Vaccination: Successes and Challenges Over 50 Years
Vaccination: A Legacy of Success and Persistent Challenges, 50 Years Since the Launch of the Expanded Programme on Immunization
Enrique Chacon-Cruz1, Erika Zoe Lopatynsky-Reyes2, Yodira Guadalupe Hernandez-Ruiz3
- Enrique Chacon-Cruz Think Vaccines LLC, Houston, Texas, USA.
 http://orcid.org/0000-0003-2466-4920
http://orcid.org/0000-0003-2466-4920 - Erika Zoe Lopatynsky-ReyesThink Vaccines LLC, Houston, Texas, USA.
 http://orcid.org/0000-0003-4121-6521
http://orcid.org/0000-0003-4121-6521 - Yodira Guadalupe Hernandez-Ruiz School of Medicine, University of Monterrey, Mexico.
 http://orcid.org/0000-0002-7037-664X
http://orcid.org/0000-0002-7037-664X
Email: [email protected], [email protected], [email protected]
OPEN ACCESS
PUBLISHED: 31 March 2025
CITATION: Chacon-Cruz, E., Lopatynsky-Reyes, E.Z., Hernandez-Ruiz, Y.G., 2025. Vaccination: A Legacy of Success and Persistent Challenges, 50 Years Since the Launch of the Expanded Programme on Immunization. Medical Research Archives, [online] 13(3). https://doi.org/10.18103/mra.v13i3.6311
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i3.6311
ISSN 2375-1924
Abstract
Fifty years have passed since the Expanded Programme on Immunization (EPI) was established by the World Health Assembly in May 1974, revolutionizing global vaccination coverage and significantly reducing the disease, social, and economic burden of vaccine-preventable diseases included in the program. This publication provides a comprehensive overview of the global impact of vaccines, covering their history—from variolation to modern and future vaccine platforms—as well as the creation of key organizations such as the Pan American Health Organization (PAHO) and the World Health Organization (WHO). It also highlights the contributions of both humanitarian and commercial entities that have played a crucial role in achieving worldwide vaccination reach. While celebrating these achievements, this work also underscores the present and future challenges in ensuring equitable vaccine access across the globe. Additionally, it emphasizes the urgent need for vaccines against numerous diseases that remain without immunization solutions. Without a doubt, vaccination stands as the most impactful public health intervention of our time.
Keywords
Vaccination, Expanded Programme on Immunization, Public Health, Vaccine-Preventable Diseases, Global Health
Introduction and brief history of vaccinology:
Variolation was practiced for centuries in the Middle East and China, where crusts from smallpox-infected individuals were administered in various ways to close contacts, providing them with protection against the disease. This method was later introduced to the United Kingdom by Lady Mary Wortley Montagu, the wife of the British ambassador to the Ottoman Empire. In April 1721, during a smallpox epidemic in England, she had her daughter inoculated by Dr. Charles Maitland, the same physician who had previously inoculated her son at the British Embassy in Turkey. She publicly promoted the procedure, making it the first recorded instance of variolation in England. Lady Montagu then persuaded Caroline of Ansbach, the Princess of Wales, to support the practice. Later that year, in August 1721, seven prisoners at Newgate Prison who were awaiting execution were offered the opportunity to undergo variolation in exchange for their freedom. All survived and were subsequently released, further demonstrating the efficacy of the procedure. This success led to the widespread adoption of variolation across Europe.
However, vaccination as we know it, began in the late 18th century when Edward Jenner revolutionized smallpox immunization. He conducted the first recorded non-randomized, unblinded clinical trial in vaccine history by inoculating human subjects with material from cowpox lesions. This pioneering approach laid the foundation for the field of vaccinology.
Vaccines prime the immune system to recognize and respond swiftly upon subsequent exposure to the same pathogen, effectively preventing disease progression and either attenuating or eliminating the infection by stimulating both B and T cells. This groundbreaking work marked the birth of active immunization, paving the way for modern vaccinology. Since then, generations of brilliant scientists have built upon his legacy, advancing immunization strategies that continue to shape global public health. The list is immense, and while the following are some of the most iconic discoveries, they represent just a fraction of the numerous groundbreaking advancements.
- Louis Pasteur: The “germ theory”, rabies, anthrax and cholera vaccines.
- Emil Von Behring: Diphtheria antitoxin.
- Kitasato Shibasaburo: Diphtheria/tetanus antitoxin.
- Achille Sclavo: First serum against anthrax, and the Sclavo Institute selected by Albert Sabin as the first oral polio vaccine (OPV) production site.
- Albert Sabin: First OPV.
- Jonas Salk: First inactivated polio virus vaccine (IPV).
- John F. Enders: First measles vaccine.
- Michiaki Takahashi: First varicella vaccine.
- Avery and Michael Heidelberger: Establishing capsular antigens as the basis of the serotypes of pneumococcal bacteria.
- John Robbins: First glycoconjugate (polysaccharide-protein) vaccine -Haemophilus influenzae type b.
And then the “quantum leap”:
- Subunit vaccines recombinant vaccines, e.g. Hepatitis B.
- Reverse vaccinology, e.g. Meningococcal B vaccine.
- Adjuvants.
- Virus-like particle vaccines, e.g. HPV vaccine.
- Viral vector vaccines, e.g. COVID-19 and Ebola vaccines.
- mRNA vaccines, e.g. COVID-19 vaccines.
- Plant vaccines, e.g. HPV vaccines.
- Structural vaccinology, e.g. RSV vaccines.
Since the World Health Organization (WHO)’s declaration of smallpox eradication in 1980, two more viruses were declared eradicated – polio 2 in 2015 and polio 3 in 2019, mainly because of the implementation of immunization programs which include cornerstone vaccines but beyond that can differ regionally.
The first Expanded Programme on Immunization (EPI) was established by the World Health Assembly in May 1974, demonstrating a proactive commitment to extending the protective benefits of vaccination globally. Inspired by the success of the smallpox eradication campaign WHO launched this collaborative initiative with the initial goal of vaccinating all children against seven major diseases: smallpox, tuberculosis, diphtheria, tetanus, pertussis, poliomyelitis, and measles by 1990.
Over time, the EPI has expanded to include vaccines targeting additional global and region-specific pathogens and expanded to age groups beyond infancy, with decisions on inclusion made by individual country programs. Since its inception, the programme has seen remarkable growth in the number of diseases covered, supported by catalytic strategies, innovative initiatives, and a unified global vision. This expansion has resulted in significant increases in both the breadth of protection and vaccine coverage.
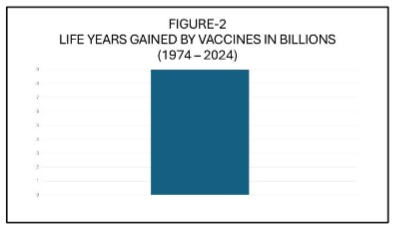
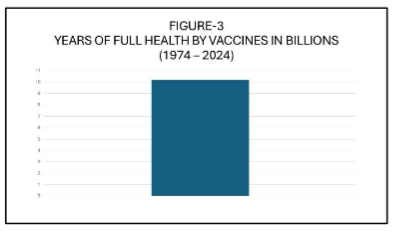
Global coverage with the third dose of the diphtheria–tetanus–pertussis (DTP3) vaccine—commonly used as a proxy for vaccine program performance—rose from less than 5% in 1974 to 86% in 2019, prior to the COVID-19 pandemic. Between 1974 and 2024, vaccination is estimated to have prevented 154 million deaths, including 146 million among children under the age of 5, of which 101 million were infants under 1 year old. Additionally, during this 50-year period, vaccination has contributed to the gain of 9 billion life-years and 10.2 billion years of full health. These achievements position vaccines and immunization as one of the most impactful healthcare interventions, second only, perhaps, to access to potable water.
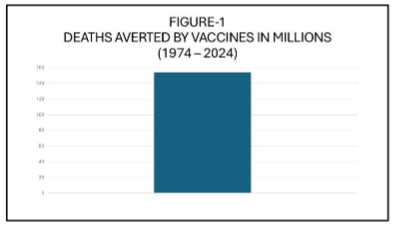
(Data obtained from Shattock AJ, et al. Contribution of vaccination to improved survival and health: modelling 50 years of the Expanded Programme on Immunization. Lancet 2024; 403: 2307–16. https://doi.org/10.1016/)
The Extensive and Complex Journey:
The following outlines a chronological sequence of achievements aimed at accomplishing the goals just described:
- 1974: The 27th World Health Assembly: Formally established EPI against diphtheria, pertussis, tetanus, measles, poliomyelitis, tuberculosis, smallpox, and other diseases, where applicable, according to country-specific epidemiological situation.
- 1979: Pan American Health Organization (PAHO): The resolution of the Pan American Sanitary Conference established the working capital for the PAHO Revolving Fund, a mechanism designed to facilitate pooled procurement and enhance access to vaccines, syringes, and cold-chain equipment at affordable prices.
- 1982: UNICEF Child Survival and Development Revolution: The Child Survival and Development Revolution emphasized four key interventions: growth monitoring, oral rehydration therapy, promotion of breastfeeding, and immunization.
- 1984: EPI’s first standardized schedule: Included were vaccinations for tuberculosis (BCG vaccine at birth); diphtheria, tetanus, and pertussis (DTP); poliomyelitis (administered alongside DTP at 6, 10, and 14 weeks); and measles (at 9 months).
- 1990: Declaration of Manhattan, Children’s Vaccine Initiative: Its goal was to accelerate efforts to develop vaccines that would strengthen and enhance the effectiveness of the Expanded Programme on Immunization (EPI).
- 1999: The Strategic Advisory Group of Experts (SAGE) on immunization: A vital arm of the WHO dedicated to global vaccine-related policies, recommendations, prequalification, strategies, research and development (R&D), and addressing various aspects of vaccine-preventable diseases.
- 2000: The Vaccine Alliance (Gavi): The “Vaccine Alliance”, a combined private-public partnership to make vaccines more affordable to developing countries, an essential tool for equity. In nearly 25 years since its launch, Gavi has made significant strides in advancing equity in vaccine manufacturing. In 2000, four of its five vaccine suppliers were based in wealthy countries. Today, the majority of its approximately 20 suppliers are located in developing countries. Gavi has created a marketplace for large-scale, low-cost manufacturing in countries like India, Brazil, China, Indonesia, and others.
- 2000 to present: ongoing acceleration of new vaccine production and implementation:
- The Meningitis Vaccine Project facilitated the development, testing, licensure, and introduction of the meningococcal A conjugate vaccine for the meningitis belt in Africa.
- The Accelerated Development and Introduction Plans for pneumococcal conjugate vaccines (PCV) and rotavirus vaccines, along with the Haemophilus influenzae type B Initiative, significantly expedited vaccine introduction in Gavi-supported countries.
- The Malaria Vaccine Implementation Programme.
- 2017: Coalition for Epidemic Preparedness Innovations (CEPI): As a global response to Ebola virus, Zika virus, and severe acute respiratory syndrome (known as SARS) outbreaks, CEPI was launched to develop safe and effective vaccines for emerging infectious diseases to prevent future epidemics. Currently CEPI plays a vital role in accelerating vaccine implementation during outbreaks, epidemics, and pandemics, as demonstrated by initiatives such as the “100-Day Mission for Pandemic Vaccine Implementation.”
- 2020–23: COVID-19 Vaccines Global Access (COVAX): COVAX was the vaccine mainstem created to accelerate the development, production, and equitable distribution of COVID-19 tests, treatments, and vaccines. Its goal was to reduce COVID-19 mortality and severe disease, while facilitating the full restoration of societal and economic activity.
- Others, but not less important:
- 2023–24: “The Big Catch-Up”
- EPI expansion
- The Global Polio Eradication Initiative
- Maternal and Neonatal Tetanus Elimination
- The Measles and Rubella Initiative
- The End TB strategy
- The Global Health Sector Strategy on Viral Hepatitis
- The Global Technical Strategy for Malaria
- The Eliminate Yellow Fever Epidemics Strategy
- The Global Strategy to Accelerate the Elimination of Cervical Cancer
- The Global Roadmap to Defeat Meningitis
A collaborative effort between the private and public sectors:
WHO, Gavi, UNICEF, the Gates Foundation, Wellcome Trust, PATH, Rotary, the International Vaccine Institute, CEPI, Clinton Health Access Initiative, GSI, the World Bank, the Pan American Health Organization Revolving Fund, and other organizations, along with governments, have collaborated to leverage vaccines as a powerful tool in combating disease and addressing health disparities. The recent decision by the U.S. government to cease financial contributions to the WHO and Gavi poses a significant challenge to this effort. However, it also presents an opportunity for all countries and private initiatives to foster a more focused, robust, and reformed approach to achieving global health goals and mitigating potential risks.
It is crucial that countries collaborate on a global scale to tackle health crises like pandemics, which do not respect national borders. However, this collaboration must be balanced with a strategy for greater financial and strategic independence. Each nation needs to invest in its own immunization and surveillance systems to ensure continuous access to public health services. This independence would serve as a vital Plan B in the event that a partner country decides to withdraw support, ensuring that local health initiatives can proceed without interruption. By enhancing national capabilities while still engaging in international cooperation, we can create a resilient global health network where every country is both a contributor and a self-sufficient entity in the fight for public health. This dual approach not only strengthens global health security but also guarantees that access to essential health services remains uninterrupted, safeguarding the health and well-being of populations worldwide.
WHO global priority endemic pathogens for vaccine research and development (R&D):
The WHO Immunization Agenda 2030 (IA2030) has established a structured approach to prioritize vaccine R&D for endemic pathogens based on regional and country-specific health needs. Through surveys conducted with policymakers and immunization stakeholders across WHO regions, eight criteria were used to assess pathogens, with two—annual deaths in children under five and contribution to antimicrobial resistance—emerging as top priorities in five of the six regions.
The survey responses revealed that these priority criteria did not significantly vary by region, demographic background, or expertise area of respondents. This consistency helped identify five pathogens—Mycobacterium tuberculosis, HIV-1, Klebsiella pneumoniae, Staphylococcus aureus, and extra-intestinal pathogenic Escherichia coli—as shared priorities across all regions. Additionally, six pathogens were uniquely prioritized in individual regions, reflecting localized health needs.
By merging the top ten pathogen lists from each region, WHO derived a global priority list of 17 pathogens for targeted vaccine R&D. To support this agenda, 34 distinct R&D use cases were identified, divided into categories based on necessary actions: Advance product development (the majority), Research, and Prepare to implement. This categorization helps streamline efforts to accelerate vaccine development and implementation for priority pathogens globally.
The following are the 17 global priority pathogens for targeted vaccine R&D:
- Plasmodium falciparum (Malaria)
- Norovirus
- Non Typhoidal Salmonella
- Leishmania species
- Group B Streptococcus
- Dengue virus
- Influenza virus
- Cytomegalovirus
- Shigella species
- Respiratory Syncytial Virus
- Hepatitis C virus
- Group A Streptococcus
- Staphylococcus aureus
- Mycobacterium tuberculosis
- Klebsiella pneumoniae
- HIV-1
- Extra-intestinal pathogenic Escherichia coli
Conclusions:
It is impossible to fully conclude such a multifaceted effort, where, despite significant achievements, there is still much to be done. In our view, scientific leaders must collaborate with their counterparts in the financial and political sectors. Without this partnership, the substantial disparities in vaccine access and implementation will persist, preventing a net global meaningful progress. First and foremost, there is no comparison between the investment in war and weapons and the investment in preventive medicine.
Conflict of Interest:
None.
Funding Statement:
There was no funding to perform this review article.
Acknowledgements:
None.
ORCID:
Enrique Chacon-Cruz – https://orcid.org/0000-0003-24664920.
Erika Zoe Lopatynsky-Reyes – https://orcid.org/0000-0003-41216521.
Yodira Guadalupe Hernandez-Ruiz – https://orcid.org/0000-0002-7037-664X.
References
1. Montero DA, Vidal RM, Velasco J, et al. Two centuries of vaccination: historical and conceptual approach and future perspectives. Front Public Health 2024; 11: 1326154. Doi: 10.3389/fpubh.2023.1326154.
2. Saleh A, Qamar S, Tekin A, Singh R, Kashyap R. Vaccine Development Throughout History. Cureus 2021; 13: e16635. Doi: 10.7759/cureus.16635.
3. Immunize.org. Vaccine History Timeline. https://www.immunize.org/vaccines/vaccine-timeline/ (Accessed February 3, 2025).
4. Clem AS. Fundamentals of vaccine immunology. J Glob Infect Dis 2011; 3: 73-8. Doi: 10.4103/0974-777X.77299.
5. WHO: Declaration of global eradication of smallpox WHA33.3. https://www.who.int/publications/i/item/WHA33-3. (Accessed February 4, 2025).
6. WHO: Polio eradication strategy 2022–2026: delivering on a promise. https://www.who.int/publications/i/item/9789240031937 (Accessed February 4, 2025).
7. World Health Assembly, 27. (1974). WHO expanded programme on immunization. World Health Organization. https://iris.who.int/handle/10665/92778 (Accessed February 4, 2024).
8. Bland J, Clements J. Protecting the world’s children: the story of WHO’s immunization programme. World Health Forum. 1998;19:162-73. PMID: 9652217.
9. Shattock AJ, Johnson HC, Sim SY, Carter A, Lambach P, Hutubessy RCW, et al. Contribution of vaccination to improved survival and health: modelling 50 years of the Expanded Programme on Immunization. Lancet 2024; 403: 2307–16. Doi: 10.1016/S0140-6736(24)00850-X.
10. Haelle T. The staggering success of vaccines. Vaccines are the first step toward health equity in many parts of the world. Sci Am 2024; 331: 86. Doi: 10.1038/d41586-024-03412-3
11. PAHO Revolving Fund. https://www.paho.org/en/revolving-fund. (Accessed January 30, 2025).
12. WHO. Strategic Advisory Group of Experts on Immunization (SAGE). https://www.who.int/groups/strategic-advisory-group-of-experts-on-immunization/. (Accessed January 28, 2025).
13. Gavi, the Vaccine Alliance. A history of Gavi, the Vaccine Alliance. 2023. https://www.youtube.com/watch?v=7QTf5CPC1Tw. (Accessed February 1, 2025).
14. The Coalition for Epidemic Preparedness Innovations (CEPI) Homepage. https://cepi.net/. (Accessed February 1, 2025).
15. WHO-COVAX. https://www.who.int/initiatives/act-accelerator/covax. (Accessed February 1, 2025).
16. Nunes C, McKee M, Howard N. The role of global health partnerships in vaccine equity: a scoping review. PLOS Glob Public Health 2024; 4: e0002834. Doi: https://doi.org/10.1371/journal.pgph.0002834.
17. Bill and Melinda Gates Foundation. Immunization. https://www.gatesfoundation.org/our-work/programs/global-development/immunization. (Accessed February 1, 2025).
18. Donors making a difference: Transforming WHO. 11 December 2024. https://www.who.int/news-room/feature-stories/detail/Donors-making-a-difference–Transforming-WHO (Accessed February 2, 2025).
19. CNN. Trump announces US withdrawal from World Health Organization. https://www.cnn.com/2025/01/21/politics/trump-executive-action-world-health-organization-withdrawal/index.html. (Accessed January 23, 2025).
20. Hasso-Agopsowicz M, Hwang A, Hollm-Delgado MG, Umbelino-Walker I, Karron RA, Rao R, et al. Identifying WHO global priority endemic pathogens for vaccine research and development (R&D) using multi-criteria decision analysis (MCDA): an objective of the Immunization Agenda 2030. EbioMedicine 2024; 4: 105424. Doi: 10.1016/j.ebiom.2024.105424.
21. WHO. Immunization Agenda 2030. A global strategy to leave no one behind. https://www.who.int/docs/default-source/immunization/strategy/ia2030/ia2030-document-en.pdf. (Accessed January 31, 2025).

