Impact of Night-Duty on Sleep and Mental Health in Security Personnel
Investigating the Impact of Night-Duty on Sleep Architecture and Mental Well-Being in the Security Personnel: A Quasi-Experimental Study
Prafull Kamble, MD, MAMS. 1; Vandana Daulatabad, MD, MAMS. 2; Estelle H Earl, MD 3; Naveen Ravi, MD 4; Archana Gaur, MD 5; Madhusudhan U, MD 6; Nitin John, MD 7
- Vandana Daulatabad, MD, MAMS Associate Professor, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India
 http://orcid.org/0000-0002-5458-9872
http://orcid.org/0000-0002-5458-9872 - Prafull Kamble, MD, MAMS Additional Professor, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India. Mobile:9823013709
 http://orcid.org/0000-0002-7943-5810
http://orcid.org/0000-0002-7943-5810 - Estelle H. Earl, MD Senior Resident, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India
- Naveen Ravi, MD Senior Resident, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India
- Archana Gaur, MD Associate Professor, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India
- Madhusudhan U., MD Associate Professor, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana-508126, India
- Nitin John, MD Professor and Head, Department of Physiology, All India Institute of Medical Sciences, Bibinagar, Telangana,508126, India
OPEN ACCESS
PUBLISHED: 31 May 2025
CITATION:DAULATABAD, Vandana et al. Investigating the Impact of Night-Duty on Sleep Architecture and Mental Well-Being in the Security Personnel: A Quasi-Experimental Study. Medical Research Archives, [S.l.], v. 13, n. 5, may 2025. Available at: <https://esmed.org/MRA/mra/article/view/6525>.
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i5.6525
ISSN 2375-1924
Abstract
Background: In a world that never sleeps, the role of security personnel is vital in maintaining order, safety, and peace. While the responsibilities of security professionals are diverse and multifaceted, one aspect of their job that often remains hidden in the darkness is the relentless demand for night-duty shifts. This research delves into the often-overlooked consequences of night-duty shifts on security personnel. The study aims to investigate impact of night shifts on the physical health, psychological well-being of security professionals. By exploring the disruptions to sleep architecture, such as N2 stage of sleep, sleep efficiency, and the potential mental health implications like mental well-being, the research seeks to enhance understanding of the physiological changes in these dedicated professionals.
Methods: Using a novel quasi-experimental design approach, the study was conducted in AIIMS Bibinagar. Polysomnography (PSG) was used to monitor and analyze the sleep patterns of security personnel on night-duty shifts compared to off-duty periods. Additionally, mental well-being was assessed through validated mini state mental examination scores as psychological questionnaire.
Results: PSG parameters like sleep time have significantly decreased, sleep efficiency along with duration of sleep stages of N2 has significantly decreased. There is a notable rise in systolic blood pressure which can be correlated to a decrease in the sleep’s efficiency and total sleep time. These changes attributed to physiological changes due to sleep deprivation for the security personnel post night-duty shifts.
Conclusions: In conclusion, the reviewed literature and our current study clearly demonstrates the detrimental impact of night-duty on sleep architecture and mental well-being among security personnel. This study aims to provide the necessary evidence to develop and implement interventions that ultimately enhancing both personal and public safety.
Keywords: Mini-mental state examination (MMSE), Night-duty, Sleep study, Security personnel
Introduction:
In a world that never sleeps, the role of security personnel is vital in maintaining order, safety, and peace. While the responsibilities of security professionals are diverse and multifaceted, one aspect of their job that often remains hidden in the darkness is the relentless demand for night-duty shifts. In our modern 24/7 society, security personnel are tasked with the challenging duty of safeguarding our homes, businesses, and public spaces at all hours. This research paper aims to investigate consequences of night-duty amongst security personnel, exploring its impact on their physical health, psychological well-being. In the demanding profession of security personnel, night-duty assignments are a common and often unavoidable aspect of the job. These assignments can profoundly affect both sleep architecture and mental well-being. Sleep architecture, which refers to the structure and pattern of sleep cycles, is critical for restorative sleep and overall health. Disruptions to this architecture can lead to sleep disorders such as insomnia and obstructive sleep apnea [1], which are prevalent in individuals working irregular hours. Furthermore, the chronic sleep deprivation and misalignment of circadian rhythms associated with night shifts can exacerbate mental health issues, including anxiety, depression, and impaired cognitive function [2].
This quasi-experimental study aims to investigate the specific impacts of night-duty on sleep architecture and mental well-being among security personnel. By employing polysomnography, a comprehensive sleep study method was monitored and sleep patterns of participants after night-duty shifts compared to their off-duty periods. Additionally, we will assess mental well-being through validated psychological questionnaires and interviews, providing a holistic view of how night-duty influences both physiological and psychological health parameters.
Existing Gaps in Research
While there is extensive literature for the effects of night shifts on sleep and mental health, specific sleep studies focusing on security personnel are limited. Most research has concentrated on healthcare workers, industrial workers, and other profession [3]. There is a need for targeted research that addresses the unique challenges faced by security personnel, including the variability of their work schedules and the psychological demands of their roles.
Aims and Objectives:
a. Primary objective: i) To assess the physiological parameters like pulse and blood pressure; ii) To assess sleep architecture by polysomnography; iii) To assess mental health status by Mini Mental State Examination (MMSE) in security personnel; iv) To compare sleep architecture using Polysomnography (PSG), pre and post night-duty; v) To compare cognitive mental health using MMSE scores, pre and post night duty.
b. Secondary objective: i) To find out the correlation between physiological parameters with PSG scores; ii) To find out the correlation between mental health parameters using MMSE to PSG parameters.
Methodology:
The study protocol was reviewed and approved by the Institutional Research Cell (IRC) and the Institutional Ethics Committee (IEC) at AIIMS Bibinagar, vide letter number AIIMS/BBN/IEC/JAN/2024/362, dated 27/01/2024. All ethical guidelines as per the Declaration of Helsinki were followed throughout the study. Prior to participation, all subjects were informed about the purpose, procedures, potential risks, and benefits of the study. Written informed consent was obtained from all participants. It was clearly communicated that participation was entirely voluntary and that participants could withdraw from the study at any stage without any adverse consequences or obligations.
Study Design: This study employed a quasi-experimental pre-post design to assess the effect of night duty on physiological, sleep, and cognitive parameters in healthy adult security personnel. Each participant was assessed at two time points: once during day duty (baseline) and once following a rotation of seven consecutive night duties.
Sample Size: A convenient sample size of 30 participants was selected. Random sampling was employed to minimize selection bias and ensure representativeness within the available population of hospital security staff.
Inclusion criteria: Healthy adult security personnel aged between 25-50 years without any other co-morbid conditions which affects sleep-wake cycle like depression, anxiety, heart failures, chronic respiratory disorders, gastro-esophageal reflux disease; those personnel willing to participate in the study voluntarily; those security personnel who had completed their rotation night-duty of seven days were included in the study as study participants.
Exclusion criteria: Security personnel not willing to participate in the study; those with any other co-morbid conditions which can affect sleep-wake cycle like depression, anxiety, heart failures, chronic respiratory disorders, gastro-esophageal reflux disease; those on medications for these disorders; those security personnel in the habit of smoking cigarettes, consuming alcohol will be excluded from the study. Participants were instructed to avoid the consumption of stimulants including coffee, tea, tobacco, or energy drinks for at least 24 hours prior to the polysomnography (PSG) assessment.
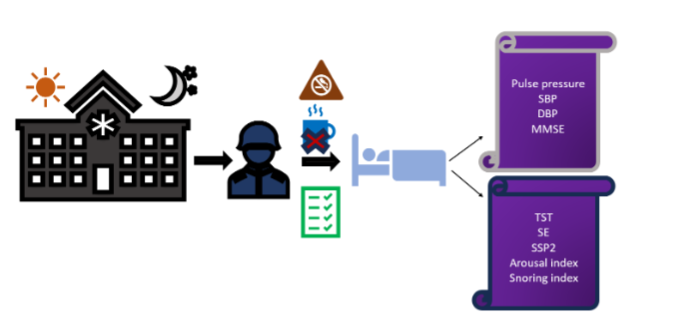
Data Collection Procedure: The study involved two sessions of assessment for each participant: Baseline assessment (during day duty) was conducted during routine day-time working hours (Figure 1). Participants’ basic demographic details such as age, weight, height, work experience, and duty schedule were recorded. Physiological parameters like Pulse, Blood pressure was measured. PSG parameters like total sleep time, sleep efficiency, sleep stage percentage (N2), arousal index and snoring index were recorded using equipment Somnomedic (Germany). Cognitive mental health using Mini mental state examination scores. Post-Night Duty Assessment (After Seven Consecutive Night Duties) was conducted immediately following a scheduled seven-day night duty rotation. The same set of measurements—physiological, cognitive, and PSG parameters—were recorded following identical procedures and using the same equipment and settings to ensure consistency.
Statistical Analysis: Data were entered into Microsoft Excel and analyzed using SPSS version 29.0. Descriptive statistics (mean, standard deviation, frequencies, and percentages) were used to summarize demographic and baseline data. Paired t-tests were used to assess significant differences between pre- and post-night duty values for continuous variables. Pearson’s correlation coefficient was used to determine the strength and direction of relationships between physiological, sleep, and mental health parameters. A p-value of <0.05 was considered statistically significant.
Results:
| Parameters | Pre | Post | T test | Significance |
|---|---|---|---|---|
| Pulse | 77.34 ± 12.5 | 79.83 ± 12.4 | 0.1417 | Significant |
| Systolic BP | 123.27 ± 11.6 | 124.13 ± 11.6 | 0.2812 | Not significant |
| Diastolic BP | 77.9 ± 7.7 | 79.9 ± 8.4 | 0.0124 | Highly significant |
The physiological parameters (Table 1) like pulse, systolic and diastolic blood pressure show significant variations in these parameters in the same individuals who had carried out tests before and after the night-duty schedule in the security personnel.
| Parameters | Pre | Post | T test | Significance |
|---|---|---|---|---|
| Total Sleep time | 4.06 ± 0.03 | 3.18 ± 0.04 | 7.67E-05 | Highly significant |
| Sleep efficiency | 6.43 ± 9.6 | 10.58 ± 11.6 | 0.004 | Significant |
| Sleep stages percentage(N2) | 61.34 ± 14.4 | 49.67 ± 14.3 | 0.000003 | Highly significant |
| Arousal index | 20.28 ± 11.0 | 22.53 ± 14.6 | 0.01 | Significant |
| Snoring index | 87.5 ± 13.3 | 66.73 ± 12.6 | 0.007 | Significant |
The polysomnography parameters like TST (total sleep time), SE (sleep efficiency), sleep stage percentage (N2), arousal index and snoring index. The parameters (Table 2) like total sleep time have significantly decreased, sleep efficiency has significantly decreased, duration of sleep stages as N2 has decreased which is a significant decrease, while arousal index and snoring index has a significant change.
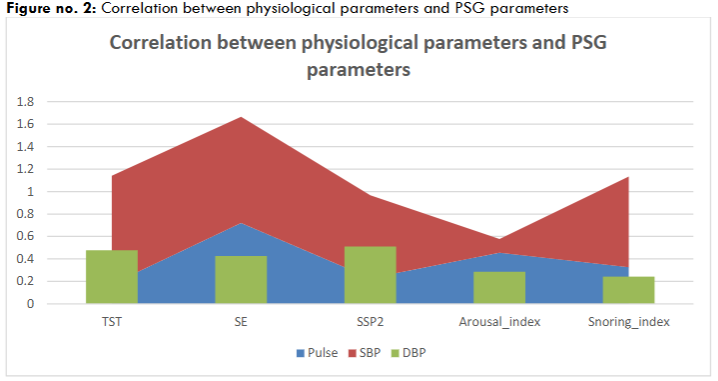
There is a significant correlation using Pearson’s correlation between physiological parameters like pulse, systolic blood pressure (SBP) and diastolic blood pressure (DBP) (Figure 2). There is a notable rise in systolic blood pressure can be correlated to a decrease in the TST and SE. These changes can be attributed to physiological changes due to sleep deprivation for the security personnel post the night-duty shifts.
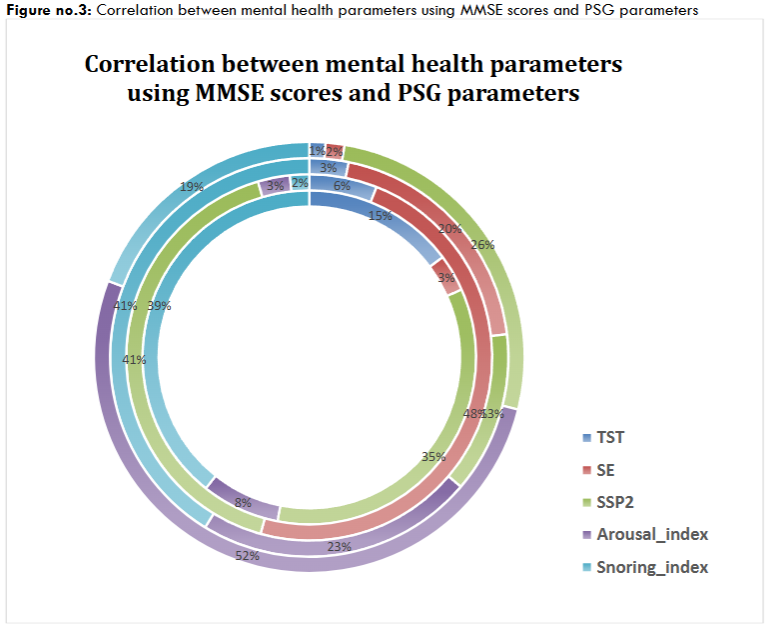
There is a significant correlation using Pearson’s correlation between MMSE scores and PSG parameters (Figure 3). The scores of MMSE are supposed within the range of 25-30 which relate to the mental state of the participants which shows significant correlation in the changes of the MMSE scores and PSG parameters.
Discussion
Disruption of Sleep Architecture: Studies using polysomnography (PSG) have documented reductions in REM sleep and slow-wave sleep among night shift workers, including security personnel [4]. These disruptions are primarily due to the misalignment of the circadian rhythm, which is naturally programmed for activity during daylight and rest during the night [5]. Shift work plays a vital role in sustaining the 24/7 operations of various industries, including healthcare, emergency services, transportation, hospitality, and manufacturing. A recent analysis by the International Labor Organization (ILO) and the European Foundation for the Improvement of Living and Working Conditions examined shift work across 187 countries, involving approximately 1.2 billion workers. This study highlights the widespread nature of shift work and its critical impact on both individuals and the global economy, Eurofound and International Labour Organization, 2019 [6]. The World Health Organization (WHO) has classified night shift work as a probable carcinogen, reflecting its potential to contribute to cancer risk. Research conducted across various countries highlights that sleep deprivation significantly affects both the academic performance of medical students and their overall health. For hospital shift workers, particularly those assigned to night shifts and emergency duties, the health implications are notable. These workers often experience various health issues that not only compromise their well-being but also diminish their job performance [7]. For security personnel, the irregular and extended hours exacerbate these disruptions, leading to chronic sleep deprivation and fragmented sleep patterns [8]. The consequences of disrupted sleep architecture are profound. N2 and REM sleep is crucial for cognitive functions such as memory consolidation and emotional regulation, while slow-wave sleep is essential for physical restoration and immune function [9]. Therefore, the reduction in these sleep stages can impair job performance and overall health, posing significant risks given the high-stress and high-responsibility nature of security work.
Prevalence of Sleep Disorders: Shift work sleep disorder (SWSD) is a common consequence of night-duty, characterized by insomnia and excessive sleepiness during wake hours [10]. Approximately 20-30% of night shift workers suffer from SWSD, which severely impacts their cognitive and physical capabilities [1]. Additionally, obstructive sleep apnea (OSA) prevalence is higher among shift workers due to increased BMI and lifestyle factors associated with irregular work hours [11]. These findings underscore the need for regular sleep assessments and interventions to manage and mitigate sleep disorders among security personnel.
Effect of physiological parameters on sleep: Research conducted by Hussain MS and Tyagi R (2018) on 70 individuals, including 35 shift workers and 30 controls, revealed higher diastolic blood pressure in shift workers [12]. A similar study by Nour Makarem et al. (2021) reported comparable results, confirming an increase in diastolic blood pressure among shift workers [13]. Additionally, our study identified a notable impact on the health of security personnel after night duty. A significant difference in the diastolic blood pressure and pulse pressure was found between pre and post night duty parameters (Table 1).
Effect of total sleep parameters: A meta-analysis by J.J. Pilcher et al. (2015), involving 36 studies, explored temporary and permanent shift rotations on total sleep time. The study highlighted that permanent shift rotations had the least negative effect on sleep health, while temporary rotations were more disruptive. Moreover, the speed of rotation influenced sleep architecture, with slower rotations causing less reduction in total sleep time compared to rapid rotations [14]. Similarly, a cross-sectional study by Sanapala Vidya et al. (2019), which examined 147 rotating shift workers and 132 regular day workers from various industries, reported that shift work significantly reduced sleep quality and quality of life (QOL). It also contributed to poor functioning and disturbances in mental and physical health [15]. In our study, total sleep time was notably reduced after night shifts compared to day shifts. Additionally, significant differences were observed in both total sleep time and sleep stage N2 (Table 2).
Arousal index: Arousal contributes to sleep fragmentation, which can impair cognitive function and trigger autonomic reflex activation, leading to elevated blood pressure and heart rate [16-19]. It is typically defined as a sudden shift in the electroencephalogram (EEG) to a higher frequency, such as alpha, theta, or beta waves, lasting at least 3 seconds and preceded by at least 10 seconds of stable sleep [20]. Our study observed a highly significant difference in the arousal index between pre- and post-night duty, indicating the impact of sleep disruption on arousal frequency.
Snoring index: Arousal is commonly observed in patients with obstructive sleep apnea (OSA), which is the leading cause of sleep disruption. OSA also increases the risk of conditions such as diabetes, hypertension, heart failure, and stroke, with severity often linked to the apnea-hypopnea index (AHI) [21,22]. Snoring is the most frequently reported symptom in individuals with OSA [23], with prevalence rates ranging from 20% to 40% [24]. Our study found a significant difference in the snoring index before and after night shifts.
Mental Health Implications: The mental health of night-duty security personnel is significantly affected by disrupted sleep patterns. Numerous studies have linked night shifts to higher rates of anxiety, depression, and stress [25]. For security personnel, these mental health issues can compromise their vigilance, decision-making, and overall job performance, increasing the risk of errors and accidents [26]. Meta-analysis on Pre-shift work factors, such as mental health, sleep quality, and job-related characteristics, were identified as key predictors of shift work tolerance (SWT) later in workers’ careers [27]. The study highlights that shift work negatively affects the sleep and mental health of new workers early on, underscoring the importance of implementing pre-shift work interventions to improve SWT and support overall health.
Occupational Health and Safety: The literature highlights the critical impact of sleep and mental health issues on job performance and safety among security personnel. Sleep-deprived individuals are more prone to errors, accidents, and decreased productivity, which can have severe implications for public safety [28]. The high-stress nature of security work requires constant alertness and quick decision-making, which are impaired by poor sleep and mental health. Therefore, addressing these issues is essential for both personal health and professional efficacy [29]. To combat these health hazards various preventive and promotive health measures like practice of various paths of Yoga, Yoganidra and meditation have to be implemented or practiced in night-duty personnels. Yoganidra provides ways to manage stress and anxiety and enhance mental wellness [30]. Yoga offers comprehensive solutions for reducing anxiety levels and improvising subjective feeling of well-being and managing health [31]. This ancient heritage of practice of Yoga is a vaccine for all the germless diseases.
Conclusion:
The reviewed literature and our study clearly demonstrate the detrimental impact of night-duty on sleep architecture, physiological parameters such as pulse pressure, blood pressure and mental well-being (cognitive functions) among security personnel. By addressing these issues through targeted research and interventions, we can improve the health and performance of security personnel, ensuring they remain effective in their critical roles. This study aims to provide the necessary evidence to develop and implement such interventions, ultimately enhancing both personal and public safety.
References:
- Sack RL, Auckley D, Auger RR, et al. Circadian rhythm sleep disorders: Part I, basic principles, shift work and jet lag disorders. Sleep. 2007;30(11):1460-1483. doi: https://doi.org/10.1093/sleep/30.11.1460
- Killgore WDS. Effects of sleep deprivation on cognition. In: Progress in Brain Research. Vol 185. Elsevier; 2010:105-129. https://doi.org/10.1016/B978-0-444-53702-7.00007-5
- Overtime and extended work shifts: recent findings on illnesses, injuries and health behaviors. 2004. U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health. https://doi.org/10.26616/NIOSHPUB2004143
- Åkerstedt T, Knutsson A, Westerholm P, et al. Sleep disturbances, work stress and work hours. J Psychosom Res. 2002;53(3):741-748. https://doi.org/10.1016/S0022-3999(02)00333-1
- Rajaratnam SM, Arendt J. Health in a 24-h society. Lancet. 2001;358(9286):999-1005. https://doi.org/10.1016/S0140-6736(01)06108-6
- Boivin DB, Boudreau P. Impacts of shift work on sleep and circadian rhythms. Pathol Biol. 2014;62(5):292-301. https://doi.org/10.1016/j.patbio.2014.08.001
- Czeisler CA, Gooley JJ. Sleep and circadian rhythms in humans. Cold Spring Harb Symp Quant Biol. 2007;72:579-597. https://doi.org/10.1101/sqb.2007.72.064
- Barger LK, Rajaratnam SMW, Wang W, et al. Common sleep disorders increase risk of motor vehicle crashes and adverse health outcomes in firefighters. J Clin Sleep Med. 2015;11(3):233-240. https://doi.org/10.5664/jcsm.4534
- Boivin DB, Boudreau P, Kosmadopoulos A. Disturbance of the circadian system in shift work and its health impact. J Biol Rhythms. 2022;37(1):3-28. https://doi.org/10.1177/07487304211064218
- Drake CL, Roehrs T, Richardson G, Walsh JK, Roth T. Shift work sleep disorder: Prevalence and consequences beyond that of symptomatic day workers. Sleep. 2004;27(8):1453-1462. https://doi.org/10.1093/sleep/27.8.1453
- Liu Y, Wheaton AG, Chapman DP, Cunningham TJ, Lu H, Croft JB. Prevalence of healthy sleep duration among adults—United States, 2014. MMWR Morb Mortal Wkly Rep. 2016;65(6):137-141. https://doi.org/10.15585/mmwr.mm6506a1
- Hussain M, Tyagi R. Effect of shift work on physiological parameters: A study among security personnel. Natl J Physiol Pharm Pharmacol. 2019;9(1). https://doi.org/10.5455/njppp.2019.9.09294221 12018
- Makarem N, Alcántara C, Williams N, Bello NA, Abdalla M. Effect of sleep disturbances on blood pressure. Hypertension. 2021;77(4):1036-1046. https://doi.org/10.1161/HYPERTENSIONAHA.120.14479
- Pilcher JJ, Huffcutt AI. Effects of sleep deprivation on performance: A meta-analysis. Sleep. 1996;19(4):318-326. https://doi.org/10.1093/sleep/19.4.318
- Vidya S, Patlolla VP, Kamuju N, Ampalam P, Kalyan N, Vasupalli KVS. Impact of shift work on sleep and quality of life in industrial workers: A cross-sectional study. Arch Ment Health. 2019;20(1):45. https://doi.org/10.4103/AMH.AMH_3_19
- Horner RL. Emerging principles and neural substrates underlying tonic sleep-state-dependent influences on respiratory motor activity. Philos Trans R Soc Lond B Biol Sci. 2009;364(1529):2553-2564. https://doi.org/10.1098/rstb.2009.0065
- Sforza E, Gaudreau H, Petit D, Montplaisir J. Homeostatic sleep regulation in patients with idiopathic hypersomnia. Clin Neurophysiol. 2000;111(2):277-282. https://doi.org/10.1016/S1388-2457(99)00242-4
- Engleman HM. Sleepiness, cognitive function, and quality of life in obstructive sleep apnoea/hypopnoea syndrome. Thorax. 2004;59(7):618-622. https://doi.org/10.1136/thx.2003.015867
- Trinder J, Kleiman J, Carrington M, et al. Autonomic activity during human sleep as a function of time and sleep stage. J Sleep Res. 2001;10(4):253-264. https://doi.org/10.1046/j.1365-2869.2001.00263.x
- Berry RB, Budhiraja R, Gottlieb DJ, et al. Rules for scoring respiratory events in sleep: Update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. J Clin Sleep Med. 2012;8(5):597-619. https://doi.org/10.5664/jcsm.2172
- Valham F, Sahlin C, Stenlund H, Franklin KA. Ambient temperature and obstructive sleep apnea: Effects on sleep, sleep apnea, and morning alertness. Sleep. 2012;35(4):513-517. https://doi.org/10.5665/sleep.1736
- Arzt M, Young T, Finn L, Skatrud JB, Bradley TD. Association of sleep-disordered breathing and the occurrence of stroke. Am J Respir Crit Care Med. 2005;172(11):1447-1451. https://doi.org/10.1164/rccm.200505-702OC
- Rundo JV. Obstructive sleep apnea basics. Cleve Clin J Med. 2019;86(1 Suppl 1):2-9. https://doi.org/10.3949/ccjm.86.s1.02
- Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med. 1993;328(17):1230-1235. https://doi.org/10.1056/NEJM199304293281704
- Wright KP, Bogan RK, Wyatt JK. Shift work and the assessment and management of shift work disorder (SWD). Sleep Med Rev. 2013;17(1):41-54. https://doi.org/10.1016/j.smrv.2012.02.002
- Scott LD, Arslanian-Engoren C, Engoren MC. Association of sleep and fatigue with decision regret among critical care nurses. Am J Crit Care. 2014;23(1):13-23. https://doi.org/10.4037/ajcc2014191
- Harris R, Kavaliotis E, Drummond SPA, Wolkow AP. Sleep, mental health and physical health in new shift workers transitioning to shift work: Systematic review and meta-analysis. Sleep Med Rev. 2024;75:101927. https://doi.org/10.1016/j.smrv.2024.101927
- Williamson AM, Feyer AM. Moderate sleep deprivation produces impairments in cognitive and motor performance equivalent to legally prescribed levels of alcohol intoxication. Occup Environ Med. 2000;57(10):649-655. https://doi.org/10.1136/oem.57.10.649
- Lockley SW, Barger LK, Ayas NT, et al. Effects of health care provider work hours and sleep deprivation on safety and performance. Jt Comm J Qual Patient Saf. 2007;33(11 Suppl):7-18. https://doi.org/10.1016/S1553-7250(07)33109-7
- Kamble P, Daulatabad VS, Tandra H, Singhal A, U M, John NA. Yoganidra to Alleviate Anxiety: An Interventional Study. Cureus. 2023;15(9):e45083. Published 2023 Sep 12. https://doi.org/10.7759/cureus.45083
- Daulatabad V S, Rukadikar C, Kamble P, Role of Yoga in relieving anxiety in MBBS Students. Indian J Clin Anat Physiol 2019;6(3):335-337 https://doi.org/10.18231/j.ijcap.2019.073

