Management of Gingival Recession: A Case Study
Management of Gingival Recession and Tooth Sensitivity: A Case Study
Ahmad Soolari, DMD, MS*1, Lourdes Sanchez, DDS2, Sahar Safi, BS, CDRT3
- Soolari Dentistry, 11251 Lockwood Drive, Silver Spring, MD 20902, USA; Diplomate of the American Board of Periodontology, Former faculty at the New York University and the University of Maryland, USA; Specialty Practice in the Silver Spring, and Potomac area of Montgomery County, Maryland, USA
www.soolaridentistry.com - Private Practice in the Silver Spring of Maryland, USA
- Certified Dental Radiation technologist at the Soolari Dentistry, 11251 Lockwood Drive, Silver Spring, MD 20902, USA
OPEN ACCESS
PUBLISHED: 30 September 2025
CITATION: Soolari, A., Sanchez, L., Safi, S., 2025. Management of Gingival Recession and Tooth Sensitivity: A Case Study. Medical Research Archives, [online] 13(9).
https://doi.org/10.18103/mra.v13i9.6909
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i9.6909
ISSN 2375-1924
ABSTRACT
This case report details a comprehensive, interdisciplinary approach for managing localized gingival recession and dentin hypersensitivity in a 44-year-old female patient. A thorough clinical evaluation revealed the primary etiology to be a combination of a thin gingival biotype, aggressive toothbrushing, and occlusal trauma. The multi-phased treatment plan included initial non-surgical periodontal therapy, occlusal adjustment, and the fabrication of an occlusal guard, followed by mucogingival surgery using a subepithelial connective tissue graft. The successful outcome, which involved a significant increase in attached gingiva, resolution of hypersensitivity, and improved esthetics, highlights the importance of addressing all contributing factors to achieve predictable, long-term results.
Keywords: gingival recession, dentin hypersensitivity, periodontal therapy, mucogingival surgery, connective tissue graft
Introduction
Gingival recession (GR), characterized by the apical migration of the gingival margin, can lead to root surface exposure, causing dentin hypersensitivity, esthetic concerns, and increased susceptibility to dental caries. The prevalence of GR is significant, with one study reporting it at 23.88%, observed more in males, and most frequently affecting the lower anterior teeth.¹ The etiology of GR is multifactorial and includes a combination of anatomical, iatrogenic, and pathological factors. Anatomical factors include a thin gingival biotype, prominent tooth position, aberrant frenal attachments, and shallow vestibules. Iatrogenic factors often involve aggressive toothbrushing or restorative margin placement, while occlusal trauma and malocclusion can also contribute by inducing excessive forces on the teeth.² The management of GR requires a comprehensive, staged approach that first addresses the underlying etiological factors before surgically restoring lost tissue. A thorough clinical evaluation, including an assessment of the gingival biotype, keratinized tissue width, frenal attachments, vestibular depth, and occlusal relationships, is essential for a tailored treatment plan. Initial non-surgical therapy, such as oral hygiene instructions and scaling and root planing, is crucial for eliminating inflammation and promoting periodontal health. Occlusal adjustment and the use of occlusal guards may also be necessary to eliminate excessive forces on the affected teeth.3 Surgical interventions, such as coronally advanced flaps, subepithelial connective tissue grafts, and guided tissue regeneration, are employed to increase the width of keratinized tissue and cover exposed root surfaces. Subepithelial connective tissue grafts, harvested from a donor site, are considered the gold standard for root coverage due to their predictable outcomes and long-term stability.4 The choice of surgical technique depends on the specific characteristics of the defect and the patient’s esthetic expectations.5 This case report details a comprehensive, interdisciplinary approach to managing localized gingival recession and dentin hypersensitivity in a patient with multiple contributing factors.
Case Presentation
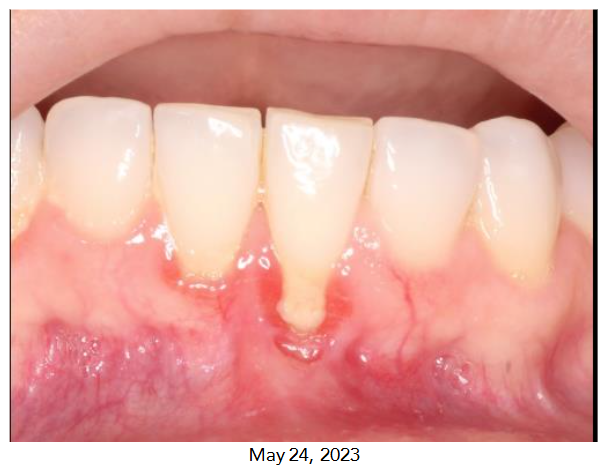
A 44-year-old female presented to our dental office with a chief complaint of hypersensitivity in her lower anterior teeth, specifically tooth #24. Clinical examination revealed a Miller Class I gingival recession on the facial aspect of tooth #24. This was accompanied by a thin gingival biotype, a lack of attached keratinized gingiva, a prominent frenal pull, and a shallow vestibule. The patient’s medical history was unremarkable, but she reported a history of previous orthodontic treatment and acknowledged a habit of aggressive toothbrushing. Occlusal analysis showed signs of occlusal disharmony, with evidence of excessive occlusal forces on the lower anterior teeth. The patient expressed concerns regarding the progressive nature of the recession and its impact on her esthetics. A diagnosis of gingival recession on tooth #24, complicated by mucogingival deficiency, frenal pull, and occlusal trauma, was established. The primary etiology was attributed to a combination of a thin gingival biotype, aggressive toothbrushing, prior orthodontic treatment, and occlusal trauma.
Treatment planning
The treatment plan for this patient was designed to address the underlying etiological factors, alleviate dentin hypersensitivity, and restore periodontal support and esthetics. The proposed, comprehensive treatment sequence included a multi-step approach:
- Initial Periodontal Therapy and Oral Hygiene Instructions: To eliminate plaque, calculus, and inflammation.
- Occlusal Adjustment: To eliminate occlusal interferences and redistribute occlusal forces.
- Frenectomy and Gingival Grafting: To address the prominent frenum and restore mucogingival tissue.
- Fabrication of an Occlusal Guard: To protect the dentition from bruxism and related occlusal trauma.
The rationale, benefits, risks, and alternatives of each treatment option were thoroughly discussed with the patient, and informed consent was obtained.
Clinical Procedures
INITIAL PERIODONTAL THERAPY AND OCCLUSAL ADJUSTMENT
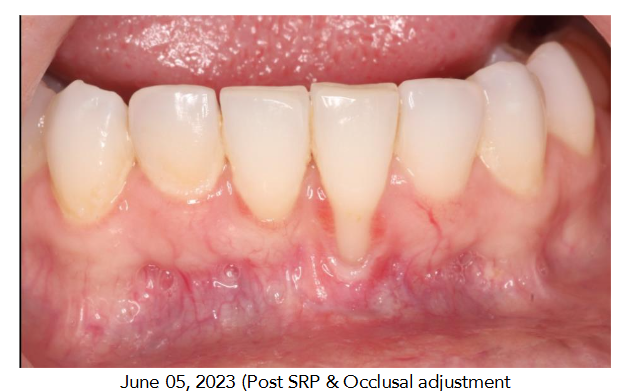
The patient received comprehensive oral hygiene instructions, including the proper use of a soft-bristled toothbrush and interdental cleaning aids. Scaling and root planing were performed to remove plaque and calculus. Occlusal adjustment was carried out to eliminate interferences and achieve a more harmonious occlusal relationship. The patient was advised to maintain meticulous oral hygiene throughout the treatment.
FRENECTOMY AND GINGIVAL GRAFTING
A frenectomy was performed to release the prominent frenal pull. A subepithelial connective tissue graft, harvested from the palate, was then carefully placed over the exposed root surface of tooth #24. The graft was secured with non-resorbable sutures. Postoperative instructions were provided, including the use of an antiseptic mouthwash and avoidance of strenuous physical activity. Sutures were removed after two weeks, and the surgical site was evaluated for initial healing and graft integration.
FABRICATION OF AN OCCLUSAL GUARD
Impressions of both the maxillary and mandibular arches were taken to create study models. These models were mounted on a semi-adjustable articulator, and a custom occlusal guard was fabricated. The guard was designed to protect the teeth from the effects of bruxism and reduce stress on the periodontal ligament. The final appliance was delivered and adjusted to ensure proper fit, and the patient was instructed on its nightly use and maintenance.
POSTOPERATIVE CARE AND MAINTENANCE
The patient was placed on a periodontal maintenance program with regular recall appointments. During these visits, oral hygiene was reinforced, and the stability of the grafted tissue was monitored. The patient reported a significant reduction in dentin hypersensitivity and satisfaction with improved esthetics.
Discussion
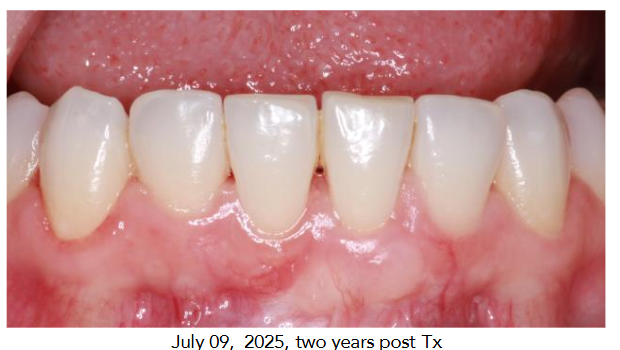
The successful outcome in this case underscores the need for a comprehensive, multi-phase approach to managing gingival recession. The primary objective was not just to cover the root surface, but to address all contributing factors to ensure long-term stability and success.6 Simply placing a restorative material, such as composite, would not have corrected the “roller coaster” tissue profile or provided the long-term stability offered by a surgical graft. A surgical approach was chosen because gingival augmentation is a highly predictable procedure for not only improving esthetics but also for facilitating home care, resisting trauma, and preventing root caries.7 This case report also demonstrates the benefits of an interdisciplinary approach. The referral and collaboration between the patient’s referring dentist and the periodontist were crucial in achieving this result. The successful management of the patient’s dentin hypersensitivity, combined with the significant increase in tissue height and deepening of the vestibule, highlights the value of a tailored treatment plan.8 At a two-year follow-up, the patient’s result showed a 6 mm increase in tissue height, which illustrates the long-term predictability of a subepithelial connective tissue graft. The patient reported high satisfaction with the final esthetic and functional outcome.
Conclusion
The successful treatment of this case demonstrates that a comprehensive, interdisciplinary approach is essential for managing complex cases of gingival recession.9 By addressing all underlying etiological factors, including occlusal trauma and a prominent frenum, and utilizing a subepithelial connective tissue graft, a predictable and long-lasting esthetic and functional outcome was achieved.10 This case highlights why a team-based approach, combining initial therapy with surgical intervention, offers the best chance for patient satisfaction and positive clinical results.
Conflict of Interest Statement: None.
Funding Statement: None.
Acknowledgements: None.
References
- Sarhan S, Ahmed E, Hussein R, Abou-Bakr A. Prevalence, etiology and clinical characteristics of gingival recession in a sample of adult Egyptian dental patients: a cross sectional study. BMC Oral Health. 2025;25(1):691.
- Mythri S, Arunkumar SM, Hegde S, et al. Etiology and occurrence of gingival recession – An epidemiological study. J Indian Soc Periodontol. 2015;19(6):671-675.
- Marshner F, et al. Systematic review and meta-analysis on prevalence and risk factors for gingival recession. J Dent. 2025;155:105645.
- Augusto M, Salman, MA and Choi D, Schincaglia GP. Root coverage predictability in the treatment of gingival recessions on mandibular anterior teeth. Res. 2022 Jul; 7(3);224-233.
- Salam TAA, et al. Assessment of Patients’ Experience and Perception Toward Dentinal Hypersensitivity for Its Diagnosis and Management: A Cross-Sectional Study. Cureus. 2023;15(2):e35214.
- Ckaudia Carbone A, Cesar Joly J, et al. Long-term stability of gingival margin and periodontal soft-tissue phenotype achieved after mucogingival therapy: A systematic review. J Clin Periodontol. 2023;50(12):1676-1704.
- Pihlstrom BL. Periodontal Risk Assessment, Diagnosis and Treatment Planning. Periodontol 2000. 2001;25:37-58.
- Dong Ta Q, et al. Modified multiple papilla full flap combined with tunneling and de-epithelialized gingival graft to manage severe gingival recession in mandibular incisors: literature review and case report. J Surg Case Rep. 2024;2024(8):rjae479.
- Soolari A, Shahami S. Periodontal plastic surgery in the esthetic zone. Inside Dentistry. 2015;11(7):54-59.
- Lahham C, Kharroubi R, AbuQubi B, et al. A novel approach to managing gingival recession in protruded roots: a case report. J Surg Case Rep. 2025;2025(2):rjaf044.

