ACL Ganglion Cyst in Children: Diagnosis and Treatment
Anterior Cruciate Ligament Ganglion Cyst: Uncommon Cause of Knee Pain
Dr. José María Busto Villarreal¹, Dr. Jimena Guadalupe Prado Peláez²*, Dr. Aldo Vázquez Godínez³, Dr. Juan Felipe Gómez Castillo⁴*
- Chief of the Joint Surgery and Sports Traumatology Service, CEMA Hospital.
ORCID: 0000-0002-2094-1954 - Head of Research and Teaching, CEMA Hospital. ORCID: 0000-0002-3129-2865
- Specialist in Imaging Medicine, CEMA Hospital. ORCID: 0000-0001-9800-063
- Fellowship in High Specialization in Joint Surgery and Sports Traumatology, Hospital CEMA. ORCID: 0009-0001-6198-036X
OPEN ACCESS
PUBLISHED 30 September 2025
CITATION Busto Villarreal, J.M., Prado Peláez, J.G., et al., 2025. Anterior Cruciate Ligament Ganglion Cyst: Uncommon Cause of Knee Pain. Medical Research Archives, [online] 13(9). https://doi.org/10.18103/mra.v13i9.6924
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v13i9.6924
ISSN 2375-1924
ABSTRACT
Purpose: Anterior cruciate ligament (ACL) ganglion cysts are rare intra-articular lesions, particularly uncommon in the pediatric population. This report describes a symptomatic ACL ganglion in a child, detailing clinical presentation, imaging findings, arthroscopic management, and postoperative outcome, and reviews the current literature.
Methods: We present the case of a 7-year-old male with a 3-month history of progressive right knee pain, culminating in extension block. Clinical examination revealed a 10° extension deficit without instability or swelling. Magnetic resonance imaging (MRI) demonstrated an intrasubstance ganglion cyst within the proximal and middle thirds of the ACL, associated with partial fiber disruption. Arthroscopic resection and aspiration of the cyst were performed, followed by a structured rehabilitation program.
Results: Arthroscopy confirmed a ganglionic lesion attached to the ACL walls, with intact menisci and no other intra-articular pathology. Complete cyst excision was achieved without complications. At 3-month follow-up, the patient was pain-free, had regained full range of motion and strength, and returned to sports activities.
Conclusion: Although rare in children, ACL ganglion cysts should be considered in the differential diagnosis of pediatric knee pain with unexplained motion restriction. MRI is the diagnostic modality of choice, and arthroscopic resection offers an effective and definitive treatment with excellent functional recovery.
Keywords:
- anterior cruciate ligament
- ganglion cyst
- knee
- arthroscopy
- pediatric orthopedics
INTRODUCTION
An anterior cruciate ligament (ACL) ganglion cyst refers to a mucin-filled cystic lesion that arises within or adjacent to the ACL. These are rare, benign, intra-articular lesions most commonly associated with the ACL rather than the posterior cruciate ligament (PCL), meniscus, or popliteus tendon. Reported prevalence in adults is up to 1.3% on MRI and up to 2% in arthroscopic studies. The true prevalence in children remains unknown, as most publications describe isolated clinical cases. They have been reported more frequently in individuals aged 2 to 18 years, with a higher incidence in males.
The pathogenesis of ACL ganglion cysts is not fully understood, although trauma and chronic strain are considered important etiological factors. Clinically, they may present with nonspecific symptoms such as knee pain, decreased range of motion, intermittent swelling, or mechanical symptoms like locking—particularly in the absence of osteoarthritis or ligament instability.
MRI is the most sensitive and specific imaging modality for diagnosis, typically showing a well-defined, fluid-filled lesion within or adjacent to the ACL, occasionally exerting a mass effect on the ligament bundles. Given the rarity of this entity, especially in pediatric patients, we present a case detailing its clinical presentation, imaging findings, surgical management, and postoperative outcome, along with a review of the literature on its etiology, diagnosis, and treatment.
CASE REPORT
A 7-year-old male presented with a 3-month history of right knee pain unrelieved by rest or analgesics, progressively worsening to the point of inability to stand upright.
Physical examination revealed no joint effusion, palpable masses, or signs of ligamentous instability. Knee extension was limited by 10°, with no other remarkable findings.
MRI of the right knee demonstrated an intrasubstance ganglion within the ACL occupying the proximal and middle thirds, associated with features suggestive of a near-complete tear, predominantly affecting the posterolateral bundle.
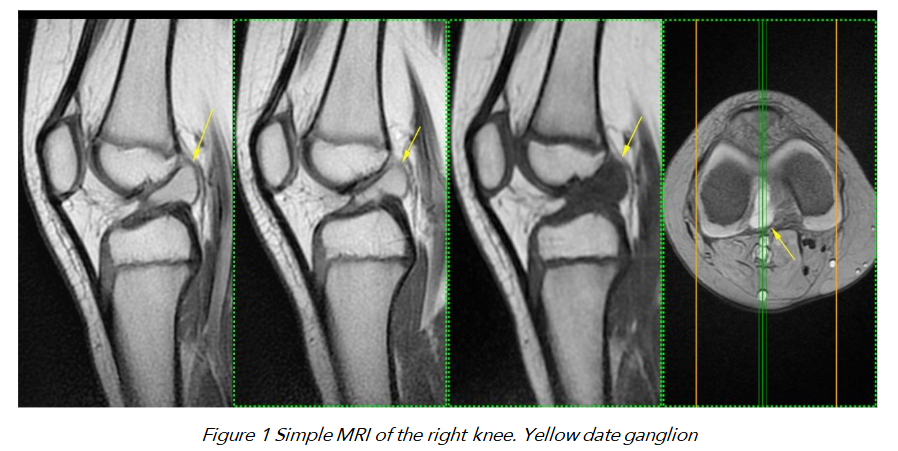
Arthroscopy revealed intact menisci with normal morphology and a ganglion cyst firmly attached to the walls of the ACL. The lesion was aspirated via puncture and the cyst walls were excised arthroscopically.
Postoperative course included a 3-month rehabilitation program comprising 30 physical therapy sessions. The patient achieved complete resolution of knee pain, full recovery of strength and range of motion, and returned to sports without limitations.
DISCUSSION
ACL ganglion cysts are rare intra-articular lesions, particularly in pediatric patients. Most are incidental findings on MRI or arthroscopy and are often asymptomatic. When symptomatic, common presentations include knee pain, reduced range of motion, or mechanical symptoms such as locking or clicking, especially at terminal flexion or extension.
Etiology remains debated, with three main hypotheses:
- Mucinous degeneration of connective tissue.
- Microtrauma-induced hyaluronic acid release, separating ACL fibers and forming a cystic cavity.
- Synovial herniation through capsular or tendinous defects secondary to trauma.
Although predominantly reported in adults, pediatric cases—such as the one described by Fillingham et al.—highlight the need to consider this diagnosis in children with unexplained knee pain. Mao et al. reviewed 31 cruciate ligament ganglia and noted that symptomatic cases respond well to surgical intervention.
Diagnosis is best achieved with MRI, which allows clear visualization of cyst morphology, content, and relation to surrounding structures. MRI also helps distinguish ACL ganglion cysts from mucoid degeneration, though both may coexist.
Management of symptomatic lesions typically involves arthroscopic resection, which offers direct visualization, complete excision, low recurrence rates, and favorable functional outcomes. Image-guided percutaneous aspiration has been described as a minimally invasive alternative in select patients, but recurrence risk is higher. Although bilateral and multiple cysts are exceedingly rare, awareness of such variants is important in atypical or persistent cases.
CONCLUSION
ACL ganglion cysts are rare, especially in the pediatric population, and should be considered in the differential diagnosis of chronic knee pain with mechanical symptoms. MRI remains the gold standard for diagnosis, allowing precise localization and characterization. Arthroscopic resection is the treatment of choice in symptomatic patients, providing rapid pain relief and restoration of function. Early recognition can prevent unnecessary delays in management and facilitate prompt return to activities.
Conflict of Interest Statement:
None.
Funding Statement:
None.
Acknowledgements:
None.
REFERENCES
- Zampeli F, Terzidis I, Bernard M, Ochi M, Anastasios G. The Anterior Cruciate Ligament: Reconstruction and Basic Science. 2nd ed. 2018:431–436.
- Casas-Duhrkop D, Ares O, Seijas R, Cugat RJ. Ganglión en ligamento cruzado anterior: a propósito de un caso. Acta Ortop Mex. 2013;27(4):246–249.
- Fillingham YA, Coe MP, Hellman M, Haughom B, Adeniran AO, Sparks MB. Report of ganglion cyst in the anterior cruciate ligament of a 6-year-old child. Knee. 2013;20(2):144–147. doi:10.1016/j.knee.2012.10.008
- Mao Y, Dong Q, Wang Y. Ganglion cysts of the cruciate ligaments: A series of 31 cases and review of the literature. BMC Musculoskelet Disord. 2012;13:2–5.
- Sonnery-Cottet B, et al. Anterior Cruciate Ligament Ganglion Cyst Treated Under Computed Tomography–Guided Aspiration in a Professional Soccer Player. Orthop J Sports Med. 2016;4(5). doi:10.1177/2325967116644585
- Vaishya R, Issa AE, Agarwal AK, Vijay V. Anterior Cruciate Ligament Ganglion Cyst and Mucoid Degeneration: A Review. Cureus. 2017;9(9):e1682. doi:10.7759/cureus.1682
- Pimprikar MV, Patil HG. Anterior Cruciate Ligament Ganglion and Decompression of Mucoid Degeneration Using a “Figure-of-4 Position.” Arthrosc Tech. 2024;13(8):103026. doi:10.1016/j.eats.2024.103026
- Krill M, Peck E. Percutaneous Ultrasound-Guided Aspiration of an Anterior Cruciate Ligament Ganglion Cyst: Description of Technique and Case Presentation. PM&R. 2014;6(12):1166–1169. doi:10.1016/j.pmrj.2014.07.008
- Demircay E, Ofluoglu D, Ozel O, Oztop P. Simultaneous bilateral ganglion cysts of the anterior cruciate ligaments. Singapore Med J. 2015;56(4):e59–e61. doi:10.11622/smedj.2015062
- Lunhao B, Yu S, Jiashi W. Diagnosis and treatment of ganglion cysts of the cruciate ligaments. Arch Orthop Trauma Surg. 2011;131(8):1053–1057. doi:10.1007/s00402-011-1286-5
- Kang CN, Lee SB, Kim SW. Symptomatic ganglion cyst within the substance of the anterior cruciate ligament. Arthroscopy. 1995;11(5):612–615. doi:10.1016/0749-8063(95)90141-8
- Andrikoula SI, Vasiliadis HS, Tokis AV, Kosta P, Batistatou A, Georgoulis AD. Intra-articular ganglia of the knee joint associated with the anterior cruciate ligament: a report of 4 cases in 3 patients. Arthroscopy. 2007;23(7):800.e1–6. doi:10.1016/j.arthro.2006.05.032

