Treatment of Referred Back Pain with Dextrose Injections
Treatment of Referred Back Pain using Fascial Dextrose 5% Injections: A Case Report
Kersschot J, Marques LF, Hajji A, Baalbaki R
OPEN ACCESS
PUBLISHED: 31 May 2025
CITATION: Kersschot, J., et al. 2025. Treatment of Referred Back Pain using Fascial Dextrose 5% Injections: A Case Report. Medical Research Archives,
[online] 13(5).https://doi.org/10.18103/mra.v13i5.6560
COPYRIGHT: © 2025 European Society of Medicine. This is an open- access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium,provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v1 3i5.6560
ISSN 2375-1924
Abstract
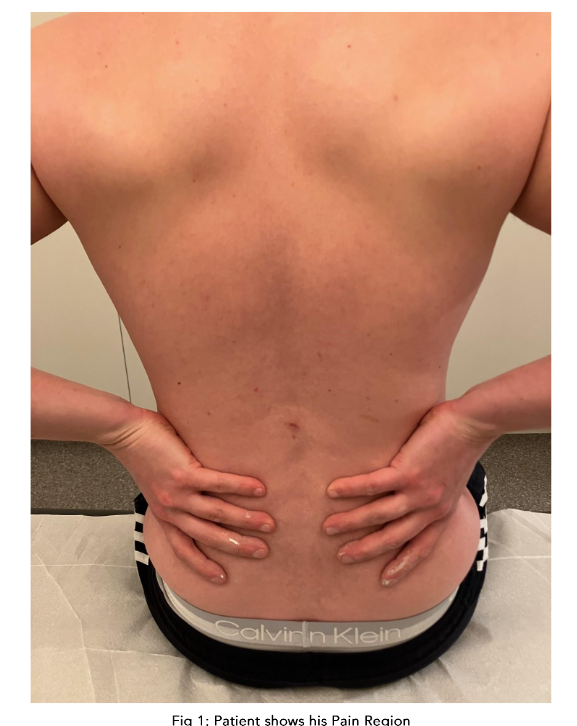
The fascial system (FS) is a complex network of connective tissue that surrounds and permeates the entire human body, encompassing both superficial and deep layers. Regional fascial dysfunctions can lead to pain, trauma, stress and other issues. Fascial dysfunction has been associated with both diminished range of motion as well as regional pain. Unfortunately, such injuries can be difficult to diagnose and treat. Glucocorticoid (GC) injections are commonly utilized in the treatment of musculoskeletal pain; however, they can have adverse effects. This case report describes the use of dextrose 5% (D5W) injections in a patient with referred pain from the lumbar region. It was hypothesized that the pain might be referred from one region to another. The patient received a total of ten D5W injections, which resulted in significant improvement in pain and function. To test this hypothesis, a detailed follow-up was conducted. Informed consent was obtained from the participant included in this case study.
Keywords: fascial system, referred pain, dextrose injections, musculoskeletal pain, glucocorticoids
Introduction
For the same reason, when dealing with Dupuytren’s grip 1, glucocorticoids is advised rather than prolotherapy. When injecting D5W into a joint cavity, the mode of action is probably not related to connective tissue proliferation but to the effect of dextrose on the cartilage. According to Prolotherapy, prolotherapy is not indicated for chronic pain syndromes outside the field of MSK pain by injecting in the subcutaneous fascia in the pain region. PT, however, cannot be used for vein sclerosis. Despite these obvious differences, some articles still use the term “prolotherapy” while they are discussing D5W.
Difference Between Glucocorticoid and Perineural Injection Therapy
Perineural Injection Therapy (PIT) and GP both apply low concentrations of sugar water (5%). PIT typically involves landmark-based injections of D5W along superficial peripheral nerves.⁵⁶⁵⁷ These injections are all administered subcutaneously, while glucopuncture also targets deeper structures, such as joints, muscles and ligaments. In contrast to PIT, GP is also applied for chronic functional complaints outside the field of MSK pain by injecting in the subcutaneous fascia in the pain region.⁵⁸ PIT according to Lyftogt typically applies buffered dextrose (pH 7.2) by adding bicarbonate to the D5W.⁵⁹⁶⁰ The latter is not added to the injectate in GP.
Conclusion
In the last decade, physicians came to see that the fascia is a system that connects different parts of the body like an invisible three-dimensional spider web. As fascia is often hypothesized to explain how MSK pain can be referred from one region to another. Recently, it has been postulated that acupuncture can regulate pain originating from subcutaneous fascial lesions. This technique may be important in patients with regional pain who show no pathological signs on MRI or ultrasound. The superficial fascia may also explain referred pain which does not correspond with myofascial trigger points, bulging discs, fast joint degeneration nor peripheral nerve patterns. It is still not completely clear how D5W injections can alter the state of fascia and interstitium. We realize that there are still a lot of unanswered questions regarding the role of the fascial system and interstitium.
Statement of Informed Consent:
Informed consent was obtained from the participant included in this case study.
References
1. Bordoni B, Mahabadi N, Varacallo MA. Anatomy, Fascia. 2023 Jul 17. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–.
2. Stecco C, Macchi V, Porzionato A, Duparc F, De Caro R. The fascia: the forgotten structure. Ital J Anat Embryol. 2011;116(3):127-38.
3. Exeter D, Connell DA. Skeletal muscle: functional anatomy and pathophysiology. Semin Musculoskelet Radiol. 2010 Jun;14(2):97-105.
4. Phan V, Shah J, Tandon H, Srbely J, DeStefano S, Kumbhare D, Sikdar S, Clouse A, Gandhi A, Gerber L. Myofascial Pain Syndrome: A Narrative Review Identifying Inconsistencies in Nomenclature. PM R. 2020 Sep;12(9):916-925.
5. Kodama Y, Masuda S, Ohmori T, Kanamaru A, Tanaka M, Sakaguchi T, Nakagawa M. Response to Mechanical Properties and Physiological Challenges of Fascia: Diagnosis and Rehabilitative Therapeutic Intervention for Myofascial System Disorders. Bioengineering (Basel). 2023 Apr 14;10(4):474.
6. Frontera WR, Ochala J. Skeletal muscle: a brief review of structure and function. Calcif Tissue Int. 2015 Mar;96(3):183-95.
7. Brooks SV, Guzman SD, Ruiz LP. Skeletal muscle structure, physiology, and function. Handb Clin Neurol. 2023;195:3-16.
8. Yoshimoto Y, Oishi Y. Mechanisms of skeletal muscle-tendon development and regeneration/ healing as potential therapeutic targets. Pharmacol Ther. 2023 Mar;243:108357
9. Kodama Y, Masuda S, Ohmori T, Kanamaru A, Tanaka M, Sakaguchi T, Nakagawa M. Response to Mechanical Properties and Physiological Challenges of Fascia: Diagnosis and Rehabilitative Therapeutic Intervention for Myofascial System Disorders. Bioengineering (Basel). 2023 Apr 14;10(4):474.
10. Stecco C, Porzionato A, Macchi V, Tiengo C, Parenti A, Aldegheri R, Delmas V, De Caro R. Histological characteristics of the deep fascia of the upper limb. Ital J Anat Embryol. 2006 Apr-Jun; 111(2):105-10.
11. Adstrum S, Hedley G, Schleip R, Stecco C, Yucesoy CA. Defining the fascial system. J Bodyw Mov Ther. 2017 Jan;21(1):173-177.
12. Vieira L. Embryology of the Fascial System. Cureus. 2020 Aug 30;12(8):e10134.
13. Bordoni B. Improving the New Definition of Fascial System. Complement Med Res. 2019;26 (6):421-426.
14. Adstrum S, Hedley G, Schleip R, Stecco C, Yucesoy CA. Defining the fascial system. J Bodyw Mov Ther. 2017 Jan;21(1):173-177.
15. Bordoni B, Myers T. A Review of the Theoretical Fascial Models: Biotensegrity, Fascintegrity, and Myofascial Chains. Cureus. 2020 Feb 24;12(2):e7092.
16. Kim MY, Na YM, Moon JH. Comparison on treatment effects of dextrose water, saline and lidocaine for trigger point injection. J Korean Acad Rehab Med 1997;21:967-973
17. Kersschot J, Karavani I. Isotonic Glucose Injections for Postherpetic Neuralgia in the Elderly. Cureus. 2022 Sep 29;14(9):e29740.
18. Kersschot J, Treatment of Dorsal Pain with Intrafascial Injections. Trends Gen Med. 2024; 2(1): 1-3.
19. Kersschot J, Glucopuncture: A Clinical Guide to Regional Glucose 5% Injections, B P International (India/UK), ebook May 2023
20. Kersschot J, Glucopuncture for Treatment of Fascial Pain in the Thumb. A Clinical Case. ISAR Journal of Medical and Pharmaceutical Sciences 2024 (1), 4: 1–5).
21. Chao TC, Reeves KD, Lam KHS, Li TY, Wu YT. The Effectiveness of Hydrodissection with 5% Dextrose for Persistent and Recurrent Carpal Tunnel Syndrome: A Retrospective Study. J Clin Med. 2022 Jun 27;11(13):3705.
22. Nasiri A, Rezaei Motlagh F, Vafaei MA. Efficacy comparison between ultrasound-guided injections of 5% dextrose with corticosteroids in carpal tunnel syndrome patients. Neurol Res. 2023 Jun;45(6): 554-563.
23. Lam KHS, Wu YT, Reeves KD, Galluccio F, Allam AE, Peng PWH. Ultrasound-Guided Interventions for Carpal Tunnel Syndrome: A Systematic Review and Meta-Analyses. Diagnostics (Basel). 2023 Mar 16;13(6):1138.
24. Kersschot J, Intra-articular Glucose Injections for Orthoregeneration of Frozen Shoulder. A Clinical Case. Medical Research Archives 2023, 11(8), 1-5.
25. Pandey N, Nayak P, Gahnolia V, A Randomized Control Trial on Efficacy of Analgesic Effect of 5% Dextrose Caudal Epidural Injection for Non-specific Low Back Pain. International Journal of Scientific Research, 2021, 10 (9), 11-13.
26. Smigel LR, Reeves KD, Lyftogt J, Rabago DP. Poster 385 Caudal Epidural Dextrose Injections (D5W) for Chronic Back Pain with Accompanying Buttock or Leg Pain: A Consecutive Patient Study with Long-Term Follow-up. PM R. 2016 Sep;8(9S): S286-S287.
27. Chao TC, Reeves KD, Lam KHS, Li TY, Wu YT. The Effectiveness of Hydrodissection with 5% Dextrose for Persistent and Recurrent Carpal Tunnel Syndrome: A Retrospective Study. J Clin Med. 2022 Jun 27;11(13):3705.
28. Lam KHS, Wu YT, Reeves KD, Galluccio F, Allam AE, Peng PWH. Ultrasound-Guided Interventions for Carpal Tunnel Syndrome: A Systematic Review and Meta-Analyses. Diagnostics (Basel). 2023 Mar 16;13(6):1138.
29. Nasiri A, Rezaei Motlagh F, Vafaei MA. Efficacy comparison between ultrasound-guided injections of 5% dextrose with corticosteroids in carpal tunnel syndrome patients. Neurol Res. 2023 Jun;45(6): 554-563.
30. Babaei-Ghazani A, Moradnia S, Azar M, Forogh B, Ahadi T, Chaibakhsh S, Khodabandeh M, Eftekharsadat B. Ultrasound-guided 5% dextrose prolotherapy versus corticosteroid injection in carpal tunnel syndrome: a randomized, controlled clinical trial. Pain Manag. 2022 Sep;12(6):687-697.
31. Cherng JH, Chang SJ, Tsai HD, Chun CF, Fan GY, Reeves KD, Lam KHS, Wu YT. The Potential of Glucose Treatment to Reduce Reactive Oxygen Species Production and Apoptosis of Inflamed Neural Cells In Vitro. Biomedicines. 2023; 11(7):1837.
32. Lam KHS, Su DCJ, Wu Y-T, Fajardo Pérez M, Reeves KD, Peng P, Fullerton B. Infraspinatus Fascial Dysfunction as a Cause of Painful Anterior Shoulder Snapping: Its Visualization via Dynamic Ultrasound and Its Resolution via Diagnostic Ultrasound-Guided Injection. Diagnostics. 2023; 13(15):2601.
33. Lam KHS, Hung CY, Chiang YP, Onishi K, Su DCJ, Clark TB, Reeves KD. Ultrasound-Guided Nerve Hydrodissection for Pain Management: Rationale, Methods, Current Literature, and Theoretical Mechanisms. J Pain Res. 2020 Aug 4;13:1957-1968.
34. Shi X, Xu H, Zhu J, Li G, Bai L. A Randomized Double-blind Trial of 5% Dextrose Versus Corticosteroid Hydrodissection for Meralgia Paresthetica. Pain Physician. 2024 Nov;27(8):E835-E842.
35. Oh MW, Park JI, Shim GY, Kong HH. Comparative Efficacy of 5% Dextrose and Corticosteroid Injections in Carpal Tunnel Syndrome: A Systematic Review and Meta-analysis. Arch Phys Med Rehabil. 2025 Feb;106(2):300-310.
36. Cherng JH, Chang SJ, Tsai HD, Chun CF, Fan GY, Reeves KD, Lam KHS, Wu YT. The Potential of Glucose Treatment to Reduce Reactive Oxygen Species Production and Apoptosis of Inflamed Neural Cells In Vitro. Biomedicines. 2023 Jun 26; 11(7):1837.
37. Gao N, Li M, Wang W, Liu Z, Guo Y. The dual role of TRPV1 in peripheral neuropathic pain: pain switches caused by its sensitization or desensitization. Front Mol Neurosci. 2024 Sep 9;17:1400118
38. Benias, P.C., Wells, R.G., Sackey-Aboagye, B. et al. Structure and Distribution of an Unrecognized Interstitium in Human Tissues. Sci Rep 2018, 8, 4947.
39. Alexander CE, Cascio MA, Varacallo MA. Lumbosacral Facet Syndrome. 2023 Aug 4. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–.
40. Heller GZ, Manuguerra M, Chow R. How to analyze the Visual Analogue Scale: Myths, truths and clinical relevance. Scand J Pain. 2016 Oct;13: 67-75.
41. Lai WF, Yoon CH, Chiang MT, Hong YH, Chen HC, Song W, Chin YPH. The effectiveness of dextrose prolotherapy in plantar fasciitis: A systemic review and meta-analysis. Medicine (Baltimore). 2021 Dec 23;100(51):e28216.
42. Kazempour Mofrad M, Rezasoltani Z, Dadarkhah A, Hamidi Panah S, Tabatabaee SM, Azarakhsh A. Neurofascial Dextrose Prolotherapy for Managing Chronic Ankle Ligament Injury. Anesth Pain Med. 2022 Jan 23;12(1):e118317.
43. Zhu M, Rabago D, Chung VC, Reeves KD, Wong SY, Sit RW. Effects of Hypertonic Dextrose Injection (Prolotherapy) in Lateral Elbow Tendinosis: A Systematic Review and Meta-analysis. Arch Phys Med Rehabil. 2022 Nov;103(11):2209-2218.
44. Catapano M, Zhang K, Mittal N, Sangha H, Onishi K, de Sa D. Effectiveness of Dextrose Prolotherapy for Rotator Cuff Tendinopathy: A Systematic Review. PM R. 2020 Mar;12(3):288-300. doi: 10.1002/pmrj.12268. Epub 2019 Dec 4. Erratum in: PM R. 2020 Oct;12(10):1064.
45. Chung MW, Hsu CY, Chung WK, Lin YN. Effects of dextrose prolotherapy on tendinopathy, fasciopathy, and ligament injuries, fact or myth?: A systematic review and meta-analysis. Medicine (Baltimore). 2020 Nov 13;99(46):e23201.
46. Krstičević M, Jerić M, Došenović S, Jeličić Kadić A, Puljak L. Proliferative injection therapy for osteoarthritis: a systematic review. Int Orthop. 2017 Apr;41(4):671-679.
47. Kersschot J, Mathieu T. Treatment of Painless Nodules With Glucopuncture in Dupuytren’s Disease in Men: A Clinical Case. Cureus. 2022 Nov 13;14(11):e31445.
48. Reeves KD, Atkins JR, Solso CR, Cheng CI, Thornell IM, Lam KHS, Wu YT, Motyka T, Rabago D. Rapid Decrease in Dextrose Concentration After Intra-Articular Knee Injection: Implications for Mechanism of Action of Dextrose Prolotherapy. Biomedicines. 2025 Feb 4;13(2):350.
49. Khateri S, Nejad FB, Kazemi F, Alaei B, Azami M, Moradkhani A, Majidi L, Moradi Y. The effect of dextrose prolotherapy on patients diagnosed with knee osteoarthritis: A comprehensive systematic review and meta-analysis of interventional studies. Health Sci Rep. 2024 Jun 24;7(6):e2145.
50. Chang SF, Huang KC, Cheng CC, Su YP, Lee KC, Chen CN, Chang HI. Glucose adsorption to chitosan membranes increases proliferation of human chondrocyte via mammalian target of rapamycin complex 1 and sterol regulatory element-binding protein-1 signaling. J Cell Physiol. 2017 Oct;232 (10):2741-2749.
51. Arias-Vázquez PI, Tovilla-Zárate CA, Castillo-Avila RG, Legorreta-Ramírez BG, López-Narváez ML, Arcila-Novelo R, González-Castro TB. Hypertonic Dextrose Prolotherapy, an Alternative to Intra-Articular Injections With Hyaluronic Acid in the Treatment of Knee Osteoarthritis: Systematic Review and Meta-analysis. Am J Phys Med Rehabil. 2022 Sep 1;101(9):816-825.
52 https://www.iart.org/foundation
53. Babaei-Ghazani A, Moradnia S, Azar M, Forogh B, Ahadi T, Chaibakhsh S, Khodabandeh M, Eftekharsadat B. Ultrasound-guided 5% dextrose prolotherapy versus corticosteroid injection in carpal tunnel syndrome: a randomized, controlled clinical trial. Pain Manag. 2022 Sep;12(6):687-697.
54. Chen CPC, Suputtitada A. Prolotherapy at Multifidus Muscle versus Mechanical Needling and Sterile Water Injection in Lumbar Spinal Stenosis. J Pain Res. 2023 Jul 18;16:2477-2486.
55. Kersschot J. Low-Dose Dextrose Prolotherapy as Effective as High-Dose Dextrose Prolotherapy in the Treatment of Lateral Epicondylitis? A Double-Blind, Ultrasound Guided, Randomized Controlled Study. Arch Phys Med Rehabil. 2023 Jul;104(7): 1154-1155.
56. Lyftogt J, Subcutaneous prolotherapy treatment of refractory knee, shoulder, and lateral elbow pain. Australasian Musculoskel Med. 2007; 12 (1), 107-109.
57. Lyftogt J. Prolotherapy and Achilles tendinopathy: a prospective pilot study of an old treatment. Australas Musculoskel Med. 2005; 10:16-19.
58. Kersschot J, Treatment of irritable bowel syndrome with glucopuncture: a case report. Int J Health Sci Res. 2024; 14(7):235-240.
59. Choong JT, Suhaimi A, Su DC, Lam KHS. Perineural Injection Therapy for Hemiplegic Shoulder Pain: A Novel Management Approach. Cureus. 2025 Feb 19;17(2):e79332.
60. Kim H, Kim HJ, Jung YH, Do W, Kim EJ. The effect of perineural injection therapy on neuropathic pain: a retrospective study. J Dent Anesth Pain Med. 2024 Feb;24(1):47-56. doi: 10.17245/jdap m.2024.24.1.47. Epub 2024 Feb 1.
61. Vinyes D, Muñoz-Sellart M, Fischer L. Therapeutic Use of Low-Dose Local Anesthetics in Pain, Inflammation, and Other Clinical Conditions: A Systematic Scoping Review. J Clin Med. 2023 Nov 21;12(23):7221.
62. Rey Novoa M, Muñoz-Sellart M, Catalán Soriano M, Vinyes D. Treatment of Localized Vulvar Pain with Neural Therapy: A Case Series and Literature Review. Complement Med Res. 2021;28(6):571-577.
63. Bashan I, Ozturk GY. Effect of Neural Therapy on shoulder dysfunction and pain in supraspinatus tendinopathy. Pak J Med Sci. 2022 Mar-Apr;38 (3Part-I):565-569.
64. Vinyes D, Muñoz-Sellart M, Gurevich M. Procaine Injections in Myofascial Tension Points in the Treatment of Anxiety Disorders: A Case Series. International Journal of Clinical Case Reports and Reviews. 2025, 22. 22. 10.31579/2690-4861/643.
65. Altınbilek T, Terzi R, Başaran A, Tolu S, Küçüksaraç S. Evaluation of the effects of neural therapy in patients diagnosed with fibromyalgia. Turkish Journal of Physical Medicine and Rehabilitation, 2019, 65(1), 1.
66. Tilscher H, Eder M, Infiltrationstherapie (Therapeutic Local Anesthesia), Hippokrates 1996, Third Edition
67. Kersschot J, Biopuncture, The Management of Common Orthopedic and Sports Disorders, Thieme Publishing 2014
68. Schneider C. Traumeel – an emerging option to nonsteroidal anti-inflammatory drugs in the management of acute musculoskeletal injuries. Int J Gen Med. 2011 Mar 25;4:225-34.
69. Ehlert D, Majjhoo A. Traumeel® Epidural Injection: A Viable Alternative to Corticosteroids – A Five-Patient Case Study. Cureus. 2019 Nov 19; 11(11):e6196.

