AI Solutions for Women’s Mental Health Disparities
Assessing Whether Women’s Unique Needs and Persistent Disparities in Mental Health Care Are Being Addressed by Emerging AI-Powered Digital Health Solutions
Perri Kasen¹, Julie Nguyen¹, Christine Hildreth¹, Emily Chapple², Kira Donaldson¹, Natasha Eslami¹, Susan Garfield¹
- Ernst & Young LLP
- Ernst & Young Services Pty Limited
OPEN ACCESS
PUBLISHED: 30 November 2024
CITATION: Kasen, P., Nguyen, J., et al., 2024. Assessing Whether Women’s Unique Needs and Persistent Disparities in Mental Health Care Are Being Addressed by Emerging AI-Powered Digital Health Solutions.
Medical Research Archives, [online] 12(11).
https://doi.org/10.18103/mra.v12i11.5996
COPYRIGHT: © 2024 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI https://doi.org/10.18103/mra.v12i11.5996
ISSN 2375-1924
ABSTRACT
Background: Mental health is a growing challenge, with women and girls disproportionately affected by conditions including anxiety and depression. These disparities are driven and exacerbated by factors such as socioeconomic status, race, and access to healthcare. Standards of care for these conditions vary, including combinations of in- and out-patient psychotherapy, pharmacotherapy, and behavioral therapies. Patients’ access to care is impacted by multifaceted system and individual level challenges, including provider shortages, cost, health literacy, and scheduling, with minority, economically disadvantaged, and neurodiverse women facing even greater barriers. Innovative digital health tools using artificial intelligence (AI) have the potential to address care gaps and narrow disparities for women and other vulnerable groups.
Methods: A systematic review of available technologies was conducted to identify current AI solutions and digital health interventions focused on depression, anxiety, or overall mental wellbeing. A solution taxonomy was developed based on similar AI-enabled services. The solutions were categorized based on intervention modality, disease focus, target population, realized outcomes, and business model. The solution’s intent and ability to address mental health challenges for women was then assessed.
Results: Current patient-facing mental health solutions include conversational AI support, healthy habit formation support, personalized care plans, screening tools, biometric risk factor identification, and digital music therapy. Among the examined technologies, 3 of 23 (13%) were designed for women and girls, and two of those solutions focused on women’s reproductive years. Just over half of assessed solutions (52%) use business-to-business-centric business models, requiring employers, payers, or providers to enable access.
Conclusions: AI-driven approaches can complement traditional mental health services by providing targeted education, improved access, and personalized care. Despite the potential to reduce gender disparities in mental healthcare, most AI solutions do not specifically address the needs of women and girls. Opportunities for greater impact include tailoring interventions to better suit women from diverse backgrounds, improving access through business model innovation, and expanding clinical integration in alignment with evidence-based treatment. Future research should focus on the long-term impact of AI interventions on mental health outcomes, designing specific tools for women and girls, and the risk of exacerbating biases by using AI in mental healthcare.
Introduction
As the industry’s recognition and understanding of health disparities has increased, digital health technology adoption has accelerated efforts to improve and personalize healthcare management, delivery, and experience. Across disease areas, care settings, and stakeholders, investment in digital health product and service development is growing exponentially: from 2015 to 2030, the digital health market is projected to grow 25x, reaching nearly $2 trillion.¹,²
With the emergence of consumer-focused artificial intelligence (AI), applications within healthcare have accelerated the growth and deepened the impact potential of digital health solutions within high need areas like mental health. Major trends for AI-enabled mental health efforts currently focus most heavily on leveraging AI for care delivery, patient engagement, and to derive actionable data-driven patient insights. Across its applications, AI also has the potential to address key aspects of mental health care where access and quality of care gaps exist. In doing so, AI as a component of mental health-focused digital health solutions may be a new tool to address the persistent disparities affecting vulnerable populations, including women and girls.
Although mental health is a critical component of overall wellbeing, women are disproportionately affected by certain mental health conditions compared to their male counterparts. Women are nearly twice as likely to be diagnosed with anxiety or depression, nearly three times as likely to be diagnosed with post-traumatic stress disorder (PTSD), and three times as likely to experience eating disorders such as anorexia nervosa or bulimia nervosa.³ Women are also disproportionately impacted by some health issues, like chronic migraines, that can impact mental health and wellbeing. Race, ethnicity, socioeconomic status, and other demographics can drive cumulative risk factors and lead to greater disparities in mental health diagnoses, access to care, and outcomes.
Despite high prevalence amongst women, mental health burdens are often under diagnosed and inadequately treated.⁴ These disparities are fueled by systemic barriers such as gender-based socioeconomic gaps, inadequate access to care, implicit bias in health and social systems, structural racism, cultural stigma, and gender norms that undermine women prioritizing their own health.⁵
The current state of AI-enabled digital health solutions targeting women’s specific mental health needs has not been explored. Specifically, little has been written assessing how AI is being leveraged to advance care beyond traditional digital health solutions. Additionally, the business models being leveraged for current solutions and used to support ongoing investment in this space have not been reviewed. This study reviews currently available solutions, ascertains the degree to which they are designed to address women’s needs specifically, reviews their business models, and identifies opportunities for future development.
Methods
This systematic review examines current AI-enabled digital mental health applications/solutions based on their clinical goals, target populations, and the degree to which they specifically seek to address women’s mental health needs. We focused on applications targeting the highly prevalent mental health conditions of anxiety and depression, though solutions were included if they indicate use for either anxiety or depression in addition to other mental health conditions. Similarly, the review was limited to patient-facing AI-enabled applications, though those with both patient- and provider-facing components were included. Wholly provider-facing solutions, including AI-powered clinician empathy and decision-making support, were excluded from analysis.
A string search approach was used to identify relevant solutions, with keywords including a combination of AI, artificial intelligence, mental health, digital health, behavioral health, anxiety, depression, health disparities, and women. This search was supplemented with data from a proprietary database tracking venture capital and private equity transactions, to understand leading mental health technology companies operating in this market. A data extraction yielded deals within the healthcare industry from 2019 to 2024. The top 50 mental health-related startups by deal size were reviewed to identify additional digital mental health solutions relevant for inclusion.
Combined, this yielded a short list of 45 mental health technology solutions. Examination of each solution’s website, marketing materials, and recent media coverage was conducted to confirm relevance for our study. At this stage, solutions were included in the final analysis based on condition of focus and inclusion of AI technology in the solution.
Further secondary research was undertaken to analyze key dimensions of each of the remaining solutions, including stage at which the technology is meant to be used in the patient journey, solution modality, disease focus, target population, realized outcomes, and business model. This secondary review leveraged publicly available information on product websites, media and press articles, and customer reviews. A six-category solution taxonomy was developed to group similar AI-enabled use cases across the solution set. These categories are detailed in Table 1.
Table 1: Solution Taxonomy Categories
Conversational AI Support | Healthy Habit Formation | Personalized Care Plans | AI Screening Tools | Biometric Risk Factor Identification | Digital Music Therapy
Results
AGGREGATE FINDINGS
The search methodology yielded 23 solutions that met the inclusion criteria.⁷–²⁹ Findings across the solution set are presented below for each dimension analyzed.
Patient journey stage
All AI solutions reviewed were designed to supplement traditional interventions like behavioral therapy and pharmacotherapy. While most of the solutions were designed using clinical research or informed by clinical guidance, these solutions are not intended to formally diagnose patients or function as stand-alone treatments.
Accordingly, the AI solutions were categorized into three stages of the patient journey: Exploration, Screening, and Management. Notably, some solutions addressed multiple stages of this journey (see Table 2). The majority of reviewed solutions addressed the Management stage of the patient journey, either in combination with another stage of the patient journey (7 of 23) or as the sole focus (15 of 23). Finally, no solutions were found that focused solely on the exploration stage of the patient journey.
Table 2: Number of solutions by stage of patient journey addressed
- Exploration: Solution includes capabilities to direct users to mental health resources
- Screening: Solution includes capabilities to identify symptoms and notify users
- Management: Solution includes capabilities to help manage mental health symptoms
(Number of solutions shown in table: 2, 1, 5, 15 depending on combinations)
Modality
The majority (19 of 23; 83%) of reviewed AI mental health solutions are designed for patient use via smartphone applications.³⁰ Three solutions (13%) integrate within patient engagement tools for providers and payers or enterprise platforms, such as Slack or Teams, for employers.
Disease focus
Among the AI solutions analyzed, the majority included depression or anxiety as a disease focus (15 of 23; 65%). Of those 15, one solution included interventions specifically targeted towards sleep. While many of the solutions mention depression and anxiety, none of the solutions are designed to treat clinical depression or anxiety. Instead, they are meant to either screen for symptoms (5 of the 23 solutions) and/or provide general wellbeing support for stress management and healthy habit formation. Two solutions were focused specifically on health concerns across the life course, including family planning, pregnancy, postpartum, and menopause, and 6 solutions were focused on emotional support and wellbeing.
Target population
The AI solutions reviewed largely have a broad target audience, with limited, if any, offerings for specific populations. 5 of 23 indicate a specific population of focus, with 3 solutions focusing specifically on women, 1 solution focusing on LGBTQIA+ individuals, and 1 solution focusing on seniors and caregivers.
Language accessibility
Language accessibility varied by solution, with 61% only offering English-based services and the remaining 39% offering services in English and at least one other language. Only 4 solutions were available in five or more languages. Additional languages offered across the solution set include French, German, Spanish, Italian, Portuguese, Swedish, Chinese, Korean, Japanese, Hindi, Punjabi, Bengali, Marathi, and Urdu.
ARTIFICIAL INTELLIGENCE SOLUTION USE CASES
Through examination of the services provided, a six-category solution taxonomy was developed to categorize similar AI use cases. It is common for existing solutions to offer more than one AI use case (see Table 3).
Table 3: Number of Solutions by AI Solution Use Case
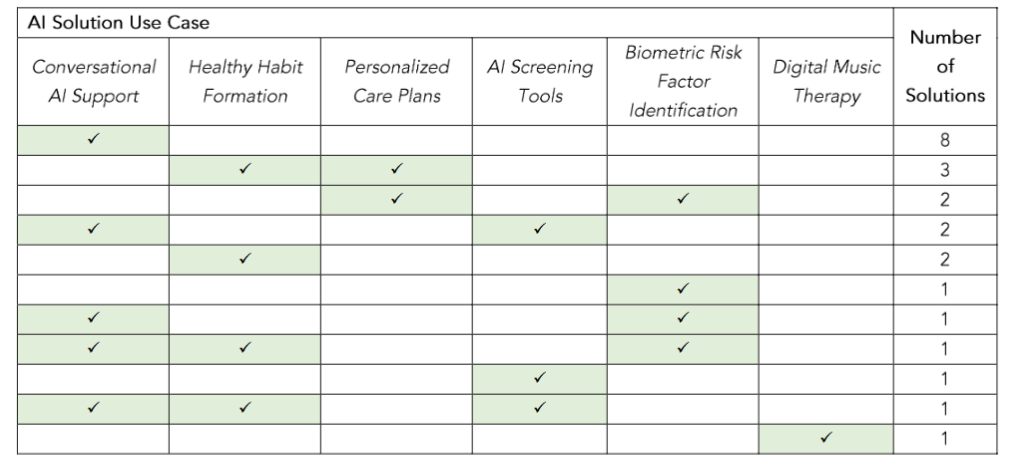
Conversation-based support
Across the solution set, the most common AI functionality within mental health solutions comes in the form of AI-powered conversational support. Found in 13 of 23 reviewed solutions (57%), this technology entails text- or voice-based virtual mental health companions that offer on-demand emotional support, including cognitive behavioral therapy. While all of these tools provide virtual chatbot support through a text-based AI chatbot, one solution is unique in its use of AI voice technology to engage users in live phone calls.
As the prevailing form of digital mental health support on the market today, conversational AI support is commonly found alongside other AI mental health use cases, including personalized care plans, healthy habit formation, screening tools, and biometric risk factor identification.
The majority of reviewed AI chatbots (10 of 13; 77%) are designed for all to use. The remaining three conversational AI support tools are explicitly designed to meet the mental health needs of women. Of these, two focus on mental wellbeing and stress management during women’s reproductive journey while the other engages women across the life course on diverse health, mental health, and parenting topics.³¹
Healthy habit formation
The second most common use case amongst the reviewed solutions was healthy habit formation support (8 of 23; 35%). These AI tools support users in setting and maintaining personal goals for behaviors known to boost mood, reduce stress, and improve cognitive function. Solutions in this category offer diverse user engagement related to movement, mindfulness, meditation, rest, and other health promoting behaviors. Several apps gamify the content to incentivize sustainable habit formation aligned with long-term mental wellbeing. One solution with this functionality is tailored to women.
Personalized care plans
Seven of the 23 reviewed solutions (30%) offer personalized care plans and mental health educational content powered by AI. This functionality entails leveraging information about user preferences and mental health symptoms to recommend tailored content that has demonstrated effectiveness in reducing stress and promoting long-term mental resiliency. The types of personalized content offered varies by solution, including cognitive behavioral therapy exercises, … (text continues beyond visible portion) guided meditation, sleep support, and mental fitness training.
This functionality is found in solutions that also offer either biometric risk factor identification, healthy habit formation support, or AI chatbots. Among solutions offering personalized care plans, five include tools to enable development of health promoting behaviors, two also leverage biomarker analysis, and one offers empathy support via a virtual assistant.
Mental health screening tools
Mental health screening functionality supported by AI was found in 5 of 23 reviewed solutions (22%). This solution type entails the use of evidence-based behavioral health screening tools, such as PHQ-9 for depression and GAD-7 for anxiety, coupled with predictive algorithms to increase early identification and triage of common mental health symptoms.
Of these tools, four offer mental health assessments as an entry point to their broader suite of digital mental health offerings, including conversational chatbots and health behavior trackers. One solution stands alone as a screening-only tool, offering assessments for more than ten mental health conditions ranging from depression to obsessive-compulsive disorder (OCD) and PTSD¹⁸. Two screening solutions highlight electronic medical record (EMR) integration as a core feature.
These tools are primarily designed for general use across population segments. One solution, however, focuses on women’s mental wellbeing across the life course through a suite of products targeting fertility, pregnancy, motherhood, and menopause. As of August 2024, this solution is authorized by the FDA as the first and only prescription digital therapeutic on the market for the treatment of postpartum depression symptoms. Clinical studies found that the predictive screening tools identified 88% of women who went on to experience postpartum depression by the beginning of their third trimester³². Accessing this tool requires a prescription from a healthcare provider.
Biometric risk factor identification
AI-powered biometric risk factor identification technology was present in 4 of 23 solutions (17%). This technology involves a variety of AI tools that analyze users’ voice, texting patterns, and body language to “predict” common mental health disorders, including depression and anxiety. These tools rely on analysis of “Medically Relevant Expressed Behaviors,” a class of novel biomarkers based on observable actions, gestures, or vocalizations that provide insight into one’s physical and mental health³³.
Biometric risk factor identification functionality is not a stand-alone offering. Two solutions also leverage a virtual chatbot to engage users and offer empathetic support, while the other two offer personalized care recommendations and education based on risk factors identified via biometric analysis.
Two of four of these solutions indicate a specific user population – one supports seniors and caregivers while the other engages women across the reproductive journey. The app that targets seniors assesses changes in vital biomarkers, including blood pressure, heart rate, respiratory rate, and blood oxygen levels, with a daily selfie and uses that insight to assess risk for depressive symptoms. The pregnancy-focused solution leverages visual and auditory inputs to detect mental disorders, mood, and stress levels from fertility to postpartum.
Digital music therapy
Found within just one solution, digital music therapy is the least common functionality found in AI mental health tools today. This technology entails the use of AI-generated personalized music playlists complemented by auditory beat stimulation, a form of auditory stimuli that induces targeted brain activity to increase cognitive focus, reduce stress, and boost mood³⁴. The digital music therapy app reviewed for this study falls into the broader category of “Software as a Medical Device.” This solution is backed by clinical studies validating the benefit of AI-generated playlists. Following a single 24-minute session of AI-curated music and auditory beat stimulation, users report a 16% reduction in anxiety on average. Though the solution is designed for use by all populations, it currently requires a doctor’s prescription and is only reimbursable through Medicare for older adults experiencing anxiety or elevated stress.
SOLUTION EFFICACY AND ACCESS
Realized outcomes
Information on realized outcomes across solutions was limited, and those that reported outcomes typically shared user adoption metrics, including the number of app downloads, active users, messages sent, and therapy sessions conducted (7 of 23; 30%) versus clinical outcomes. Some solutions highlighted user-reported improvements such as improved mood (7 of 23; 30%). Additionally, a few of the solutions are currently undergoing clinical trials to measure more definitive outcomes (2 of 23; 9%).
Business model
Among the solutions reviewed, their business models largely focused on either business-to-business (B2B) or direct-to-consumer (DTC) sales.
Six different types of go-to-market channels were identified:
- B2B: Employer-sponsored benefit,
- B2B: School-sponsored benefit,
- B2B: Clinician integration (solutions offered to the clinician’s entire patient panel through integration with a clinician technology platform),
- DTC: Individual user subscription,
- Digital Therapeutic (solutions requiring a prescription from a clinician), and
- Free.
Table 4 outlines frequency of business models used across the solution set.
A little over half of the solutions reviewed used more than one go-to-market channel in their business models (12 of 23; 52%). The majority of the solutions (14 of 23; 61%) included direct-to-consumer subscriptions in their business models, with varying price points based on subscription length. Business-to-business channels were also commonly included in the business models (11 of 23; 48%), which may limit access for individuals who are not members of these programs. A few solutions were either free or still in testing, offering free access to study participants (4 of 23; 17%). One solution was a digital therapeutic with FDA approval, requiring a prescription and qualifying for insurance reimbursement.
Table 4: Number of Solutions by Go-to-Market Channel
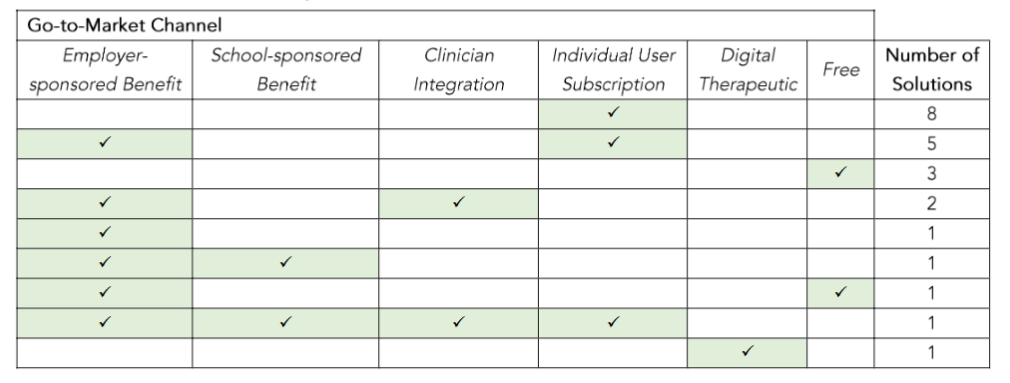
Discussion
DIGITAL MENTAL HEALTH TOOLS LARGELY COMPLEMENT – RATHER THAN REPLACE – TRADITIONAL MENTAL HEALTH CARE
The majority of digital and AI-enabled mental health solutions today are not designed to be a replacement for traditional mental health care, including psychotherapy, pharmacotherapy, and behavioral therapies. As these tools extend care to those who may need additional support in-between appointments, the greatest opportunity described is when they are used in coordination with provider care plans. By sharing mental wellbeing data with provider teams, these AI technologies provide insight into patients’ experiences between clinical appointments and enable improved treatment quality tailored to individual patients.
Most technologies reviewed offer multiple forms of AI-enabled mental health support, pointing to the growing trend of mental health apps offering integrated solutions to address users’ multifaceted needs. Notably, many reviewed solutions explicitly mention the potential risks of using these tools in isolation, particularly for those experiencing severe mental health symptoms. In this manner, AI-driven approaches can complement traditional mental health services by providing targeted education, improved access, and personalized care.
CURRENT BUSINESS MODELS CONTRIBUTE TO INEQUITABLE ACCESS TO DIGITAL MENTAL HEALTH TOOLS
Just over half of assessed solutions (52%) use some form of B2B business models, requiring employers, payers, or providers to enable access for their employees, members, or patients. There is a growing market for employer wellbeing solutions to serve the mental health needs of their employees, estimated to reach more than $58 billion USD globally by 2027³⁵. Similarly, payer and provider organizations are increasingly contracting with third party vendors to offer AI-enabled patient engagement tools as a complement to traditional clinical care³⁶. B2B business models may increase access to mental health support by engaging individuals who may not otherwise seek care. However, they are likely to perpetuate existing disparities by targeting already served populations.
Direct-to-consumer (DTC) business models are used by 61% of reviewed solutions, requiring users to pay monthly or annual subscriptions that range from $5 to nearly $500 USD. While these tools may be more affordable than out-of-network therapists that can cost more than $200 USD per session, DTC business models may perpetuate existing access and affordability barriers to timely, effective mental health support.
INNOVATION IN ARTIFICIAL INTELLIGENCE-POWERED MENTAL HEALTH SOLUTIONS IS NOT YET GENDER EQUITABLE BY DESIGN AND DOES NOT ADDRESS CURRENT DRIVERS OF MENTAL HEALTH DISPARITIES FOR WOMEN
Despite their potential to reduce gender disparities in mental healthcare, most AI solutions do not specifically address the unique mental health needs of women and girls. Of existing women-centric AI mental health solutions today, the majority prioritize wellbeing during the reproductive journey thereby leaving women’s non-pregnancy related mental health needs to be addressed by universal solutions. The market is not currently serving the mental health needs of adolescent girls and older women navigating stress during puberty and menopause, respectively.
Considering existing research that demonstrates women are much more likely to prefer female mental health providers, the lack of women-centric design within current AI mental health solution market may not meet demand for gender-tailored interventions³⁶. Access to these solutions is further complicated by existing business models that prioritize higher income populations, creating questions of affordability for women of lower socioeconomic status who are more likely to face compounding stressors across life domains (i.e., school, work, home).
This study underscores the reality that solutions on the market today are not designed to address the complex root causes of mental health disparities for women. Current solutions focus on identification and management of mental health symptoms, with little technology supporting prevention of mental health challenges before they begin. It is notable that just two reviewed solutions offer functionality focused on the Exploration phase of the patient journey, while the majority prioritize identification and management of existing disease.
With a focus on alleviating downstream mental health symptoms, these tools aim to engage users in individual-level interventions that bolster one’s mental resiliency and expand coping skills. While necessary, this approach is not sufficient to address the multifaceted structural and societal factors that contribute to higher levels of stress, marginalization, and inequity facing women across the globe.
ADDITIONAL SYSTEM AND INDIVIDUAL-LEVEL ADOPTION BARRIERS LEAVE WOMEN AT RISK
Individuals may face additional barriers to using AI-powered mental health tools beyond functional considerations of consumer channel and personal cost. For example, the digital divide – unequal access to modern telecommunications technology such as broadband internet – reinforces care gaps for digitally underserved geographies. Personal health literacy levels affect beliefs about mental health and care seeking patterns, while digital literacy levels shape one’s ability to navigate AI solutions. With 61% of AI tools included in this study offering English-only language platforms, non-English speakers, who may experience adverse social determinants of health that contribute to disparities in care and outcomes, face compounding challenges in accessing current digital mental health solutions³⁶.
Concerns also exist about user preferences and trust of generative AI. Emerging evidence shows women are adopting generative AI in the workplace at slower rates than their male counterparts, with gender disparities persisting across age groups and multiple geographies³⁷. Considering the prevalence of B2B business models enabling access to AI mental health tools through employer wellbeing benefits, it will be important for future research to consider adoption through an intersectional gender lens.
Conclusion
This systematic review of AI-enabled mental health solutions found that the majority of current AI tools are designed to supplement traditional care, with a focus on management and general wellbeing rather than clinical diagnosis or standalone treatment. Nearly all of the solutions reviewed were not tailored to specific populations or women, despite the prevalence of mental health disparities among women. Business models and language accessibility barriers further exacerbate disparities, with B2B channels potentially excluding those not covered by employer, payer, or provider programs, and individual user subscription models presenting affordability issues.
Prioritization of vulnerable populations – including women who represent more than half of the world’s population – must be a strategic priority within technological innovation. Opportunities for greater impact include tailoring AI-enabled interventions to better suit women from diverse backgrounds, improving access through business model innovation, and expanding clinical integration in alignment with evidence-based treatment. Additional clinical research is needed to understand AI technology’s differential adoption and impact by gender³⁴. Additional barriers to adoption, including the digital divide, health literacy, and trust in generative AI, must also be addressed to improve access and address drivers of health disparities.
A coordinated ecosystem approach that leverages interventions at societal, organizational, and individual levels is needed to comprehensively address the upstream and downstream factors contributing to mental health disparities disproportionately affecting women. As digital health solutions continue to transform the healthcare industry, future research should focus on digital health tools that foster prevention, the long-term impact of AI interventions on mental health outcomes, design considerations for specific tools for women and girls, and practices to ensure equitable access.
Conflict of Interest:
The authors have no conflicts of interest to declare.
Funding Statement:
None.
Acknowledgements:
None.
References
1. Statista. Digital Health.; 2024. Accessed August 12, 2024. https://www.statista.com/study/27232/digital-health-statista-dossier/
2. Fortune Business Insights. Digital Health Market Size, Share & COVID-19 Impact Analysis, By Product Type.; 2024. Accessed August 12, 2024. https://www.fortunebusinessinsights.com/industry-reports/digital-health-market-100227
3. American Psychiatric Association. Mental Health Disparities: Women’s Mental Health. Published online 2017. Accessed August 12, 2024. https://www.psychiatry.org/getmedia/aa325a61-5b60-4c71-80f1-dc80cf83c383/Mental-Health-Facts-for-Women.pdf
4. Floyd BJ. Problems in accurate medical diagnosis of depression in female patients. Social Science & Medicine. 1997;44(3):403-412. doi:10.1 016/S0277-9536(96)00159-1
5. Centers for Disease Control and Prevention (CDC). Mental Health Disparities by Race and Ethnicity. Centers for Disease Control and Prevention (CDC). Accessed August 12, 2024. https://www.cdc.gov/mentalhealth/learn/index.htm
6. PitchBook. Accessed August 12, 2024. https://pitchbook.com/data
7. Minding Health. 2024. Accessed August 12, 2024. https://www.ablemind.co/healthcare
8. Curio. 2024. Accessed August 12, 2024. https://www.curiodigitaltx.com/
9. BlueSkeye Avocado. 2023. Accessed August 12, 2024. https://www.blueskeye.com/avocado
10. Breakthru. 2024. Accessed August 12, 2024. https://breakthru.me/
11. Calm. 2024. Accessed August 12, 2024. https://www.calm.com/
12. Clare&Me. 2024. Accessed August 12, 2024. https://www.clareandme.com/
13. Earkick. 2024. Accessed August 12, 2024. https://earkick.com/
14. Elomia. 2024. Accessed August 12, 2024. https://elomia.com/
15. Ema. 2023. Accessed August 12, 2024. https://www.emaapp.co/solutions
16. Evolve. 2024. Accessed August 12, 2024. https://evolveinc.io/
17. Flow Lab. 2024. Accessed August 12, 2024. https://flowlab.com/en/
18. Mindstep. 2023. Accessed August 12, 2024. https://www.letsmindstep.com/en-us/apis
19. Headspace. 2024. Accessed August 12, 2024. https://www.headspace.com/
20. Kintsugi. 2022. Accessed August 12, 2024. https://www.kintsugihealth.com/solutions/kintsugiapp
21. LUCID. 2022. Accessed August 12, 2024. https://www.lucidtherapeutics.com/
22. MindDoc. 2024. Accessed August 12, 2024. https://minddoc.com/us/en
23. Serena. 2024. Accessed August 12, 2024. https://serena.chat/
24. Sibly. 2022. Accessed August 12, 2024. https://www.sibly.com/
25. Together by Renee. 2024. Accessed August 12, 2024. https://togetherapp.com/
26. Happify. 2024. Accessed August 12, 2024. https://happify.com/
27. Woebot Health. 2024. Accessed August 12, 2024. https://woebothealth.com/
28. Wysa. 2024. Accessed August 12, 2024. https://www.wysa.com/
29. Youper. 2024. Accessed August 12, 2024. https://www.youper.ai/about-us
30. Leventhal R. Nearly two-thirds of US consumers are mobile health app users. EMarketer. https://www.emarketer.com/content/nearly-two-thirds-of-us-consumers-mobile-health-app-users. February 21, 2023. Accessed August 12, 2024.
31. Femtech Insider. Ema App Raises Nearly $2M in Funding for Its Conversational AI for Women’s Health. Femtech Insider. https://femtechinsider.com/ema-app-2m-bridge-round/. February 27, 2024. Accessed August 12, 2024.
32. Using AI to predict health problems before they’re problems. 2024. Accessed August 12, 2024. https://www.curiodigitaltx.com/
33. BlueSkeye AI Capabilities. 2023. Accessed August 12, 2024. https://www.blueskeye.com/capabilities
34. Pelc C. Anxiety: Personalized playlists and ‘auditory beat stimulation’ may help. Medical News Today. https://www.medicalnewstoday.com/articles/anxiety-personalized-playlists-and-auditory-beat-stimulation-may-help#1. September 3, 2022. Accessed August 12, 2024.
35. Lamb J, Israelstam G, Agarwal R, Bhasker S. Generative AI in healthcare: Adoption trends and what’s next. July 25, 2024. Accessed August 12, 2024. https://www.mckinsey.com/industries/healthcare/our-insights/generative-ai-in-healthcare-adoption-trends-and-whats-next
36. Wang PG, Brisbon NM, Hubbell H, et al. Is the Gap Closing? Comparison of Sociodemographic Disparities in COVID-19 Hospitalizations and Outcomes Between Two Temporal Waves of Admissions. J Racial and Ethnic Health Disparities. 2023;10(2):593-602. doi:10.1007/s40615-022-01249-y
37. Kreacic A, Stone T. Women are falling behind on generative AI in the workplace. Here’s how to change that. World Economic Forum. April 2, 2024. Accessed August 12, 2024. https://www.weforum.org/agenda/2024/04/women-generative-ai-workplace/




