Global CME Strategies for Orthopedic Trauma Education
How can a global organization make education local?
Research Article
Authors: Ana Maria Montero1, Alexandra Wentschel2, Kodi E. Kojiwar3, Michael R. Baumgaertner4, Jezeh Reichmuth5, Monica Ghidinelli6
Affiliations:
1. Education Institute, AO Foundation, Davos, Switzerland
2. Instituto de Ortopedia, Hospital das Clínicas HCFMUSP, Faculdade de Medicina, Universidade de São Paulo, São Paulo, Brazil
3. Department of Orthopedics, Prince Mohammed bin Abdulaziz Hospital, Riyadh, Saudi Arabia
4. Department of Orthopedics and Rehabilitation, Yale University School of Medicine, USA
5. Department of Orthopedics, University of Basel, Switzerland
6. Department of Orthopedics, University of São Paulo, Brazil
OPEN ACCESS
PUBLISHED: June 2025
CITATION: MORENO, Ana Maria et al. How can a global organization make education local? Workplace education for surgeons treating orthopedic trauma cases. Medical Research Archives, [S.l.], v. 13, n. 6, june 2025. Available at: <https://esmed.org/MRA/mra/article/view/6677>
COPYRIGHT: © 2025 European Society of Medicine. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
DOI: https://doi.org/10.18103/mra.v13i6.6677
ISSN 2375-1924
ABSTRACT
Continuing medical education (CME) and continuing professional development (CPD) events every year, provided by medical societies, medical education providers, or hospitals. Such in-person CME/CPD events require participants to travel to a designated location, posing logistical challenges such as time constraints, travel and accommodation costs, and potential disruptions to clinical practice. Workplace-based CME/CPD initiatives are a viable alternative to address the challenges associated with traditional models. This paper explores how a global organization can adapt educational offerings to local contexts, enhancing accessibility and relevance for healthcare professionals.
Keywords
- Continuing Medical Education
- Workplace-based Education
- Healthcare Professionals
- Local Contexts
Introduction
Continuing medical education (CME) and continuing professional development (CPD) events every year, provided by medical societies, medical education providers, or hospitals. Such in-person CME/CPD events require participants to travel to a designated location, posing logistical challenges such as time constraints, travel and accommodation costs, and potential disruptions to clinical practice. Workplace-based CME/CPD initiatives are a viable alternative to address the challenges associated with traditional models. This paper explores how a global organization can adapt educational offerings to local contexts, enhancing accessibility and relevance for healthcare professionals.
Methodology
The module was designed to be flexible; a complete module for face-to-face events contains up to 4 weeks of teaching material. Faculty can tailor the event duration from 60 minutes to 4 hours to meet the needs of the participants and the hospital. The module packages include a user manual for the course director, a pre-and post-course knowledge assessment based on clinical vignettes, pre-reading material, lecture slide sets, cases for small group discussions, a certificate of attendance, instructions for evaluation forms, and an evaluation form. The faculty can select content appropriate for their participants according to their experience level, hospital requirements, and knowledge increase.
Delivery Method
Data were collected from June 2022 to June 2024 (total activities recorded), with a substantial increase in 2023, documenting 76 events (45.0%). Through June 2024 (study endpoint), 52 events were implemented, comprising 30.8% of total activities. Data demonstrated the highest implementation, with 3 events followed by Pakistan (20 events), Egypt (17 events), and Mexico (12 events).
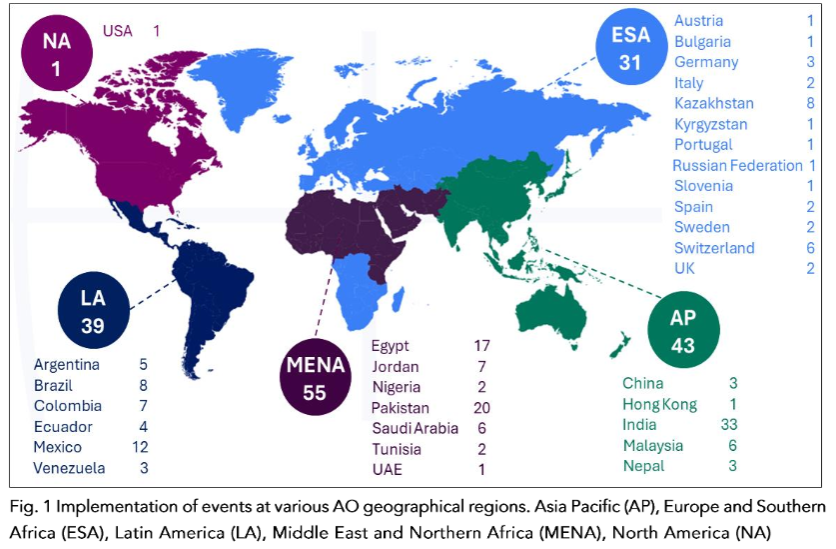
Results
The polytrauma module demonstrated predominant engagement, comprising 65 educational sessions and attracting 1,206 participants (30.5% of the total attendance). The open fractures and geriatric hip fracture standardized initiatives demonstrated notable enhancements in clinical competencies. Statistical validation showed participants’ self-reported knowledge increased significantly post-event, with the highest representation (23.57%) observed in the open fractures module.
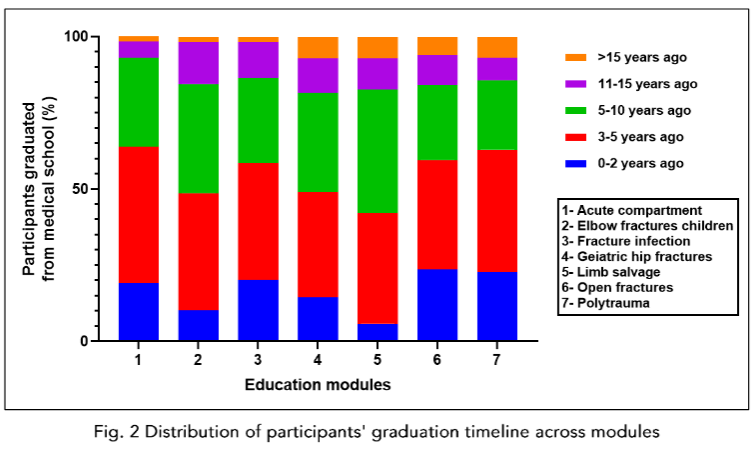
Discussion
As expected, the data indicated predominant participation of young professionals who had completed medical school 3-5 years prior, reaching 44.68% in the polytrauma module (below 50% in limb salvage). Within 0-2 years post-qualification, recent graduates constitute a notable majority, with their highest representation (23.57%) observed in the open fractures module.
Educational Outcomes
Learning (Moore’s Level 3) was measured based on participant self-reports of the acquisition of new knowledge relevant to their clinical practice, validating their current clinical approaches. A minimal proportion (2.10%) gained new insights but was unable to implement them, and 0.62% acquired knowledge but opted against the application.
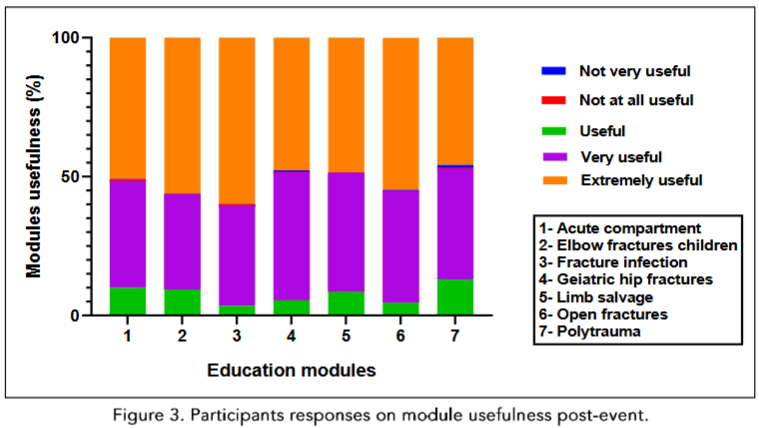
Conclusion
In conclusion, the study revealed the significant impact of workplace-based CME initiatives on clinical practice. By addressing these high-priority areas, the modules may contribute directly to reducing trauma-related morbidity and mortality, as supported in similar settings where trauma education has led to improvements in clinical care and patient outcomes.
Limitations
Despite these promising results, several limitations must be acknowledged. While we observed substantial improvements in participants’ competence, the study did not include a long-term follow-up to assess whether these changes translated into sustained improvements in patient care.
Conflicts of Interest Statement
The authors declare no conflict of interest.
Funding Statement
No specific funding was obtained for this study.
Acknowledgments
We thank all the course chairpersons and questionnaire participants for their contributions.
References
2. Walton M, Harrison R, Burgess A, et al. Workplace training for senior trainees: a systematic review and narrative synthesis of current approaches to promote patient safety. Postgrad Med J [Internet]. 2015;91(1080):579–87. Available from: http://dx.doi.org/10.1136/postgradmedj-2014-133130
3. O’Brien Pott M, Blanshan AS, Huneke KM, et al. Barriers to identifying and obtaining CME: a national survey of physicians, nurse practitioners and physician assistants. BMC Med Educ [Internet]. 2021 Mar 19;21(1):168. Available from: https://pubmed.ncbi.nlm.nih.gov/33740962
4. Alsaleem SA, Almoalwi NM, Siddiqui AF, et al. Current Practices and Existing Gaps of Continuing Medical Education among Resident Physicians in Abha City, Saudi Arabia. Int J Environ Res Public Health [Internet]. 2020 Nov 16;17(22):8483. Available from: https://pubmed.ncbi.nlm.nih.gov/33207729
5. Minor S, Poenaru D. The in-house education of clinical clerks in surgery and the role of housestaff. The American Journal of Surgery [Internet]. 2002; 184(5):471–5. Available from:
http://dx.doi.org/10.1016/s0002-9610(02)01001-2
6. Stefanescu MC, Sterz J, Hoefer SH, et al. Young surgeons’ challenges at the start of their clinical residency: a semi-qualitative study. Innov Surg Sci [Internet]. 2018 Jun 4;3(4):235–43. Available from: https://pubmed.ncbi.nlm.nih.gov/31579787
7. King R, Taylor B, Talpur A, et al. Factors that optimise the impact of continuing professional development in nursing: A rapid evidence review. Nurse Educ Today [Internet]. 2021;98:104652. Available from:
http://dx.doi.org/10.1016/j.nedt.2020.104652
8. Filipe HP, Silva ED, Stulting AA, et al. Continuing professional development: best practices. Middle East Afr J Ophthalmol [Internet]. 2014;21(2):134–41. Available from: https://pubmed.ncbi.nlm.nih.gov/24791104
9. Lave J, Wenger E. Situated Learning [Internet]. Cambridge University Press; 1991. Available from: http://dx.doi.org/10.1017/cbo9780511815355
10. Joeris A, Höglinger M, Meier F, et al. The impact of the AO Foundation on fracture care: An evaluation of 60 years AO Foundation. Injury [Internet]. 2019; 50(11):1868–75. Available from:
http://dx.doi.org/10.1016/j.injury.2019.07.016
11. Gosch M, Kammerlander C, Fantin E, et al. Design and Evaluation of a Hospital-Based Educational Event on Fracture Care for Older Adult. Geriatr Orthop Surg Rehabil [Internet]. 2021 Mar 31;12:21514593211003856–21514593211003856. Available from: https://pubmed.ncbi.nlm.nih.gov/33868767
12. Kraus MD, Mueller M, Schmitz B, et al. Development of a Performance Improvement Program: A Workplace-Based Educational Intervention on Magnetic Resonance Imaging in Spinal Trauma. J Surg Educ [Internet]. 2016;73(3):416–21. Available from: http://dx.doi.org/10.1016/j.jsurg.2015.12.005
13. Moore DE, Green JS, Gallis HA. Achieving desired results and improved outcomes: Integrating planning and assessment throughout learning activities. Journal of Continuing Education in the Health Professions [Internet]. 2009;29(1):1–15. Available from: http://dx.doi.org/10.1002/chp.20001
14. Moore DE, Chappell K, Sherman L, et al. A conceptual framework for planning and assessing learning in continuing education activities designed for clinicians in one profession and/or clinical teams. Med Teach [Internet]. 2018;40(9):904–13. Available from: http://dx.doi.org/10.1080/0142159x.2018.1483578
15. Kern D, Thomas P, Hughes M, et al. Curriculum Development for Medical Education: A Six-step Approach. Baltimore, MD: The John’s Hopkins University Press; 2009
16. Ghidinelli M, Cunningham M, Uhlmann M, et al. Designing and implementing a harmonized evaluation and assessment system for educational events worldwide. J Orthop Trauma. 2021;35 (suppl 2):S5–S10. available from:
https://journals.lww.com/jorthotrauma/Documents/Learning%20in%20the%20AO_Looking%20Back%20and%20Moving%20Forward.pdf
17. Mock CN, Quansah R, Addae-Mensah L, et al. The development of continuing education for trauma care in an African nation. Injury [Internet]. 2005;36(6):725–32. Available from:
http://dx.doi.org/10.1016/j.injury.2004.12.044
18. Tchorz KM, Thomas N, Jesudassan S, et al. Teaching Trauma Care in India: An Educational Pilot Study From Bangalore. Journal of Surgical Research [Internet]. 2007;142(2):373–7. Available from: http://dx.doi.org/10.1016/j.jss.2006.07.010
19. Petroze RT, Byiringiro JC, Ntakiyiruta G, et al. Can focused trauma education initiatives reduce mortality or improve resource utilization in a low-resource setting? World J Surg [Internet]. 2015 Apr;39(4):926–33. Available from: https://pubmed.ncbi.nlm.nih.gov/25479817
20. O’Brien L, Broom L, Ullah MM. Outcomes and Participant Experience of an Online Train-the-Trainer Program for Bangladeshi Health Professionals: A Case Study Evaluation. Journal of Continuing Education in the Health Professions. 2015; 35(1), 46–56. doi:10.1002/chp.21262
21. Thies KC, Bergmans E, Billington A, et al. The European Trauma Course: Transforming systems through training. Resusc Plus [Internet]. 2024 Mar 15;18:100599. Available from:
https://pubmed.ncbi.nlm.nih.gov/38515443
22. Kolb AY, Kolb DA. Experiential Learning Theory: A Dynamic, Holistic Approach to Management Learning, Education and Development [Internet]. The SAGE Handbook of Management Learning, Education and Development. SAGE Publications Ltd; 2009. p. 42–68. Available from: http://dx.doi.org/10.4135/9780857021038.n3
23. Michael Nnaemeka Ajemba, Chinweike Ikwe, Judith Chioma Iroanya. Effectiveness of simulation-based training in medical education: Assessing the impact of simulation-based training on clinical skills acquisition and retention: A systematic review. World Journal of Advanced Research and Reviews. 2024;21(1).
24. Kanneganti A, Sia CH, Ashokka B, et al. Continuing medical education during a pandemic: an academic institution’s experience. Postgrad Med J. 2020;96(1137).
25. Hancock K. Modular Online Learning Design: A Flexible Approach for Diverse Learning Needs (book review). Journal of the Canadian Health Libraries Association / Journal de l’Association des bibliothèques de la santé du Canada. 2021;42(1).

