficial for reducing symptoms of depression, this positive potential to improve quality of life and mental health was outweighed by a lack of engagement and connections in the social, interpersonal youth sports environment following the mandatory pandemic-related shutdown.50
A key component of a pediatric athlete’s interpersonal experience is their family unit, as participation is linked to their family’s routine/schedule, financial decisions, food/meal choices, travel plans, and social relationships.51-55 Youth sport parents are central in this process, as their investment of time and energy is often linked to a sense of fulfillment and shared achievement with their child.56 Thus, cancellation of youth sports during the pandemic not only impacted the child, but also their parents and family unit.55 To this end, Dorsch et al. reported on parents’ feelings towards sport participation during the pandemic, finding a decline in participation rates of nearly 50% across free play, focused practice, and game/competition environments – primarily due to parents’ fear of themselves or their child becoming ill.57 In the same vein, Reynolds et al. reported that physical space restrictions led to fewer child-parent interactions and a diminished connection through sport.58 They further described parents’ feelings of grief, frustration, and sadness due to the restrictions that ultimately impacted the youth athlete and the parent-athlete relationship. Similarly, Donker et al. found that the pandemic led to decreased support, lessened “positive parenting” practices, and more frequent negative interactions between the parent and adolescent.59 Specifically, the authors highlighted worsened parent-adolescent relationships if the adolescent exhibited high stress levels and active coping strategies. While there is certainly evidence that the pandemic strained the quality of parent-athlete relationships, those who were able to maintain a high-quality relationship provided encouraging signs, as adolescents with a closer relationship with their parents were found to struggle less with mental health and experience lower levels of loneliness.45
One popular solution to mitigating social isolation in the midst of activity and physical space restrictions was through virtual engagement. Bates et al. investigated the impact of virtual sport-based activities promoting learning and positive youth development among socially vulnerable youth and their families.17 They found that families engaged in the provided virtual programming an average of three times per week, indicating that the activities were enjoyable and promoted relationship-building and interactions with members of their extended family and community. While virtual programming may not be as widely adopted following the shutdown, these findings highlight an accessible and impactful avenue for socially vulnerable youth to experience the interpersonal benefits of sports. In contrast, for more competitive youth athletes familiar with a more intense training regimen, Philippe et al. described a deterioration of the coach-athlete relationship primarily due to distance, which was reflected in the athletes’ practice performance. Specifically, athletes faced challenges in connecting socially through sport due to their adapted practice environment. This drastically strained the quantity and quality of coach-athlete interactions, which in turn resulted in reduced motivation of the athlete to practice or train for their sport.60
Additionally, the economic hardship that the pandemic brought to many families greatly impacted their availability of the resources required to remain engaged in training, while increasing the accessibility gap between families of different income classes.55 For example, athletes from higher income households could more feasibly invest in private training, high-quality at-home training regimens, or virtual workouts that required technology and reliable internet connectivity. Alternately, athletes from lower income families were less likely to train if their parents increased their work hours to offset the financial burden of the pandemic. Family income has been explicitly linked to youth sport participation decisions prior to the pandemic,61 suggesting that this association would have an even greater impact when financial burdens stemming from the pandemic impacted an athlete’s interpersonal support system.
ORGANIZATIONAL
Moving from the person-related domains of the EHPM, it is important to transition to understanding the proverbial “playing board” in which these interactions take place, starting with the organizational level. Existing frameworks of motivation and their link to behaviors indicate that organizational structures work in interaction with individual’s intentions, mediating them through perceived behavioral control.62 For example, data collected during the pandemic indicates that youth athletes received greater exposure to different forms of sport and physical activity.63 Organizations are then urged to match this expanded and diversified interest, which may or may not fall within the scope of that organization’s access and available resources. For example, many organizations shifted their sport focus to outdoor venues and virtual sport programming, but this required a geographic, financial, and technological affluence that was not feasible for all organizations.64 It has been documented that urban communities generally provide more opportunities for sport and physical activity;22 however, due to population density and physical distancing restrictions enacted during the pandemic, the use of facilities in urban organizations was limited. On the other hand, though rural communities have less physical activity facilities, there were more opportunities for sport participation.
Additionally, heightened media exposure for sport participants, stakeholders, and even fans helped position the importance of sport-related organizations. Many organizations implemented the concept of mediazation which includes the elements of perception, structure, and behavior of the community.64 Essentially accentuating the perception of increased media importance in promoting healthy behaviors, organizations began to understand how the process of communication can change the social and cultural environment that supports the active behavior between individuals and institutions. These increased awareness and heightened value of sport and physical activity may increase the potential impact of youth sport organizations, and efforts should be made to capitalize on this increased attention through rostering connections between organizations and the stakeholders they serve.
COMMUNITY
Communities are the next level of influence on the individual in the EMHP. For the purposes of this manuscript, communities are defined as collections of organizations and institutions that function under the jurisdiction of one or more power structures.33 Behaviors that promote health among individuals are often shaped by their relationships with communities due to factors like geographic proximity, mediation frameworks, and cultural norms. Unlike the person-centered levels of the EHPM, few researchers investigated community-based factors that influenced adolescent sports participation as a health promoting behavior during the COVID-19 pandemic.
Among researchers who identified community-based influences on athlete health during the pandemic, many investigated community-level communications and guidance related to sport participation recommendations, the residual impact of activity restrictions on athlete health, and the economic fallout related to altered sports schedules. For example, Pierce et al. studied the perceptions and opinions of pandemic-related guidelines developed by the National Federation of State High School Associations (NFHS) to help inform return to sport decision-making by sports facility operators and event managers.14 The authors reported that guidelines such as monitoring and enforcing social-distancing, limiting player-to-player contact, restricting event admission to individuals without pre-existing health conditions, and the administration of health screening questionnaires to event attendees were deemed mandatory by parents and other youth sports stakeholders for a safe return to sports during the pandemic. Similarly, Mirabito et al. examined pandemic-related communications and guidance from the National Collegiate Athletic Association (NCAA) and several collegiate athletic conferences about ongoing sport participation and found that fragmented and contradictory messaging negatively impacted the ability of the collegiate sports community to deliver safe sports experiences to student-athletes.65
Many decisions to limit sport participation during the COVID-19 pandemic were made at the community level. These decisions ultimately led to a dramatic decrease in physical activity rates and several associated negative health outcomes. For example, Bullock et al. studied associations between pandemic-related sport participation restrictions and sports-related injuries among high school students. The authors reported that prolonged sport stoppage of high school sports due to the COVID-19 pandemic resulted in increased injury incidence among high school sports participants compared with the previous high school academic year.66 Thus, community initiatives to monitor and reduce these injury rates should be implemented to ensure an adaptive, health sport environments for their community members.
PUBLIC POLICY
Public policy influences all other levels of the EMHP and often impacts the individual both directly and indirectly. While there were many policy changes enacted to reduce interpersonal interaction and promote COVID-19 prevention, there has been no research to directly measure the impact of differing policies (i.e., quarantine) on youth sport participation. However, structures and policies enacted prior to the COVID-19 pandemic, like universal health care or health care infrastructure, have likely impacted individual experiences during and following the pandemic.67 Social, economic, and racial inequities that were present prior to the pandemic were magnified by the policy responses to it.68 The COVID-19 pandemic disproportionately impacted sport participation of socially vulnerable youth21 and will require focused efforts at the policy and funding level to recover. Further, the impact of policies enacted during the COVID-19 pandemic may have impacted team sports differently than individual sports that don’t require training facilities and significant interpersonal interaction. In runners, for example, the Fall 2020 season status (i.e., cancelled, delayed, full season) did not significantly change the number of regular or high intensity runs per week, nor did it influence their weekly running distance.39
Overall, the COVID-19 pandemic can be seen as a case study on the impact of policies enacted that canceled or severely reduced access to sport participation in youth. These policies, though necessary, had a significant impact on youth athlete mental and physical health in ways that had short-term and possibly long-term implications.
Summary & Implications
Our literature review (summarized in Appendix A) sought to collate existing research related to youth athletes and youth sport systems during the COVID-19 pandemic, to take stock of the disruptions and deficits that these groups experienced during this time, as well as how these changes impacted their overall experiences. Through this structured approach guided by the EMHP, we have aimed to identify meaningful strategies and future initiatives that can be applied in youth sport settings to stabilize, and ultimately maximize, the success of youth sport programming as society moves beyond the pandemic.
- Capitalize on increased awareness of psychosocial health→ noted fluctuations in psychosocial variables (e.g., loneliness, depression, anxiety) implies that those reporting these outcomes would be more sensitive to their importance in their quality of life. Therefore, it would stand to reason that individuals would be more receptive to the need of psychosocial health promotion efforts, which includes those who are responsible for making decisions at the institutional, community, and public policy levels. Youth sport stakeholders and mental health proponents should capitalize on this organic swell of interest, putting into place practical initiatives to help youth sport athletes develop mental, social, and “life skills” that can benefit their long-term quality of life as they develop and navigate ups and downs on and off the field.
- Monitor multi-level health-related disruptions associated with the pandemic and their potential stabilization→ a clear trend among the intrapersonal and interpersonal research related to the pandemic indicates that youth athletes and associated stakeholders experienced multifaceted negative impacts to their overall health.2,6, 55,60 While sport and physical activity participation may have alleviated these deficits in some cases, it is important to determine if these health variables rebound to a more typical level as society returns closer to “normal.” If this does not occur, further longitudinal efforts should be made, in conjunction with the ecological approach of this model, to determine barriers and facilitators to this stabilization process.
- Identify important organizational and community characteristics to capitalize on “local knowledge”→ handling the challenges imposed by the pandemic made clear that organizational and community characteristics influence their stakeholder’s desired approach in maximizing the quality of their youth sport programming.17,55 However, research from the pandemic that parsed out similarities and differences in sport programming may aid in identifying future points of leverage (e.g., receptiveness to virtual programming)17,60 that are tailored to the characteristics of these groups (e.g., high vs. low income areas)2,17 so that organizations and community stakeholders can facilitate a targeted, localized approach in developing youth sport opportunities for the families they serve.
- Expand our understanding of policy-level initiatives that were influenced, or implemented in response to the pandemic→ one notable area of the EMHP that was lacking in our review of literature was that of the policy level. Previous research has noted important policy level measures related to the health of pediatric athletes,69 suggesting that to best understand how individuals act and interact, it is first vital to take stock of the higher-level guiding structures that are influencing their experience. Research into how sport stakeholders changed policy and procedures related to health promotion of their athletes would be an excellent place to start in understanding their impact. Moving forward, then tracking how these policies are implemented, evolve, and impact youth athletes would help in taking lessons learned from the ultimately short-term window of the pandemic, while providing a more stable foundation for positive growth of youth sport organizations and programs moving forward.
- Structure research designs to account for multi-levels of the Ecological Model of Health Promotion→ in examining and identifying gaps in the literature related to each construct of the EMPH, there were a handful of instances in which variables from multiple levels of the model were included in study design (e.g., association between parent attitudes and child behaviors at the interpersonal level).57,59 However, there was only one study that explicitly used an ecological framework to guide their research,66 and therefore there were a lack of studies which examined multiple levels of the model in conjunction. Proponents of ecologically-guided research have critiqued this common lack of connection and interaction in existing literature, a characteristic even occurring in studies explicitly labeled as “ecological.”70 Thus, it is critical to adopt more ecologically-grounded designs to not only understand athletes in a vacuum, but instead to position them at the center of the ecological playing field, and then to understand how the surrounding levels of this model (i.e., organizational, community, and policy) inform and interact with the athlete in shaping their experience.
Conclusions:
This evidenced-based review of recent literature, through the lens of the EMPH, identified trends, gaps in knowledge, and several proposed practical strategies for promoting the holistic health of adolescent athletes and associated stakeholders as society aims to move forward productively from the COVID-19 pandemic. While adolescent researchers have developed a thorough understanding of the multifaceted health impact imposed by the pandemic, further research and practical efforts must be employed in order to monitor, and ultimately restore, adolescent athlete’s health-related quality of life to pre-pandemic levels.
Conflicts of Interest Statement:
The authors have no conflicts of interest to declare
References
- Dayton JD, Ford K, Carroll SJ, Flynn PA, Kourtidou S, Holzer, RJ. The deconditioning effect of the COVID-19 pandemic on unaffected healthy children. Pediatr Cardiol. 2021;42:554-559.
- McGuine TA, Biese KM, Petrovska L, et al. Changes in the health of adolescent athletes: a comparison of health measures collected before and during the COVID-19 pandemic. J Athl Train. 2021;56(8):836-844.
- Paterson DC, Ramage K, Moore SA, Riazi N, Tremblay MS, Faulkner G. Exploring the impact of COVID-19 on the movement behaviors of children and youth: a scoping review of evidence after the first year. J Sport Health Sci. 2021;10(6):675-689.
- Golberstein E, Wen H, Miller BF. Coronavirus disease 2019 (COVID-19) and mental health for children and adolescents. JAMA Pediatr. 2020;174(9):819-820.
- Pons J, Ramis Y, Alcaraz S, Jordana A, Borrueco M, Torregrossa M. Where did all the sport go? Negative impact of COVID-19 lockdown on life-spheres and mental health of Spanish young athletes. Front Psychol. 2020;11: 611872.
- Racine N, McArthur BA, Cooke JE, Eirich R, Zhu J, Madigan S. Global prevalence of depressive and anxiety symptoms in children and adolescents during COVID-19: a meta-analysis. JAMA Pediatr. 2021;175(11):1142-1150.
- Fraser E. Long term respiratory complications of COVID-19. BMJ. 2020;370:m3001
- Humphreys H, Kilby L, Kudiersky N, Copeland R. Long COVID and the role of physical activity: a qualitative study. BMJ Open. 2021;11(3):e047632.
- Chew HSJ, Lopez V. Global impact of COVID-19 on weight and weight-related behaviors in the adult population: a scoping review. Int J Environ Res Public Health. 2021;18(4):1876.
- Mel A, Stenson M. The lingering impact of COVID 19 shutdowns on physical activity habits in the United States. Phys Act Health. 2022;6(1):42-54.
- Varea V, Gonzalez-Calvo G, García-Monge A. Exploring the changes of physical education in the age of Covid-19. Phys Educ Sport Pedagogy. 2022;27(1):32-42.
- Strachan L, Côté J, Deakin J. A new view: Exploring positive youth development in elite sport contexts. Qual Res Sport Exerc Health. 2011;3(1):9-32.
- Logan K, Cuff S, LaBella CR, et al. Organized sports for children, preadolescents, and adolescents. Pediatrics. 2019;143(6):e20190997.
- Pierce D, Stas J, Feller K, Knox W. COVID-19: Return to youth sports: Preparing sports venues and events for the return of youth sports. Sports Innov J. 2020;1:62-80.
- Costello FE, Duggan K, Lang E, Norris S. A safe return to sport and the right to play during COVID-19. CMAJ: 2021;193(8):E291-E291.
- Vincent HK, Patel S, Zaremski JL. Impact of COVID on sports injury patterns, changes in mental well-being, and strategies to prepare for future pandemics in sport. Curr Sports Med Rep. 2022;21(6):196-204.
- Bates S, Greene D, O’Quinn L. Virtual sport-based positive youth development during the COVID-19 pandemic. Child Adolesc Soc Work J. 2021;38(4):437-448.
- Faraji S, Ghayour Najafabadi M, Rostad M, Anastasio AT. The effect of COVID-19 quarantine on physical and social parameters of physical education providers and youth sport coaches. Work. 2020;67(4):767-769.
- Post EG, Rivera MJ, Doss D, Eberman LE. Parent decision-making regarding youth sport participation during the COVID-19 pandemic. J Community Health. 2020;47(4):687-696.
- Root HJ, Abdenour TE, Eason CM, DiSanti JS, Post EG. Collegiate athletic trainers’ experiences implementing return-to-sport policies and procedures during COVID-19: A qualitative research study. J Athl Train. 2022;57(11-12):1100-1110.
- Son H, Berdychevsky L. COVID-19’s impacts on community-based sport and recreation programs: The voices of socially-vulnerable youth and practitioners. Leis Sci. 2022:1-22.
- Teare G, Taks M. Exploring the impact of the COVID-19 pandemic on youth sport and physical activity participation trends. Sustainability. 2021;13(4):1744.
- Côté J, Hancock DJ. Evidence-based policies for youth sport programmes. Int J Sport Policy Polit. 2016;8(1):51-65.
- Gould D, Carson S. Life skills development through sport: Current status and future directions. Int Rev Sport Exerc Psychol. 2008;1(1):58-78.
- Harris K, Adams A. (2016). Power and discourse in the politics of evidence in sport for development. Sport Manag Rev. 2016;19(2):97-106.
- Nobari H, Fashi M, Eskandari A, Villafaina S, Murillo-Garcia Á, Pérez-Gómez J. Effect of COVID-19 on health-related quality of life in adolescents and children: A systematic review. Int J Environ Res Public Health. 2021;18(9):4563.
- Paterson DC, Ramage K, Moore SA, Riazi N, Tremblay MS, Faulkner G. Exploring the impact of COVID-19 on the movement behaviors of children and youth: a scoping review of evidence after the first year. J Sport Health Sci. 2021;10(6):675-689.
- Racine N, McArthur BA, Cooke JE, Eirich R, Zhu J, Madigan S. Global prevalence of depressive and anxiety symptoms in children and adolescents during COVID-19: a meta-analysis. JAMA Pediatr. 2021;175(11):1142-1150.
- Ettekal AV, Agans JP. Positive youth development through leisure: Confronting the COVID-19 pandemic. J Youth Dev. 2020;15(2):1-20.
- Kelly AL, Erickson K, Turnnidge J. Youth sport in the time of COVID-19: Considerations for researchers and practitioners. Manag Sport Leis. 2022;27(1-2):62-72.
- Whitley MA, Smith AL, Dorsch TE, Bowers MT, Centeio EE. Reenvisioning postpandemic youth sport to meet young people’s mental, emotional, and social needs. Transl J Am Coll Sports Med. 2021;6(4): 1-7.
- Watson A, Koontz JS. Youth sports in the wake of COVID-19: a call for change. Br J Sports Med. 2021;55(14):764-764.
Appendix
Appendix A: Summary of Key Findings by Levels of Ecological Model of Health Promotion
| Level of Model | Literature Summary Findings |
|---|---|
| Intrapersonal | This was the most frequently-researched level of the model in exploring the experiences of youth athletes during the COVID-19 pandemic. Youth athletes experienced multifaceted deficits (physical, mental, social), which are still rebounding to normal levels as the pandemic subsides. Training schedules were disrupted, leading to physical and mental de-training effects. Youth athletes’ perceptions of the meaning of sport in their lives also appears to have been influenced by the pandemic, with many athletes changing their goals or competitive engagements. Youth sport participation appears to have mediated some of the negative effects of the pandemic that were experienced society at large. |
| Interpersonal | Interpersonal connection with family and social support system created a more positive experience for youth sport families during the pandemic. Those who lacked connection were at higher risk for increased anxiety, loneliness, and lower health-related quality of life. Parents had to adjust their expectations for their children’s sport activities, while also seeking alternative avenues to connect, such as virtual sport and exercise programming. Families were also impacted by economic hardships stemming from the pandemic, which further exacerbated the mental health challenges they were experiencing. |
| Organizational | Sport organizations were required to adjust their structure and delivery to suit the increasingly diverse demands and levels of access of youth sport families during the pandemic. Increased media exposure of sport programming during the pandemic positioned the importance of sport organizations in delivering opportunities for exercise engagement and health promotion. Organizations in more population-dense areas experienced greater challenges due to physical proximity restrictions, emphasizing the importance of a tailored approach that matches each organization’s member needs. |
| Community | Community guidelines and protocols helped structure youth sport participation in a safe, effective way during the pandemic, which highlights the importance of community entities in ensuring positive sport opportunities for their members. Consistency of communication was a key consideration at the community level, and establishing and refining shared protocols and expectations will remain a critical element of community programming for youth athletes and their families moving forward. Overall, community-level research of youth athletics during the pandemic was quite limited, likely due to restrictions that strained the ability to connect with other members of the community. |
| Public Policy | Public policy to guide physical distancing and safe engagement for youth sport opportunities were prevalent and essential to re-opening sports. However, research that directly measures, or compares, the impact of public policy measures related to the pandemic is lacking. Further efforts to understand how policy impacted participation, and ultimately experiences, during the pandemic may be illuminating in understanding effective policy measures as society moves forward from the pandemic. |

