Prostate Cancer Prevention: Managing Occult Prostatitis
A Novel Prostate Cancer Prevention Strategy: Prevention and Management of Occult Prostatitis
Akbar Khan, MD, IMD, DHS, FAAO¹; Douglas Andrews, BSc, ND¹; Humaira Khan, MBBS, MCPS, MHSc¹
- Medicor Cancer Centres, 4576 Yonge Str., Suite 301, Toronto, ON, Canada, M2N 6N4
OPEN ACCESS
PUBLISHED: 31 October 2024
CITATION: Khan, A., Andrews, D., et al., 2024. A Novel Prostate Cancer Prevention Strategy: Prevention and Management of Occult Prostatitis. Medical Research Archives, [online] 12(10).
https://doi.org/10.18103/mra.v12i10.5804
COPYRIGHT: © 2024 European Society of Medicine. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v12i10.5804
ISSN 2375-1924
Abstract
Prostate cancer is a significant public health concern. Worldwide incidence data from 2020 indicates approximately 1.4 million new cases diagnosed annually, and mortality data indicates over 375,000 annual deaths. Trends indicate increasing incidence and mortality. Clearly, improved prostate cancer prevention, early detection and treatment are needed. Better primary prostate cancer prevention is the most crucial. Occult infections have been implicated in many different chronic diseases. Due to this relationship between chronic disease and chronic infection, the authors have been promoting advanced screening for chronic occult infections using DNA amplification/detection methods such as Polymerase Chain Reaction (PCR) for over 5 years. After conducting over 100 PCR-based infection tests in clinic patients, the authors have observed a very strong correlation between patients with known prostate cancer and the presence of pathogens associated with chronic prostatitis. Published literature confirms that the same relationship has also been noted by others. It is accepted that one etiology of cancer is chronic infection, e.g. Helicobacter pylori can cause gastric carcinoma. Although evidence exists that relates chronic prostate infection to development of prostate cancer, a causative relationship is not currently widely accepted. Given the current evidence, the straightforward prevention strategies derived from it, and the significant potential benefits, it is essential to urgently reassess the prevailing perspectives on prostatitis and prostate cancer. Novel primary and secondary prostate cancer prevention strategies are proposed based on prevention, diagnosis and treatment of chronic prostatitis.
Keywords:
- prostate cancer
- chronic prostatitis
- occult infection
- cancer prevention
Introduction
According to data from 174 countries from the World Health Organization’s Global Cancer Observatory (GLOBOCAN) 2020 database, there are approximately 1.4 million cases of prostate cancer diagnosed annually and over 375,000 annual deaths from prostate cancer. Both incidence and mortality are steadily increasing. Chronic diseases, including cancer, are a tremendous burden to the public and to health care systems. USA data from 2014 notes that 60% of adult Americans had at least one chronic disease or condition, and 42% had multiple diseases. Chronic diseases have a profoundly negative effect on quality of life for patients and their families. Chronic diseases are also the leading drivers of health care costs. Although effective preventive strategies exist for many chronic diseases, they remain significantly underutilized.
The incidence, mortality, public burden and healthcare costs of prostate cancer create a pressing need for improved prevention and management, and methods to ensure acceptance and uptake of those strategies. Enhanced primary prostate cancer prevention is perhaps the most crucial, since primary prevention is considered the best disease management strategy.
The current state of prostate cancer prevention is primarily focused on secondary prevention (also known as early detection). Digital rectal exam, measurement of blood level of prostate-specific antigen (PSA) or prostate imaging (ultrasound, computerized tomography or magnetic resonance imaging) may be used for secondary prevention, but there is disagreement about these modalities. Rectal examination can miss anterior prostatic tumors. False positives are common with PSA testing and can result in unnecessary biopsies, which are invasive and carry a risk of infection. Ultrasound, computerized tomography and MRI are costly. Computerized tomography (CT) screening also carries some risk associated with repeated radiation exposure. Lifestyle-based primary prevention methods, such as diet, physical activity, moderation of alcohol consumption, limiting toxin exposure and stress management are always relevant. However, they are often underutilized in busy doctors’ offices, since discussion of these topics is time-consuming and may not be adequately renumerated in certain funding models. Novel primary prevention strategies are desperately needed which are simple, cost effective and non-invasive. Screening for chronic prostate infection using the advanced DNA-based pathogen identification tests like Polymerase Chain Reaction (PCR) or Next Generation Sequencing (NGS) has the potential to fill this void.
Chronic Infections and Etiology of Cancer
Chronic infections (occult or apparent) have been implicated in many different chronic diseases including autoimmune, neuro-degenerative and cardiovascular. It is well-known that chronic infections also cause cancer, partly because of the resulting chronic inflammation.
| Infection | Associated Cancer(s) |
|---|---|
| Human Papillomavirus (HPV) | Cervical cancer, anal cancer, oropharyngeal cancer, penile cancer, vulvar cancer |
| Hepatitis B Virus (HBV) | Liver cancer (hepatocellular carcinoma) |
| Hepatitis C Virus (HCV) | Liver cancer (hepatocellular carcinoma), non-Hodgkin lymphoma |
| Epstein-Barr Virus (EBV) | Burkitt lymphoma, Hodgkin lymphoma, nasopharyngeal carcinoma, gastric cancer |
| Helicobacter pylori | Stomach cancer (gastric cancer), MALT lymphoma |
| Human T-cell Leukemia Virus-1 (HTLV-1) | Adult T-cell leukemia/lymphoma |
| Kaposi’s Sarcoma-associated Herpesvirus (KSHV) | Kaposi’s sarcoma, primary effusion lymphoma, Castleman disease |
| Schistosoma haematobium | Bladder cancer |
Evidence exists that also relates chronic infections to other cancers. For example, fungal infections are implicated in skin cancer, viral infections in breast cancer, atypical bacterial infections in lung cancer and cytomegalovirus infection in glioblastoma multiforme. Still, it is not generally accepted that most other cancers have infectious etiologies. For prostate cancer, there is evidence correlating this diagnosis with chronic infectious prostatitis.
Potential Infectious Etiology of Prostate Cancer
Due to the relationship between multiple chronic diseases (including cancer) and chronic infections, the authors have been promoting highly sensitive and specific screening for chronic infections as part of their wellness and cancer prevention programs. Established DNA amplification/detection such as polymerase chain reaction (PCR) for blood or urine testing has been used in their clinic over 5 years.
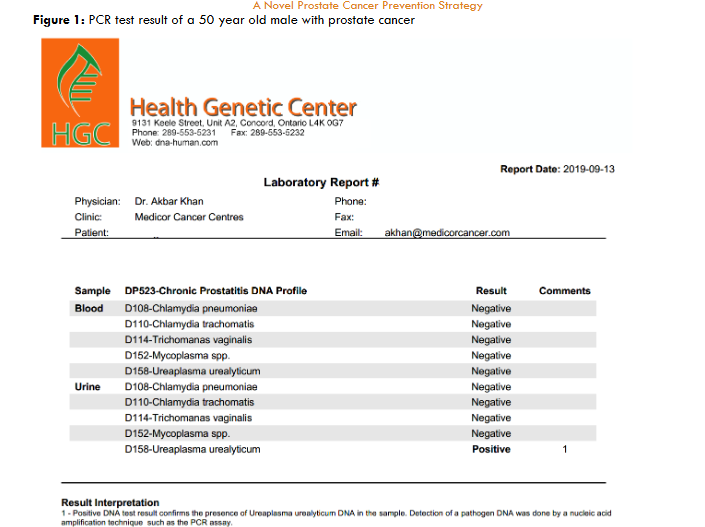
The authors have observed a striking correlation between patients with biopsy-proven prostate cancer and the presence of previously undetected pathogens associated with chronic prostatitis. In other words, virtually 100% of patient with prostate cancer who were tested for common pathogens known to cause prostatitis were found to be positive for one or more such pathogens. Typical pathogens found were mycoplasma species, ureaplasma urealyticum, chlamydia species and trichomonas. This simple observation led the authors to examine the literature to see if others have also noted similar findings. In fact, published literature confirms that this relationship has been noted by other scientists. Interestingly, most of the patients in the authors’ practice were asymptomatic (no prostatitis diagnosis) prior to the cancer diagnosis.
Chronic prostatitis is a common problem, estimated to affect 9 – 14% of men worldwide. A lack of symptoms in men with chronic prostatitis is also common. For example, in a study of 71 infertile men, asymptomatic chlamydial prostatitis was found in 51%. In another study, C. acnes was found to be significantly more common in prostate cancer tissue samples and hypothesized to trigger chronic inflammation. In regions where prostatic infections are left untreated, mortality from prostate cancer can be twice as high as world rates. There are also studies that show a low correlation between infectious agents and prostatitis. Such studies are seriously limited by the low sensitivity of their diagnostic methods (e.g. antimicrobial culture compared to PCR or NGS can easily miss atypical organisms that are difficult to culture). The diversity of findings among studies highlights the challenges and complexities in establishing a microbial link to prostate cancer. Since correlation of prostate infection with prostate cancer does not prove causation, a closer look at the existing evidence is needed.
SEXUALLY TRANSMITTED PATHOGENS CAUSE REPRODUCTIVE CANCERS
Evidence currently supports the concept of infections (mostly sexually transmitted) as etiologic agents in various reproductive cancers. Perhaps the most well-accepted is HPV which is a known cause of penile, cervical, vaginal and vulvar cancers. Chronic infectious prostatitis is also primarily caused by sexually transmitted pathogens. These include neisseria gonorrhoea, chlamydia species, ureaplasma urealyticum and mycoplasma species.
CHRONIC INFLAMMATION CAUSES CANCER
Acute inflammation is a normal mechanism for the body to address tissue damage or infection. In simple terms, acute inflammation is a process whereby immune cells such as macrophages and neutrophils migrate to the area of infection or injury, release chemicals like chemokines and cytokines, and assist in overcoming the damaging factors, leading to recovery. Acute inflammation is clinically manifested by redness, heat, swelling, pain and loss of function. One cause of chronic inflammation is the presence of infectious agents that the body cannot remove due to weakened immunity. Chronic inflammation can become a pathological process leading to ongoing tissue damage, fibrosis and even cancer. Chronic inflammation can contribute to cancer formation and progression by several mechanisms such as immune suppression, tissue remodeling, DNA damage, and promotion of cell proliferation.
Chronic inflammation is a prominent feature of chronic prostatitis. Since mechanisms explaining how chronic inflammation may lead to cancer are known (as indicated), this strengthens the notion that chronic prostatitis leads to prostate cancer. In addition to chronic inflammation, there are many other known etiologies of cancer (for example, genetics, toxin exposure, radiation exposure, smoking). These factors have been extensively addressed by others.
Limitations of Analysis Asserting Causation
Based on the existing science as noted above, it is possible to draw a logical conclusion that chronic prostatitis likely is an etiologic factor in the formation of prostate cancer. This does not provide conclusive proof, however. An ideal study to prove this concept would be a large multicenter prospective case-control trial spanning several decades in which 2 groups of men are monitored: one group with known asymptomatic prostatitis established by advanced testing such as PCR or Next Generation Sequencing (“NGS”), and one group with a proven absence of prostatitis. The incidence of prostate cancer in both groups could then be compared. To the authors’ knowledge, no such trial exists. Such a trial could also be considered unethical (to monitor chronic prostatitis for decades without treating it). The cost of such a trial would be high, and there would be many confounding factors such as genetic, immune and environmental variables that are difficult to account for. As a result of these virtually insurmountable issues, it is proposed that the current degree of evidence and logical conclusions be put into practice for prostate cancer prevention without delay. The argument to do so is based on the following:
- Prostate cancer is a prevalent condition with serious public health implications.
- A prevention strategy based on the existing evidence is simple.
- A prevention strategy based on the existing evidence is cost-effective.
- A prevention strategy based on the existing evidence is safe.
- The potential benefits are profound (reduced cancer incidence), and the harms are minimal.
Proposed Novel Primary and Secondary Prevention of Prostate Cancer
A simple, safe and cost-effective primary prevention based on the nature of chronic prostatitis being primarily sexually transmitted is recommended. This includes discouraging casual sexual activity with multiple partners and promoting steady relationships. In cultures where casual sexual activity is common, education with a goal to modify cultural norms should be considered. Encouraging the use of barrier methods for sexually transmitted infection (STI) prevention could be encouraged as a harm reduction strategy. The message that prevention of STIs can prevent prostate cancer is important to disseminate. This concept starkly contrasts with existing mainstream thinking which the authors feel is decidedly outdated, i.e. that chronic prostatitis cannot be prevented.
For secondary prevention, it is proposed that all men who have a sexual history of multiple casual partners be offered education and screening for chronic prostatitis with PCR or NGS testing of urine or semen samples. All cases of asymptomatic prostatitis that are diagnosed should be treated with appropriate antimicrobial therapy. For practitioners who prefer a non-stigmatizing approach, annual screening could be offered to all men regardless of sexual history.
| Criteria | Suggested Prevention |
|---|---|
| History of casual sexual contacts / multiple partners | PCR/NGS infection screening of urine/semen samples and treatment as needed |
| Ongoing casual sexual contacts / multiple partners | Education, Sexual Behavior Change, Barrier STI Prevention, Annual PCR/NGS infection screening of urine/semen samples and treatment as needed |
* labs such as MicroGen Diagnostics in USA https://microgendx.com/ and Health Genetic Center in Canada https://dnamelab.com/
Conclusions
Although prostatitis as an etiology of prostate cancer is not proven, there is meaningful evidence which allows a logical scientific conclusion to be drawn. Since a proper clinical study which could prove or disprove this question would be prolonged, extremely costly and virtually impossible to conduct, this may be the best evidence available. It is up to the medical community to decide whether prostate cancer is a serious enough problem that deserves immediate action, including PCR / NGS prostatitis screening, treatment and public education about sexual behavior.
Future Directions
Eradication of chronic prostate infection can be difficult, since conventional therapy typically relies on antimicrobial drug therapy alone and does not factor in immune insufficiency. Research on the use of integrative therapies is warranted since there is evidence that they can address weak immunity in addition to providing antimicrobial action, with minimal or no side effects. Such strategies include diet changes, medical ozone therapy, silver nanoparticle therapy, mushroom supplements, high dose vitamin D and low dose naltrexone.
Grants or Financial Support:
None
Institutional Review Board Statement:
Not applicable
Conflict of Interest Declaration
- The authors have a financial interest in providing diagnostics and treatments for chronic prostatitis.
- The authors have no financial interest in the infection testing laboratories listed in this publication.
References
- Wang L, Lu B, He M, Wang Y, Wang Z, Du L. Prostate Cancer Incidence and Mortality: Global Status and Temporal Trends in 89 Countries From 2000 to 2019. Front Public Health. 2022;10:811044. Published 2022 Feb 16. doi:10.3389/fpubh.2022.811044
- Levine S, Malone E, Lekiachvili A, Briss P. Health Care Industry Insights: Why the Use of Preventive Services Is Still Low. Prev Chronic Dis 2019;16:180625. DOI: http://dx.doi.org/10.5888/pcd16.180625
- Kisling LA, Das JM. Prevention Strategies. [Updated 2023 Aug 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan. https://www.ncbi.nlm.nih.gov/books/NBK537222/. Accessed October 3, 2024
- Prabhakaran VM. Early detection of prostate cancer. Role of prostate-specific antigen. Can Fam Physician. 1996;42:709-712.
- Mahmoudi G, Toolee H, Maskani R, Jokar F, Mokfi M, Hosseinzadeh A. COVID-19 and cancer risk arising from ionizing radiation exposure through CT scans: a cross-sectional study. BMC Cancer. 2024;24(1):298. Published 2024 Mar 5. doi:10.1186/s12885-024-12050-x
- Marino P, Mininni M, Deiana G, et al. Healthy Lifestyle and Cancer Risk: Modifiable Risk Factors to Prevent Cancer. Nutrients. 2024;16(6):800. Published 2024 Mar 11. doi:10.3390/nu16060800
- Ozkardes C, Harman JS. Physician Compensation Method Effects on Preventive Service Delivery. J Gen Intern Med. 2022;37(2):480-481. doi:10.1007/s11606-020-06580-w
- Consortium OPATHY, Gabaldón T. Recent trends in molecular diagnostics of yeast infections: from PCR to NGS. FEMS Microbiol Rev. 2019;43(5):517-547. doi:10.1093/femsre/fuz015
- Turizo-Smith AD, Córdoba-Hernandez S, Mejía-Guarnizo LV, Monroy-Camacho PS, Rodríguez-García JA. Inflammation and cancer: friend or foe? Front Pharmacol. 2024;15:1385479. Published 2024 May 10. doi:10.3389/fphar.2024.1385479
- National Cancer Institute. Cancer Causes and Prevention: Infectious Agents. https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents. Accessed September 9, 2024.
- Hosseini K, Ahangari H, Chapeland-Leclerc F, Ruprich-Robert G, Tarhriz V, Dilmaghani A. Role of Fungal Infections in Carcinogenesis and Cancer Development: A Literature Review. Adv Pharm Bull. 2022;12(4):747-756. doi:10.34172/apb.2022.076
- Horakova D, Bouchalova K, Cwiertka K, Stepanek L, Vlckova J, Kollarova H. Risks and protective factors for triple negative breast cancer with a focus on micronutrients and infections. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2018;162(2):83-89. doi:10.5507/bp.2018.014
- Budisan L, Zanoaga O, Braicu C, et al. Links between Infections, Lung Cancer, and the Immune System. Int J Mol Sci. 2021;22(17):9394. Published 2021 Aug 30. doi:10.3390/ijms22179394
- Rahman M, Dastmalchi F, Karachi A, Mitchell D. The role of CMV in glioblastoma and implications for immunotherapeutic strategies. Oncoimmunology. 2018;8(1):e1514921. Published 2018 Oct 16. doi:10.1080/2162402X.2018.1514921
- Oseni SO, Naar C, Pavlović M, et al. The Molecular Basis and Clinical Consequences of Chronic Inflammation in Prostatic Diseases: Prostatitis, Benign Prostatic Hyperplasia, and Prostate Cancer. Cancers (Basel). 2023;15(12):3110. Published 2023 Jun 8. doi:10.3390/cancers15123110
- Boutin S, Weitnauer M, Hassel S, et al. One time quantitative PCR detection of Pseudomonas aeruginosa to discriminate intermittent from chronic infection in cystic fibrosis. J Cyst Fibros. 2018;17(3):348-355. doi:10.1016/j.jcf.2017.12.007
- Khalvati Fahlyani B, Behzad-Behbahani A, Taghavi SA, et al. Development of an In-House TaqMan Real Time RT-PCR Assay to Quantify Hepatitis C Virus RNA in Serum and Peripheral Blood Mononuclear Cells in Patients With Chronic Hepatitis C Virus Infection. Hepat Mon. 2015;15(8):e28895. Published 2015 Aug 31. doi:10.5812/hepatmon.28895
- Iffland A, Zechel M, Lewejohann JC, et al. Experience with PCR Testing for Enteric Bacteria and Viruses of Emergency Department Patients with Acute Gastroenteritis: Are There Implications for the Early Treatment of Clostridioides difficile Infection?. Antibiotics (Basel). 2024;13(3):243. Published 2024 Mar 6. doi:10.3390/antibiotics13030243
- Albert E, Alberola J, Bosque M, et al. Missing Cases of Herpes Simplex Virus (HSV) Infection of the Central Nervous System When the Reller Criteria Are Applied for HSV PCR Testing: a Multicenter Study. J Clin Microbiol. 2019;57(2):e01719-18. Published 2019 Jan 30. doi:10.1128/JCM.01719-18
- Perletti G, Monti E, Magri V, et al. The association between prostatitis and prostate cancer. Systematic review and meta-analysis. Arch Ital Urol Androl. 2017;89(4):259-265. Published 2017 Dec 31. doi:10.4081/aiua.2017.4.259
- Zhang L, Wang Y, Qin Z, et al. Correlation between Prostatitis, Benign Prostatic Hyperplasia and Prostate Cancer: A systematic review and Meta-analysis. J Cancer. 2020;11(1):177-189. Published 2020 Jan 1. doi:10.7150/jca.37235
- Shoskes DA. Use of antibiotics in chronic prostatitis syndromes. Can J Urol. 2001;8 Suppl 1:24-28.
- Suominen J, Grönroos M, Terho P, Wichmann L. Chronic prostatitis, chlamydia trachomatis and infertility. Int J Androl. 1983;6(5):405-413. doi:10.1111/j.1365-2605.1983.tb00555.x
- Davidsson S, Carlsson J, Mölling P, et al. Prevalence of Flp Pili-Encoding Plasmids in Cutibacterium acnes Isolates Obtained from Prostatic Tissue. Front Microbiol. 2017;8:2241. Published 2017 Nov 16. doi:10.3389/fmicb.2017.02241
- Abdul-Nasir S, Lee H, Rahman MH, Bajgai J, Lee K-J, Kim C-S, Kim S-K. Unveiling the Dual Threat: How Microbial Infections and Healthcare Deficiencies Fuel Cervical and Prostate Cancer Deaths in Africa. Pathogens. 2024; 13(3):243. https://doi.org/10.3390/pathogens13030243
- Schaeffer AJ, Knauss JS, Landis JR, et al. Leukocyte and bacterial counts do not correlate with severity of symptoms in men with chronic prostatitis: the National Institutes of Health Chronic Prostatitis Cohort Study. J Urol. 2002;168(3):1048-1053. doi:10.1016/S0022-5347(05)64572-7
- Weidner W, Brunner H, Krause W. Quantitative culture of ureaplasma urealyticum in patients with chronic prostatitis or prostatosis. J Urol. 1980;124(5):622-625. doi:10.1016/s0022-5347(17)55586-x
- Cao W, Liu L, Tong MH. Hunan Yi Ke Da Xue Xue Bao. 2003;28(2):177-179.
- Kádár A, Bucsek M, Kardos M, Corradi G. Chlamydia trachomatis kimutatása in situ hibridizációval krónikus prostatitisben (metodikai elözetes közlemény) [Detection of Chlamydia trachomatis in chronic prostatitis by in situ hybridization (preliminary methodical report)]. Orv Hetil. 1995;136(13):659-662.
- Brunner H, Weidner W, Schiefer HG. Quantitative studies on the role of Ureaplasma urealyticum in non-gonococcal urethritis and chronic prostatitis. Yale J Biol Med. 1983;56(5-6):545-550.
- Krieger JN, Riley DE. Prostatitis: what is the role of infection. Int J Antimicrob Agents. 2002;19(6):475-479. doi:10.1016/s0924-8579(02)00086-9
- Nigam M, Mishra AP, Deb VK, et al. Evaluation of the association of chronic inflammation and cancer: Insights and implications. Biomed Pharmacother. 2023;164:115015. doi:10.1016/j.biopha.2023.115015
- Hannoodee S, Nasuruddin DN. Acute Inflammatory Response. [Updated 2024 Jun 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan. https://www.ncbi.nlm.nih.gov/books/NBK556083/. Accessed September 9, 2024
- Wu J, Lv X, Zhu S, Li T, Cheng H, Chen J. Critical Roles of Balanced Innate Lymphoid Cell Subsets in Intestinal Homeostasis, Chronic Inflammation, and Cancer. J Immunol Res. 2019;2019:1325181. Published 2019 Nov 5. doi:10.1155/2019/1325181
- Harvard Health Publishing, Harvard Medical School. Chronic Prostatitis. https://www.health.harvard.edu/a_to_z/chronic-prostatitis-a-to-z. Accessed September 9, 2024.
- Wlodarska M, Willing BP, Bravo DM, Finlay BB. Phytonutrient diet supplementation promotes beneficial Clostridia species and intestinal mucus secretion resulting in protection against enteric infection. Sci Rep. 2015;5:9253. Published 2015 Mar 19. doi:10.1038/srep09253
- Forgie AJ, Fouhse JM, Willing BP. Diet-Microbe-Host Interactions That Affect Gut Mucosal Integrity and Infection Resistance. Front Immunol. 2019;10:1802. Published 2019 Aug 6. doi:10.3389/fimmu.2019.01802
- Song M, Zeng Q, Xiang Y, et al. The antibacterial effect of topical ozone on the treatment of MRSA skin infection. Mol Med Rep. 2018;17(2):2449-2455. doi:10.3892/mmr.2017.8148
- Harapan BN, Harapan T. The role of ozone therapy in severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection and coronavirus disease 2019 (COVID-19): a review. Med Gas Res. 2023;13(4):165-171. doi:10.4103/2045-9912.369237
- Rowen RJ. Ozone therapy as a primary and sole treatment for acute bacterial infection: case report. Med Gas Res. 2018;8(3):121-124. Published 2018 Sep 25. doi:10.4103/2045-9912.241078
- Ballo MK, Rtimi S, Pulgarin C, et al. In Vitro and In Vivo Effectiveness of an Innovative Silver-Copper Nanoparticle Coating of Catheters To Prevent Methicillin-Resistant Staphylococcus aureus Infection. Antimicrob Agents Chemother. 2016;60(9):5349-5356. Published 2016 Aug 22. doi:10.1128/AAC.00959-16
- Tiwari V, Tiwari M, Solanki V. Polyvinylpyrrolidone-Capped Silver Nanoparticle Inhibits Infection of Carbapenem-Resistant Strain of Acinetobacter baumannii in the Human Pulmonary Epithelial Cell. Front Immunol. 2017;8:973. Published 2017 Aug 16. doi:10.3389/fimmu.2017.00973
- Szymańska E, Orłowski P, Winnicka K, et al. Multifunctional Tannic Acid/Silver Nanoparticle-Based Mucoadhesive Hydrogel for Improved Local Treatment of HSV Infection: In Vitro and In Vivo Studies. Int J Mol Sci. 2018;19(2):387. Published 2018 Jan 28. doi:10.3390/ijms19020387
- Criscuolo AA, Sesti F, Piccione E, et al. Therapeutic Efficacy of a Coriolus versicolor-Based Vaginal Gel in Women with Cervical Uterine High-Risk HPV Infection: A Retrospective Observational Study. Adv Ther. 2021;38(2):1202-1211. doi:10.1007/s12325-020-01594-6
- Yeh H, Vo DNK, Lin ZH, et al. GMI, a protein from Ganoderma microsporum, induces ACE2 degradation to alleviate infection of SARS-CoV-2 Spike-pseudotyped virus. Phytomedicine. 2022;103:154215. doi:10.1016/j.phymed.2022.154215
- Ahad S, Tanveer S, Malik TA. Anticoccidial activity of aqueous extract of a wild mushroom (Ganoderma applanatum) during experimentally induced coccidial infection in broiler chicken. J Parasit Dis. 2016;40(2):408-414. doi:10.1007/s12639-014-0518-3
- Ginde AA, Blatchford P, Breese K, et al. High-Dose Monthly Vitamin D for Prevention of Acute Respiratory Infection in Older Long-Term Care Residents: A Randomized Clinical Trial. J Am Geriatr Soc. 2017;65(3):496-503. doi:10.1111/jgs.14679
- Giraldo DM, Cardona A, Urcuqui-Inchima S. High-dose of vitamin D supplement is associated with reduced susceptibility of monocyte-derived macrophages to dengue virus infection and pro-inflammatory cytokine production: An exploratory study. Clin Chim Acta. 2018;478:140-151. doi:10.1016/j.cca.2017.12.044
- Mansur JL, Tajer C, Mariani J, Inserra F, Ferder L, Manucha W. Vitamin D high doses supplementation could represent a promising alternative to prevent or treat COVID-19 infection. El suplemento con altas dosis de vitamina D podría representar una alternativa promisoria para prevenir o tratar la infección por COVID-19. Clin Investig Arterioscler. 2020;32(6):267-277. doi:10.1016/j.arteri.2020.05.003
- Toljan K, Vrooman B. Low-Dose Naltrexone (LDN)-Review of Therapeutic Utilization. Med Sci (Basel). 2018;6(4):82. Published 2018 Sep 21. doi:10.3390/medsci6040082

